* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download null
Self-experimentation in medicine wikipedia , lookup
Declaration of Helsinki wikipedia , lookup
Race and health wikipedia , lookup
Medical research wikipedia , lookup
Adherence (medicine) wikipedia , lookup
Public health genomics wikipedia , lookup
Nanomedicine wikipedia , lookup
Preventive healthcare wikipedia , lookup
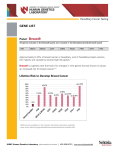
Explor i ng r esearc h at th e U n iversity of N ebraska M edical C enter discover UNMC an d beyon d... targeted delivery to ailing bones FA L L 20 08 discover UNMC exploring research at the success against the odds University of Nebraska Medical Center and beyond... UNMC Discover is published twice a year by the Vice Chancellor for Research and the Department of Public Affairs at the University of Nebraska Medical Center. The magazine is supported by UNeMed Corporation, the technology transfer organization for UNMC. Issues of the magazine can be found at www. unmc.edu, News link. Permission is granted to reprint any written materials herein, provided proper credit is given. Direct all requests to ekumru@unmc. edu. Subscriptions to UNMC Discover are free. To subscribe, go to unmc.edu/discover. UNMC’s mission is to improve the health of Nebraska through premier educational programs, innovative research, the highest quality patient care and outreach to underserved populations. UNMC is accredited by The Higher Learning Commission of the North Central Association of Colleges and Schools (HLC-NCA) and enjoys full accreditation of all its professional academic programs. UNMC does not discriminate in its academic, employment or admissions programs, and abides by all federal regulations pertaining to same. Director of Public Affairs: Renee Fry, J.D. Senior Associate Director: Tom O’Connor Managing Editor: Karen Burbach Publications Editor: Elizabeth Kumru Design: Daake Design Photography: Scott Dobry Elizabeth Kumru Andrew Nelson Dewayne Gimeson, Chadron State College Research Advisory Board: Thomas Rosenquist, Ph.D. • Kenneth Cowan, M.D., Ph.D. Courtney Fletcher, Pharm.D. • John Gollan, M.D. The research enterprise at the University of Nebraska Medical Center continues to grow, against the odds. When the economy struggles, institutions often view their research dollars as discretionary budget items that can be reduced, rather than seeing basic discovery as the engine that ultimately revives the economy. The National Institutes of Health (NIH) is an example of this phenomenon. The NIH is the most successful and most respected biomedical research institution in the world. Its support of the basic sciences is unique. For 50 years or more, the NIH has provided the basis for most of the major discoveries in human biology. These discoveries have led to improved therapies, which have prolonged and enriched lives. Nevertheless, over the past few years, the annual funding increases for the NIH have failed to meet inflation and the availability of NIH dollars has fallen by about 25 percent. We are losing a myriad of opportunities to support wonderful, innovative projects. We do not know which discoveries will most directly lead to improved diagnosis, treatment or cure; but we do know no gains are made without discovery. We hope and trust that our leaders in government and in the private sector will see the grave error inherent in this strategy and change directions, soon. Nevertheless, the competitive environment is intense and for many institutions, disheartening. But at UNMC, we have had continuous gains. The first quarter for this fiscal year set a new record for total extramural research funding of more than $32 million. This remarkable achievement is the result, in part, of the determined efforts of a reliable corps of deans, directors and department chairs who understand well that the principal role of the academic health sciences center is discovery. These men and women have worked hard and used great vision to keep or recruit outstanding scientists and nurture them. Of course, the fundamental strength of our research enterprise is in the scientists themselves, whose creativity and performance under duress has been remarkable. This issue of UNMC Discover focuses on a few of these admirable men and women. It is impossible to read about their excellent, innovative work and not see with greater clarity why UNMC is succeeding against the odds, and why it is so important to expand the research enterprise globally. Robert Lewis, Ph.D. • James Linder, M.D. Keith Mueller, Ph.D. • Rubens Pamies, M.D. Jeffrey Payne, D.D.S. • John Reinhardt, D.D.S. Warren Sanger, Ph.D. • James Shull, Ph.D. Joe Sisson, M.D. • Shelley Smith, Ph.D. Virginia Tilden, D.N.Sc. • Paula Turpen, Ph.D. Margaret Wheelock, Ph.D. • Irving Zucker, Ph.D. Tom Rosenquist, Ph.D. UNMC Vice Chancellor for Research FA L L 20 08 contents lotus leaf and fake diamonds lead to better orthopaedic implants Nature inspires UNMC scientist 4 New coating makes implants more durable apathy – why should you care? Drug jolts people to care about their chronic illness 7 growing our own UNMC researchers mentor junior investigators 10 i targeted delivery New system taxis drugs to ailing bones 14 the care connection i NursingINNOVATION study examines new model of care for chronic disease 20 determined to make earlier diagnosis a reality Pancreatic cancer eludes detection – but not for long 22 under the microscope Clinical researcher co-authors largest study on HIV drugs 26 Lotus leaf and fake diamonds lead to better orthopaedic implants by Chuck Brown Inspiration often comes from unexpected places. Just ask UNMC’s Fereydoon Namavar, Sc.D. In the case of a coating he designed for orthopaedic implants, the scientist – who worked on NASA’s Mars Rover, Star Wars and optical communications projects before entering the world of biomedical research 10 years ago – found inspiration in his mother-in-law’s jewelry case and the leaves of the lotus flower. One day a few years back, Dr. Namavar listened as his mother-in-law shared how much she liked her cubic zirconia jewelry – except for one thing that bothered her. “When it would get wet, it would fog up,” said Dr. Namavar, professor and director of the nano-biotechnology laboratory in the UNMC Department of Orthopaedic Surgery. fall 2008 While bad news for his mother-in-law, this was an epiphany for Dr. Namavar. A common issue with implants is wear and tear because joint surfaces rub together. This can lead to repeat surgeries, as well as send an unhealthy mix of wear particles into a person’s blood stream. The wear and tear happens, in part, because surfaces used on orthopaedic implants are too soft and lack the ability to stay wet. With orthopaedic implants, ideally, it is important that one of the two contact surfaces be wettable, while the other is hydrophobic or rejects water, Dr. Namavar said. He needed opposites, a Yin and a Yang. “If both were wet, the surfaces would stick together and drastically increase friction,” Dr. Namavar said. “But, when Atomic force microscopy image of cubic zirconia showing pyramidal nanostructures with sizes ranging from 130 to 210 nanometers. you have these opposites together, you have lower friction and smoother motion on the surface.” Dr. Namavar’s ears immediately perked up when his motherin-law complained about how cubic zirconia fogs up when wet. “I knew I had my substance,” he said. “I thought, ‘here is a material that could be hard and also seems to be able to stay wet.’” In other words, cubic zirconia might work just as well in a hip joint as it does in a gold tennis bracelet. As he designed his implant coating, Dr. Namavar wanted to alter the properties of cubic zirconia to attain maximum wettability. The cubic zirconia would provide the Yin (wet) to his existing model, the lotus leaf, the Yang (dry). The lotus leaf is considered a symbol of purity in many cultures because of its self-cleaning properties. “When a drop of water hits a lotus leaf, it rolls off the surface, washing away dirt and dust,” Dr. Namavar said. “This is because the lotus leaf is water resistant, or hydrophobic.” Hydrophilic (wettable) and hydrophobic properties of substances are actually flip sides of the same coin and thus identical at a nanostructure level, he said. As a result, Dr. Namavar decided to alter the physical properties to mimic the hydrophobic lotus leaf to make his coating super-hydrophilic or more wettable. To alter the cubic zirconia, Dr. Namavar uses a technique called ion-bombardment, during which he exposes a substance to a large amount of ions – atoms that have gained an electrical charge by losing an electron. Dr. Namavar’s team uses a special ion beam assisted deposition (IBAD) process to enhance the zirconia’s hardness and ability to stay wet. They are one of the few research teams at an academic institituion in the country that uses the IBAD process. “Utilizing billions of energetic ions as an ionic hammer, we have forged nano pyramidal structure films possessing combined properties of super-hardness and complete wetting behavior,” Dr. Namavar said. With his coating made of altered pure cubic zirconia, Dr. Namavar knew he had created a harder, wettable substance that stands to improve the life of orthopaedic implants. By altering the hydrophilic (wettability) properties of these novel materials, Dr. Namavar also created a substance that bones like to grow on. Tests done in collaboration with John Jackson, Ph.D., associate professor, pathology and microbiology, and Graham Sharp, Ph.D., professor, genetics, cell biology and anatomy, have shown that bone stem cells actually attach to and grow on Dr. Namavar’s coating. “I knew I had my substance. I thought, ‘here is a material that could be hard and also seems to be able to stay wet.’ ” Fereydoon Namavar, Sc.D. UNMC discover “We hope this leads to prolonged life of orthopaedic implants and fewer revision surgeries due to reduced friction and wear of the implant, as well as enhanced bone growth.” Fereydoon Namavar, Sc.D. Thomas Gustafson, intern, prepares the ion beams assisted deposition (IBAD) system that produces the nanocrystalline coating. fall 2008 “It seems that our pyramidal nano-structures have a charge distribution, which the cells find hospitable,” he said. “This was an unexpected development and one we were thrilled to encounter.” Dr. Namavar and his team plan to do tests on animal models. “We hope this leads to prolonged life of orthopaedic implants and fewer revision surgeries due to reduced friction and wear of the implant, as well as enhanced bone growth,” Dr. Namavar said. Dr. Namavar said his work has been aided by strong support from Kevin Garvin, M.D., chairman of the department of orthopaedic surgery, and Hani Haider, Ph.D., an associate professor of orthopaedic surgery. Collaborations have been important to his work, Dr. Namavar said. A grant from the Nebraska Research Initiative has allowed him to work with Barry Li Cheung, Ph.D., of the chemistry department at the University of Nebraska-Lincoln, and Renat Sabirianov, Ph.D., and Wai-Ning Mei, Ph.D., of the physics department of the University of Nebraska at Omaha. Dr. Garvin said Dr. Namavar’s coating could prove particularly important as the health care system faces a surge in the elderly population, which will lead to more implant surgeries. “By making implants last longer, this coating could make life better for patients and physicians alike,” Dr. Garvin said. “Patients, of course, may be able to avoid the discomfort and inconvenience of multiple surgeries, which also would take stress off a system that already is overburdened.” ap-a-thy, n., 1. lack of emotion. 2. lack of interest; listless condition; indifference. apathy Why Should You Care? by Tom O’Connor It’s easy to be apathetic. It’s something we all experience. Some days we just wake up and have no motivation. Nothing seems to matter. However, in some chronic diseases apathy turns into a clinical syndrome characterized by poor initiation, loss of motivation, indifference and lack of persistence. Apathy syndrome impairs self-management behaviors, leads to functional decline, poor compliance with treatment and generally poor outcomes in chronic diseases. That’s why two UNMC physicians – Prasad Padala, M.D., and Cyrus Desouza, M.D. – zeroed in on apathy as one of the key culprits in patients with Alzheimer’s disease and chronic conditions such as diabetes and obesity. Dr. Padala, assistant professor, psychiatry, and Dr. Desouza, associate professor, endocrinology, also hold appointments at the Omaha Division - VA NebraskaWestern Iowa Health Care System. Dr. Padala has two grants to study the connection between apathy and Alzheimer’s UNMC discover Prasad Padala, M.D. “Apathy is considered an untapped behavioral problem. If treated well, it can have significant impact on management of dementia and diabetes.” Prasad Padala, M.D. disease. Dr. Desouza’s grants focus on the impact of apathy treatment in people who are obese. They also have two federal grants that are under review. The two researchers are studying a well-known drug – Ritalin – as a treatment for apathy. Yes, the same Ritalin that is used to slow hyperactive children. “Ritalin works differently in adults and children,” Dr. Padala said. “With adults, it gives them more energy. Simply put, it increases the dopamine in the brain.” Dopamine is like the gas in your car. Low dopamine levels in the front of the brain can lead to apathy. “Apathy is one of the most profound and disabling aspects of Alzheimer’s disease,” said William Burke, M.D., professor and vice chairman of the UNMC Department of Psychiatry. One study determined that apathetic persons are nearly three times more likely than those without apathy to be impaired in day-to-day activities such as dressing, bathing, walking, eating and using the toilet. In addition, apathy is linked to cognitive dysfunction in dementia patients. With no interest or motivation, it becomes difficult for these patients to use their remaining cognitive function. Their memory, learning and communication skills deteriorate. “People are getting excited about apathy now because it may be a behavioral marker for a more rapidly progressing fall 2008 dementia,” Dr. Padala said. “Apathy is considered an untapped behavioral problem. If treated well, it can have significant impact on management of dementia and diabetes.” Dr. Padala is conducting a VA-funded placebo-controlled study for apathy treatment in 60 veterans with Alzheimer’s dementia. He said that early study results have been promising, as illustrated by the comments from the wife of an Alzheimer’s patient who is taking Ritalin. “After one month in the study, she came to me and said, ‘Thank you for giving my husband back to me. He’s doing things that he hasn’t done in the last five years,” Dr. Padala said. Diabetes is a major public health problem in the United States. It is much more common among veterans than in the general population. Self-management is a critical component to treating diabetes. “The key to living with diabetes is disease management,” Dr. Desouza said. “You have to exercise, watch your diet closely, keep your weight down and continually monitor your blood sugars. It’s not easy. You have to be driven. “Apathy can be devastating for patients with diabetes. Once they lose interest and stop managing the disease, the health ramifications can be dramatic,” he said. Dr. Desouza knows how difficult it is to motivate patients with diabetes. Despite all the innovations in treatment and guidelines, only about 10 percent of patients meet the benchmarks for diabetes control (blood sugar, blood pressure and cholesterol). The use of Ritalin is encouraging in the group of study participants, he said. “However, the brain is very complicated. We don’t know if improvement is due to the neuro chemical reaction resulting from taking Ritalin. More research needs to be done.” Ritalin is not the optimal drug, Dr. DeSouza said. Although it does increase dopamine, it also has several side effects, such as sleep disturbances, decreased appetite and increased blood pressure. Cyrus Desouza, M.D. Children who are hyperactive receive 80 mg of Ritalin as their daily dose. Adults in the studies are given much lower doses of Ritalin with Alzheimer’s patients receiving 10 mg and obesity patients receiving 20 mg. The lower dose helps lessen the side effects. “We need to find a pharmaceutical agent that can impact apathy,” Dr. Desouza said. “Ritalin is the best drug we have right now, but we are hopeful that we can find a better agent.” Dr. Desouza has funding to study the impact of treating apathy on weight loss initiatives. Through the Omaha VA, 125 veterans were enrolled in the pharmacological and nonpharmacological treatments for apathy. As part of the study, Drs. Padala and Desouza also are investigating a group therapy, “Medical Crisis Counseling,” for treatment of apathy. “There seems to be a common thread linking Alzheimer’s disease and diabetes, since people with diabetes are three times more likely to develop Alzheimer’s disease than non-diabetic individuals,” Dr. Padala said. Apathy may be that thread. Dr. Padala recently received funding from the Alzheimer’s Association to improve functional status, quality of life and glycemic control in patients with co-morbid dementia and diabetes. “This is ground breaking work,” Dr. Burke said. “They are trying to