* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Coronary Artery Disease
Survey
Document related concepts
Remote ischemic conditioning wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Saturated fat and cardiovascular disease wikipedia , lookup
Drug-eluting stent wikipedia , lookup
Cardiovascular disease wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Cardiac surgery wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
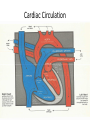
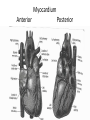
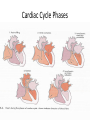
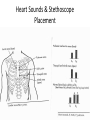
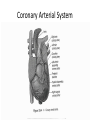
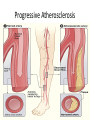
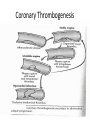
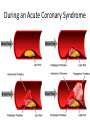
Oxygen Needs Interference with O2 Transport Case Study Oxygen Needs Interference with O2 Transport Coronary Artery Disease Complications Dysrhythmias Pulmonary Embolism Hypertension Complication Congestive Heart Failure Peripheral Vascular / Arterial Disease Oxygen Needs Interference with O2 Transport Care of Patients with: Coronary Artery Disease Risk Factors Myocardial Infarction Alterations in: Rate & Rhythm (Cardiac Conduction) Effect on Cardiac Output Content Approach Anatomy & Physiology Review Demographics/occurrence Pathophysiology Clinical Manifestation Medical / Surgical Management Nursing Process (APIE) Assessment - Nursing Actions - Education Anatomy & Physiology Right Heart Left Heart Systole Valve Closure: Diastole Valve Closure: Cardiac Circulation Myocardium Anterior Posterior Cardiac Cycle 1. Passive Filling – preload 2. Atrial contraction – Aortic & Pulmonic semilunar valves close – S2 3. Isovolumetric ventricular contraction – all valves closed 4. Ejection – ventricular systole – Mitral & Tricuspid valves close – S1 - afterload 5. Isovolumetric ventricular relaxation – all valves closed Cardiac Cycle Phases Heart Sounds & Stethoscope Placement Coronary Arterial System Physiology: Oxygen Supply to the Cardiac Muscle during the Cardiac Cycle Coronary artery oxygen deficit during ventricular contraction & ejection (systole) Coronary artery filling during ventricular filling (diastole) What is the impact of heart rate on coronary artery filling? Oxygen Supply to the Cardiac Muscle during the Cardiac Cycle The actual time available for diastole shortens significantly as the heart rate increase % of a Minute 70% 50% 33% Heart Rate 60 120 188 Results: Less time for ventricular filling & coronary artery filling + as HR increases, increased oxygen is needed each minute to eject the same volume of blood. Stroke volume: volume ejected in one heart beat Cardiac Output: volume ejected in one minute Cardiac Output = Stroke Volume x Heart Rate Factors Determining Myocardial Oxygen Needs Decreased Oxygen Supply: Noncardiac: Anemia, hypoxemia, pneumonia, asthma, COPD, low blood volume Cardiac: Arrhythmias/dysrhythmias, congestive heart failure (CHF), coronary artery spasm, coronary artery thrombosis, valve disorders Increased Oxygen Demand or Consumption: Noncardiac: anxiety, cocaine use, hypertension, hyperthermia, hyperthyroidism, physical exertion Cardiac: aortic stenosis, arrhythmias, cardiomyopathy, hypertension, tachycardia CAD - Demographics CAD - Demographics Comparison of death by CV Disease and Breast Cancer – by Women’s Age 400 300 Cardiovascular Disease Breast Cancer 200 100 0 35-54 55-74 >=75 Coronary Artery Disease (CAD) Pathophysiology ASHD, IHD, CVHD = CAD AHA 1.1 mil Americans will have an MI in 2003 460,000 will die About half of those deaths occur within 1 hour of the start of symptoms and before the person reaches the hospital. Major cause: Atherosclerosis—focal deposit of cholesterol & lipids CAD – Risk Factors Unmodifiable: Age, Gender, Ethnicity, Genetic predisposition/family history Modifiable Major: Dyslipidemia--Elevated serum lipids*, hypertension*, cigarette smoking, obesity— visceral/central obesity Modifiable Contributing: Diabetes Mellitus*, stressful lifestyle * may have genetic predisposition CAD – Risk Factors • Metabolic Syndrome: – – – – – – Insulin Resistance Hyperglycemia >110mg/dL Hypertension - > 130/85 Increased triglycerides >110mg/dL Decrease HDL <40 men; < 50 women Central Obesity • men: waist > 40” women: waist > 35” Risk Factors One of the Major Modifiable Physical Inactivity Types of Plasma Lipoproteins HDL – Contain more protein and less lipid Carry lipids away from arteries to liver for metabolism This process prevents lipid accumulation within arterial walls Higher levels are desirable LDL – Contain more lipids than any other lipoproteins Affinity for arterial walls Increased levels correlate closely with an increased incidence of atherosclerosis Lower levels are desirable VLDL Contain of triglycerides Correlation with heart disease is uncertain Plasma Lipoproteins Atherosclerosis Elevated serum lipids Cholesterol > 200mg/dl Triglyceride > 200mg/dl HDL < 35 mg/dl – major risk 45-59 mg/dl – average risk > 60 mg/dl – negative risk LDL < 130 – desirable 130 – 159 mg/dl – borderline risk > 160 mg/dl – high risk Progressive Atherosclerosis Drug Therapy for Dyslipidemia Bile Acid Sequestrants (Questran) - Binds with bile salts Niacin - Inhibits synthesis of VLDL & LDL Fibric Acid Derivatives (Atromid)– Decrease VLDL HMG CoA Reductase Inhibitors (Statins - Lipitor, Pravachol, Zocor) – Block synthesis of cholesterol Cholesterol Absorption Inhibitor (Zetia)– Inhibits intestinal absorption of cholesterol Natural Lipid Lowering Agents Niacin - < LDL levels Omega-3 fatty acids – fish/flaxseed oil <Triglycerides & > HDL levels Milk thistle – Silymarin - > HDL levels Fiber - < Cholesterol Phytosterols - < Cholesterol Soy - < Cholesterol absorption from GI tract CoEnzyme Q10 – HMG CoA reductase inhibitors – natural statins Coronary Thrombogenesis During an Acute Coronary Syndrome Angina Clinical Manifestations Angina – Chest Pain Stable Angina Pectoris – intermittent, same pattern of onset, duration, intensity of symptoms - 3-5 mins. Silent Ischemia – 80% of patients with ischemia are asymptomatic Prinzmetal’s Angina – variant – not precipitated by physical activity – may be due to spasm Nocturnal Angina – occurs at night but not necessarily during sleep or in recumbent position Angina Decubitis – recumbent position – relieved by standing Unstable Angina – Unpredictable or may evolve from stable angina – increasing frequency, duration, intensity CAD Clinical Manifestation – Diagnostics History & Physical Examination EKG / Echocardiogram / Stress Echocardiogram Thallium Stress Test (perfusion scanning) cold spots where tissue is inadequately perfused CAT scan- calcium score/CT coronary angiogram MUGA (Multiple gated radioisotope scan) – left ventricular function MRI of the heart PET (Positron emission computed tomography) – evaluate coronary artery patency