* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Pain management case studies Pharmacy
Survey
Document related concepts
Prescription costs wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Environmental persistent pharmaceutical pollutant wikipedia , lookup
Toxicodynamics wikipedia , lookup
Pharmacognosy wikipedia , lookup
Drug interaction wikipedia , lookup
Paracetamol wikipedia , lookup
Patent medicine wikipedia , lookup
Neuropharmacology wikipedia , lookup
Serotonin syndrome wikipedia , lookup
Psychopharmacology wikipedia , lookup
Transcript
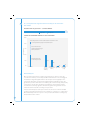
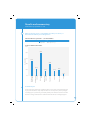
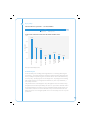
Pain management case studies Pharmacy ACC case studies no. 1 and 2 – November 2009 Produced by the Provider Engagement & Performance Unit, Health Purchasing & Provider Relationships, ACC. This case study has been recognised by the NZCP for continuing education points for their pharmacist members. The opinions expressed in this document are not necessarily the official views of ACC. Date of study: December 2008/January 2009 Date of report: November 2009 © ACC 2009 All rights reserved. No part of this document may be reproduced in any form without written permission from ACC. Contents Case study 1 – Ankle Sprain • Vignette 2 • Background 3 • Results and commentary 5 • Additional vignette information 1 13 • Additional vignette information 2 14 Case study 2 – Back Pain 22 • Vignette 22 • Background 23 • Results and commentary 25 Commentators The commentary for these case studies is kindly provided by: Cases 1, 2 Dr Linda Bryant Clinical Advisory Pharmacist Comprehensive Pharmaceutical Solutions Dr Evan Begg Professor of Clinical Pharmacology/Medicine University of Otago, Christchurch Acknowledgements: ACC would like to acknowledge the assistance of: The Members of the ACC Pharmaceutical Sector Liaison Group The New Zealand College of Pharmacists 1 Case Study 1 – Ankle sprain Vignette Mrs Smith is a 75-year-old widow who hobbles in looking somewhat bruised and battered and with plasters on her skinned hand, elbow and knee. Her ankle is slightly swollen and tender, although it has reasonable movement. She says she tripped about an hour ago when she misjudged the culvert outside her house and “made a right mess” of herself. She is feeling a bit sore and her ankle is painful; however, she has been to her general practice and been assured that it is just a sprain. As her daughter is visiting this weekend (three days away) and wants to take her to the garden show, she wants something to help her ankle and mobility. You know Mrs Smith and have a record of her prescriptions. She takes: Bendrofluazide 2.5mg mane hypertension Cilazapril 5mg mane hypertension, heart failure Frusemide 80mg mane heart failure Metoprolol CR 95mg mane hypertension, post MI, heart failure Aspirin 100mg mane cardiovascular disease Felodipine ER 10mg mane hypertension Simvastatin 40mg nocte cardiovascular disease Zopiclone 11.25mg nocte sleep, especially since husband died 18 months ago Amitriptyline 25mg nocte unsure, but seems to help sleep Omeprazole 10mg mane GORD Lactulose 10 – 20ml prn constipation Paracetamol 1g prn osteoarthritis of the knee Mrs Smith tells you her blood pressure is very good – just like a young person’s, at about 120/70mmHg or less. She does get a little dizzy at times, so doesn’t want anything that might make her “fuzzy”. 2 Background Dr Linda Bryant Mrs Smith is one of those people for whom medicines have accumulated over time. Sometimes this occurs because there is a view that she is doing well and ‘don’t fix what ain’t broke’. Sometimes this is exacerbated by a focus on risk factors such as for cardiovascular events, and an attitude of ‘the lower the better’, which is not necessarily the case for older people. People like Mrs Smith may present well, but often will not readily mention some symptoms such as the dizziness and the falls because perhaps she considers that this is a part of growing old. Unfortunately this means that medicines may not be reviewed as they should and, as the person ages, the dosages become excessive, and some medicines may not be necessary any more. An outcome of this is the increased risk of falls. While falls may result in non-fracture injuries such as head injuries and lacerations, any internal injury, hip fractures in particular, can have a major detrimental impact on the person’s mobility, independence, quality of life, general health status and financial situation.1 Studies show that 17% of post-menopausal women are likely to suffer a hip fracture. Of these there is a 10% early mortality, with 20% to 33% dying over the following 12 months.2, 3, 4 Morbidity is also high. Fifty per cent of women with a fractured hip are unlikely to ever walk without assistance, and 25% will require long-term care.4, 5 Falls prevention is an issue that all pharmacists should be aware of. The ACC website (www.acc.co.nz) has more information and resources regarding falls prevention, as does the falls prevention strategy website.6 For Mrs Smith, the acute situation needs to be addressed – both the pain and her concern about the time she is looking forward to spending with her daughter. Then there is the rehabilitation time to be considered, and, in the longer term, prevention of recurrence. Dr Evan Begg This is a not uncommon scenario of an elderly woman, presumably living alone, who has tripped and fallen and has a ‘sprained ankle’. She has had another recent fall, has been dizzy at times, and has a low recorded BP at present (for her age). Her past history includes hypertension, CHF and an MI, for which she is on lots of medicines (polypharmacy). Constipation and an apparent requirement for zopiclone and amitriptyline complete a typical picture of prescribing for the elderly. This case study illustrates both an acute management situation and opportunity for future medicines rationalisation and falls prevention. 3 1. Manage the acute problem: • make sure any wounds are clean and protected • re-examine the ankle to make sure the GP diagnosis of ‘sprain’ is fair, or whether it needs further investigation (X-ray) • advise RICE, +/- physiotherapy or graded exercise plan (to stop stiffness and to avoid DVT) • analgesia – paracetamol +/- codeine +/- low-dose NSAID • manage expectation of going to garden show in three days (or not!). 2. Some reasons for the acute problem: • postural hypotension – too much antihypertensive medication • background zopiclone and amitriptyline • probable variable compliance (everyone on this number of drugs is subject to variable compliance). 3. Rationalise her current therapy and prevention of falls recurrence: 4 • assess/avoid/handle postural hypotension • is her home dangerous for falls (e.g. two-storied) • reduce/rationalise drugs for hypertension – discuss with GP • reduce other drugs if possible (e.g. does she need simvastatin, zopiclone, amitriptyline?) • attempt to withdraw zopiclone and amitriptyline in the long term – discuss with client/GP • avoid constipating drugs (e.g. amitriptyline and felodipine). Codeine will add to this problem • consider providing compliance aids – yellow card, pill organiser • provide medicine education – patient information leaflets/pharmacy counselling. Results and commentary Total number of respondents n = 286 1 As there is no fracture, what non-pharmacological advice would you give Mrs Smith? response rate to question 1 – % of respondents 100% Responded No response non-pharmacological advice – % of respondents 48% 49% RICE RICE plus other 3% Other Dr Linda Bryant It is good to see virtually everyone advised RICE, and of the almost 50% who provided further advice, there was a focus on Mrs Smith and her desire to attend the garden show, and an indication of when to return to the general practitioner if there was no improvement within 48 hours or a worsening of pain. Some people added the ‘P’ to RICE, recommending Protection such as an ankle support, which is also helpful. With three days before the garden show, Mrs Smith had an opportunity to rest her ankle and elevate it (ankle above her knee, above her hip). It would certainly have been a good idea for her to use at least a walking stick for the garden show – or even a wheelchair as was suggested, if it was a large garden show (three to four hours on her feet). For rehabilitation, Mrs Smith should also slowly improve her range of movement with gentle pointing and flexing of her foot. Being 75, Mrs Smith can lose condition (strength, balance, range of movement) very quickly, which increases her risk of further falls and injury. She needs to have a balance between RICE for two to three days and resuming gentle activity/muscle strengthening, as well as maintaining cardiovascular health. It is also important to remember that fear of falling is a risk factor for falling – and Mrs Smith may have felt somewhat shocked and lost confidence. This is something to check on in terms of Mrs Smith’s progress. A mild sprain requires about two to six weeks before a return to full activity and a moderate sprain may take two to three months. Mrs Smith’s activity level should be monitored. The Pharmaceutical Society of New Zealand Self Care fact cards on Pain Relief and Arthritis are very useful and provide good information, particularly as, in the acute period when Mrs Smith may be a little ‘shaky’, she may not remember all your advice. 