* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download anaphylaxis management
Survey
Document related concepts
Transcript
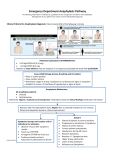
ANAPHYLAXIS MANAGEMENT 3 RS FOR TREATING ANAPHYLAXIS DON’T LOSE PRECIOUS TIME!!! Early recognition of an anaphylactic reaction is mandatory, since death occurs within minutes to hours after the first symptoms. AT THE EMERGENCY ROOM POSITION AIRWAY, BREATHING, CIRCULATION Assess airway patency because of the probability of edema or bronchospasm If there is severe laryngeal edema, intubation may be difficult to do. Instead, ventilate the patient with a bag-valve-mask (cricothyrotomy is reserved when both intubation and bag-valve-mask ventilation are not possible) High flow oxygen. O2 saturation must be maintained at above 90% ESTABLISH IV ACCESS For fluid therapy isotonic crystalloid solutions (such as NSS or LRS) to address the hypotension Since there is hypotension and tachycardia, a fluid bolus of 1L can be given. Further fluid therapy depends on patient response MONITORING Cardiac monitoring: ECG Blood Pressure monitoring Pulse Oximetry: to monitor respiratory output and gas exchange MEDICATIONS EPINEPHRINE Drug of choice for life threatening reactions Given in patients with systemic manifestations of anaphylaxis Can counteract the bronchospasm, hypotension, and GI symptoms EPINEPHRINE Increases systemic vascular resistance elevating diastolic pressure Bronchodilation increasing inotropy Increasing chronotropy of the heart reduces edema EPINEPHRINE Alpha Receptor Reverses vasodilation by vasoconstriction Reduces edema Beta Receptor Dilates broncial airways On the heart: inc inotrophy and chronotropy Suppress histamine and leukotriene release Inhibit activation of mast cells DOSAGE Given IV (if not possible, IM on anterolateral thigh) B. DIPHENHYDRAMINE (ANTIHISTAMINE) against cutaneous effects of anaphylaxis antagonize cardiac and respiratory effects continued for 2-3 days after treatment of the acute anaphylactic event. Adult 25-50 mg IV/IM q4-6h 50 mg PO q4-6h OTHER DRUGS... Beta Agonists Corticosteroids May be given should there be bronchospasm Continued because patient has asthma May be used to decrease the incidence or severity of delayed reactions Does not influence the acute course of disease Methylprednisolone 125mg IV or Hydrocortisone 250500 mg IV Glucagon used in addition to epinephrine, not as a substitute May be given if hypotension does not resolve after epinephrine and IV fluids Can be given in a patient taking a betablocker inotropic, chronotropic, and vasoactive effects causes endogenous catecholamine release 1 mg IV q5mins MANAGEMENT: FOLLOW UP ALLERGEN AVOIDANCE Avoid exposure to inciting agent (such as peanuts). If peanuts were not included in the breakfast or the inciting agent cannot be identified, referral to an allergologist. Instruct the patient to return should there be recurrent symptoms despite allergen avoidance and antihistamine EPI PEN Patient may be allowed to carry a selfinjectable epinephrine. There should be proper educations regarding its use, technique, storage, and when to replace.