* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download document 8925848
Survey
Document related concepts
Transcript
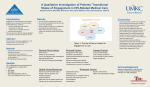
VOL.6 NO.2 J U N E / J U LY 2 0 0 7 THE NEWSLETTER OF COLUMBIA UNIVERSITY MEDICAL CENTER The College of Physicians & Surgeons • The College of Dental Medicine • The School of Nursing • The Mailman School of Public Health The Coordinated Doctoral Program in the Basic Sciences of the Graduate School of Arts & Sciences H I V I N N Y C Researchers on Battlefront Of Local HIV Epidemic N E W G R A N T S F U N D C L I N I C A L T R I A L S F O R N E X T- G E N E R AT I O N P R E V E N T I O N , T R E AT M E N T W ith 64 percent of the world’s HIV-positive people, subSaharan Africa is the location most often thought of as the epicenter of the HIV/AIDS epidemic, so much so that the epidemic in the United States is often forgotten. “There is a widespread misperception that HIV is under control here, but the HIV incidence in some New York City populations is higher than in many African countries,” says Wafaa El-Sadr, M.D., professor of clinical medicine and epidemiology and chief of infectious diseases at Harlem Hospital. Two new grants recently awarded to Dr. El-Sadr and Scott Hammer, M.D., the Harold C. Neu Professor of Infectious Diseases, will allow Columbia to continue to focus needed attention on the HIV/AIDS epidemic in New York City. With support from a $20 million, seven-year grant from the NIH, the Source: NYC Department of Health & Mental Hygiene, 2007 People with HIV as a percentage of population in 2005. The South Bronx, Central Brooklyn, Harlem, and lower Manhattan have the highest proportions Columbia Collaborative HIV/AIDS Clinical Trials Unit, led by Dr. Hammer, provides New Yorkers with access to the latest drugs and vaccine candidates in clinical trials. A highlight of this grant is the close collaboration of adult and pediatric clinical HIV research at CUMC with Philip LaRussa, M.D. professor of clinical pediatrics, as the principal investigator of the latter. An additional $3 million, seven-year grant will help the Center for Innovative Research to Control AIDS, directed by Dr. El-Sadr, test ways other than vaccines to prevent HIV transmission. Both grants were awarded in March as part of a reorganization of the HIV/AIDS clinical trials networks of the National Institute of Allergy and Infectious Disease (NIAID). Columbia has been a part of the networks since 1987, when the networks were estabplease see Page 7 of people living with HIV in the city. L E A D E R S H I P C O N T E N T S n n HIV in New York: CUMC Physicians in the Trenches School of Nursing Leads in Primary Care, Education and Research EVP Column: A Year of Progress 1 School of Nursing Becomes National Trendsetter 2 3A 4 5 6 7 C O L U M B I A - T R A I N E D N U R S E S F I L L P R I M A RY C A R E G A P, E N G A G E I N GROUND-BREAKING RESEARCH Ethical Implications of a Pandemic Flu n n P&S Scientists Pinpoint Neuronal Culprits in ALS New Lyme Center Launches Craniofacial Surgeons Repair Young Lives n n Research Briefs Mailman Researchers Join Hunt for Killer of Bees Awards & Honors recent study led by a team of researchers from the School of Nursing found that in intensive care units at hospitals across the country patients are more likely to acquire potentially deadly infections where there is inadequate nurse staffing. The study showed that an increase in nurses’ overtime hours was linked to higher rates of ventilator pneumonia, catheter infections and skin ulcerations. “Nurses are the hospitals’ safety officers, but nursing units that are understaffed and have overworked nurses are shown to have poor patient outcomes,” says Patricia Stone, Ph.D., M.P.H., R.N., assistant professor of nursing and the study’s lead author. “Improvements in nurse working conditions are needed for the safety of our nation’s sickest patients. With the looming nursing shortage, hospitals direly need to address working conditions to help retain current staff and recruit people into nursing.” This work by Dr. Stone is one of many patient care and health policy studies that researchers at the school are working on. (See sidebar on p. 8 for a sampling). The school is at the forefront of education advances as well, having just graduated its second class of students with the Doctor of Nursing Practice (DrNP) degree. These 20 clinical experts – all experienced nurse practitioners when they entered the program – now have additional education and skills necessary to care for patients in a variety of settings, from hospital to ambulatory care clinic. The DrNP program is the first of its please see Page 8 NON-PROFIT ORG. U.S POSTAGE PAID NEW YORK, NY PERMIT NO.3593 C O L U M B I A M E D I C A L U N I V E R S I T Y E V P J O U R N A L C E N T E R Dear Colleagues & Students, M y first year at Columbia has been extraordinarily rewarding. I am personally grateful for the support of the collec- InVivo is published by the Office of Communications and External Relations. InVivo covers the latest advances and news at Columbia University Medical Center. LEE GOLDMAN, M.D., Executive Vice President for Health tive Columbia University Medical Center community. Several initiatives have focused on creating a true CUMC community. The deans of the Mailman School of Public Health (Dr. Allan Rosenfield), the College of Dental Medicine (Dr. Ira Lamster) and the School of Nursing (Dr. Mary Mundinger) now serve officially as vice presidents of CUMC. and Biomedical Sciences and Dean of the Faculties of Health We meet together regularly to address issues and common interests and concerns. Using philanthropic funds, we conducted a Sciences and Medicine MARILYN L. CASTALDI, Chief Communications Officer BONITA EATON ENOCHS, Assistant Vice President for competitive process to encourage submission of proposals for four-school research projects. The winning proposal, “The Impact of Social Inequities on the Complex Relationship between Oral Health and Peripheral Vascular Disease: An Interdisciplinary External Relations and Director of Publications Evaluation,” selected from among 14 applications, will be supported by the David A. Gardner New Initiatives Fund, created by EDITORIAL STAFF Board of Visitors member Lynn Shostack in memory of her husband. ANNA SOBKOWSKI, Director of Science Communications For P&S, it was a year of transition and a year of many accomplishments. We achieved strategic growth through the recruit- and Editor ment of many outstanding senior faculty whose expertise and professional breadth are already complementing our scientific and SUSAN CONOVA, Science Writer InVivo clinical work. A new Department of Neuroscience and the new 701 West 168th Street, P&S Box 153 Center for Human Genetics are prime examples of organizing for New York, NY 10032 Phone: 212-305-7131; Fax: 212-305-4521 greater potential. Similar initiatives are just starting in transplantation and in cardiovascular research. Our clinical research hub for the campus, the newly renamed Irving Institute for Clinical & Translational Research, has become a central internal funding [email protected] www.cumc.columbia.edu/news/in-vivo agency, helping to drive multi-department, multi-school clinical research across the medical center. P&S graduate programs, Design: Graphic Expression Inc., NYC which are already highly rated for their excellence by the Chronicle of Higher Education, are being reshaped to enrich cross-disciplinary exposure consistent with current research trends. The M.D./Ph.D. program is expanding, thanks to renewed and E D U C A T I O N increased NIH funding. Teaching Academy Announces 2007 Research Grants The Glenda Garvey Teaching Academy at CUMC provides support for innovative educational research projects, particularly those that involve more than one