5 Table 1 and Chart 1 summarise the additional advice provided by respondents who also recommended RICE. table 1 RICE plus other 49.3% Physical support Pain mitigation strategies 16.4% Use walking stick/crutches/hire wheelchair/postpone garden visit 15.4% Wear ankle support/ankle brace/support stockings 8.0% Gentle massage/gentle movements involving ankle 7.3% Rub Voltaren Emulgel/Antiflamme/Arnica on ankle for swelling/bruising 2.8% Regular paracetamol/increase paracetamol for pain relief 4.2% Local treatment/(moist) heat/vibration treatment/ physiotherapy/ drink plenty of fluids 5.6% Falls prevention measures/self-care card on sprains and strains/sensible shoes 7.3% Review after couple of days of RICE – if worse go to doctor/ physiotherapist 7.3% Avoid Heat, Alcohol, Running, Massage (H.A.R.M.) 4.2% Attend to skinned hand, elbow and knee/prevent infection of grazes/abrasions 3.8% Suggest vision/glasses check by optometrist/BP check/ medications review/mention dizziness to GP Informational advice Other chart 1: rice and other responses 40% % of respondents 30% 15.4% 4.2% 20% 2.8% 3.8% 7.3% 10% 7.3% 4.2% 5.6% 7.3% 16.4% 8.0% 0% Physical support Pain mitigation strategies Note: Graph includes multiple answers. 6 Informational advice Other Dr Evan Begg Nearly everyone got the correct response – RICE, with very useful and varied supportive suggestions. Good point about a wheelchair for the garden show, as clearly her predisposition to falling will not have been alleviated by then. It would be wise to counsel her that if she does not feel well enough, she may not be able to attend the show. A slow and deliberate mobilisation strategy would also be helpful. 2 Would you recommend any pharmacological treatment to Mrs Smith? response rate to question 2 – % of respondents 100% Responded No response Recommend pharmacolgical treatment – % of respondents 92% Yes 8% No Dr Linda Bryant Yes, the option of having pharmacological treatment available is important, as almost every respondent indicated. Some people are particularly stoic but it is important to assure Mrs Smith that pain relief is important, both acutely and when she is ‘rehabilitating’. There is no benefit in being stoic and suffering unnecessary pain. It is usually negotiating the choice of pain relief that is the issue. Dr Evan Begg It was no surprise to see that nearly 100% of pharmacists wanted her to have some analgesia. This is appropriate. 7 3 If so, what pharmacological treatment would you recommend to Mrs Smith? response rate to question 3 – % of respondents 92% 8% Responded No response chart2: recommended pharmacological treatment 100% 1% Possibly Panadeine®/codeine but with catution/no Panadeine®/codeine 6% Take paracetamol/possibly codeine but with caution % of respondents 80% 60% 40% Continue/increase/ maximise paracetamol usage/ take her paracetamol 40% 20% 41% Take paracetamol/ recommend paracetamol 39% 22% 0% Oral meds Topical products (including NSAIDs) 3% Oral NSAIDs Vitamin (avoid/take with supplement caution) 6% Additional information sought Dr Linda Bryant Over one-third of pharmacists opted for paracetamol alone, which is a very safe, cost-effective medicine, and it is likely that Mrs Smith will have some at home (given her medication list). Getting Mrs Smith to take the paracetamol regularly for two to three days will need to be negotiated. Suggesting that it will help her get to the garden show, and she will be less ‘worn down’ by pain and broken sleep, will probably convince her to try this. She should be assured that she only needs this intensity of treatment for a few days (at least until after the garden show) and then she can reduce the number of tablets according to her pain level. Some recommended paracetamol plus codeine. The amount of codeine in the OTC products is generally suboptimal, and can contribute to constipation, a condition that Mrs Smith already seems to be prone to. The potential adverse effects outweigh any extra benefit from the codeine. 8 About one in five pharmacists suggested using an oral NSAID, with some stipulating with caution. Some specified to avoid completely. With the risk of exacerbating heart failure and the ‘triple whammy’ (an ACE inhibitor + a diuretic + an NSAID)7 increasing the risk of renal dysfunction, an NSAID should be avoided completely unless pain is severe, in which case a general practitioner would be best to manage the potential adverse effects by undertaking close monitoring of renal function and heart failure. There is some debate about the use of NSAIDs in muscle injuries and little good quality evidence of any benefit above regular paracetamol use, particularly for mild to moderate sprains. There is also continuing debate about the use of NSAIDs immediately after an acute injury, such as a sprain, inhibiting the role prostaglandins have in helping healing.8 For Mrs Smith the risks would outweigh any potential extra benefit over paracetamol. Topical NSAIDs can be effective and safe as pain relief for sprains, but there is a financial cost associated with this. Regular paracetamol dosing will provide similar analgesia. There were some recommendations for vitamin supplements. Vitamin D (colecalciferol) is the important vitamin for reducing fracture risk in the older person because as skin ages it is unable to absorb/convert sunlight to Vitamin D3 as efficiently as young skin. The Auckland Bone Clinic recommends that people over 70 years receive Vitamin D. It is important to note that the dosage required is around 50,000iu (1.25mg) monthly, which requires a prescription. The following venn diagram shows the overlap of pharmacological treatment recommended by respondents. venn diagram 1: recommended pharmacological treatments Oral meds 119 (45.6%) 60 (23.0%) 35 16 (13.4%) (6.1%) Topical products 23 (8.8%) Oral NSAIDs 4 4 (1.5%) (1.5%) 9 Dr Evan Begg Most respondents wanted to optimise paracetamol use. Recent FDA arguments9 have been to reduce paracetamol dosing in the elderly, rather than follow the usual 4gm per day for everyone. Her paracetamol clearance may be about half that of a 30 year old, so doses may need to reflect this (e.g. 500mg q6h). The New South Wales Therapeutic Group Inc. has developed paracetamol use guidelines for in-hospital use. These may be relevant to the community setting when determining dosing.10 Only a few (<6%) wanted to prescribe codeine in addition, and if so, with caution. It would be useful to avoid codeine, considering her constipation, which might be worse with immobility over the next few days. It was interesting also that most respondents wanted to avoid NSAIDS. This is rational on the surface (aggravation of BP and CHF, and the problems when given with ACE inhibitor + two diuretics) but probably unnecessarily cautious, since she is currently being overdiuresed, overtreated for hypertension, and having seriously symptomatic postural hypotension. A few days of a low-dose NSAID (e.g. diclofenac 25mg bd or ibuprofen 200mg tds) in this situation is likely to