* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Dr. Ramesh TB Presentation
Clostridium difficile infection wikipedia , lookup
Diagnosis of HIV/AIDS wikipedia , lookup
Meningococcal disease wikipedia , lookup
West Nile fever wikipedia , lookup
Brucellosis wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Sarcocystis wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Marburg virus disease wikipedia , lookup
Trichinosis wikipedia , lookup
Neonatal infection wikipedia , lookup
Chagas disease wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Onchocerciasis wikipedia , lookup
Hepatitis C wikipedia , lookup
Visceral leishmaniasis wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Hepatitis B wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Leptospirosis wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Oesophagostomum wikipedia , lookup
Schistosomiasis wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
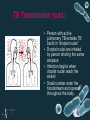
Tuberculosis Update Epidemiology and Prevention Dr. Jaishri Ramesh Alliance Occupational Medicine Objectives • Describe select trends in tuberculosis (TB) incidence in the United States and California • Present select Santa Clara County specific TB data • Discuss TB Transmission • Discuss TB Pathogenesis and clinical presentation – infection vs disease • Describe characteristics that impact TB transmission • The role of TB Control Tuberculosis Etiology • Tupberculosis (TB) , one of the oldest known diseases is still one of the major causes of global mortality. • TB is primarily a bacterial pulmonary disease that has many manifestations, affecting bone, CNS, spinal and many other organ systems. • TB is caused by an acid fast bacteria Mycobaterium tuberculosis • Species: The Mycobacterium tuperculosis complex (MTC) consist of Mycobacterium africanum, Mycobacterium bovis, Mycobacterium canettii, Mycobacterium micotti, Mycobacterium tubersulosis Tuberculosis Epidemiology Key Facts/Global Impact • TB is second only to HIV/AIDS as the greatest killer worldwide due to a single infectious agent. • In 2012, 8.6 million people fell ill with TB and 1.3 million died from TB. • Over 95% of TB deaths occur in low & middle income countries, and it’s among the top three causes of death for women aged 15-44. • In 2012 an estimated 530,000 children became ill with TB + 74,000 HIV negative children died of TB World Health Organization Key Facts/Global Impact (cont.) • TB is a leading killer of people with HIV causing one fifth of all deaths. • Multi drug resistant TB (MDR-TB) is present in virtually all countries surveyed. World Health Organization Key Facts/Global Impact (cont.) Good News! • The estimated number of people falling ill with TB each year is declining, although very slowly which means that the world is on track to achieve the Millennium Development Goal to reverse the spread of TB by 2015. • The TB death rate dropped 45% between 1990 and 2012. • An estimated 22 million lives saved through the use of “Stop TB Strategy” recommended by WHO. World Health Organization Center for Disease Control Tuberculosis (TB) incidence overall and among U.S.- and foreignborn persons, by year — United States, 2000–2015* osis (TB) incidence overall and among U.S.- and foreign-born persons, by year — United States, 2000–2015* Center for Disease Control Center for Disease Control 0 5 0 4,000 1930 1980 1970 1960 1950 1940 8,000 TB Cases California 1985-2015 California Department of Public Health California Department of Public Health Case Rate per 100,000 Number of Tuberculosis Cases and Case Rates: CA, 2004-2013 * Number of Cases Case Rate per 100,000 Population National Case Rate (3.0 per 100,000) California Department of Public Health TB Rates by Racial/Ethnic Group California 2015 California Department of Public Health Trends in TB Cases Santa Clara County 2006-2015 TB Case Rates for California and San Francisco Bay Area Counties 2015 Case #1 • One of our employer contacts for a large company called to state that she received a call from the SCC TB nurse informing her that one of her employees was diagnosed with active TB and that they are in the process of identifying the “contacts” of the Index case who would receive letters from the SCC TB RN to go to Alliance Occupational Medicine for Exposure Protocol. • She called again 1 week later to inform us that 19 contacts (other employees) were identified and would be coming in. • Are these Recordable injuries? TB Transmission How is TB spread? • TB is spread from person to person by inhaling droplets of infected material produced when a person with “contagious” TB exhales forcefully (such as coughing, sneezing, singing, or laughing). • Small children are less likely to transmit the bacteria. TB Transmission (cont.) • Person with active pulmonary TB exhales TB bacilli in “droplet nuclei” • Droplet nuclei are inhaled by person sharing the same airspace • Infection begins when droplet nuclei reach the alveoli • Small