school or that can be generalized to all schools. Grants are worth as much as $20,000 and can last two years. Recipients of 2007 educational grants and their This year the Mailman School of Public Health fortified its position as a leader in global health, with research and service programs in more than 80 countries. The school’s International Center for AIDS Care and Treatment Programs, (ICAP), recipient of the largest government grant in Columbia University history, provided HIV/AIDS care through ICAP-supported sites to more than 250,000 people in Africa and Thailand. The Reproductive Health Access, Information and Services in Emergencies initiative, a program addressing a full range of reproductive health needs for refugees and internally displaced persons, launched with the largest foundation grant in Columbia’s history. Two new centers – the Center for Study of Social Inequalities and Health (Departments of Epidemiology and Sociomedical Sciences) and the Imprints Center for Genetic and Environmental Lifecourse Studies (Department of Epidemiology) – were established to provide greater understanding of the origins and influences affecting health and disease. Innovations at the College of Dental Medicine are expanding the scope of traditional dental research. An NIH-funded initia- projects: tive is exploring the promise of stem cells to create soft tissue for craniofacial reconstruction. Faculty are leading research into RONALD B AY E R , PH.D., professor of socio- lasers and new imaging techniques that will transform dental care in the future and are offering instruction on use of new techmedical sciences, Mailman School of Public Health. nologies in patient care. The College has continued to be a leader on national healthcare policy, advocating for expanded oral “Development of a Health Sciences-wide Course on healthcare for both children and the elderly. Globally, dental faculty and students are working to develop sustainable oral health the Ethics of Public Health.” programs in Sub-Saharan Africa through the Millennium Villages program, while continuing with many active local public servH E E R A C H A N G , M . D . , D . D . S . , assistant pro- ice programs like the Community DentCare Network. fessor of oral and maxillofacial surgery, College of The School of Nursing enjoyed unprecedented growth this year in record numbers of students applying and being admitted. Dental Medicine. “Case Based Learning for the Research faculty continues to achieve prominence as leaders in areas of national priorities in science. The school ranks first in Management of Medically Compromised Patients in NIH per capita funding and 13th in aggregate funding (up from 27th in 2006). Clinical practice is distinguished with the Doctor Dental Practice.” of Nursing Practice (DrNP) degree – developed and instituted first at Columbia – now being adopted by over 200 schools of W E N D Y C H U N G , M . D . , P H . D . , assistant pro- nursing. The third class of DrNP students graduated in May, and all are actively engaged in advanced practice. fessor of pediatrics, P&S. “Conversations in Genetics: A key factor in ensuring the continued evolution and invigoration of our research, education, and clinical initiatives will be Development of Educational DVDs to Teach Medical the opportunity to grow physically as well as programmatically. Even as we embark on a comprehensive space planning process, Genetics.” we are working on plans to expand classroom space within the Hammer building to benefit all four schools. N I C H O L A S F I E B A C H , M . D . , professor of clinical medicine; J O H N E N C A N D E L A , P H . D . , director, My thanks to the CUMC community for its support and inspiration during my first year at Columbia. I wish you all an enjoyable summer as we continue our commitment to making CUMC arguably the best in all that we do. Scholarly Resources; K A T H E R I N E N I C K E R S O N , M.D., associate professor of clinical medicine; A N D R E W M U T N I C K , M . D . , assistant clinical pro- fessor of pediatrics, P&S. “Improving House Staff Teaching of Medical Students: Learning to Give Effective Feedback in the Clinical Setting.” please see Page 6 2 Lee Goldman, M.D. H E A L T H P O L I C Y & E T H I C S C R A N I O F A C I A L R E S E A R C H If Pandemic Flu Strikes, Who Will Get Scarce Ventilators? Creating Implants from Stem Cells While many of us are trying to lose fat this summer, researchers in the College of Dental Medicine will be If a pandemic similar to the 1918 “Spanish” flu hit New York today, the state projects more than 770,000 people would be admitted to the hospital during a sixweek outbreak. Of those, nearly 60,000 would need mechanical ventilators. The state has a stockpile of ventilators, but in a severe pandemic, the demand would outstrip the supply. Adding more ventilators to the stockpile would not solve the problem because severe staff shortages are projected, and there would not be enough workers to operate all ventilators. Last year, the New York State Department of Health and the New York State Task Force on Life & the Law assembled a group of physicians, lawyers, ethicists and policymakers to draft a plan for fair allocation of ventilators during an emergency. The plan calls for hospitals to triage all patients and deny ventilators to those who score poorly on an assessment that predicts mortality. Many patients on ventilators at the beginning of the pandemic would be taken off against their wishes. (Full details of the plan are available at http://www. health.state.ny.us/diseases/communicable/influenza/pandemic/ventilators/). After the state’s plan was presented to CUMC faculty at a special town meeting sponsored by the Center for Bioethics, InVivo spoke with Neil Schluger, M.D., chief, Division of Pulmonary, Allergy, and Critical Care Medicine and professor of medicine, epidemiology and environmental health sciences, who was a member of the working group that drafted the plan. trying to devise ways to add fat back to our bodies. With a new $2.5 million grant from the National Institute of Biomedical Imaging and Bioengineering, Jeremy Mao, D.D.S., Ph.D., associate professor of dental medicine, will try to construct soft adipose tissue implants out of a patient’s own stem cells. Cancer surgery, chronic diseases, trauma and congenital anomalies can all cause disfigurements that lead to physical and psychosocial suffering. During reconstruction, surgeons will often graft soft tissue from other sites on the patient’s body, but that creates additional wounds. Attempts have been made to use fat cells left over after liposuction, but these cells have a limited lifespan and the implants essentially deflate within weeks. Dr. Mao’s plan is to create long-lasting soft tissue implants from mesenchymal stem cells harvested from In the winter of 1918, a new influenza virus spread around the world, killing 40 million the patient’s own tissues such as bone marrow or adi- to 50 million people and possibly as many as 10 percent of the world’s young adults. pose tissue. Mesenchymal stem cells can differentiate The plan addresses this potential problem by only pitting a patient against his or her own chance of survival, not against that of another patient’s. That takes a bit of the burden away from the doctor. Still, physicians would be the ones turning off the ventilators. I’ve had to withdraw care from a few patients who subsequently died. In certain cases it is the right thing to do, but few things in medicine have shaken me up as much as having to do that. Does the plan violate doctors’ basic What prevents healthcare providers duty to care for their patients? from ignoring the plan? There is a real tension here. In medicine you have an absolute obligation to your patient, regardless of what is happening to other patients