assist the paracetamol and avoid the need for codeine, and may even improve the postural hypotension. The background omeprazole should cover GI worries also. It all depends on the seriousness of the pain. If serious, then an NSAID might need to be considered (and she should not contemplate attending the garden show). The recommendations of a few regarding vitamin supplements are probably useful to consider for the long term. 10 4 Why would you recommend this treatment? response rate to question 4 – % of respondents 92% 8% Responded No response The following venn diagrams show the overlap of why the pharmacological treatment was recommended. venn diagram 2: Why oral meds were recommended Effective treatment 61 (26.5%) 12 45 (19.6%) 37 (5.2%) (16.1%) Safe treatment 34 (14.8%) 37 To prevent adverse events 4 (16.4%) (1.7%) venn diagram 3: Why topical products were recommended Effective treatment 32 (31.1%) 35 (34.0%) 2 14 (1.9%) (13.6%) Safe treatment 9 (8.7%) 10 To prevent adverse events 1 (9.7%) (1.0%) 11 venn diagram 4: Why Oral NSAIDs were recommended Effective treatment 21 (35.6%) 6 (10.2%) 5 10 (8.5%) (16.9%) Safe treatment 9 (15.3%) 6 To prevent adverse events 2 (10.2%) (3.4%) Dr Linda Bryant The rationale for selecting a particular medicine, noted by the majority of respondents, included good consideration of the safety of the medicine, and avoidance of adverse effects. These are suitable considerations when balancing the risk-benefit of a treatment. Being 75 years old and on multiple medicines, Mrs Smith is at a high risk of adverse effects and medicine interactions. Her cardiovascular condition, particularly her heart failure, is at increased risk of exacerbation with NSAIDs. She also appears to be prone to constipation (lactulose) and her zopiclone and amitriptyline may make her more prone to the CNS effects of codeine. There is also a need to consider the financial situation of a 75-year-old woman and, along with safety and effectiveness, cost-effectiveness of treatment needs to be considered. Dr Evan Begg This is a typical cost-benefit situation, as most respondents have noted. Overall it is likely that optimising paracetamol, in the setting of RICE, will probably be adequate for pain relief. If more analgesia is required, then a couple of days of a low dose of a low-toxicity NSAID (ibuprofen or diclofenac) would be better tolerated than codeine. 12 Additional vignette information 1 During the course of your conversation Mrs Smith tells you that she also had quite a nasty fall a few months ago. Again, she did not fracture anything as a result of this incident, but did end up with a number of bruises. What non-pharmacological advice would you now give Mrs Smith given that this is not the first time she has had a fall? (Hint: look at ACC website for information on falls prevention and referral into the Tai Chi programmes on www.acc.co.nz) response rate to question 5 – % of respondents 99.7% Responded No response 0.3% chart 3: response themes 100% 91.6% 80% 63.5% % of respondents 5 60% 49.1% 40% 33.3% 20% 4.9% 1.4% 0% Exercise Preventive care Health management Home safety Nutrition Self-monitoring Dr Linda Bryant For older people, poor nutrition, lack of mobility and social isolation appear to herald the start of a relatively rapid deterioration. The advice to promote activities such as Tai Chi is excellent, as it provides not only good learning to help prevent falls, but also an opportunity for socialisation. (People at home alone for more than 16 hours per day and who lack a social network have an increased risk of falling.) 13 Checking the environment is important (ACC pamphlets are available at www. acc.co.nz), as well as checking for possible visual and hearing loss issues. It is also important to recognise that the fear of falling is a high risk factor for a fall (20% to 40% of older people who haven’t fallen have a fear of falling; 40% to 70% of older people who have fallen have a fear of falling).11, 12 Dr Evan Begg Falls are probably the key problem for Mrs Smith, and can be disastrous in this age group. Her polypharmacy in this context is therefore of some concern, and there may be opportunity to review her current medicines use. This question was generally handled well, in terms of fall prevention, environmental awareness, and exercise. Perhaps more elaboration as to the why and what sort of exercise would have been helpful (i.e. all gentle, with slow strengthening, and assisted (physio) in the early phases). However, any advice re exercise and exercise programmes needs to be tempered by an assessment as to the likely adherence. Mrs Smith has had 75 years establishing her behaviour pattern, and she is unlikely to adopt any radical change, so any change will need to be introduced slowly and be well supported. Simplifying her medication to avoid postural hypotension would also be a priority at this stage. Additional vignette information 2 Mrs Smith says she sometimes has trouble remembering to take her medicines and is interested in your medicine use (compliance) review service. She understands that you will send a report of her review to her general practitioner and agrees for you to undertake a medicine use review for her. 14 What are some questions you would want to ask with respect to adherence to this medication regimen? response rate to question 6 – % of respondents 99.3% Responded No response 0.7% chart 4: adherence themes 100% 78.5% 80% 58.8% 60% 28.9% 29.9% 29.2% Other 40% Compliance aids % of respondents 20% 10.6% Vision Dose form suitability Dosage times/suitability (time to take) 0% Medicines knowledge (extra/excess medicines is a subset) 12.3% Effectiveness/AE 6 Dr Linda Bryant Respondents covered this well and the questions asked, particularly around potential adverse effects (drowsiness, dizziness) and the perceived effectiveness or necessity (zopiclone, frusemide), indicated concerns about some of the medicines potentially increasing the risk of falls. There was also concern about the need to take, and accuracy of taking, so many medicines. With blood pressure being relatively low (query heart rate), and concerns about dizziness, the considerations about the need for all the blood pressure lowering 15 medicines were raised. With heart failure requiring the ACE inhibitor and -blocker, the felodipine could be reduced/stopped, and perhaps the cilazapril and thiazide combined in one tablet (Inhibace Plus®) to reduce the number of medicines and reduce the risk of medicine being taken incorrectly. Similarly, when pursuing the taking of medicines, the continued need for frusemide at 80mg should also be considered. The other area of questioning regarding knowledge or effectiveness of medicines concerned zopiclone and amitriptyline, with concern that sedatives (especially when combined) increase the risk of falls. Amitriptyline can cause postural hypotension and possible blurred vision, which are also contributing factors. It can also contribute to constipation. The 78.5% of respondents who provided dosage times/suitability (time to take) as a response also provided responses as outlined in Table 2. table 2 Dosage times/suitability (time to take) % Effectiveness/AE 23.2 Medicines knowledge (extra/excess medicines is a subset) 45.1 Dose form suitability 9.2 Vision 7.8 Compliance aids 20.8 Other 20.8 Note: Table contains multiple answers. Dr Evan Begg Discussion of dosing times, while very useful, seemed to be considered more important by respondents than reducing the number of medications (although this may have been assumed within medicine rationalisation). It would be useful to assess her ideas about why she was falling so often, and whether she thought she needed all the medication. There is a lot of pressure (e.g. in some guidelines for antihypertensive and statin use) to prescribe medicines for small reductions in absolute risk, which become somewhat meaningless if the patient suffers adverse consequences from complications of a fall (e.g. DVT). It would be useful to enquire about whether she has had or been offered compliance aids such as yellow cards, pill organisers, and patient information leaflets. These should be discussed. The problem of zopiclone ‘addiction’ and amitriptyline