number enter the bloodstream and spread throughout the body. TB Pathogenesis • Within 2-10 weeks the immune system intervenes by producing immune cells that surround the bacilli forming a hard shell. (latent TB infection) 30% Latent TB Infection • When a person has Latent TB infection, TB germs in their body are inactive or sleeping. The body’s defenses wall-off the germs and keep them from growing. • A person with Latent TB infection: – – – – Does not feel ill and has no symptoms Is not contagious Usually has a positive TB skin test Usually has a normal chest x-ray TB Pathogenesis • TB disease will develop when the immune system cannot keep the tubercle bacilli under control and they begin to multiply (active TB disease) • TB disease can develop very soon after infection or many years after infection • TB disease may occur in any organ of the body Does everyone who is exposed to TB become infected and get sick? • Approximately 70% of exposed people will NOT become infected. • Approximately 30% of exposed people will become infected. – 5% of infected people will develop TB disease within 1-2 years of infection. – 95% will contain the infection • 5% will get disease later in life • 90% will never develop disease Risk Factors for Progression to Disease: • • • • • • • • HIV infection Injection of illicit drugs Recent infection (within the past 2 years) Chest radiograph findings suggestive of previous TB Diabetes mellitus Silicosis/certain types of cancers Prolonged therapy with corticosteroids Low body weight (10% or more below ideal) TB Pathogenesis Progression to TB Disease TB infection and diabetes TB infection No risk factors TB Disease (10% over a lifetime) TB infection (no TB disease) TB infection (no TB disease) TB infection And HIV TB Disease (30% over a lifetime) TB infection (no TB disease) TB Disease (7-10% per year.) Active TB Disease • When a person has active TB Disease: • The germs in their body have awakened and are multiplying • They may feel sick • They may be contagious • The TB skin test is usually positive • Chest x-ray is usually abnormal • Sputum culture is usually positive. Symptoms of TB Include: • • • • Fatigue Weight loss (unexplained) Loss of appetite Cough - Persistent for 3 weeks or longer • Fever and/or chills • Night sweats What Determines Whether TB Will Spread? Characteristics of the person with TB disease Characteristics of the exposure Characteristics of the person who is exposed The Characteristics of the Person with Disease • Location: Pulmonary (lung) TB is the most common and contagious type of TB • Amount of M. tuberculosis: The more germs in the person’s lung the greater the number of infectious droplets come out when the person coughs. Laboratories can check the sputum under a microscope. If the sputum smear is “positive” for TB bacteria, the person is highly infectious. • Symptoms: coughing. The more a person coughs, the more particles are expelled into the air. Some people with TB have very few symptoms, and are less likely to infect others. The Characteristics of the Exposure • Location of the exposure: Closed rooms without significant air circulation or filtration are the most risky. • Closeness and time: The closer one is physically and the longer the time spent together the more likely transmission will occur. Characteristics of the Person Exposed • Individual factors: some people are more vulnerable to being infected with TB than others. • Prior TB infection: someone who has been previously infected is less likely to become infected from a new exposure Tuberculosis Diagnosis: Tuberculosis Skin Tests • The diagnosis of TB should not be based on the result of a tuberculin skin test • A positive tuberculin skin test only indicates a greater likelihood of TB infection, not necessarily TB disease • A negative tuberculin skin test does not exclude TB. There are many reasons for a false-negative tuberculin skin test TB Blood Tests Interferon – Gamma Release Assays or IGRAs • Measure how the Immune System reacts to Mycobacteria TB • An IGRA measures how strong a person’s immune system reacts to TB bacteria by testing the person’s blood in the laboratory. • 2 IGRAs are approved by FDA in the US. – Quantiferon, TB Gold in tube test (QFT-GIT) – T-Spot, TB test (T-Spot) TB Blood Tests (cont.) • Positive IGRA: This means that the person has been infected with TB bacteria. Additional tests like a CXR are needed to determine if the person has latent TB infection or TB disease. • Negative IGRA: This means that the person’s blood did not react to the test and that latent TB infection or TB disease is not likely. TB Blood Tests (cont.) IGRAS are the preferred method of TB infection testing for the following: • People who have received BCG (Vaccine for TB disease) • People who have a difficult time returning for a 2nd appointment to look for a reaction to the 1st. There is no problem with repeated IGRAs. PRINCIPLES OF TUBERCULOSIS CONTROL Elements of TB Control • Preventing