in the hospital. This plan is radically different and takes a public health approach, where the focus is on the community rather than on the individual. The plan asks physicians to do what we generally don’t do – and don’t like to do: deny or withdraw care. There are times when we withdraw care if we think further medical intervention is completely futile. But if we start rationing ventilators, we would need to withdraw or withhold care over the stated wishes of the patient or the patient’s family. Will physicians be able to do that? I don’t think anybody is sure what is going to happen. The plan is totally voluntary. It has no chance of working unless all hospitals in an affected area play by the same rules. Presumably, the governor would declare a state of emergency and put the plan in effect, but every hospital would still have to agree to it. A massive educational campaign will have to be undertaken to help physicians and the public understand that more deaths would result from not following the plan and that it is fairest for everyone. It doesn’t favor the wealthy, the young, or the better educated. None of those factors – even to the point of not favoring healthcare workers if they got sick, because they would be out of work for months, just like everyone else – will increase a patient’s access to a ventilator. What happens to people who are Is there anything in the plan that will not eligible for a ventilator or are make this any easier on physicians? removed from a ventilator? The plan is very careful not to pit one patient against another. This is an issue that always comes up in medical ethics sessions. Nobody wants to abandon one patient for a supposedly worthier one. They would require palliative care. It would be horrible not to give someone a ventilator and then also not provide further care. But palliative care is not something that hospitals have a lot of expert- ise with. Improving palliative care capacity is going to be a real challenge. Have there been any medical advances since 1918 that might make a similar virus less lethal today? Probably not. Our medical arsenal today consists of immunization and treatment. Immunization is not yet a realistic possibility. Making a vaccine for a pandemic influenza is more difficult than making one for regular influenza, and a vaccine specific for the virus would not be available for at least six months after a pandemic starts. On the treatment side, there’s Tamiflu. Nobody knows how this drug will work in a pandemic. In studies with regular flu, patients who took the drug experienced, on average, one fewer day of symptoms. I don’t think this is going to save many lives. The two most important advantages we have today are surveillance and containment. Local, national, and international agencies are closely monitoring domesticated animals. Birds infected with avian flu are killed, and that may be having some effect. In Vietnam, there haven’t been too many cases lately of avian flu in humans. We also know how to quarantine more effectively, limiting the activities of people who have been exposed to a sick patient to try to prevent them from spreading the disease. Somewhat reassuring is the fact that avian flu has not yet developed a great capacity to spread from person to person. Maybe we’ll get lucky with avian flu and it won’t cause a pandemic. But there is always the next thing around the bend that no one has yet heard of. We won’t be lucky forever. into bone, fat, cartilage and other types of cells. Using a patient’s stem cells, Dr. Mao says, results in replacement tissue that is completely compatible with the patient. Stem cells also can replenish the supply of cells in the implant to prevent shrinkage. Dr. Mao’s team of biologists, biomedical engineers, imaging experts, and surgeons has already shown that it can use human mesenchymal stem cells to create a long-lasting implant. The implant is created by placing these stem cells into an FDA-approved scaffold that mimics the conditions needed to turn the stem cells into fat cells. Dr. Mao found that when implanted into mice the stem cells successfully created fat cells and that the implants can retain their size and shape for at least a month. Because the implants can be molded into any size or shape, they may be used in the future for facial and breast reconstruction. Dr. Mao’s team has also been able to reconstruct the shape and dimensions of the bioengineered tissue from images of the patient’s soft tissue defects. Dr. Mao says his interest in soft tissue bioengineering grew out of his previous studies on mesenchymal stem cells and an unmet clinical need for biologically derived approach to reconstruct soft tissue. “The implants can be used for multiple purposes, but it’s really the soft tissue defects resulting from breast cancer surgeries and facial tumor surgeries that we want to be able to heal one day,” Dr. Mao says. — Susan Conova 3 N E W C E N T E R First-of-its-Kind Center to Study Chronic Lyme The Lyme & Tick-borne Diseases Research Center, the N E U R O S C I E N C E Toxins Released from Astrocytes Found to Kill Motor Neurons in ALS first university center for the study of Lyme disease in the United States, has been created at CUMC. The center, with the ongoing support of Time for Lyme Inc. and the Lyme Disease Association, brings together a multi-disciplinary team of CUMC physician-scientists who employ the most recent advances in medical technology to help unravel the complexities of Lyme and tick-borne diseases. Lyme disease is the fastest growing organismtransmitted disease in the United States. New York, New Jersey, Connecticut and Pennsylvania accounted for 64 percent of all cases of Lyme disease reported to the CDC last year. May through August are the peak months for contracting Lyme disease. Located within the New York State Psychiatric Institute, the center is headed by Brian Fallon, M.D., M.P.H., associate professor of psychiatry. It focuses on clinical research to develop novel therapies, basic science to unravel disease mechanisms and to A strocytes, cells that usually nourish neurons, are responsible for the death of motor neurons in at least some cases of amyotrophic lateral sclerosis (ALS), according to a study led by Serge Przedborski, M.D., Ph.D., co-director of Columbia’s Center for Motor Neuron Biology and Disease. The findings represent a shift in knowledge about ALS, a fatal disease that affects about 30,000 people in the United States. People with ALS become increasingly paralyzed as their motor neurons, which control movement, degenerate over the course of the disease. Until now, scientists have not known which cells to blame for the deaths: the motor neurons themselves, neighboring cells, or a combination of both. The new research steers the blame to a toxin released by neighboring astrocytes. It was published in the May issue of Nature Neuroscience, alongside an independent Harvard study that found similar results. The researchers – including postdoctoral fellows Makiko Nagai, M.D., Ph.D., Diane Re, Ph.D., and Tetsuya Nagata, “There has, perhaps, been too much emphasis placed on using embryonic stem cells as replacements for cells killed M.D., Ph.D. – and Alcmene Chalazonitis, Ph.D., senior research scientist in anatomy & cell biology, discovered the toxin in experiments with cells from mice with a rare form of ALS. In this form of ALS, the disease is caused by a mutation in the superoxide dismutase gene (SOD1), which is responsible for only a small percentage of cases in people, but is the sole known cause of the disease. To identify which cell causes motor neurons to die, the researchers mixed and matched ALS motor neurons and astrocytes with the same cells from normal mice. The ALS motor neurons thrived when paired with normal astrocytes, though they were slightly smaller than