use might have been raised, along with acknowledging the difficulty in removing these. In terms of dosing times, compliance is best with once daily dosing, and nearly as good with twice daily dosing. Dosing more frequently is associated with a marked fall-off in compliance. In the elderly, the half-life of most drugs is prolonged, which often allows dosing that is tds or qid in younger patients to be changed to bd or od. 16 What outcomes would you expect to achieve by improving her adherence? response rate to question 7 – % of respondents 99.3% Responded No response 0.7% chart 5: Responses by theme 100% 80% 71.5% 68.3% % of respondents 60% 40% 32.0% 31.7% 20% 8.8% 8.5% Other Compliance aid Improved medicines knowledge Falls prevention Meds rationalisation 0% QOL improvement 3.9% Chornic condition improvement 7 Dr Linda Bryant The ultimate goal is an improvement in health-related quality of life for people, although this is difficult to measure routinely. Improvement in adherence, as respondents indicated, should improve the control of chronic conditions (cardiovascular disease/heart failure, osteoarthritis), and reduce falls, which can have a high negative impact on quality of life. These outcomes would be achieved through the rationalisation of medicines and improved knowledge of medicines and how to use them appropriately. 17 venn diagram 5: Overlap of two main themes by respondents Chronic condition improvement 68 (25.1%) 126 (46.5%) Meds rationalisation 77 (28.4%) Dr Evan Begg Her medications could probably be reduced (not too abruptly) by about half, with obvious improvements in compliance and well-being. She should feel improvement in terms of decreased postural hypotension from stopping felodipine, as blood pressure effects from this relate almost immediately to blood concentrations. Similarly, removing one of the diuretics would decrease the postural hypotension. This would probably be best achieved by removing the thiazide, and halving the dose of frusemide. It would probably be too much for her to have the amitriptyline stopped at this stage since she will be cherishing sleep. It would be very useful to have discussions with the GP on the various options for simplifying her therapy, particularly with regard to postural hypotension. 18 8 How would you measure whether those outcomes were achieved? response rate to question 8 – % of respondents 99% Responded No response 1% Table 3 # % 68 25.1 Chronic condition improvement 49 72.1 QOL improvement 24 35.3 Meds rationalisation 29 42.6 Falls prevention 29 57.4 Dispensing patterns 17 25.0 Improved medicines knowledge 1 1.5 Compliance aid 3 4.4 Other 8 11.8 77 28.4 Chronic condition improvement 35 45.5 QOL improvement 27 35.1 Meds rationalisation 42 54.5 Falls prevention 23 29.9 Dispensing patterns 20 26.0 Improved medicines knowledge 5 6.5 Compliance aid 4 5.2 Other 5 6.5 126 46.5 Chronic condition improvement 95 75.4 QOL improvement 58 46.0 Meds rationalisation 59 46.8 Falls prevention 51 40.5 Dispensing patterns 37 29.4 Improved medicines knowledge 7 5.6 Compliance aid 5 4.0 Other 13 10.3 Q7: Chronic condition improvement theme Q8 Theme Q7: Meds rationalisation Q8 Theme Q7: Chronic condition improvement theme and meds rationalisation Q8 Theme Note: Table includes multiple answers. Note: The Q7 headings link back to venn diagram 5. 19 Dr Linda Bryant When considering a service, the question after “What outcomes do we expect to achieve?” is “So, how do we know we have achieved the expected outcomes?”. Evaluation of a service is important for sustainability. Measuring the quality of life for an individual (as opposed to a study population) is difficult and time consuming. While disease-specific instruments (heart failure, asthma, etc) may be more amenable to measuring change, they are too specific for multiple co-morbidity use. For Mrs Smith, quality of life would be more specific to her own goals, such as attending the garden show. To monitor the impact of our intervention we would expect that Mrs Smith would be comfortable with any changes made to her medicines (i.e. reduced pain, reasonable sleep, less dizziness), would have improved adherence (monitor collection) and would have fewer falls (an objective measure). There is no mention of previous hospitalisations, but there would be an expectation that improvement in her medicines (choice and use) would help prevent hospitalisations, though this is difficult to compare without a randomised controlled study. Clinical indicators (e.g. blood pressure, HbA1c, lipid profile, etc) should be in the optimal ranges for this client. Dr Evan Begg Respondents recognised that there is much that can be done to improve her overall well-being, and in particular to decrease the likelihood of recurrence of her falls. A controlled plan for her rehabilitation, and her medicine rationalisation, will need a multidisciplinary approach. This will involve the GP (medicine and dose adjustments), practice nurse (BP monitoring, and compliance aids and counselling), physiotherapist (immediate management and future proofing), pharmacist (compliance aids and counselling, attendance to dexterity related to pill bottles) and occupational therapist (home visit and fall avoidance procedures). Involvement of a family member/friend could also be very fruitful. Effectiveness will be ‘measured’ as usual in follow-up visits. She is likely to report greater well-being, less postural hypotension and fewer falls. 20 Bibliography ACC Falls Prevention Strategy 2005 - 2015. http://www.acc.co.nz/preventing-injuries/injury-prevention-strategies/PI00132 Best Practice Advocacy Centre (BPAC) Polypharmacy POEM. May 2006. http://www.bpac.org.nz/resources/campaign/polypharmacy/polypharm_poem.asp Prevention of Hip Fracture Amongst People Aged 65 Years and Over. June 2003. New Zealand Guidelines Group. http://www.nzgg.org.nz/guidelines/dsp_guideline_popup.cfm?&guidelineID=6 References 1. Norton R, Butler M, Robinson E, Lee-Joe T, Campbell AJ. Declines in physical functioning attributable to hip fracture among older people: a follow up study of case-control participants. Disability and Rehabilitation 2000; 22:345-351. 2. Norton D, Measday J, Grenfell R, Mackay C, Teed A, Macdonald C. GPpharmacist liaison: a rural case study. Australian Family Physician 2003; 32(3):191-192. 3. Keene G, Parker M, Pryor G. Mortality and morbidity after hip fracture. BMJ 1993; 307:1248-1250. 4. Riggs B, Melton L. The worldwide problem of osteoporosis: insights afforded by epidemiology. Bone 1995; 307(Suppl):505-511s. 5. Ryan P, Blake G, Fogelman I. Postmenopausal screening for osteopenia. British Journal of Rheumatology 1992; 31:823-828. 6. http://www.acc.co.nz/preventing-injuries/injury-prevention-strategies/ PI00132 7. Savage, R. A dangerous trio. Prescriber Update June 2002. http://www.medsafe.govt.nz/profs/PUarticles/DangTrio.htm 8. Braund R, Abbott JH. Analgesic choice when treating musculoskeletal sprains and strains. New Zealand Journal of Physiotherapy 2007; 35: 54-60. http://www.physiotherapy.org.nz/index02/Publications/.../35(2)p54-60.pdf 9. 30 June 2009 – www.time.com/time/health/article/0,8599,1908042,00.html 10. December 2008 http://www.ciap.health.nsw.gov.au/nswtag/publications/ posstats/Paracetamol231208.pdf 11. Boyd R, Stevens JA. Falls and fear of falling: burden, beliefs and behaviours. Age and Ageing 2009; 38:423-438. 12. Scheffer AC, Schuurmans MJ, van Dijk N, van der Hooft T, de Rooij SE. Fear of falling: measurement strategy, prevalence, risk factors and consequences among older persons. Age and Ageing 2008; 37:19-24. 