determine if treating apathy will not only benefit the day-to-day life of people with Alzheimer’s but if it might also have additional medical benefits in improving glucose control and increasing activity levels. This is a completely novel and exciting approach to a number of well known, often intractable, problems.” Are you apathetic? CHANGE IN APATHY OVER 12 WEEKS APATHY EVALUATION SCALE 59 54 49 If you answer ‘yes’ to any of these questions, you might suffer from apathy syndrome and should seek more detailed testing: 44 39 34 29 ❚ Have you lost interest in the world around you? 24 BASELINE 4 WEEKS 8 WEEKS 12 WEEKS Significant improvement in apathy scores was seen in the subjects with a mean decrease of 20 points on the apathy scale (p<.0001). Most improvement in apathy was noted at the fourth week visit, although the improvement continued throughout the study period. ❚ Are you more difficult to engage in conversation or in doing chores? ❚ Have you lost interest in doing things or in starting new activities? ❚ Are you apathetic or indifferent? UNMC discover UNMC researchers mentor junior investigators Growing Our Own by Lisa Spellman Mentor: a trusted friend, counselor, teacher, a more experienced person. Much like spreading fertilizer on young seedlings, federal grants awarded to two experienced UNMC researchers – Peggy Wheelock and Alexander Kabanov – are helping young investigators advance their careers, enhance their education and build their networks through mentoring. Here are their stories. 10 fall 2008 Junior investigator Jenny Wang, Ph.D., was about to submit her first R01 grant application to the National Institutes of Health (NIH), and she wanted it to be perfect. Fortunately, so did Peggy Wheelock, Ph.D., who suggested Dr. Wang wait to submit the grant. Having sat on review boards, Dr. Wheelock knows what it takes to write a grant that will pass muster. That was in June and for the next four months Dr. Wheelock patiently helped Dr. Wang re-write and refine her grant proposal until it was nearly perfect. “It was the nicest thing anyone could have done for me,” Dr. Wang said. “Her support was just the confidence boost I needed.” Right up until the last minute Dr. Wheelock was still asking Dr. Wang if she wanted her to read it, just one more time. “I said no, she had already helped me make it more understandable for the reviewers,” Dr. Wang said. “Once we had a draft that she felt was solid, I was completely comfortable submitting it in October.” It’s not unheard of for Dr. Wheelock, professor of oral biology in the UNMC College of Dentistry, to take time away from her research to pour over the grant proposal of a junior investigator. In fact, Dr. Wheelock spent countless hours reading and re-reading Dr. Wang’s grant proposal. Dr. Wang, who came to UNMC last year from the Roswell Park Cancer Institute in Buffalo, N.Y., is one of five junior investigators finding guidance under Dr. Wheelock’s wing. The mentoring program is part of a $10.9 million Centers of Biomedical Research Excellence (COBRE) grant that was originally awarded to Dr. Wheelock in 2003. Dr. Wheelock also is the director of the Nebraska Center for Cellular Signaling, which was established in 2003 with the Grow • Nurture • Support Peggy Wheelock, Ph.D. initial COBRE funding. The center focuses on the study of cell signaling and involves multidisciplinary collaboration between researchers. Under the grant, Dr. Wheelock mentors several junior investigators and oversees the progress of others whom she has paired with senior researchers. Researchers from UNMC, the University of Nebraska-Lincoln and Creighton University Medical Center lead five projects within the grant. Each project involves the study of cellular signaling with a focus on its role in producing tumors. The five-year grant was recently renewed by the National Center for Research Resources (NCRR), a division of the NIH, partly due to the success of seven junior investigators at UNMC who, with the help of this program, obtained their own R01 grants from the NIH. “The grant allows us to bring together outstanding junior and senior faculty with similar interests, which greatly enhances the science knowledge and opportunities for collaboration,” Dr. Wheelock said. When they first met, Dr. Wang was struck by Dr. Wheelock’s warmth and friendly personality. “Right away, she asked me how I was doing and offered to help in any way she could,” said Dr. Wang, an assistant professor in the UNMC Eppley Institute. Colleagues say Dr. Wheelock’s willingness to help is what has made her successful as a mentor. “Dr. Wheelock is approachable. The junior investigators working with her know this and are comfortable going to her,” said Rob Lewis, Ph.D., a professor in the Eppley Institute. “She will do everything she can to help her junior investigators succeed.” That includes pairing every junior investigator with two mentors who can help them navigate the complex world of grant writing. It also may mean extending a junior investigator’s funding from the usual three years to four – to give them more time to work on their research. “Dr. Wheelock could buy a lot of fancy equipment and fund core facilities, but instead she invests in human capital and the potential of young investigators,” Dr. Lewis said. The nurturing and feeding of seed money has worked so well, Dr. Wheelock has another five years to show more results. “The COBRE grant we received in 2003 helped us strengthen the biomedical research infrastructure in Nebraska. We’ve established a multi-disciplinary thematic center that enhances the research of young investigators and now we have seven success stories,” Dr. Wheelock said. Dr. Wheelock said one objective of the renewed funding will be to initiate pilot projects that further encourage and support collaborative, multi-disciplinary projects. “Teaching one how to be a successful, productive scientist is not a trivial task,” said Paula Turpen, Ph.D., director of research resources at UNMC. “The fact that three of the COBRE mentors (Drs. Wheelock and Lewis and Keith Johnson, Ph.D.) have been recognized as UNMC Distinguished Scientists in the past two years only confirms the quality of mentors in the Center for Cell Signaling. There is no doubt that the seven new NIH-funded junior faculty will continue to benefit from the guidance they received while participating in the COBRE program.” Steve Caplan, Ph.D., assistant professor, biochemistry and molecular biology, is one of the seven researchers who received a boost from the COBRE grant. Dr. Caplan joined the grant in 2004 when Dr. Wheelock selected him for a pilot project. He was later asked to become a project leader and was paired with two mentors: Richard MacDonald, Ph.D., biochemistry and molecular biology, and Dr. Lewis. “They taught me how to write better grants and advised me on where to submit my application,” Dr. Caplan said. “Peggy also helped, reading through parts of my grant proposals and manuscripts. She sets the tone for the mentorship part of the grant.” Dr. Caplan’s area of study is in protein trafficking – how proteins get from place to place in the cell. While it is basic research, he collaborates with other researchers who study specific protein receptors and want to better understand how proteins move around. Even though he no longer qualifies as a COBRE project leader, Dr. Caplan maintains a connection to Dr. Wheelock and her work. He finds himself in the nurturing role. “I try to help out as much as I can with the new investigators coming in, because I believe in what Dr. Wheelock is doing,” Dr. Caplan said. “She is an incredible role model, who dedicates a huge amount of time to mentoring while maintaining her own lab. She never stops worrying about what everyone else who is involved with the grant is doing. She is amazing.” The Research Project Grant (R01) is the original and historically oldest grant mechanism used by the Natiional Institutes of Health. The R01 provides support for health-related research and development based on the mission of the NIH. UNMC discover 11 Alexander Kabanov, Ph.D. New COBRE grant to grow nanomedicine program Alexander Kabanov, Ph.D., just received $10.6 million and he knows exactly what he’s going to do with it. The UNMC researcher hopes to save as many lives as he can by finding better ways to treat and cure hypertension, Parkinson’s disease and cancer. He plans to do this through nanomedicine, an emerging area of science that uses small polymeric particles to deliver drugs safely to disease sites. He has formed a team of highly talented junior investigators whose own complimentary projects will help Dr. Kabanov grow a world-class program in nanomedicine. Each of the junior