* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Referral History
Childhood immunizations in the United States wikipedia , lookup
Duffy antigen system wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Neonatal infection wikipedia , lookup
Acute pancreatitis wikipedia , lookup
IgA nephropathy wikipedia , lookup
Globalization and disease wikipedia , lookup
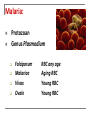
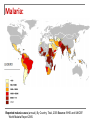
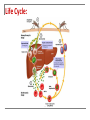
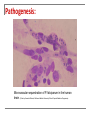
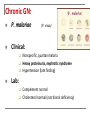
SMOKESCREEN DR EM Klaus 31st May 2010 Department Internal Medicine Division Nephrology Consultant : Prof B van Rensburgh Case Presentation: 14y Female Secondary School Student Nigeria Father recent immigrant to RSA Referral from Nephrologists in Rumuigbo, Port Harcourt, Nigeria for renal biopsy Referral History: Illness started end March 2010: Fever Progressive facial, leg swelling Oliguria No antecedent history: No skin sepsis, no sore throat No arthralgia, skin rash or mouth ulcers Referral History: Ill with facial and gross bipedal pitting oedema Pyrexia; Temp axillary 38°C Episodes of rigor, pallor was anicteric Respiratory: Rate: 24bpm Chest clear Cardio: P=68bpm; BP=110/80 Normal heart sounds; no murmurs or friction rub heard Referral History: Abdominal: Minimal Ascites No organomegaly Sideroom: Urinalysis 3+ proteinuria Numerous RBC, leukocytes and epithelial cells Granular casts Referral History: Lab: Na= 127.9 mmol/l K= 4.5 Cl= 97.2 BUN = 13.8 mmol/l Creat =159 umol/l eGFR=35 ml/min Total chol =7 mmol/l Referral History: Referral History: Lab: Peripheral Blood smear = P. falciparum malaria Referral History: Management: Hospitalized 2 – 21 April 2010 Rx: Quinine IVI Rocephin & Ciprofloxacin IVI Renal function not improved. Diagnosed as acute GN Fluid restrict Furosemide IVI Single Dialysis Prednisolone & Azathioprine History: Medication on arrival Universitas: Proguanil 50mg BID PO Prednisone 30mg BID PO Azathioprine 50mg BID PO Lasix 100mg BID PO daily ASA 75mg OD PO Norvasc 10mg OD PO Simvastatin 20mg OD PO Examination: 4th May 2010 Mass=54kg; Apyrexial General: L=155cm BP=130/80 BMI=22,5 kg/m² P=78 Bipedal oedema and peri-orbital oedema No jaundice, anemia Bilateral Malar rash – involving nasolabial folds Resp: Left pleural effusion Abdom: Ascites CVS: normal Neuro: normal MS: No vasculitis, synovitis Examination: 4th May 2010 Side room: Urine Dipstix: Urinalysis: 3+ prot; 4+blood; 3+ Leucocytes; WBC casts; Granular casts Na=125 K=3.5 C02=17 BUN=64.8 Creat=894 CRP=6.2 Alb=12 Chol=8,6 Urine Prot: Creat = 0.22mg/mg Examination: 4th May 2010 Renal U/S= Left=13,9cm Right=15,1cm Grade 2 hyperechoic with NO hydronephrosis Left pleural effusion + Ascites in pelvis Special Investigations: Urine (5th May) = Burkholderia Cepacia Sensitive to Ciprofloxacin, Bactrim Sputa MCS = Negative 24 hr Urine (6th May) = Volume = 566ml Creat Clearance = 8,7 ml/min Prot = 0,31g/24 hr Special Investigations: Malaria = Negative HIV = Negative RPR = Negative Hep B/C = Negative ASOT = <50 ANCA = Negative C3 = Negative; C4 = Negative ANA = Positive, Speckled, Titre 1:640 Anti ds DNA Positive Renal Biopsy: 13th May Immuno Florescence: Granular positivity with IgA, IgG, IgM, C1q, C3 and C4 Light Microscopy: All 9 glomeruli had extracapillary proliferation with formation of fibrocellular cresents compatible with CLASS IV LUPUS NEPHRITIS. Activity score 18/24 Chronicity 4/12. Problem Statement: 14 y Female 1. Class IV Lupus Nephritis Complication: Nephrotic Syndrome Renal Failure UTI Malaria- Associated Renal Disease Malaria: Protozoan Genus Plasmodium Acquired: Sting of infected Anopheles mosquito Blood transfusions (Prevalence amongst blood donors in a teaching hospital in Nigeria 32%) Infected vector introduced in aircraft (“aircraft malaria”) Malaria: Protozoan Genus Plasmodium Falciparum Malariae Vivax Ovale RBC any age Aging RBC Young RBC Young RBC Malaria: Reported malaria cases (annual), By Country, Total, 2003 Source: WHO and UNICEF. World Malaria Report 2005. Malaria immune status: NB in assessing suspected severe malaria Individuals might have partial immunity (i.e. grown up in areas with malaria transmission throughout the year) Could have asymptomatic parasitaemia with P. falciparum Presenting illness may be due to another cause (e.g. meningococcal meningitis in an older child with possible cerebral malaria). In patients without malaria immunity diagnosis established if parasitaemia present. Life Cycle: Pathogenesis: 1. Antigen-monocyte interaction 2. 