21 Case Study 2 – Back pain Vignette Mrs Jones is a relatively new patient to your pharmacy. She is a 35-year-old laboratory technologist, but having had chronic back pain for nine months now has meant that she is unable to work more than three to four hours a day. Mrs Jones has been to the chronic pain clinic at the hospital. Her current medicines are: Amitriptyline 10mg daily neuropathic pain Paroxetine 30mg mane depression Tramadol Up to 100mg three times daily prn neuropathic pain Paradex® 2 tablets prn neuropathic pain Sumatriptan 50mg as required migraine Paramax® 2 prn migraine Mrs Jones generally takes two tablets (50mg) of tramadol when she gets up every morning. About twice a week she also takes two tablets in the late afternoon – though she tries to avoid these as she has heard that they are narcotics. She also takes two tablets of Paradex® most nights. Sumatriptan is taken about once every two weeks as required for migraines, and Paramax® about twice a week if she thinks she’s getting a migraine, and they often work. Mrs Jones says that she thinks she is doing fairly well and wants to extend her work hours. Her GP told her that there is another drug she could use for pain (gabapentin) and she wishes to know more about it. Her general health is fine in terms of blood pressure, etc. 22 Background Dr Linda Bryant Chronic pain is a very difficult condition to treat, and there is a lot of misunderstanding about this condition, with some public perception that this is ‘malingering’.13 Yet it is a very real and devastating condition. Because of the complexity of the condition it is often treated through a chronic pain clinic, which is a specialised clinic with a strong interdisciplinary focus. As well as the medical pain specialist, the team usually includes specialist nurses, clinical psychologists, physiotherapists, and good connections with social services. The treatment is very much individualised (pharmacological and non-pharmacological), and sometimes the combination of medicines is very complex. The impact of chronic pain on a person’s lifestyle and functioning is often dramatic and extensive. There is a need for clear communication among the healthcare providers and identification of the lead provider for care relating to the chronic pain, to avoid mixed messages occurring. It appears that Mrs Jones is doing well, as she says herself, but that she is eager to “do even better”, perhaps pushing herself. Having progressed this well, and looking to change something, it is probably timely for the team that individualised her treatment to review it, because, as the respondents to the case study indicated, this combination of conditions and medicines will need as much care and monitoring to change as it probably took to reach. Dr Evan Begg This is a problem of a relatively young working (professional) woman (aged 35) with chronic back pain, migraines and background depression. She has (appropriately) been referred to the chronic pain clinic, and is now on multiple medications affecting the CNS. Paradoxically, she is enquiring about a possible additional drug for neuropathic pain, yet feels she is currently doing well. Overall this is far more a diagnostic problem than a simple medicines rationalisation. It is most likely that one of her three neuropsychiatric problems is dominant, and the others of varying importance. Once this is clarified, simplifying the medications should be the aim. 1. The fundamental problems: • chronic back pain: Information is needed on timing of onset, aggravating and alleviating features, diagnosis and how firm this is, investigations, and response or otherwise to the different medicines 23 • migraine: There is little information about her migraine history. This is likely to have been a much more chronic problem than the back pain, and the current frequency of attacks is worrying • depression: Again there is little information. Is this the fundamental problem? Maybe her psychiatrist should be more involved? • psychosocial setting: Is there a reason for a general inability to cope? • work setting: Is this aggravating all of the above? 2. Polypharmacy: 24 • her medications have an effect on most central neurotransmitters, making predictability of effect very difficult • her multiple interactions make it very difficult for this to be simply embraced, in the setting of much that is unknown about the primary problems • she is interested in the new drug (gabapentin) mentioned by her GP. Results and commentary Total number of respondents n = 280 What are the key areas you would question Mrs Jones about, to determine the advice you would give her? response rate to question 1 – % of respondents 99.3% Responded No response 0.7% chart 6: Thematic responses 100% 81.3% 80% % of respondents 60% 54.0% 42.1% 40% 25.9% 19.1% 20% 19.1% 21.2% Allergies Migraine oriented Comorbidity Exercise/lifestyle Alternative advice/ support sought Meds oriented queries 0% Activities that impact on back pain 5.8% Back pain severity, location, regularity 1 Dr Linda Bryant As the majority of pharmacists suggested, there is a necessity to determine the type of pain, how much it has improved, over what sort of time period, and any changes in activity types or pain levels, particularly as Mrs Jones indicates that she considers that she is doing so well that she could extend her work hours. Noting changes to 25 medicines use, such as a reduction in her use of prn analgesia, would help establish any variability in pain levels. A check on any changes in frequency or intensity of her migraines and whether her response to her migraine medication remained stable would also be helpful. Although it seems that Mrs Jones is doing well (wanting to increase her work hours) I would be interested in any comments she makes about symptoms that could indicate possible serotonin toxicity (muscle weakness, hyperreflexia, lack of coordination, shivering, fever, chills, sweats, irritability, raised body temperature, nausea, abdominal cramps, tachycardia, headache, hypo- or hypertension and CNS symptoms). From the improvement Mrs Jones has indicated she is experiencing, exploring her knowledge of the dosing of the medicines, and her views on her medicines’ effectiveness and potential adverse effects, would be useful to try and understand why, beyond her mentioning it, she is interested in gabapentin, particularly when she appears to be ready to extend her work hours. It may be that she is comfortable with her current treatment and is trying to balance the option of changing medicines against staying with a treatment that is working for her. I would be interested in what other medicines had been tried, including complementary medicines. This is because I note that Mrs Jones had been to the chronic pain team, and I am aware that these teams are usually fairly conservative and do not initiate ‘complex’ regimes without having first tried the more straightforward regimes. I would also ask about non-pharmacological methods of pain control, and check whether/when Mrs Jones had her next appointment with the chronic pain team. Mrs Jones has indicated that she is primarily using regular amitriptyline (10mg nocte), Paradex® (2 nocte) and tramadol (100mg mane) for pain, with an occasional extra two tramadol in the late afternoon about twice a week. Dr Evan Begg As correctly noted by nearly all respondents, multiple themes emerge. The order of batting in this regard was medicine queries (81%), back pain (54%), exercise/lifestyle (42%), and others (around 20% to 25%). To me the fundamental nature of the three underlying complaints needs to be resolved, and more attention needs to be paid to the migraines and depression. Certainly the migraines seem to be a larger current problem than the back pain, and the depression may be in a quiescent phase (as she is keen to increase her working hours). The setting of this case, however, biases us towards the back pain. Having elucidated more about the problems, a full medicines history (extending far earlier than nine months) would be useful to try to identify drugs she likes/dislikes, and whether she generally likes to rely on medicines or not. This raises further questions about other lifestyle cures and alternative medicines. We need to know a lot more about where she is coming from. 26 2 Are there any potential (medicines) interactions in Mrs Jones’ current therapy? response rate to question 2 – % of respondents 100% Responded No response potential (medicines) interactions – % of respondents 99.6% Yes No 0.4% Dr Linda Bryant There are a number of potential medicine interactions in the current therapy for Mrs Jones, as all but one respondent identified. There are potential pharmacodynamic and pharmacokinetic interactions. The issue becomes whether they are clinically important or not for the individual. Dr Evan Begg All respondents except one correctly answered ‘yes’. 