investigators will be paired with mentors, including Dr. Kabanov. “The research projects funded by this grant will one day provide drug therapies to physicians that 12 fall 2008 target disease without harming the surrounding healthy tissue, which will result in better clinical outcomes for patients,” Dr. Kabanov said. He received a five-year COBRE (Centers of Biomedical Research Excellence) grant award in October from the National Center for Research Resources (NCRR), a part of the National Institutes of Health (NIH). As the director of the Nebraska Center for Nanomedicine, a part of the regent approved Center for Drug Delivery and Nanomedicine, and the Parke-Davis Chair in Pharmaceutics in the College of Pharmacy at UNMC, Dr. Kabanov tried for five years to get the grant. It was worth the wait. “While working on the grant proposal, I got to know UNMC and its scientists and administrators much better, giving me a deeper sense of pride for the institution,” he said. “Those years also gave me time to develop myself into a leader and for that I am very grateful.” GROWING OUR OWN There are other benefits to having the COBRE grant. “It allows us to attract the best and brightest scientists to Nebraska and develop novel technologies that could contribute to the economy of the state with the help of spin-off companies that would bring the results of the scientific research to public use,” Dr. Kabanov said. Not a bad combination, saving lives – and helping the economy. The COBRE is part of the Institutional Development Awards Grow • Nurture • Support (IDeA) network created by the NIH/NCRR to more equally distribute funding to states that have not traditionally received as much funding. The awards support multidisciplinary centers – each concentrating on one general area of research – that strengthen institutional biomedical research capability and enhance research infrastructure. “By bridging the research funding gap in IDeA states, we are building innovative research teams, leveraging the power of shared resources, and enhancing the science and technology knowledge of the state’s workforce,” said NCRR Director Barbara M. Alving, M.D. “It allows us to attract the best and brightest scientists to Nebraska and develop novel technologies that could contribute to the economy of the state.” Alexander Kabanov, Ph.D. Research seedlings The four young investigators whose projects will be supported through Dr. Kabanov’s COBRE grant are: Project 1: Principal investigator: Elena V. Batrakova, Ph.D., assistant professor of pharmaceutical sciences. Mentor: Howard Gendelman, M.D., chairman, department of pharmacology and experimental neuroscience; director, Center for Neurovirology and Neurodegenerative Disorders. Dr. Batrakova’s project focuses on creating a drug delivery system to treat Parkinson’s disease using nanozymes and immune cells in the brain as the delivery agent. Nanozymes are tiny particles consisting of an enzyme in a protective polymer coat. Project 2: Principal investigator: Matthew Zimmerman, Ph.D., assistant professor, cellular and integrative physiology. Mentor: Irving Zucker, Ph.D., professor and chairman of the cellular and integrative physiology department. Dr. Zimmerman’s research project focuses on using antioxidant therapy and nanozymes to treat hypertension. The COBRE grant will support the research projects of four junior faculty members, all of whom have been paired with an established faculty member, Dr. Kabanov said. The grant promotes collaboration among researchers with complementary backgrounds, skills and expertise. “All four projects focus on how polymer nano systems may be used to enhance the delivery of drugs, inhibit tumor growth, and improve treatment of cancer, neurodegenerative and central nervous system-associated cardiovascular disorders,” Dr. Kabanov said. The grant also will help establish core facilities needed to carry out the objectives of the multidisciplinary collaborative program. The first is a bioimaging core lab that will allow noninvasive diagnostics of neurodegenerative disease. The second will focus on preparation of new nanomaterials and ensure that these materials are safe for human use. Dr. Kabanov has prepared the ground and planted the seeds of research success. This grant provides the fertilizer that he needs to help grow the program. Ultimately, it is up to Dr. Kabanov and his team of researchers to make it thrive. Project 3: Principal investigator: Huanyu Dou, Ph.D., assistant professor, pharmacology and experimental neuroscience. Mentor: Surinder Batra, Ph.D., professor, biochemistry and molecular biology. Dr. Dou’s research project focuses on developing a cell-based nanoformulated anti-tumor therapy that would improve biodistribution of the drug to the tumor and reduce chemotherapy-induced neurotoxicity. Project 4: Principal investigator: Joseph Vetro, Ph.D., assistant professor, pharmaceutical sciences, and Center for Drug Delivery and Nanomedicine. Mentor: Alexander Kabanov, Ph.D., director, Center for Drug Delivery and Nanomedicine. Dr. Vetro’s research focuses on inhibiting the growth of cancer tumors by using specially developed nanocarrierse that disrupt the tumor’s ability to recruit surrounding blood vessels. UNMC discover 13 i Targeted delivery i INNOVATION by Elizabeth Kumru New system taxis drugs to ailing bones 14 fall 2008 What you are about to read may cause you to brush your teeth after every meal. You may also want to rinse your mouth each night with a special mouthwash created by a UNMC researcher. The mouthwash, formulated by Dong Wang, Ph.D., associate professor of pharmaceutical science in the UNMC College of Pharmacy, will not only protect your teeth from harmful plaque, but it also may help prevent bone loss in the jaw. UNMC discover 15 Dr. Dong Wang in his laboratory in UNMC’s College of Pharmacy. Run your tongue over the back of your teeth. If it feels as if they are coated with something, that’s biofilm. Biofilm, or plaque, is a sticky film of bacteria that constantly forms on the teeth. Food and drink that contain sugar or starch are converted by the bacteria in plaque to produce acids that attack tooth enamel. Over time, the enamel breaks down and cavities form. It’s difficult for mouthwash to break through plaque. While brushing takes it away, plaque resumes its cycle of buildup after brushing is completed. A polymer chemist by training, Dr. Wang has taken a commercially available polymer, or macromolecule, and formulated it into a novel drug delivery system to carry antimicrobial agents directly to teeth. The U.S. Food and Drug Administration has approved the polymer as a pharmaceutical excipient, or drug carrier. For commercialization, Dr. Wang envisions a mouth rinse formula that protects teeth from plaque. “The beauty of this design is the simplicity. All you have to do every night before bed is to brush your teeth and then rinse your mouth with our special formula. “We certainly will look at different flavors. I want something that’s tasty,” he said. The mouth is home to some of the most common diseases known to humans. Besides tooth decay, known to at least one-half of American children, unchecked plaque can lead to loss of bone around the teeth (periodontitis). Other diseases that affect the gums and lining of the mouth, include canker sores, oral herpes or cold sores and gingivitis. Although, collectively, it has declined among young children, tooth decay still can be a problem for individual children, and even teens and adults. If untreated, this type of decay can infect the internal structure and ultimately cause loss of the tooth. Nearly 12 percent of the adult population – more than 35 million people in the United States – lose bone support around their teeth. At present, Dr. Wang is collaborating with Kenneth Bayles, Ph.D., professor of pathology and microbiology, and his team to evaluate the formula against bacteria found in the oral cavity. “This synergistic effort with Ken’s group is our first test in the real world,” Dr. Wang said. Dr. Wang came to UNMC in January 2005 from the University of Utah where he started his research in targeted drug delivery for bones and joints. After his arrival in Omaha, the Beijing native began a collaboration with Richard Reinhardt, Ph.D., D.D.S., the B.J. and Ann Moran Professor of Periodontology and co-director of 16 fall 2008 undergraduate periodontics at the UNMC College of Dentistry. Together, they have designed several systems for oral applications. One system developed by Drs. Wang and Reinhardt is a bonetargeting cyclodextrin conjugate that targets and selectively binds to teeth and bones. The agent delivered can be released slowly over time, which increases the therapeutic