usual. Normal motor neurons, in by neurodegenerative diseases,” says coauthor Hynek Wichterle, Ph.D., assistant professor of pathology, who developed the technique used to coax embryonic stem cells into motor neurons. “Because embryonic stem cell derived motor neurons can be generated in large quantities they will initially serve as a useful tool to identify the toxin produced by astrocytes and to discover new drugs that can save neurons.” ALS researchers at CUMC have already started such investigations. Tens of thousands of compounds are being screened for their therapeutic potential by Christopher Henderson, Ph.D., codirector of the Motor Neuron Center and professor of contrast, died when paired with ALS pathology. identify better diagnostic tests, and education of medical students and physicians on how to best evaluate and treat patients. The center’s renowned collaborating scientists include Dr. Claire Fraser (led the team that mapped the Borrelia genome), Dr. Janis Weis (pathogenesis of Lyme arthritis), Dr. John Mann (translational neuroscience), Dr. Steven Schutzer (novel diagnostic tests), Dr. Ian Lipkin (foreign pathogen identification), Dr. Jorge Benach (Borrelia and co-infections), Dr. Scott Photo: Charles Manley Hammer (infectious diseases), Dr. Diego Cadavid (neuropathology and neurology), Dr. Ronald Van Heertum (neuroimaging), and Dr. Aaron Mitchell (molecular pathogenesis). The center is developing a brain bank for autopsy specimens from patients with neurologic Lyme disease to study the neuropathology of the disease. Dr. Fallon and his team recently completed a PET imaging study of chronic Lyme disease, which highlights ways that functional brain imaging can be used to identify biomarkers with potentially valuable diagnostic and treatment implications for patients with chronic Lyme disease. Lyme disease, when diagnosed and treated early, is rarely a problem. When early diagnosis is missed, the manifestations can be diverse and treatment more complex. For more information on Lyme disease research at CUMC, visit: http://www.columbia-lyme.org/. 4 ALS research team, from left: Diane B. Re, Alcmene Chalazonitis, Serge Przedborski, Tetsuya Nagata and Hynek Wichterle. The new discovery may open new avenues for diagnosis and treatment. “If our experiments faithfully model the situation occurring in ALS patients, then we can envision that blocking the putative toxin produced by mutant astrocytes may be effective in slowing the progress of this disease,” says Dr. Przedborski, who is also Page and William Black Professor of Neurology and professor of pathology and cell biology. “The presence of an astrocytic toxin also suggests that embryonic stem cells once placed into an ALS spinal cord to replace lost motor neurons will be subjected to a deadly environment. Thus, optimal response to such repair procedures may have to involve concomitant administration of drugs capable of abating the astrocytic toxicity.” astrocytes or with the ALS astrocyte’s culture medium. “It is like growing up in a bad neighborhood,” Dr. Przedborski says. “The ALS astrocytes create a bad neighborhood that has a negative influence on otherwise good neurons.” The neighborhood was just as bad for motor neurons derived from embryonic stem cells, the researchers discovered. When paired with toxic ALS astrocytes, about half of the embryonic stem cellderived neurons died, matching the death rate of natural motor neurons. Without strategies to protect motor neurons from the toxin, new neurons introduced into a patient will most likely suffer the same fate as their natural predecessors. Dr. Przedborski’s lab is working to identify the unknown toxin, or toxins. There are still many questions to answer, however, before it is known whether astrocytes play a deleterious role in all ALS patients, most of whom have normal SOD1 genes. “We do not know yet if astrocytes in patients with normal SOD1 release a toxin,” Dr. Przedborski says. “If the answer is yes, then our findings could be a critical piece of the puzzle, but we still have a long way to go.” The research was supported, in part, by the Muscular Dystrophy Association’s Wings Over Wall Street, the ALS Association, Project ALS, the NIH, U.S. Department of Defense, the Parkinson’s Disease Foundation, and the Bernard and Anne Spitzer Fund. — Susan Conova Y O U N G F A C U L T Y P U B L I C H E A L T H Craniofacial Surgeon on Mission To Improve Young Lives Understanding HIV Risk in Married Women F O R J U N E W U O F T H E C L E F T / C R A N I O FA C I A L C E N T E R , A M E D I C A L M I S S I O N T O C H I N A HIV infection among women worldwide. Now, an A D D S A G L O B A L P E R S P E C T I V E T O H E R W O R K W I T H C H I L D R E N W I T H FA C I A L D E F E C T S NIH-funded collaborative study including the Marital sex is known to be a leading risk factor for Mailman School of Public Health reveals that cultur- B read and butter surgery,” is how June Wu, M.D., assistant professor of surgery, describes the cleft lip and palate surgeries she performed during her first medical mission to China recently. But what is routine for Dr. Wu has turned out to be life-changing for two of her young patients in Xian, who are in the process of being adopted from the orphanage in which they live. “We treat the most disadvantaged segment of society – the babies and children who can’t advocate for themselves,” Dr. Wu says. “This operation gives them a better chance of being adopted, or at the very least improves their appearance so they can integrate into society.” Dr. Wu, P&S’96, went to China this past May when Jeffrey Ascherman, M.D., associate professor of clinical surgery and director of the Cleft/Craniofacial Center at CUMC, was unable to make what would have been his seventh overseas medical mission. “I wasn’t originally supposed to be the physician going on this mission, but the experience sold me on the idea of going on more of them,” Dr. Wu says. Conditions in China were challenging. Children with cleft lip or palate are often more severely disfigured there than in the United States, because their problem has often been neglected. A child born with a severe cleft lip and palate in the United States may be fitted within a few weeks after birth with a retainer that slowly forces the two sides of the palate together. By the time surgery is performed, when the baby is between 3 to 6 months old, the sides are in a more normal position. This reduces the size of the cleft and makes the operation somewhat less difficult. It also reduces the chances that the repair will pull apart after surgery, and improves facial aesthetics. But on her trip Dr. Wu saw children as old as two, whose clefts, without treatment, had continuously enlarged. These were trying conditions for any surgeon, but particularly for one who is accustomed to spending an hour at the beginning of an operation painstakingly delineating her surgical plan – the blueprint for the operation – on a patient’s face. “I suppose I’m a bit of a perfectionist,” she says. Dr. Wu also has an artistic sensibility that infused her choice of medical specialty. “I knew in my first year of medical school that I wanted to be a plastic surgeon. I like plastic surgery because it’s not just technical, there’s an artistic component,” she says. After medical school, Dr. Wu completed an integrated general and plastic surgery residency at Montefiore and was “ al expectations and changing attitudes about love and marriage encourage male infidelity. Jennifer Hirsch, Ph.D., associate professor of sociomedical sciences and lead author, conducted the six-month study in a rural Mexican village. She found that the forces that promote extramarital sex – access to alcohol and women; patterns of economically driven mobility; and the segregation of men’s and women’s “spheres” in