27 3 If yes, what are they? chart 7: potential (medicines) interactions identified 200% 180% 13.6% Other combinations 160% 16.1% Paradex® plus Paroxetine % of respondents 140% 120% 66.7% Paroxetine plus Tramadol 1.8% Paramax® plus Tramadol 28.0% Amitriptyline plus Paradex® 12.5% Paradex® plus Tramadol 100% 60.2% Paraoxetine plus Sumatriptan 80% 60% 58.8% Amitriptyline plus Paroxetine 40% 49.8% Amitriptyline plus Tramadol 20% 24.4% Serotonin enhancers 0% Serotonin toxicity 12.2% 9.0% Multiple CNS depressants CNS toxicity 59.5% Paracetamol toxicity Other Note: Graph includes multiple answers. Table 4 Serotonin toxicity 28 % Amitriptyline, Tramadol, Paroxetine, Sumatriptan all Serotonin Enhancers / Multiple Serotonin Enhancers increase risk of Serotonin toxicity (synergistic effects) 24.4 Amitriptyline + Paroxetine = increased risk of Serotonin toxicity / increased drowsiness / increased Serum Amitriptyline / Paroxetine decreases metabolism of Amitriptyline / increased risk of TCA toxicity / increased CNS toxicity 58.8 Paroxetine + Tramadol = increased risk of Serotonin toxicity / decreased analgesic effect of Tramadol / increased CNS toxicity / increased risk of seizure / inhibits Tramadol metabolism 66.7 Paradex® + Paroxetine = increased risk of Serotonin toxicity / increase in Paroxetine levels 16.1 Sumatriptan + Amitriptyline = risk of Serotonin toxicity 4.7 Tramadol + Sumatriptan = Serotonin syndrome/CNS toxicity 5.0 Metoclopramide (Paramax®) + Paroxetine = Serotonin syndrome/Extrapyramidal side effects 3.9 Table 4 continued CNS toxicty Multiple CNS depressants increase risk of CNS toxicity / drowsiness/sedation/ impaired concentration / more risk of accidents 9.0 Amitriptyline + Tramadol = increased risk of CNS toxicity / lower seizures threshold / increased risk of seizures / drowsiness / respiratory depression / cholinergic effects / decreased analgesic effect of Tramadol / increased toxicity of Tramadol / cons 49.8 Paroxetine + Sumatriptan = increased blood pressure / increased risk of CNS toxicity / serotonin toxicity / exacerbate migraines / dyskinesia 60.2 Paradex® + Tramadol = Opioid duplication / antagonise gastrointestinal effects of Metoclopramide / increased drowsiness / constipation / risk of respiratory depression 12.5 Amitriptyline + Paradex® = Opioid duplication / increased Amitriptyline / increased drowsiness 28.0 Metoclopramide (Paramax®) + Tramadol both CNS depressants / Tramadol inhibits 1.8 effect of Metoclopramide in Paramax® / CNS/respiratory depressant effects Paracetamol toxicity Paramax® + Paradex® = risk of Paracetamol “double-up” / paracetamol toxicity / liver toxicity 59.5 Other % Drug interaction(s) not clinically significant / may be beneficial 4.7 Dextropropoxyphene (Paradex®) may antagonise effects of Metoclopramide 1.8 (Paramax®) on G.I. system Other drug interactions/effects 5.4 Monotherapy preferable to combination of drugs for this treatment 0.4 Note: Table includes multiple answers. Dr Linda Bryant Paroxetine is an inhibitor of cytochrome P450 2D6 (CYP2D6), and is a selective serotonin reuptake inhibitor. This leads to potential interactions with: • Amitriptyline Metabolised by CYP2D6 and therefore inhibition of the CYP2D6 by paroxetine can increase the serum concentrations of amitriptyline. This may result in up to a 400% increase of the Area Under the Curve (AUC). There is wide variation in the activity of CYP2D6 among individuals, even without taking into account the poor metabolisers (7% to 10% of the Caucasian population) and extensive metabolisers. This combination should be used with caution and the person advised of the symptoms of tricyclic antidepressant toxicity (e.g. sedation, dry mouth, blurred vision, constipation, urinary retention) and/or excessive serotonergic activity (e.g. CNS irritability, altered consciousness, confusion, myoclonus, ataxia, abdominal cramping, hyperpyrexia, shivering, pupillary dilation, diaphoresis, hypertension and tachycardia). 29 • Tramadol The mechanism of action of tramadol is through binding to the μ-opioid receptors, and through inhibition of noradrenalin and serotonin reuptake. It is metabolised to the active analgesic metabolite M1, through CYP2D6 and to a lesser extent CYP3A4. M1 appears to be metabolised by CYP3A4. Inhibition of CYP2D6 can inhibit this metabolism and reduce the amount of M1 and cause accumulation of the parent compound, tramadol. This leads to the potential reduction in analgesia (less metabolite), and has an additive effect on the serotonin and noradrenaline receptors, leading to possible serotonin toxicity. While there are reports of this interaction causing serotonin toxicity, it is not inevitable. With tramadol and antidepressants both reducing the seizure threshold, there is the possibility that this combination can promote a seizure, particularly for people with a low seizure threshold. • Sumatriptan Paroxetine inhibits the reuptake of serotonin. Sumitriptan (and other 5-HT1D agonists or triptans) can also increase serotonin concentrations and so there is a risk of precipitating serotonin syndrome. This is normally not of clinical importance but mild to severe serotonin toxicity may occur in up to 10% of people, as can (rarely) dyskinesia. The triptans may have low affinity for 5-HT1A (the sub-receptors affected by SSRIs) and do not penetrate the bloodbrain barrier well. It may be difficult for Mrs Jones to differentiate between serotonin syndrome and sumitriptan-induced cardiac adverse effects (chest tightness) and other possible adverse effects such as nausea, tingling, dizziness. The symptoms of the serotonin toxicity - nausea, abdominal cramps, tachycardia, headache, fever, chills, sweats, hypo- or hypertension and CNS symptoms - may also appear similar to the symptoms of migraine. • Paradex® (dextropropoxyphene) Dextropropoxyphene is a ‘dirty’ drug which is metabolised primarily by CYP3A4 and also appears to be a weak inhibitor of CYP2D6. This may potentially lead to increased CNS effects with the antidepressants and tramadol. The combination of these medicines has the potential to contribute to serotonin toxicity/CNS adverse effects. The pharmacokinetic and pharmacodynamic actions need to be considered and quantified for Mrs Jones as an individual, particularly when there are any changes to her medicines. Paracetamol As was indicated, there is a risk of paracetamol overdose, due to her taking two medicines containing paracetamol on a prn basis, though her current usage is well within the recommended maximum daily dosage. 30 Dr Evan Begg It was pleasing that nearly all picked serotonin toxicity/syndrome as the main problem, followed by CNS toxicity. Paracetamol toxicity also featured in around 60% of answers; however, it should be noted that the aggregate doses of this were quite low, and there are no clear interactions involving paracetamol (apart from administration of two separate drugs containing it). When addressing drug interactions, it is useful to think in terms of pharmacodynamic interactions (altered action), and pharmacokinetic interactions (altered concentrations). Pharmacodynamic interactions dominate in this case, although substantial pharmacokinetic interactions are also present and aggravate the pharmacodynamic effects. The main pharmacodynamic interactions are serotonin enhancement (amitriptyline, paroxetine, tramadol and sumatriptan), which will cause a whole variety of CNS and gut stimulatory effects, mu narcotic CNS agonist effects (tramadol and dextropropoxyphene), which will largely manifest as CNS depression, and gut effects (amitriptyline, paroxetine, tramadol, dextropropoxyphene and metoclopramide) via anticholinergic, serotonin, and mu opioid effects. The net gut effects are difficult to predict since there are both stimulatory serotonin effects (involving most drugs) and prokinetic dopamine effects (metoclopramide) competing with mu opioid inhibitory effects (tramadol, dextropropoxyphene), and anticholinergic effects (amitriptyline). The main pharmacokinetic interaction involves CYP2D6 inhibition by paroxetine, which effectively phenocopies the patient to appear to be like a genetically slow metaboliser. Therefore all other drugs metabolised by CYP2D6 are potentially affected. Specifically here, these include amitriptyline and its active metabolite nortriptyline, and tramadol and its active metabolite nortramadol (M1). Given that paroxetine is being given (with assumed compliance) at a full dose (30mg per day), a full enzyme-inhibiting effect on the other drugs can be assumed. Thus the amitriptyline dose, aimed at neuropathic pain rather than depression, could in fact be approaching antidepressant concentrations. In terms of tramadol, the pharmacokinetic effect of CYP2D6 inhibition is rather complex since both parent tramadol and one of the major metabolites (nortramadol (M1)) are both active, but not in identical ways. Overall, since nortramadol is more potent, and is largely mu opioid in effect, we could expect enhanced serotonin activity from increased parent drug, and decreased mu opioid activity from decreased nortramadol, thus decreasing the analgesic effect of tramadol. 