index, or effectiveness, and overall performance of the agent. “The major advantage of the invention over the traditional formulation is that it offers a very simple mechanism of drug retention in the target area,” Dr. Wang said. To their surprise, a control study revealed that the carrier itself has some bone-building effect. Now the team is exploring the possibility of using this compound to treat osteoporosis. “This will be a great addition to the tools dentists have to fight bone loss and tooth decay,” Dr. Reinhardt said. Dr. Wang’s other research interests include the development of improved diagnostic and therapeutic systems for diseases such as rheumatoid arthritis, cancer bone metastasis and osteomyelitis. For the treatment of rheumatoid arthritis, Dr. Wang says his polymeric drug delivery system acts like a Mini Cooper in the way it delivers medications precisely to the destination. “The delivery system is small, agile and delivers drugs to an exact address in the body,” he said. Traditionally, a drug enters the body through a pill or injection and travels around to fulfill its purpose. But it also goes places it shouldn’t, which can cause harmful side effects to bones, organs and tissues. For people with rheumatoid arthritis (RA), the prescribed medications can cause such side effects as osteoporosis, nausea, easy bruising, mouth sores and possible kidney and liver damage. Dr. Wang’s drug delivery method uses a more efficient approach with a polymeric structure that could differentiate the healthy and arthritic joint. By preferentially delivering drugs to the arthritic joint, the “Mini Cooper” drug carrier would enhance therapeutic efficacy and potentially reduce side effects. Dr. Wang’s joint-targeting delivery system for arthritis treatment is supported by a three-year, $660,000 R01 grant from the National Institutes of Arthritis and Musculoskeletal and Diseases. He is collaborating with one of the world’s foremost RA experts, James O’Dell, M.D., the Larson Professor and vice chairman of internal medicine, and chief of UNMC’s section of rheumatology/immunology. “The delivery system is small, agile and delivers drugs to an exact address in the body.” Dong Wang, Ph.D. UNMC discover 17 The MRI pictures demonstrate the targeting of the macromolecular dexamethasone prodrug to the ankle joints of the arthritic rats (upper panel). The prodrug Does not stay in the healthy animal and is quickly cleared via urination (lower panel). “The strength of Dr. Wang’s approach is that he pursues scientific understanding, while keeping an eye on the clinical problems that require a solution.” On the left is a micro-computed tomography image of an arthritic rat treated with the macromolecular dexamethasone prodrug that Dr. Wang invented. The image shows preservation of the bones in the ankle joint. The image on the right shows severe deterioration of the bone in an arthritic rat that was not treated. Dr. O’Dell’s seminal contributions to improvements in RA therapy include his research on combination disease-modifying anti-rheumatic drugs (DMARD) and the use of tetracyclines as therapy for RA. Perhaps his best known work is his study of triple combination DMARD therapy in the treatment of refractory RA published in the New England Journal of Medicine in 1995. “Dr. Wang is doing exciting and cutting-edge research that will help us deliver medicine to sites of inflammation in the body,” Dr. O’Dell said. “With his system, we also have the ability to image those sites more clearly. This will allow us to better diagnose and treat patients with inflammatory arthritis such as RA.” With RA, people initially are offered glucocorticoid therapy for their disease. “But, one side effect of those drugs is osteoporosis,” Dr. Wang said. “With our polymer carrier, the drugs will be delivered directly to the arthritic joint and provide long-lasting relief – up to three weeks in animal studies. Potentially, we may use this as a safer bridging therapy to allow the effects of DMARD therapy to kick in.” 18 fall 2008 James Linder, M.D. UNeMed Corporation, the marketing and licensing arm for UNMC, has negotiated with the University of Utah to combine technology Dr. Wang developed there with his new RA inventions developed at UNMC. Human trials may begin in two years. As a creative thinker, Dr. Wang also wants to know how his drug delivery systems can be used in the treatment of breast and prostate cancer that has escaped chemotherapy and taken refuge in the bone. “With our bone-targeting polymeric delivery system, it is possible that we can stop bone damage from cancer metastasis and kill cancer cells in the bone. The bone often provides a safe hiding place and a launching pad for the spread of cancer to other organs,” he said. If it seems that Dr. Wang is everywhere, it’s because he is eager to explore how his delivery systems can be applied to other diseases. James Linder, M.D., president and CEO of UNeMed, said that’s characteristic of successful researchers. “The strength of Dr. Wang’s approach is that he pursues scientific understanding, while keeping an eye on the clinical problems that require a solution. This is a key attribute of anyone who does translational research,” Dr. Linder said. Dr. Wang also credits his success to the strong support he has received from his college and department. Dr. Wang’s drug delivery research is a perfect example of translational research that bridges the gap between basic science and the patient, said Courtney Fletcher, Pharm.D., dean of UNMC’s College of Pharmacy. “His projects illustrate to the public how their investment in research at UNMC and the College of Pharmacy can directly improve human health,” Dr. Fletcher said. Research that translates into practical use requires a curious clinician. “Clinicians know the science and ask questions and asking the right question is part of the success,” Dr. Wang said. “Physicians sometimes use different language, so we as researchers need patience to learn their language. It’s a very humbling experience. The same also applies to our collaborations with biologists. “Pharmaceutical research goes nowhere if we don’t have a clinical problem. The participation of physicians is essential.” Web Extra More on Dr. Wang’s research www.unmc.edu/discover Ankle joints of rats demonstrate the effectiveness of Dr. Wang’s drug delivery system. Image (A) shows the joint treated with an arthritis drug using Dr. Wang’s system is well-preserved, which is similar to the bone in a healthy rat (B). When an arthritic rat was treated without the system, the rat’s ankle joint experienced significant bone loss (C), which is similar to an arthritic rat that did not receive any treatment (D). Xin-ming Liu, Ph.D., research associate, works with Dr. Wang on chemical synthesis for the drug delivery system. Dr. Wang recognized On Oct. 23, Dr. Wang was honored as the recipient of UNeMed’s first Emerging Inventor Award and received a $25,000 innovation grant for unrestricted research from UNeMed during the 2008 Innovation Awards. The Emerging Inventor demonstrates exceptional skill and appreciation for scientific achievements. Dr. Wang was among dozens of UNMC inventors who were recognized for their new inventions, patents and licensed technologies. UNeMed Corporation, the marketing and licensing arm for UNMC, sponsored the awards. “Dr. Wang’s research is a promising step in the search for treatment for the joint damage and pain experienced by people who have rheumatoid arthritis. In addition, his other research efforts focus on osteoporosis and are equally as promising as therapeutics,” said Sara Conrad, licensing associate for UNeMed. Dr. Wang filed eight New Invention Notifications that have resulted in the filing of seven provisional patents and one international patent application covering several variations of the conjugates and their synthesis, Conrad said. Michael Dixon, Ph.D., vice president and chief operating officer of UNeMed, said Dr. Wang is one of UNMC’s most prolific inventors. “His inventions have drawn significant interest from both the clinicians and the pharmaceutical industry. His osteoporosis and arthritis technology have great potential to reach the clinic and improve health care,” he said. Dennis Robinson, Ph.D. chairman of pharmaceutical sciences, UNMC College of Pharmacy, said Dr. Wang is a worthy recipient of UNeMed’s first Emerging Inventor Award. “Since joining us in 2005, Dr. Wang’s enthusiasm and commitment has enabled him to rapidly establish a research program of outstanding quality and creativity,” he said. “He continues to build a growing national and international reputation for his research in drug delivery strategies that target bone and joints. Dr. Wang