society and in family life – are pervasive and extremely powerful. While the overall HIV infection rate in Mexico is low at 0.3 percent, certain groups have higher levels. In returning migrants, for example, infection rates are as high as about 1 percent because many men travel to areas such as New York City, where HIV-prevalence is much higher and where they engage in unsafe extramarital sex during their long absences. When migrant workers return to their Mexican wives, they are said to be on their honeymoon and resume marital sexual relations. June Wu performs surgery in China. drawn to pediatric craniofacial surgery. “Plastic surgery is often associated with adults trying to achieve a flawless appearance,” Dr. Wu says. “But for children, plastic surgery often helps a child look more average. In many cases, children would be shunned and never able to function normally in society without surgery. Surgery puts them on a level playing field and also relieves the heavy emotional toll on the family.” After finishing her fellowships in craniofacial surgery and vascular anomalies at Children’s Hospital of Boston, Dr. Wu was recruited to Columbia by Dr. Ascherman two years ago. “I’ve known June since she was a medical student, and when we started expanding the pediatric surgery program, I knew she would be a wonderful addition,” Dr. Ascherman says. “June is very committed to children, and since she began, she’s been a very important part of our team.” Dr. Wu is already planning to return to China next year, both to treat children and help her Chinese colleagues learn the latest surgical techniques. “The trip was definitely a learning experience for me,” Dr. Wu says. “The conditions are very different and challenging, but the work is extremely rewarding. I’m very much looking forward to going back.” “Women are infected by their returning husbands, the very people with whom they are supposed to be having sex and, according to social conventions of Mexico, the only people with whom they are ever supposed to have sex,” says Dr. Hirsch. Dr. Hirsch collaborated with anthropologists from Brown, University of Toronto, University of Washington, and Washington University who worked at sites from New Guinea to Vietnam and reported similar findings. These findings have farreaching implications for public health policy, especially with respect to U.S. funding for AIDS prevention, which requires that a third be spent teaching — Susan Conova abstinence and monogamy. “If you tell people to Center’s Team Approach Ensures Best Results for Cleft Lip and Palate Defects For the approximately 1 in 700 children born with cleft lip or palate in the United States, a team of specialists is often required to repair the defect and obtain the best possible outcome. Since such children usually speak with nasal intonations that may be hard to understand, speech therapists usually begin working with the child as soon as he or she begins to speak. Otolaryngologists manage the frequent ear infections many children experience because of malfunctioning Eustachian tubes. And oral surgeons graft bone into the gumline when bone is lacking, to hold the child’s permanent teeth in place as they grow in. The Cleft/Craniofacial Center at CUMC coordinates such care among all specialists. The center was created in 1994 by Jeffrey Ascherman, M.D., associate professor of clinical surgery and the center’s director. Since then, center physicians have treated hundreds of children with cleft lip/palate and other craniofacial abnormalities. be abstinent until marriage, but their greatest risk of HIV infection actually comes after marriage, it’s not useful advice,” says Dr. Hirsch. Dr. Hirsch recommends making condoms available in places where men are likely to meet partners for extramarital sex and exploring ways that migration policies contribute to marital risk. “We found that it’s not as if there are men who engage in extramarital sex and men who don’t. There are contexts in which all men are much more likely to,” she says. “We have to do a better job of thinking about what those contexts are, and working within that framework.” 5 M A I L M A N S C H O O L R E S E A R C H B R I E F S R E S E A R C H In Search of the Honeybee Killer The potentially devastating phenomenon known as colony collapse disorder (CCD), which is decimating bee hives across the country, has received much publicity lately. Now, W. Ian Lipkin, M.D., the Jerome L. and Dawn Greene Professor of Epidemiology at the Mailman School of Public Health, who is part of a consortium actively investigating CCD, says the group may have found a pathogen responsible for die-offs in the majority of colonies. Bees are integral to the world’s food supply, pollinating more than 90 primary agricultural crops valued at about $15 billion. Colony collapse disorder is not a new phenomenon, but it is occurring at an unprecedented rate. Beekeepers began reporting major losses in November 2006. As of April, more than a quarter of bee colonies in the United States were lost with no signs of abatement. The honeybees in stricken colonies often simply vanish, leaving only a few workers and a queen behind. Scientists have many theories as to a possible cause of CCD. Everything from electromagnetic radiation to stress to an infectious agent has been cited. Dr. Lipkin, who headed the lab that discovered West Nile virus in 1999, has the task of teasing out the infection piece of the puzzle, using the same high-throughput DNA analysis that he uses to identify viruses, bacteria and parasites behind human diseases. Single Protein May I.D. Aggressive Cancers The most aggressive breast cancers may be detected by the levels of a single protein called stathmin, according to a new study led by Ramon Parsons, M.D., Ph.D., the Avon Foundation Professor of Pathology and Medicine, and Åke Borg of Sweden’s Lund University. In a retrospective analysis of samples from tumor banks, the researchers found that survival after diagnosis for breast cancer declines 8 percent to 16 percent for every one point increase in stathmin activity, which is scored on a scale from 0 to 12. “Patients with these types of aggressive biophysics and in neuroscience, the study tumors have few good treatment options found that the “Met” form of BDNF pre- and there is a real need for effective drugs,” vents inactive neurons from withering away says the study’s first author, Lao Saal, during brain development. BDNFmet – in P&S’09. “The good news is that inhibiting which a methionine amino acid replaces the the PI3K/PTEN pathway has enormous more common valine at position 66 in the potential for improving survival and there protein – is present in about 10 percent of are many attractive therapeutic targets in the population. the pathway that may be exploited.” The study focused on the olfactory bulb. Because microarrays are expensive and The advantage of this brain region is that hard to use in clinical settings, the during the initial wiring of the sense of researchers also looked for a simpler way to smell, thousands of neurons compete detect PI3K/PTEN defects. Simple immun- against each other for access to a few odetection of stathmin proved an accurate hundred cells. Active neurons have the surrogate for the full signature and may advantage in this competitive playing field. evolve into a clinically useful diagnostic test. BDNFmet reduces this competition and The research was supported, in part, by the lets more inactive neurons gain access to NIH and the Avon Foundation. the cells in the olfactory bulb, the Neuronal Competition Leads to More Psychiatric Disorders researchers found. had been unclear because previous assays Children born with an uncommon form of could not detect all defects in the pathway. the brain. Dr. Gogos says that one way a certain brain protein are approximately