31 4 Do you think these are clinically important interactions for Mrs Jones? response rate to question 4 – % of respondents 98.6% Responded No response 1.4% Are these clinically important interactions? 7.1% 91.4% No Yes No response 1.4% Dr Linda Bryant When we look at a list of medicines as ‘purists’, Mrs Jones’ list immediately screams out an alert – and we tend to want to ‘fix it up’. In order to rationalise our ‘gut instincts’, because there are potentially clinically important interactions possible in this list of medicines, it is important to question Mrs Jones, particularly about any possible adverse effects she is experiencing. Mrs Jones may not recognise some drugrelated problems as adverse effects, such as insomnia due to serotonin toxicity, some cognitive slowing, increased heart rate, etc, so we have to be aware of the specific adverse effects that are likely, and ask specific questions to determine the relevance to the particular person. Dr Evan Begg Most people correctly indicated ‘yes’. Serotonin toxicity was again stressed (71%), followed by CNS toxicity (38%) and paracetamol toxicity (32%) (see Chart 8). While the serotonin axis was expected, I wonder if some people have underestimated the CNS toxicity, and overestimated the possibility of paracetamol toxicity. 32 If yes, why? response rate to question 5 – % of respondents 91.4% Responded 8.6% No response chart 8: Why these are clinically important interactions 80% 70.7% 60% 37.9% 40% 31.6% 18.0% 12.9% 11.3% Potentially life threatening Review meds Migraine linkage Paracetamol toxicity CNS toxicity 0% Serotonin toxicity 9.0% 8.6% Other 20% Not clinically important % of respondents 5 Note: Graph contains multiple answers. Dr Linda Bryant In this case Mrs Jones is feeling well enough that she is considering extending her work activity – an indication that the combination must be working adequately and she is probably not experiencing obvious adverse effects. Her list of medicines may not look pretty – but they appear to be working for her. Any changes risk interfering with a stable interaction, noting that her medicines use, even of prn medicines, is reasonably consistent. The prescribed dose of amitriptyline is low, although the serum concentration may be higher than we would expect if Mrs Jones was not on paroxetine. This will need to be remembered if the paroxetine is stopped, remembering that antidepressants are continued for at least six to nine months after a response – therefore the fact that Mrs Jones appears to be ‘doing fairly well now’ is not necessarily a reason to stop the paroxetine. 33 The tramadol dose is also relatively low, and so there is a need to ensure that she does not start increasing the dose without medical input. Similarly, the use of Paradex® is low (two at night) and Paramax® use is intermittent. The potential interactions above do occur and can be dramatic, but they are not clinically important in every person. Chronic back pain is a complex problem and management is usually a fine balance between providing ideal treatments and obtaining suitable analgesia. Mrs Jones’s list begs for some intervention and it is difficult to resist the temptation to interfere with her medication profile, but we simply have inadequate historic information at this stage. Dr Evan Begg The serotonin and CNS effects possible are described above in question 3. There is not enough information available to know if she has suffered from these effects or not, and clearly appropriate questions need to be asked. Regarding paracetamol, the purported doses seem to be 1g daily for five of seven days, and 2g for the other two days. This does not seem particularly concerning, especially since she is relatively young and there are no clear pharmacokinetic interactions (paracetamol is largely glucuronidated, with some sulfation, and none of the other drugs inhibit these processes). CNS toxicity may result from the summation of amitriptyline plus nortriptyline, tramadol plus nortramadol, and dextropropoxyphene. Of these, consideration should be given to discontinuing dextropropoxyphene (an awful narcotic drug, very lethal in overdose), and somehow rationalising the complex CYP2D6 pharmacology. The key drug in this regard is paroxetine, as it is influencing amitriptyline and tramadol (and respective metabolite) concentrations. It would be great if paroxetine could be discontinued, but this should only take place under the direction of someone with detailed knowledge of her depression and its timing. 34 What information would you discuss with Mrs Jones regarding the use of gabapentin? response rate to question 6 – % of respondents 99.6% Responded No response 0.4% chart 9: gabapentin information 100% 90.7% 80% % of respondents 60% 55.6% 38.0% 40% 31.2% 29.7% 21.9% 20% 1.4% Other 3.9% Health check 3.9% Treatment type Compliance information Interactions Contraindication Indication for use Funding 0% Dosage regime 4.3% Treatment length 9.7% Adverse effects 6 Note: Graph contains multiple answers. Dr Linda Bryant From the first question I would have explored Mrs Jones’ reasons for asking about the gabapentin. Some people like to know what else is available ‘just in case’, the general practitioner may have tweaked her interest, or Mrs Jones may think that the gabapentin will be the panacea that will get her back to work faster (perhaps she perceives that her current treatment is ‘second rate’ because she is not on the latest ‘new’ medicine). I would assure Mrs Jones that gabapentin was an effective medicine, by comparing it with tricyclic antidepressant efficacy. There is not a lot of difference in numbersneeded-to-treat (NNT) and so selection is really based on the individual. The NNT for neuropathic pain (number to reduce pain by 50%) is approximately four (note that this is not complete resolution of pain). 35 Although the adverse effects are usually minor and tolerance can develop, the potential for unwanted effects include: table 5 Number needed to harm Somnolence ∼ 11% NNH 9 Fatigue ∼ 6% NNH 17 Dizziness ∼ 12% NNH 8 Ataxia ∼ 5% NNH 20 Possible weight gain 1.7% Diplopia 4% tremor, muscle weakness/pain, difficulty concentrating It is particularly important that Mrs Jones knows that she could not drive or operate machinery until she has established whether these adverse effects affect her (preferably one to two weeks). There is also little information for use during pregnancy and so if Mrs Jones wishes to become pregnant, she should enter a group discussion with her general practitioner, pain team ± gynaecologist. Dr Evan Begg Given that Mrs Jones reported to be generally fairly happy with the status quo, it would seem that her question re gabapentin was probably largely exploratory, and in response to the GP mentioning it. In other words, perhaps she was only asking for general information as a step care possibility for the future. In this case most discussion should focus on the relative value of gabapentin compared with current neuropathic drugs, especially related to efficacy. It would of course be useful, as noted, to discuss the downsides of adding gabapentin, and in particular CNS toxicity (in the context of pharmacodynamic interactions). The idea could be raised of replacing a current drug, e.g. amitriptyline, with gabapentin, thereby avoiding some pharmacokinetic interactions (gabapentin is eliminated largely renally unchanged, and therefore is not subject to CYP2D6 inhibition). A major downside of gabapentin, and all the other CNS acting drugs, is potential effects on driving and operating machinery. Alcohol history is also relevant in this regard. 