is an excellent scientist with a truly exciting future.” UNMC discover 19 The care connection by Elizabeth Kumru Diabetes is a difficult disease to manage. It affects the entire body. Management of blood sugar levels through healthy diet and physical activity is critical. Effective management helps patients lower the risks of developing such health problems as kidney disease, heart and blood vessel disease, blindness and neuropathy. But for millions of uninsured adults, help with management skills and preventive care seem like a luxury. A team of UNMC College of Nursing researchers want to change that paradigm for patients with Type 2 diabetes mellitus (T2DM) and health care providers across Nebraska. They are studying how the chronic care model can help patients take small incremental steps toward effectively managing their diabetes and other diseases. “This project will help us determine the effectiveness of our interventions. We know in theory that prevention is good, self-management works and nursing clinics are valuable. Now we’re putting all these elements together into one comprehensive care plan,” said Susan Beidler, Ph.D., associate professor, community based health, and director of the Morehead Center for Nursing Practice. The UNMC team is led by project director Teresa Barry, Ph.D., assistant professor, families and health systems, and Dr. Beidler, assistant project director. They are in the second year of a five-year, $1.6 million Health Resources and Services Administration (HRSA) grant. “We want to help empower people with diabetes to manage their disease better through small, achievable steps in lifestyle changes,” Dr. Barry said. “We find a higher degree 20 fall 2008 Nursing study examines new model of care for chronic disease of success if goals are set by the patient rather than the health care provider.” T2DM is the most common form of diabetes, affecting 95 percent of the 21 million people with diabetes. T2DM also is more prevalent in minorities and the uninsured. Lack of insurance leads to significant disparities in access and quality of care received, Dr. Barry said. In the United States, there are 47 million uninsured people. The diabetes rate among uninsured blacks is twice as high as Caucasians and three times as high among Hispanics, according to the Census Bureau report: Income, Poverty, and Health Insurance Coverage in the United States, 2007. “For individuals who have limited access to health care and other resources, trying to manage a chronic condition such as T2DM creates stress and can lead to depression and feeling powerless to improve their health,” Dr. Barry said. Untreated, the disease can lead to severe complications and increased cost to the health care system and patient. “We’re trying to change these outcomes,” Dr. Beidler said. The research project tests the effectiveness of a “three pronged” approach to care. It involves enhancing undergraduate and graduate student learning opportunities in caring for patients with chronic conditions, incorporating the latest evidence-based practice guidelines in provider practice, and promoting patients’ ability to manage their diabetes better. “If we prove this strategy of care is successful, it can be used in every clinic and applied to other chronic diseases,” Dr. Beidler said. Patients who are eligible to be in the study have limited financial resources and find it difficult to get medication and follow through with their appointments, Dr. Barry said. Often, preventive efforts are not valued because patients don’t feel sick and the long-term implications of the disease are not understood. The research project uses the UNMC Mobile Nursing Center as one way that patients with limited access to a Jan Herzog, project nurse coordinator, and Lucy Zavala, a bilingual medical assistant, inspect the diabetes foot models they use for patient education. Drs. Susan Beidler and Teresa Barry are studying how a chronic care model can help patients with diabetes manage their disease. regular health care provider can get referrals for care and free health screening for diabetes and other conditions. This site also gives students an opportunity to work with underserved patients. Study participants in Omaha who need follow-up care can get health care services from the UNMC Community Health Center or other local health clinics. Participants outside of Omaha are referred to a local health care provider for care. To date, the study has enrolled 42 low-income patients through the UNMC Family Health Care Center, which is part of the Community Health Center at 5155 S. 36th St. People enrolled in the study are mostly Hispanic who have little or no insurance. They are offered education support in English or Spanish, group sessions at the clinic, and home visits. The key component of the study involves the patient using a diabetes action plan. This action plan helps the patient pick a goal they feel they can meet, such as walking two blocks three days a week. The patient and health care provider can talk about the patient’s progress toward their self-management goals, as well as possible barriers or changes to the goals. Goal setting, using the action plan, is an ongoing process and successes are acknowledged and celebrated. So far, 13 people have participated in the home visit program that is conducted through the Ambulatory Care Community Health Nursing Project. This project pairs undergraduate public/community health nursing students with a patient or family for education and self-management support in their home environment where day-to-day management issues can be dealt with realistically. When needed, Lucy Zavala, a bilingual medical assistant at the health center, provides interpretative services for the home visits. The research has shown that home visits have helped gain the trust of patients. Jan Herzog, the project nurse coordinator at the health center, said that behavior changes can be difficult, but home visits reinforce two messages for the patient. “It says ‘we care about you and your challenges’ and ‘we take your disease seriously,’ ” she said. Research shows that home visits also motivate patients to stick to their self-management plan, Zavala said. “They know we are coming to visit and they want to show improvement. The patients feel comfortable being taken care of in their own home and it has made a difference in their plan of care. They feel a sense of trust and comfort having someone in their home who can speak their language and understand their culture,” she said. Resources available to assist patients with developing a self-management plan include food models to show correct portion sizes, illustrated booklets on nutrition and cooking and handouts on exercise. Plastic foot models are used to demonstrate proper foot care and identify possible complications that may occur. The team plans to expand the study with other community partners in other College of Nursing sites in Lincoln, Scottsbluff and Kearney. In addition, Drs. Barry and Beidler are exploring opportunities for interprofessional education and practice with other health care team members. Ultimately, they hope this model of care will be implemented in health care practices across the state to help patients deal with chronic diseases beyond diabetes. “Then we will truly have established a care connection,” Herzog said. UNMC discover 21 determined to make earlier diagnosis a reality by Karen Burbach Pancreatic cancer eludes detection – but not for long George Watson knows the grim statistics for pancreatic cancer. One in 76 people will develop pancreatic cancer, according to the American Cancer Society. Once diagnosed, a person has less than a 5 percent chance of living more than five years. Even so, the Chadron (Neb.) State College professor and private practice attorney is determined to beat the odds. “When you first get the diagnosis, you think it’s terminal,” Watson said. “But there is a percentage who overcome it.” Watson increased his odds for survival by being eligible for the Whipple procedure (see sidebar). But, researchers at UNMC’s Eppley Cancer Center, led by Tony Hollingsworth, Ph.D., want to increase every patient’s odds by identifying diagnostic markers that detect pancreatic cancer before symptoms appear and when surgical removal is still possible. “I’ve dedicated my career to making earlier diagnosis of pancreatic cancer a reality,” Dr. Hollingsworth said. Tissue donated by Watson helps Dr. Hollingsworth and the UNMC team, one of the largest pancreatic cancer research groups in the country. “Anything I can do that helps in the diagnosis and treatment is important for the future,” Watson said. The National Cancer Institute (NCI) funds three