The new study identified a group of 246 BDNFmet may protect against these disor- 50 percent less likely to develop obsessive- genes that form a genetic microarray signa- ders is by allowing more neurons to survive compulsive disorder, depression and other ture that detects aberrant PI3K/PTEN path- the competition. psychiatric diseases during childhood. The work was supported by the NIH, a way activity. Breast, prostate, and bladder A new study by CUMC researchers now Burroughs Wellcome Fund Career Award in cancers exhibiting this signature had very shows why this form of brain-derived neu- the Biomedical Sciences, the Whitehall poor prognosis, confirming the PI3K/PTEN rotrophic factor (BDNF) may be so protective. Foundation and NARSAD: The Mental Stathmin predicts survival, the researchers found, because it mirrors the activity of an entire molecular pathway inside cancer cells. When active, the PI3K/PTEN pathway promotes tumors in model systems. But its prognostic significance in human cancers pathway has a major impact on patients. Led by Joseph Gogos, M.D., Ph.D., Psychiatric disorders in children may stem from an excessive loss of compromised neurons during competition in other parts of Health Research Association. assistant professor of physiology and cellular Dr. Lipkin joined the investigation in December at the request of Dr. Diana Cox-Foster, a scientist at Penn State who is coordinating a nationwide team of CCD researchers that includes scientists from Penn State, Garvey Education Grants continued from Page 2 Columbia, the University of Arizona and the USDA. “I was initially hesitant to sign on because bees are not among the organisms we normally study,” Dr. Lipkin P E N E L O P E B U S C H M A N G E M M A , M . S . , A P R N , assistant professor of clinical nursing; Marlene McHugh, M.S., FNP, assistant pro- fessor of nursing; and Anita Nirenberg, M.S., NP, assistant professor of clinical nursing, School of Nursing. “Creating an Educational Partnership says. “But Dr. Cox-Foster was persuasive. After discussions with the pathogen discovery team here – Thomas Briese, Gustavo Palacios, Lan Quan and Sean in Palliative and End of Life Care.” K AT H L E E N H I C K E Y, F N P, A N P, ED.D., assistant professor of nursing, School of Nursing. “REAL: Remote Electronic Conlan – we jumped in with both feet.” The Greene Lab joined a formidable research initia- Arrhythmia Learning.” tive. “This is the largest single effort to address CCD,” Dr. Lipkin says. “The researchers meet by phone every three days, and smaller groups are in constant contact P A T R I C I A M I L L E R , E D . D . , associate professor of clinical rehabilitation medicine, and Mathew Maurer, M.D., Herbert Irving Assistant Professor of Clinical Medicine, P&S. “Facilitating Change to Promote Health in Older Adults: An Interdisciplinary Education Program.” throughout the day. The result is that the project, just eight months old, is moving very rapidly.” Early on, the consortium determined that infec- LY N N E QUITTELL, M . D . , clinical professor of pediatrics, P&S,. “Intercontinental Real Time Global Health Teaching: Creating University Synergies – A Model for the Future.” tious agents must play a critical, if not exclusive, role in CCD. To determine this, they looked at repopulation of affected hives. Ordinarily, bees will recolonize T R A N S P L A N T A T I O N C E L E B R A T I O N abandoned hives, but those that have succumbed to CCD are rendered untouchable. However, if combs from CCD hives were irradiated, the bees would repopulate the combs, pointing to an infectious pathogen. A non-biological agent would not have dissipated with irradiation. The next challenge was to positively identify that pathogen. Materials were collected from hives affected by CCD as well as from still-healthy hives. Using high throughput genetic analysis and applying algorithms that allowed them to identify possible culprits, the researchers screened for all types of infectious agents: bacteria, viruses, parasites, mites, and fungi. They then compared the genetic profiles of the suspicious targets across individual colonies in search of the “smoking gun” that was present in affected colonies but absent in healthy colonies. Once the pathogen is definitively identified, the plan is to develop strategies to outsmart it, perhaps by developing transgenic bees that are resistant to 6 Nearly 1,000 organ transplantation patients, donors and their families reunited with their medical teams at the West 168th Street Armory in May to celebrate a second chance at life. Columbia physicians are working on many fronts to improve clinical outcomes and quality of life for those who need transplants. In lung transplants, for example, the Center for Lung Disease and Transplantation has pioneered scientific investigations to better understand and treat major post-transplantation complications. In heart transplants, infection, drugs to treat it, and tools for surveillance a major focus is in the area of left ventricular assist devices (LVADs). Kidney transplantation, liver regeneration, and mechanisms that to facilitate containment. affect diseases of the pancreas are other areas receiving research attention. HIV Battlefront continued from Page 1 lished to carry out the next generation of HIV/AIDS vaccine, prevention, and treatment research. Drs. Hammer and El-Sadr have been fighting AIDS since the epidemic began in the early 1980s, when patients filled hospitals with a mysterious disease that had no known cause, no treatment, and no hope for survival. Though the outlook for people with HIV in the United States has dramatically improved since then, New York City is still the epicenter of the HIV/AIDS epidemic in this country. More than 100,000 New Yorkers are living with HIV and the city has more AIDS cases than San Francisco, Los Angeles, Miami and Washington D.C., combined. Progress in further reducing the spread of the virus has also stalled, and in some groups infections are on the rise. Among young gay men of color in New York City and several other urban areas in the United States, the virus is spreading at a rate twice that in Uganda. The trends in New York City reflect what is happening across the country: More and more women are getting HIV, and blacks and Latinos are disproportionately affected. Inner Cities See HIV Rise “Cities in the United States with disenfranchised populations face similar problems,” Dr. Hammer says. “Our inner cities present us in some respects with our own ‘developing world’ challenges.” The Columbia Collaborative HIV/AIDS Clinical Trials Unit gives people with HIV in northern Manhattan allimportant access to clinical trials. The unit conducts clinical trials for drugs to treat AIDS itself, as well as the co-infections that are common among people with HIV, and the debilitating side effects of current AIDS treatments. Clinical trials give patients access to new drugs and new strategies to make treatments more effective, more durable and more tolerable,” Dr. Hammer says. “The advances we’ve seen to date would not have been possible without a commitment on everyone’s part to a strong clinical research effort.” With medical care integrated into the research clinics, trial participants receive the best HIV treatment available. “We don’t just recruit people for studies. We reach out to the community to get important feedback, to learn what kinds of studies they want to see, and to provide useful information to help people protect themselves and maintain their health,” Dr. Hammer says. “We enter into partnerships with HIV-infected patients and strive to provide them with decades of survival. Our goal is a full, productive life for people with HIV infection; the disease can now be considered chronic and manageable over the long-term.” Despite the effectiveness of today’s