* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download 30_Extracellular bact BA
Survey
Document related concepts
Monoclonal antibody wikipedia , lookup
Herd immunity wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Infection control wikipedia , lookup
DNA vaccination wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Neonatal infection wikipedia , lookup
Social immunity wikipedia , lookup
Molecular mimicry wikipedia , lookup
Complement system wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Immune system wikipedia , lookup
Adaptive immune system wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Transcript
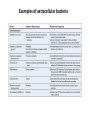
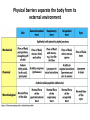
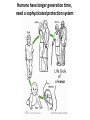
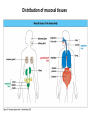
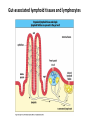
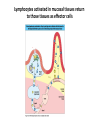
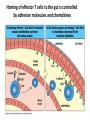
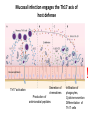
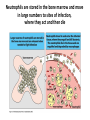
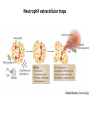
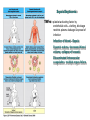
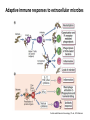
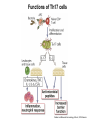
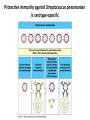
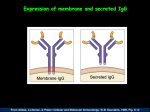
THE IMMUNE RESPONSES TO EXTRACELLULAR PATHOGENS PATHOGENS Viruses, Bacteria, Fungi Parasites Unicellular protozoa Multicellular worms REQUIRES HIGH INITIAL DOSE FOR INFECTION ESCAPE MECHANISMS TO AVOID DEFENSE MECHANISMS HUMAN BODY RESOURCE RICH ENVIRONMENT FOR PATHOGENS DEFENSE MECHANISMS Physical barriers/Innate immunity – STOP MOST INFECTIONS WITHOUT CALLING Adaptive immunity Diseases – Medical practice DISEASE Innate immunity fails to terminate infection Activation of adaptive immunity Successful evasion and subversion of the immune system by pathogens Pathogens have short generation time Virus 3 hrs 3 hrs Humans have longer generation time, need a sophysticated protection system Examples of extracellular bacteria Distribution of mucosal tissues Physical barriers separate the body from its external environment Movie: Mucosal immune tolerance and immune response Five ways in which the commensal gut microbiota benefit their human hosts The structure of mucins gives mucus its characteristic protective properties Secretory immunoglobulins become attached to the mucus, where they stand ready to bind commensal and pathogenic organisms Defensins disrupt microbial membranes Gut-associated lymphoid tissues and lymphocytes Epithelial cells contribute to the defense of mucosal tissue Uptake and transport of antigens by M cells Capture of antigens from the intestine by dendritic cells Lymphocytes activated in mucosal tissues return to those tissues as effector cells Homing of effector T cells to the gut is controlled by adhesion molecules and chemokines Mucosal infection engages the Th17 axis of host defense ! Th17 activation Secretion of chemokines Production of antimicrobial peptides Infiltration of phagocytes, Cytokine secretion Differentiation of Th17 cells The systemic and mucosal immune systems use different strategies for coping with infections Innate immune mechanisms establish a state of inflammation at sites of infection Immune defense involves recognition of pathogens followed by their destruction Phagocytosis and degradation of invading microorganisms by a tissue macrophage Neutrophils are stored in the bone marrow and move in large numbers to sites of infection, where they act and then die Neutrophil extracellular traps Exotoxins vs. endotoxin Exotoxins – secreted by living bacteria - Cytotoxicity of various mechanisms - Inhibition of various cellular functions Endotoxin – released by dying cells - Cell wall – Gram (-) LPS - Induction of cytokines septic shock Sepsis/Septicemia TNF-α→platelet activating factor by endothelial cells→clotting, blockage restricts plasma leakage & spread of infection Infection of blood – Sepsis Sysemic edema, decreased blood volume, collapse of vessels Disseminated intravascular coagulation, multiple organ failure Adaptive immune responses to extracellular microbes Cellular and Molecular Immunology, 7th ed., 2014 Elservier Mechanisms by which antibodies combat infection Many common diseases are caused by bacterial toxins The four subclasses of IgG have different and complementary functions. Functions of Th17 cells Cellular and Molecular Immunology, 8th ed., 2015 Elservier MECHANISMS OF PROTECTION INNATE IMMUNITY Complement activation Gram (+) Gram (-) peptidoglycan LPS Mannose + MBL alternative pathway alternative pathway lectin pathway Phagocytosis Antibody and complement mediated opsonization Inflammation LPS Peptidoglycan TLR macrophage activation TLR macrophage activation ACQUIRED IMMUNITY Humoral immune response Targets: cell wall antigens and toxins T-independent T-dependent cell wall polysaccharide bacterial protein isotype switching affinity maturation memory B cells Cellular Immune response: Th17 cells Evasion mechanisms of extracellular bacteria Proteins to increase adhesion Bordetella pertussis Inhibition of phagocytosis Str. pneumoniae M protein, S. aureus coagulase enzyme - fibrin capsule Antigenic variants Neisseria gonorrhoeae (pilin) Inhibition of complement-dependent cell lysis Str. pyogenes Sialic acid rich capsule inhibits activation of the alternative complement pathway Some Gram-neg bacteria have a lipidA component that inhibits the MAC complex Scavenging of reactive oxigen intermediates Catalase positive staphylococci Degradation of IgA antibodies Neisseria, H. influenzae Protective immunity against Streptococcus pneumoniae is serotype-specific Bacterial superantigens activate CD4 T cells by cross-linking MHC class II molecules with α:β T-cell receptors and CD28 co-stimulatory molecules in the absence of antigenic peptides Subversion of the immune system by extracellular bacteria Superantigens of staphylococci – staphylococcal enterotoxins (SE) PROFESSIONAL APC 2 2 1 1 – toxic shock syndrom toxin-1 (TSST-1) Mimic specific antigen Induce massive but ineffective T-cell activation and proliferation in the absence of specific peptide 2 – 20% of CD4+ T-cells, which are not specific for the bacteria but share V get activated and develop to effector T-lymphocytes Over production of cytokines – IL-1, IL-2, TNF-α Systemic toxicity – shock T cell Suppression of adaptive immunity by apoptosis Evasion of IgA-mediated defense by staphylococcal superantigen-like protein 7