36 What information would you discuss with Mrs Jones’ general practitioner regarding the introduction of gabapentin into her medicine regime? response rate to question 7 – % of respondents 99.3% Responded No response 0.7% chart 10: informational themes 70% 62.2% 60% 50% % of respondents 42.8% 40% 30% 27.7% 27.3% 29.9% 20% 7.9% Other 5.4% Interactions Health check Adverse effects AE/monitoring Try another med first Change meds regime Funding 0% 6.8% Pregnancy advice 12.6% 10.8% 10% Dose regime 7 Dr Linda Bryant Mrs Jones is currently on a complex regime that has been established by the chronic pain clinic. Although there are unlikely to be pharmacokinetic interactions, there are potential pharmacodynamic interactions and therefore the pain team should be consulted (directly or through the general practitioner) prior to the introduction of gabapentin. Because of the complexity of chronic back pain, there would need to be a good reason for changing treatment. Mrs Jones does not appear to be suffering any adverse effects, and she seems to be having an improvement in pain relief. While I can see some potential changes to her medicines, this would require close supervision of Mrs Jones and ensuring she had an understanding of the potential adverse effects. For example, the amitriptyline appears to be effective and even though there may be higher serum concentrations than expected from a 10mg dosage, it could be increased to 20mg. If there were no unacceptable adverse effects, then the prn medicines, Paradex® initially, then tramadol, could be reduced. 37 With respect to gabapentin, I would reiterate the comparative efficacy of gabapentin in terms of NNT compared with amitriptyline (i.e. little difference), and mention the adverse effects to be expected, plus the requirement for slow dose titration. I would also include a comment about the reduced bioavailability of gabapentin with increasing doses (i.e. doubling the dose does not double the serum concentration or AUC). Dr Evan Begg More information is required about the history and diagnoses, as without correct diagnoses any treatment is inappropriate. The major points of interest were the dosing regimen, and the possible addition of gabapentin. A large number (43%) also discussed the possibility of changing medications (mainly in the direction of simplifying the regimen). The possibility of gabapentin introduction allowing the removal of perhaps amitriptyline and Paradex® was raised. It would be useful also to review the depression angle, as paroxetine is the major drug causing interactions. Perhaps there could have been a higher priority on psychosocial aspects of all of the problems, and potential lifestyle adjustments. There is some tension between who is primarily managing the patient – the GP, the chronic pain team, or the psychiatrist. 38 What advice would you have given Mrs Jones if she had presented nine months ago with acute lower back pain? (Hint: Look at the ACC New Zealand Acute Lower Back Pain Guide) response rate to question 8 – % of respondents 99.3% Responded No response 0.7% chart 11: advice provided by themes 100% 88.5% 80.2% 80% 60% 50.7% 47.5% 40% 23.4% 23.4% 19.1% 20% 17.6% 15.1% 7.2% 7.9% Assess work environment Meds recommended Clinical aseessmnet No heavy lifting Work rotation Exercise See other health professional See GP if no improvement Continue working Stay active Assess clinical history 0% Assess pain history 5.0% ACC ALBP for self-management 12.6% 9.7% Other % of respondents 8 Note: Graph includes multiple answers. 39 table 6: informational themes % Assess pain history 9.7 Assess clinical history 23.4 Stay active 88.5 Continue working 47.5 See GP if no improvement 23.4 See other health professional 50.7 Exercise 19.1 Work rotation 17.6 No heavy lifting 12.6 Clinical assessment Meds recommended 5.0 80.2 ACC ALBP for self-management 7.2 Assess work environment 7.9 Other 15.1 Note: Table includes multiple answers. Dr Linda Bryant Yes, ‘backs like (safe) movement’ and so staying active is important advice. This is contrary to the advice of some years ago when people would be told to rest in bed, leading to weakened muscles and more problems. The advice to stay active, continue working and do exercise (but no heavy lifting) was very appropriate. Referral for safe exercises and activity may be appropriate. In order to maintain safe mobility, clear information needs to be provided on back care (see the New Zealand Acute Low Back Pain Guide14) and good analgesia. Regular (with emphasis on regular) paracetamol is still a good basal analgesia. Mrs Jones is young with no apparent risk factors, and so supplementation with an NSAID prn could be helpful. If you had concerns about Red Flags, or Mrs Jones didn’t find any improvement in two to three days, then referral to a medical practitioner would be required. It may also be appropriate to give Mrs Jones an indication of the timeframe for improvement (usually resolves in four to six weeks, but expect significant improvement within one to two weeks). Red Flags Red Flags help identify potentially serious conditions. They include: 40 • urinary or faecal incontinence, abnormal gait, lower limb weakness • severe worsening pain, especially at night or when lying down • significant trauma • weight loss, history of cancer, fever • use of intravenous drugs or steroids • patient over 50 years old. Yellow Flags Yellow Flags indicate psychosocial barriers to recovery. They include: • belief that pain and activity are harmful • ‘sickness behaviours’ (like extended rest) • low or negative moods, social withdrawal • treatment that does not fit best practice • problems with claims and compensation • history of back pain, time-off, other claims • problems at work, poor job satisfaction • heavy work, unsociable hours • overprotective family or lack of support. Dr Evan Begg The main themes highlighted were that she should stay active, and that medications would be recommended. To me a detailed assessment and accurate diagnosis would be the main priority. The diagnosis will dictate the therapeutic direction. Page six of the New Zealand Acute Low Back Pain Guide outlines the steps you need to take to assess the presentation of acute low back pain to exclude Red Flags. This assessment is critical as it will determine whether you are able to recommend treatment or have to refer the client to a doctor. Page 10 of the Guide outlines the management options for acute low back pain. Page 23 outlines Yellow Flag assessments and management options if your client returns to you after trying treatment to manage the pain. 41 Bibliography Baxter K (ed). Stockley’s Drug Interactions. 8th ed. RPS Publishing, 2007. Flockhart D. Cytochrome P450 drug interaction table. http://medicine.iupui.edu/clinpharm/DDIs/ Management of non-specific back pain and lumber radicular pain. BPAC Journal June 2009. http://www.bpac.org.nz/magazine/2009/june/nsbackpain.asp Neurontin Product Data Sheet. http://www.medsafe.govt.nz/profs/Datasheet/n/Neurontincap.htm New Zealand Acute Low Back Pain Guide. http://www.nzgg.org.nz/guidelines/0072/acc1038_col.pdf Saarto T, Wiffen PJ. Antidepressants for neuropathic pain. http://www.cochrane.org/reviews/en/ab005454.html Wiffen PJ, McQuay HJ, Rees J, Moore RA. Gabapentin for acute and chronic pain. http://www.cochrane.org/reviews/en/ab005452.html References 13. ‘Malingering’ is defined as: Exaggerating or feigning illness in order to escape duty or work. 14. http://www.acc.co.nz/about-acc/research-sponsorship-and-projects/researchand-development/evidence-based-healthcare-reports/index.htm#Clinical_ Guidelines 42 43 44 www.acc.co.nz 0800 222 070 ACC5327 Printed November 2009 ISBN: 978–0–478–31468–7
















































![My_Body[1] - Junior2TopicWiki](http://s1.studyres.com/store/data/008060165_1-be31cd2568d5e2c9fee6ce67732b07b4-150x150.png)