antiretroviral drugs, vaccines remain the best chance of ultimately beating HIV. The Columbia Collaborative HIV/AIDS Clinical Trials Unit – the only NIHfunded HIV Vaccine Trials Network site in the city (in collaboration with the New York Blood Center and principal investigator, Dr. Beryl Koblin) – is currently testing vaccines in Phase I and II trials, including early efficacy trials. The current generation of vaccine candidates may not prevent HIV infection, but may alter its course once an individual becomes infected. “We hope these vaccines can slow the progress of the disease in someone who becomes infected,” Dr. Hammer says. “By reducing the amount of virus in the body, the vaccines may also help reduce further transmission in the population.” Since a vaccine that completely prevents infection may be a decade or more away, the Center for Innovative Research to Control AIDS will continue Dr. ElSadr’s efforts to identify other means of prevention, including vaginal microbi- cides that would give women more control over prevention. Other efforts include behavioral interventions and the use of antiretroviral drugs as a means to prevent acquisition of HIV. “Even with a vaccine available, other prevention strategies should still be useful,” Dr. El-Sadr says. “One intervention will not bring the transmission rate down to zero, so there is room for a menu of effective preventions, with A W A R D S & H O N O R S Columbia President Lee Bollinger, Provost Alan Brinkley and the Trustees have approved a $2 million initiative from the Professional Schools’ Diversity Council to help diverse junior faculty develop scholarly profiles to become eligible for tenure. Departments can apply for funds for research grants to some targeted to specific populations.” support the scholarly work of untenured colleagues. Goal: Learn Status/Receive Care The CUMC recipients and their projects: L U I S A One big impediment to prevention strategies that is often forgotten, Dr. ElSadr says, is the large numbers of people – about one in four in New York City – unaware that they are infected with HIV. Because most HIV infections are transmitted by people who do not know they have the virus, simply increasing the number of people who know their status may significantly reduce the spread. Such knowledge coupled with behavioral interventions can go a long way to stemming the spread of HIV. “Studies show that people who know their status adopt appropriate behaviors to reduce the spread of the virus,” Dr. ElSadr says. “People who find out they’re negative are motivated to adopt behaviors to stay that way. And people who are positive adopt behaviors to prevent spread to others.” The advent of rapid HIV tests that can produce results in 10 minutes has led Dr. El-Sadr to introduce testing in nontraditional settings, including emergency departments, in outpatient and inpatient services at Harlem Hospital Center, and at community street fairs. “When we find people who are positive, counselors take them by the hand to the clinic and we assure them we will take care of them,” Dr. El-Sadr says. “We’re always surprised by the number of individuals we find who never suspected that they had HIV.” — Susan Conova BORELL, PH.D., D.D.S., assistant M . P. H . , professor of epidemiology and assistant professor of dentistry, to investigate health disparities within Hispanic communities; GEORGE JENKINS, D . M . D . , assistant professor of clinical dentistry, to start research into the triage population at the College of Dental Medicine to allow for better needs assessment of the community being served and the identification of health problems associated with particular populations; K A T H I E - A N N JOSEPH, M.D., assistant professor of surgery, to determine what biological mechanisms impact breast cancer recurrence and survival rates in African-American women; N A A OYO K W AT E , PH.D., assistant professor of sociomedical sciences, to research the health effects of residential racial segregation or mixed living areas on minority health; P E T E R M . P. H . , MUENNIG, M.D., assistant professor of health policy and management, to research qualitative properties of stress and how prestige affects the stress response; MIGUEL M U N O Z - L A B O Y, M . P. H . , DR.PH, assistant professor of sociomedical sciences, to investigate sexual risk behaviors among bisexual Latino women and men; G U S T A V O P A L A C I O S , P H . D . , assistant professor of clinical epidemiology, to further his research on the importance of environmental triggers in individuals genetically disposed to disease, Columbia HIV/AIDS Clinical Research Sites especially the role of viruses in the development of The research led by Drs. Hammer and El-Sadr is not possible without collaboration with other researchers who bring a wealth of type-1 diabetes mellitus; D E A N P R E D D I E , M . D . , expertise and have gained the trust of their communities. Clinical research sites and their leaders are listed below. assistant professor of clinical medicine, for a pilot proj- n HIV Prevention and Treatment Research, CUMC, PI: Scott Hammer, M.D. (treatment, vaccine trials) ect on home dialysis in preparation for establishing a n Harlem Family Center, Harlem Hospital, PI: Wafaa El-Sadr, M.D. (treatment and prevention trials) home hemodialysis program at Columbia; C A R L O S n New York Blood Center, Bronx, PI: Beryl Koblin, Ph.D. (vaccine and prevention trials) R O D R I G U E Z , M . D . , M . P. H . , assistant professor n New York Blood Center, Union Square; PI: Beryl Koblin, Ph.D. (vaccine and prevention trials) of clinical medicine and clinical epidemiology, to n IMPAACT at CUMC; PI: Philip LaRussa, M.D., professor of clinical pediatrics (maternal, pediatric and adolescent treatment and research cardiovascular disease in Hispanic popula- prevention trials) tions; D I A N A R O M E R O , P H . D . , assistant pro- n University of Medicine & Dentistry of New Jersey, PI: Sally Hodder, M.D. (prevention trials) fessor of population and family health, to conduct sec- n Bronx-Lebanon Hospital Center, PI: Jessica Justman, M.D., assistant professor of clinical medicine (in Epidemiology) ondary analyses of the National Survey of Family (microbicide trials) Growth to explore social and economic status as it relates to sexual and reproductive health and family growth; I L Y A S W A S H I N G T O N , P H . D . , assistant professor of ophthalmic science, to launch research on age-related macular degeneration; PAT R I C K W I L S O N , P H . D . , assistant professor of sociomedplease see Page 8 7 A W A R D S & H O N O R S Nursing Leader continued from Page 1 continued from Page 7 ical sciences, to examine situational factors that promote high-risk sex among HIV-positive men who have sex with other men. L E E G O L D M A N , M . D . , executive vice president, was awarded the 2007 John Phillips Memorial Award by the American College of Physicians (ACP) at the college’s annual medical education meeting in San Diego in April. The award is bestowed for outstanding work in clinical medicine, including all phases of clinical research or the practice of medicine. The award was established to honor Dr. Phillips, the late governor and regent of the ACP. J E S S I C A K A N D E L , M . D . , associate professor of surgery, has been elected a member of the American Surgical Association. She joins others from the department who are already members. JENNIFER LEVINE, M.D., M . S . W . , a pedi- atric oncologist and medical social worker, has been named an CureSearchAflac Young Investigator in Adolescent and Young Adult Oncology for 2007-2009. J E F F R E Y L I E B E R M A N , M . D . , chairman of the Department of Psychiatry at P&S and director of the New York State Psychiatric Institute, received the 2007 Adolph Meyer Award at the