3. ↑ expression intracellular adhesion molecule-1 and CD 14 Interaction Th1 and Th2 cytokines TNF α secretion Infected RBC express surface antigens (Pf155/RESA) favouring Th2 lymphocyte response P. falciparum activates the alternative Complement pathway + intrinsic coagulation cascade Pathogenesis: Plasmodium falciparum Infection induces changes RBC that cause them to : Adhere to each other and to the endothelium. Changes in RBC deformability Sequestered in the microcirculation Maturation of the parasite occurs prior to haemolysis and infection of new red blood cells. Blockage of the microcirculation → organ dysfunction and failure Pathogenesis: Microvascular sequestration of P. falciparum in the human brain. (Photo by Kamolrat Silamut, Wellcome Mahidol University Oxford Tropical Medicine Programme) WHO criteria for severe malaria: One or more of the following clinical or laboratory features Laboratory test 1. Hyperparasitemia Clinical manifestations 2. Acidosis Hyperlactatemia 1. Prostration (Defined as the inability to sit upright in a child normally able to do so, or to drink in the case of children too young to sit.) 2. 3. 4. 5. 6. 7. 8. 9. Impaired consciousness Multiple convulsions 3. 5. Renal impairment Hypoglycemia 6. Severe anemia 4. Respiratory distress (acidotic breathing) Pulmonary oedema (radiological) Circulatory collapse Abnormal bleeding Jaundice Hemoglobinuria Taken from WHO Guidelines for the Treatment of Malaria. (WHO, Geneva Switzerland: 2006). Full details of the definitions can be found in “WHO severe falciparum malaria” (Trans R Soc Trop Med Hyg 2000; 94 (Suppl. 1): 1–90). Classic presentation of severe malaria is: Discoloured urine due to haemoglobinuria from severe intravascular haemolysis: ‘blackwater fever’ Classic presentation of severe malaria is: Acute Renal Failure: Fluid, electrolyte disturbance and Renal Failure common esp P falciparum Mortality: 15 – 45% Untreated mortality: > 70% Acute Renal Failure Treatment: Common complication of severe malaria (non-immune adults and children) Treatment: Renal replacement therapy — preferably by hemofiltration when available HD superior to PD (in terms of mortality and cost-effectiveness) Nicholas Day, Arjen M. Dondorp, The Management of Patients with Severe Malaria. Am. J. Trop. Med. Hyg., 77(Suppl 6), 2007, pp. 29–35 Metabolic Acidosis Treatment: Common complication of severe malaria Strong associated with mortality Lactic acid, impaired renal bicarbonate handling and other unidentified acids play major roles Hemofiltration rapidly eliminate acidosis in malaria patients with renal failure, even in the presence of lactic acidosis. Early hemofiltration may be a useful in acidosis and renal impairment (NO trial data yet) Nicholas Day, Arjen M. Dondorp, The Management of Patients with Severe Malaria. Am. J. Trop. Med. Hyg., 77(Suppl 6), 2007, pp. 29–35 Glomerulonephritis Acute Transient GN Chronic GN Acute Transient GN: P.ovale, P. vivax, P.falciparum Acute nephritic / nephrotic syndrome Microscopic hematuria, mild proteinuria Low C3 and C4 Circulating immune complexes Mesangial proliferation Fine granular deposits of IgM and C3 Chronic GN: P. malariae Clinical: (P. vivax) Nonspecific, quartan malaria Heavy proteinuria, nephrotic syndrome Hypertension (late finding) Lab: Complement normal Cholesterol normal (nutritional deficiency) Chronic GN: P. falciparum Infects all RBC Severe Malaria Th1 response P. malariae Senescent RBC Indolent infection Th2 response Prolonged parasitemia, increased humoral and cell-mediated response Prognosis of Chronic GN : Despite successful treatment of malaria: ESKD in 3 -5 years Unmodified by steroids, immunosuppressive agents Progression: Genetics Malnutrition EBV Autoimmunity References: 1. Nicholas Day, Arjen M. Dondorp, The Management of Patients with Severe Malaria. Am. J. Trop. Med. Hyg., 77(Suppl 6), 2007, pp. 29– 35 2. WHO Guidelines for the Treatment of Malaria. “WHO severe falciparum malaria” Trans R Soc Trop Med Hyg 2000; 94 (Suppl. 1): 1–90). 3. Gary Maartens Severe malaria. CME June 2008 Vol.26 No.6 4. Johnson , Feehaly. Comprehensive Nephrology -3rd edition Disclosure Statement: No conflict of interest to be declared with this presentation