morbidity and mortality from tuberculosis • Preventing transmission/infection • Preventing progression from infection to disease • Surveillance Preventing Morbidity & Mortality • Identifying and treating persons with active or suspected TB disease – Reporting – Case management – Home assessment – DOT Preventing Transmission/Infection • Case finding & prompt treatment of cases/suspects • other – isolation of infectious persons – institutional infection control – minimizing contact – covering cough – personal respiratory protection during contact Prevention of Progression to Disease • Contact Screening – contact investigations – source case investigations – follow through completion of therapy • Population Screening – Class B immigrants – School mandates Surveillance • Uses – monitoring disease trends – targeting prevention efforts – evaluating interventions • Data – # of cases – rates – demographics TB Control Receives Case Reports • All cases and suspect cases must be reported to the local health department (LHD) w/in 1 working day of making or presuming a TB diagnosis • Cases and suspects are assigned to a nurse for case management. INFECTION AND ENVIRONMENTAL CONTROLS FOR TUBERCULOSIS Regulation of Tuberculosis Infection Control • • • • • CDC - Centers for Disease Control OSHA and Cal/OSHA - Occupational Safety and Health Administration OSHPD - Office of Statewide Health Planning and Development ASHRAE - the American Society of Heating, Refrigerating and Air-Conditioning Engineers, Inc. AIA – American Institute of Architects Facilities at Increased Risk of Tuberculosis Transmission • • • • Healthcare Correctional Drug and alcohol treatment Shelters serving homeless and HIV-infected persons Hierarchy of Infection Control Measures • ADMINISTRATIVE CONTROLS to reduce risk of exposure • ENGINEERING CONTROLS to prevent spread and reduce concentration of droplet nuclei • PERSONAL RESPIRATORY PROTECTION in areas where there is increased risk of exposure Administrative Controls • Control infection - Early detection, isolation, and treatment • Prevent the spread of infection, systems to: - Provide respiratory protection - Reduce air contamination • Educate staff, visitors, clients! If you have a COUGH… • PLEASE COVER YOUR MOUTH (Cough into your upper sleeve not your hand) • Ask the receptionist for a MASK Education and Training Cal OSHA requires that workers be trained on: • Signs, symptoms, transmission, risk factors • TB screening and prophylaxis for latent TB infection (LTBI) • Engineering and work practice controls • Personal protective equipment, use and limitations • Employer and employee responsibilities for reducing risk of TB • Employees must have the opportunity to ask questions at the training Engineering Controls The Engineering Model Patient emits infectious droplets which float in the air indefinitely unless removed or killed Clean Air In Contaminated Air Out Engineering Controls Contain contaminated air : • Negative pressure rooms, sputum induction booths Reduce concentration of infectious droplet nuclei: • Dilution ventilation • HEPA filters • UV fixtures Direct Flow of Air • Introduce air near staff • Exhaust near patient Clean Air In Contaminated Air Out Dilution Ventilation • Supplies clean air • Mixes with room air • Exhausts contaminated air • One room air change removes 63% of droplets, if mixing is perfect • Six air changes per hour (ACH) removes 99.9% of droplets in 69 minutes Dilution Ventilation Effectiveness • Maximize air changes • Optimize room air mixing • Direct flow of air – Over staff – Across patient – Then exhaust Contaminated Return Air • Exhaust directly to atmosphere away from air intakes (25 ft) • Use HEPA filtration if air is re-circulated High Efficiency Particulate Air (HEPA) Filters • Removes 99.97% of 0.3 µm particles • Used to clean air before: – Recirculation to other parts of facility – Recirculation to same room – Exhaust to atmosphere Personal Protective Equipment An Effective Respirator for Tuberculosis • Filters particles of 1 micrometer with an efficiency of 95% (NIOSH, 95% = N 95) • Comes in various sizes and shapes to fit different faces An Effective Tuberculosis Mask WORKS When… • There is a correct fit • The mask is conscientiously placed • The mask is given proper care How do we assure that these essential elements are met? What To Do? • Call Public Health early • Allay fears/anxiety – Education/Information – Refer to PMD if necessary • Above all, maintain patient confidentiality Protocol for Evaluation & Treatment of TB Exposure • • • • Initial Evaluation – History & Physical TB test – PPD or IGRA CXR if positive TB test Repeat TB test if initial test negative 10-12 weeks • CXR if 2nd test positive • Evaluation for latent TB treatment Any Questions? Thank you! Dr. Jaishri Ramesh Alliance Occupational Medicine 1901 Monterey Rd. San Jose, CA. 95112 2737 Walsh Ave. Santa Clara, CA. 95054 315 S. Abbott Ave. Milpitas, CA. 95035 [email protected] (408) 228-8400