American Psychiatric Association (APA) meeting in May. The award is APA’s kind in the world. Now, about 200 schools nationwide are setting up clinical doctorate programs, in the wake of an October 2004 position statement from the American Association of Colleges of Nursing that called for moving the current level of preparation required for advanced nursing practice roles from the master’s degree to the doctorate level by the year 2015. An urgent need for nurses with such advanced training is necessary in light of looming practitioner shortages. Almost all states will have a shortage of primary care physicians by 2020, according to a 2006 report from the American Academy of Family Physicians. “Normally, nurse practitioners care for patients in ambulatory care settings,” says Judy Honig, DrNP, EdD, CPNP-PC, who directs the Doctor of Nursing Practice program. “These nurses will be uniquely prepared as primary care providers to see patients across a variety of settings. With more chronic illness and an aging population, there’s a growing need for more primary care, and the DrNP will be qualified to provide that.” It’s all part of a sea change for nursing as a profession – a change in which Columbia is playing a critical role. “We have the largest number of applicants to the School of Nursing that we’ve ever had, and they are entering because of the way the profession is evolving,” says Jennifer Smith, DrNP, M.P.H., M.B.A., senior associate dean. “Nurses are changing the face of health care.” The stage was set for nurses’ evolving role as primary care providers by programs like Columbia Advanced Practice Nurse Associates (CAPNA), the innovative nurse practitioner-run practice based at East 60th Street. While other nurse practitioner-run primary care practices were already in existence when CAPNA opened its doors in 1998, the program differs from most others in that its nurse practitioners are reimbursed at the same rate as doctors. They also have admitting privileges to New York-Presbyterian Hospital. These faculty advanced practice nurses diagnose and treat illness and perform physical exams and tests, making nearly 80 referrals per month to Columbia specialists. “We are well regarded by CUMC physicians,” says Dr. Smith. “That we’ve thrived for 10 years is a testament to the kind of care we deliver, as everyone in New York wants to go to the best specialist. But it’s so hard to find primary care now that we fill a niche with our focus on prevention and education. In the long run this not only helps patients live healthier lives, but also saves money. And when patients who have insurance have a choice and choose us, that really says something. They like the kind of health care our nurse practitioners are able to give.” Just two decades ago, Columbia’s School of Nursing was struggling with low enrollments and the changing role of women in the workforce – particularly difficult for a profession that is still primarily female. But Mary O’Neil Mundinger, DrPH, RN – appointed dean in 1986 – brought the school roaring back. She required all nurses on the fac- highest honor. Dr. Lieberman received the award for his stellar and outstanding contributions to the ulty to either have a faculty practice or a program of research. That attracted experienced clinicians and researchers, who stepped into the classroom to teach what they loved, and soon Columbia began accumulating an impressive list of accomplishments: n n n n n the first randomized trial comparing nurses and physicians in primary care – and demonstrating that health outcomes were equal the highest per capita NIH faculty research funding the first and only nursing school to be designated a World Health Organization collaborating Center for the International Nursing Development of Advanced Practice the first and only Nurse Principal Investigator in the NIH’s priority funding to establish 21 translational research centers the first nursing school faculty to gain admitting privileges at a major teaching hospital Today, students and faculty at the SON practice at more than 200 sites in New York City, applications to the school are up 30 percent and the program ranks 13th in NIH research funding – up from 27th in 2005. “The new nurse is a researcher, a teacher, and a practitioner,” says Dr. Smith. “Nurses are helping to drive changes in health care, with an understanding of the importance of a focus on quality, education and prevention. Columbia is in the forefront of that movement.” — Gina Shaw Advances in Nursing Research advancement of psychiatry through research. School of Nursing faculty are among the nation’s most prominent researchers in the field. They also participate in interdisciplinary teams with P A N O S P A P A P A N O U , D . D . S . , P H . D . , profes- sor of dentistry and director of the Division of faculty from medicine, neurology, ophthalmology, public health and bioinformatics and are the recipients of multiple NIH funded grants. n Suzanne Bakken, DNSc, R.N., Alumni Professor of Nursing and professor of medical informatics, a nationally known expert in bioinfor- Periodontics, has been elected councillor of the matics, has received more than $1 million in federal research grants this year alone. Her study, “Wireless Informatics for Safe and Periodontal Research Group of the International Evidence-based (WISE) APN Care,” is supported by the Health Resources and Services Administration. The National Cancer Institute Association of Dental Research. awarded her a grant to study integration of resources from the Institute’s Cancer Information Service into an existing PDA-based mobile decision-support system. B R I A N S C U L L Y , M . D . , professor of clinical med- icine and infectious diseases and L U C I E N C O T É , n M . D . , special lecturer in neurology, Gertrude H. Centers for Disease Control and Prevention. Her expertise in infection control was recently recognized with a $2 million, two-year grant Sergievsky Center, have been chosen by CUMC’s Society of Practitioners to receive its Elaine Larson, Ph.D., R.N., professor of pharmaceutical and therapeutic research, has received multiple awards from the NIH and the from the CDC for a study of non-pharmaceutical interventions for pandemic influenza. 2007 n Joyce Anastasi, Ph.D., DrNP, R.N., FAAN, LAc., Helen F. Pettit Professor of Clinical Nursing, is a renowned expert in HIV/AIDS. Her Distinguished Practitioner Awards. The awards were research focuses on symptom management and the use of alternative therapies to complement traditional interventions for patients presented at the society’s June meeting. Both were with HIV and has been funded by the NIH for more than 10 years. honored for their clinical expertise, contributions to clinical medicine, and the inspirational roles they have played for clinicians and students. n Mary Woods Byrne, Ph.D., M.P.H., CPNP, professor of nursing and the Stone Foundation and Elise D. Fish Professor of Clinical Health Care for the Underserved, runs a federally funded research program focused on the assessment and early intervention for infants, toddlers and children and their caregivers at risk for sub-optimum development and inadequate parenting. Her current NIH-funded P E T E R S H A P I R O , M . D . , associate professor of research focuses on parenting and child outcomes in a prison nursery. clinical psychiatry and associate director of the Psychiatric Consultation/Liaison Service at NYP, has Save the Date: White Coat Ceremonies received the 2007 Bakken Award from the Bakken The College of Physicians & Surgeons The College of Dental Medicine Time: 12:30 p.m. Time: 2:00 p.m. Date: Aug. 24, 2007 Date: Aug. 24, 2007 Location: Alumni Auditorium, P&S building, 630 W.168th St. Location: Rm. 401, Hammer building, 701 W. 168th St. Heart-Brain Institute of the Cleveland Clinic. 8