* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Cardiovascular System 1
Survey
Document related concepts
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Heart failure wikipedia , lookup
Coronary artery disease wikipedia , lookup
Rheumatic fever wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Artificial heart valve wikipedia , lookup
Myocardial infarction wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Cardiac surgery wikipedia , lookup
Electrocardiography wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
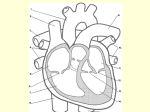
Biology 219 – Human Physiology Clemens Cardiovascular System 1: The Heart Text: Ch. 14 A. Overview of the Cardiovascular System 3 components: heart blood vessels blood Heart → arteries → arterioles → capillaries → venules → veins ( → return to heart) Right heart pumps deoxygenated blood to lungs (pulmonary circulation); lower pressure Left heart pumps oxygenated blood to entire body (systemic circulation); higher pressure B. Heart Anatomy atria - receiving chambers ventricles - pumping chambers 1. Chambers and Great Vessels RA ← vena cavae RV → pulmonary trunk (artery) LA ← pulmonary veins LV → aorta Pulmonary circulation: RV → pulmonary trunk → LUNGS → pulmonary veins → LA Systemic circulation: LV → aorta → BODY → vena cavae → RA 2. Heart Valves a. Atrioventricular (AV) valves - prevent backflow from ventricles to atria tricuspid valve - RA } RV bicuspid (mitral) valve - LA } LV chordae tendineae attached to papillary muscles prevent prolapse of AV valves b. Semilunar valves - prevent backflow from arteries to ventricles pulmonary valve - RV } pulmonary trunk aortic valve - LV } aorta C. Cardiac Muscle Cells autorhythmic cells spontaneously initiate APs intercalated discs allow AP to spread between cardiac muscle cells sinoatrial (SA) node - primary pacemaker 1. Excitation-Contraction Coupling - similar to skeletal muscle: AP → T tubules → SR → releases Ca2+ Ca2+ → troponin → tropomyosin → uncovers myosin binding sites → contraction - Ca2+ also enters from the ECF through Ca channels during contraction Ca2+ is pumped back to SR by Ca2+ ATPase during relaxation phase Ca2+ is also transported back out to ECF `by a Na-Ca exchanger D. Cardiac Action Potentials 1. Pacemaker Potential in Autorhythmic Cells (1) slow depolarization toward threshold = pacemaker potential “funny channels” permeable to Na+ and K+ (2) rapid AP depolarization - due to Ca2+ inflow (3) repolarization Autonomic NS control: sympathetic - faster depolarization → ↑ heart rate parasympathetic - slower depolarization → ↓ heart rate 2. Myocardial Action Potential in Contractile Cells (0) initial AP depolarization - similar to other APs (voltage-gated Na+ channels) (1) slight repolarization (2) plateau phase (100-200 ms) - due to slow, inward Ca2+ flow (L-type Ca channels) results in long AP duration and long refractory period (200-300 ms) Biology 219 – Human Physiology (3) repolarization - due to delayed opening of voltage-gated K channels E. Conduction System of the Heart 1. autorhythmic cells - “pacemakers” 2. conduction fibers - specialized to spread AP rapidly through ventricles. sinoatrial (SA) node ↓ atrial depolarization ↓ atrioventricular (AV) node ~ 0.1 second delay ↓ AV bundle (of His) ↓ R & L bundle branches ↓ Purkinje fibers ↓ ventricular depolarization F. Electrocardiogram (ECG) [Lab Exercise] P wave - atrial depolarization QRS complex - ventricular depolarization T wave - ventricular repolarization Clemens