pancreatic cancer programs of excellence – one is at UNMC. The $5.3 million, five-year Specialized Program of Research Excellence (SPORE) grant in pancreatic cancer – sought after 22 fall 2008 by the country’s most prestigious research and medical facilities – funds translational research. “The SPORE grant earned by Dr. Hollingsworth and his colleagues is an outstanding achievement and important milestone for scientific research at UNMC and the UNMC Eppley Cancer Center,” said Ken Cowan, M.D., Ph.D., director of the cancer center. “The National Cancer Institute continues to recognize the important work being done at the Eppley Cancer Center.” For Dr. Hollingsworth and his team, there is an unrelenting drive to learn more about the basic biology of pancreatic cancer and study new biomarkers that enable them to diagnose the disease earlier. They also want to better understand the progression of the disease and develop new therapies that extend a patient’s life. “We’re at the cutting-edge of making a difference in people’s lives,” Dr. Hollingsworth said. A 6-inch long, spongy organ, the pancreas resembles a pear on its side and helps the body digest food and regular body sugar levels. Cancer occurs when cells in the pancreas develop genetic mutations, which cause cells to grow uncontrollably. Tumors form as these cells accumulate. “If we could shut down that process, we could significantly extend the patient’s life span,” Dr. Hollingsworth said. Early detection of the disease, however, is a major hurdle. Tony Hollingsworth, Ph.D. “We’re at the cutting-edge of making a difference in people’s lives.” Tony Hollingsworth, Ph.D. The location of the pancreas, deep in the abdomen, hinders early discovery of the disease and, unlike mammography, which provides early detection of breast cancer, there are no screening tools for pancreatic cancer. By the time tumors are found they often measure 1 centimeter or more and have metastasized or spread. “The disease has to be managed differently,” said UNMC researcher Surinder Batra, Ph.D. “We need a more systematic approach with pancreatic cancer because there’s so little time.” Watson went to the doctor in February for a nagging ache in his upper stomach. At first, he was treated for acid reflux and indigestion, but nothing changed. When he became jaundiced, doctors ordered a flurry of tests. The ultrasound and CAT scan showed a tumor on the pancreas. “I didn’t know much about pancreatic cancer, but knew it was a bad one to get,” Watson said. Fortunately, the cancer had not spread beyond the pancreas. Dr. Batra says a simple blood test – one that detects a protein produced by pancreatic cancer – would help alert patients to the disease. An internationally patented biomarker – first identified by UNMC researchers in 2001 and featured on the April 2007 cover of the Molecular Cancer Research Journal – shows promise in the early detection of the disease. Mucin 4, a human gene also known as MUC4, is associated with the disease progression and can be found in blood and tissue. A high level of the biomarker, detected through a costeffective blood test, may mean that cancer is in the body. “MUC4 expression is strongly associated with the lifespan of patients and could be a new early and specific marker for the diagnosis and prognosis of pancreatic cancer,” Dr. Batra said. “About 80 to 90 percent of pancreatic cancer patients have high levels of MUC4 in tumors, fine needle aspiration biopsies and blood, which that makes it easy for us to diagnose cancer.” Preliminary studies of the blood test show promise and a validation trial, funded by the NIH RO1 and SPORE grants, is underway. “The results of our trial could help us better manage the disease, determine who should go to surgery, how we should treat the patient and how we might stop or decrease expression,” Dr. Batra said. MUC4 may not be the only marker, though. Several of Dr. Hollingsworth’s projects focus on the study of MUC1, a glycoprotein that scientists believe plays an important role in the normal function of the pancreas. MUC1, they have found, interacts with and alters the function of p53, a tumor suppressor gene. “We want to study the big questions and understand how the tumors invade and metastasize so we can understand why the UNMC discover 23 “Patients should have hope and take comfort in the fact that there are researchers who care.” Tony Hollingsworth, Ph.D. SPORE grant spawns many projects The UNMC Eppley Cancer Center’s pancreatic program receives nearly $15.5 million in external funds, most of which comes from the National Cancer Institute (NCI). Of that, $5.3 million is part of a competitive five-year Specialized Program of Research Excellence (SPORE) grant in pancreatic cancer. The SPORE grant compliments the cancer center’s work with the NCI’s Early Detection Research Network (EDRN) and the UNMC-based Pancreatic Cancer Collaborative Registry. It also supports translational research projects, creates a new core in biostatistical support and provides partial support for UNMC’s tissue bank and unique rapid autopsy program. The EDRN brings together dozens of institutions to evaluate new ways to test for cancer risk and accelerate the translation of biomarker information into clinical use. The registry, meanwhile, unites at least 12 centers, including Johns Hopkins University, the University of Pittsburgh, Evanston Northwestern Healthcare and the University of Genoa (Italy), with expertise in pancreatic cancer research. The one-of-a-kind, Web-based registry has collected critical information and biological samples from 1,600 patients to develop prevention and treatment strategies. UNMC’s tissue bank, directed by Julia Bridge, M.D., and its unique rapid autopsy program, which allows cancer patients to donate entire organs, help researchers to study the disease. “The rapid autopsy program allows us to acquire a large volume of rarely obtained tissues,” said Tony Hollingsworth, Ph.D., who directs the program and the volunteer efforts of more than 30 technicians, students, nurses, residents and faculty members. “The program enables us to undertake many studies that are not otherwise possible.” 24 fall 2008 disease is so deadly,” Dr. Hollingsworth said. “Patients should have hope and take comfort in the fact that there are researchers who care.” Dr. Hollingsworth’s team helped discover MUC1 years ago. Since then, they have learned that it protects the cell surface and sends information about the cell surface to the nucleus. That information will be used to design tumor vaccines and make better diagnostic tests for pancreatic cancer. Plans already are underway on a clinical trial of an immunotherapy protocol that induces the patient’s immune system to recognize or attack the pancreatic cancer tumor – just as if it was a foreign invader. Watson’s father, George Watson Sr., had prostate and lung cancer, but there is no known history of pancreatic cancer in his family. After the diagnosis, Watson and his wife, Kathleen, decided to seek treatment eight hours from home at UNMC’s hospital partner, The Nebraska Medical Center. “You have to get to a place that deals with pancreatic cancer,” he said. “We’re fortunate here in Nebraska that we have a place.” Jean Grem, M.D., a nationally known expert in gastrointestinal malignancies, explores novel therapeutic approaches in both colon and pancreatic cancer. She has developed a clinical trial that uses a patient’s molecular profile to determine the best drug therapy for metastatic colorectal cancer. Plans are underway for a clinical trial to determine whether there is an advantage to using the peptide inhibitor of N-cadherin to reduce Aaron Sasson, M.D. Surinder Batra, Ph.D. the growth and spread of tumors and the incidence of metastasis. UNMC researchers have evidence that expression of N-cadherin by human cancer cells results in tumors that are highly aggressive. The peptide inhibitor, however, has reduced the severity of tumors in mice, said UNMC researcher Keith Johnson, Ph.D., who works on the project with Peggy Wheelock, Ph.D., and Dr. Grem. Another clinical trial will study the effects of a telomerase inhibitor at three levels: in cultured pancreatic cancer cells, in mice bearing pancreatic tumors and in patients with advanced pancreatic cancer. In cancer cells, an enzyme called telomerase prevents the protective caps at the end of chromosomes, or telomeres, from shortening, which, in normal cells, naturally occurs as we age. Once telomeres get too short, a healthy human cell stops dividing. Cancer cells are immortal, said UNMC researcher Michel Ouellette, Ph.D., because they tend to express telomerase, which prevents the shortening process and allows malignant cells to grow out of control. Researchers hope the telomerase inhibitor limits the lifespan of cancer cells and blocks the regrowth of residual disease after conventional therapy. That’s the type of news patients like Watson want to hear. Cancer treatments forced Watson – for the first time in 33 years – to miss this past summer’s student excursion to London. During his career, he has taken more than 800 Chadron State College students abroad on international study programs. “The trips give students a different perspective of life in general,” he said. Cancer does the same. “The diagnosis changes the reality of your life almost immediately,” Watson said. “I have tried to take the outlook that cancer should not alter my life plans, but it does make you more aware of the things that are important and the things that are peripheral.” Whipple procedure gives hope to people with pancreatic cancer George Watson was fortunate, in that, his cancer had not spread beyond the pancreas. That silver lining gave him the only chance for a cure. “The gold standard is to have the Whipple procedure, if possible,” said the father of three. Only 15 to 20 percent of pancreatic cancer patients are eligible for surgery and, of those, only 15 to 20 percent live five years, said Aaron Sasson, M.D., associate professor of general surgery at UNMC, and chief of GI surgical oncology. Prior to surgery, Watson underwent an intensive treatment regiment to shrink the tumor that sat near an artery. The regiment included three months of chemotherapy and radiation therapy under the guidance of Jean Grem, M.D., and Chi Lin, M.D. On July 8, Dr. Sasson surgically removed the rest of the growth in a Whipple operation. Dr. Sasson and his team (Drs. Quan Ly and Chandrakanth Are) are specialists with advanced training in the management of pancreas and hepatobiliary malignancies. His team takes an intensive approach to surgery, often removing blood vessels that surround the pancreas in order to eradicate the tumor. “Surgery can be quite complicated and last five to seven hours,” Dr. Sasson said. In the Whipple operation, the head of the pancreas, a portion of the bile duct, the gallbladder and the small intestine is removed. A portion of the stomach also may be removed. Then, the remaining pancreas, bile duct and intestine are sutured back into the intestine. To ensure the best outcome, the American Cancer Society recommends the Whipple operation be performed in experienced centers, such as The Nebraska Medical Center, that do a high volume of these complex surgical procedures. Dr. Sasson and his team perform more than 50 pancreas operations each year, the majority being Whipples. The death rate is significantly lower in hospitals that perform a high volume of these procedures, Dr. Sasson said. “Everything, so far, is good,” Watson said, later during a four-week cycle of chemotherapy. “The prognosis is only as good as the next test.” UNMC discover 25 Clinical researcher co-authors largest study on HIV drugs Susan Swindells, M.D., diagnosed common illnesses and injuries in an indigent, city-run clinic in Columbus, Ohio, when HIV first emerged in the early 1980s. “Patients started to turn up with symptoms we didn’t know about and there was no one to ask,” she said. “At that time, if you treated three people, you became an expert.” Thousands of patients later, Dr. Swindells is now an internationally renowned expert in human immunodeficiency virus, or HIV, and co-author of the largest study ever conducted to evaluate commonly used HIV drugs. The study, which was led by researchers at the University of Pittsburgh School of Medicine and published in the New England Journal of Medicine this past summer, confirmed that one of the most frequently prescribed triple-drug combinations for initial HIV infection is the most effective for suppressing HIV, but that a twodrug regimen is comparable. “The study showed that the triple-drug therapy currently preferred by clinicians is indeed the most effective treatment for HIV disease. It also is the simplest treatment regimen as all three drugs can be given once a day as one pill, compared to the two-drug regimen that requires seven pills a day. For those with prescription insurance, this means only one copayment each month,” said Dr. Swindells, the Terry K. Watanabe Professor of Internal Medicine in the section of infectious diseases and medical director of the UNMC HIV Clinic. Although, the one-a-day, three-drug regimen is preferred, it doesn’t work with all patients, Dr. Swindells said, including pregnant women and individuals with viral resistance. The study focused in part on nucleoside reverse transcriptase inhibitors (NRTIs), which are one of the first class of HIV drugs approved by the U.S. Food and Drug Administration. Although effective and commonly prescribed, NRTIs can produce severe side effects in some patients. The study, which included 753 participants at 55 centers, found that the popular three-drug combination of efavirenz plus NRTI therapy was more effective at achieving and maintaining reduction of the virus than another commonly prescribed drug combination of lopinavir-ritonavir plus NRTI. Interestingly, a two-drug combination of lopinavir-ritonavir plus efavirenz had a similar level of effectiveness as each of the tripledrug regimens that contained NRTIs. The study was conducted as part of the AIDS Clinical Trials Group (ACTG) – the largest HIV clinical trials organization in the With many patients, the goal is to get them to function as normal as possible 26 fall 2008 under the microscope by Karen Burbach world – with funding from the National Institute of Allergy and Infectious Diseases. Dr. Swindells, whose main research interests are in opportunistic infections, is chairwoman of ACTG’s Optimization of Co-Infection and Co-Morbidity Management Committee. The Manchester, England native also is involved with an international research study to determine how best to treat HIV and tuberculosis. Unlike some health care workers who looked the other way, Dr. Swindells embraced the challenges posed by HIV in the 1980s. “When you’re the clinic of last resort it’s difficult to say ‘go somewhere else’ because there’s nowhere else to go,” she said. In 2007, the UNMC HIV Clinic served 926 people, including 126 new cases. “We still see a steady trickle of new people – even in 2008 when we know how not to get HIV,” she said. But, unlike the early days, there is greater hope for today’s patients. “I tell my patients that HIV is a serious, chronic disease similar to diabetes in that you have to take care of yourself, eat right, take your medicine and go to the doctor,” she said. “You may develop some complications, but the chances of living to 60 are good.” who are we? In 2000, a group of individuals formed a not-for-profit organization called Nebraskans for Research (NFR). The group wanted to serve as a positive voice in support of medical research in Nebraska. In 2007, philanthropist, Richard Holland helped form Nebraska Coalition for Lifesaving Cures (NCLC). This new organization was made up of business, education, and community leaders who shared the same goals as Nebraskans for Research. The two organizations joined and took the name Nebraska Coalition for Lifesaving Cures. what do we do? We concentrate on two key areas: education and public advocacy. For the past eight years we’ve worked to support the efforts and accomplishments of Nebraska-based medical researchers, science educators and young collegiate scientists. In particular, we have advocated for stem cell research, therapies and cures in Nebraska. Under its new name, Nebraska Coalition for Lifesaving Cures continues to advocate awareness across the state for the accomplishments of Nebraska-based medical research and the improvement in people’s lives that research provides. Stem cell research, a relatively new breakthrough, holds the promise of providing treatments and cures for many diseases – including diabetes, Parkinson’s and spinal cord injuries – that alone, affect thousands of Nebraskans. how can you help? We invite you to join our Coalition to help support and protect lifesaving research and cures in Nebraska. Joining will cost you nothing – but it could help save the life of someone you love. To join Just fill out the form attached and return the self-addressed post card. If you would prefer, go online to www.NebraskaCures.com. research today for healthier tomorrows. 8401 West Dodge Road • Suite 111 • Omaha, NE 68114 • 402.390.2461 • www.NebraskaCures.com discover UNMC University of Nebraska Medical Center 985230 Nebraska Medical Center Omaha, Nebraska 68198-5230 Address Service Requested Non-Profit Org. U.S. Postage Paid Omaha, NE Permit No.454