* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Document
Prenatal testing wikipedia , lookup
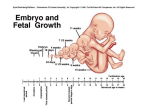
Prenatal development wikipedia , lookup
Women's medicine in antiquity wikipedia , lookup
Maternal physiological changes in pregnancy wikipedia , lookup
Breech birth wikipedia , lookup
Menstrual cycle wikipedia , lookup
Fetal origins hypothesis wikipedia , lookup
Management of Obstetrical Hemorrhage Jeffrey Stern, M.D. Incidence of Obstetrical Hemorrhage • • • • 4% of SVD 6.4 % of C-sections 13% of maternal deaths (1:10,000 to 1:1,000) 10% risk of recurrence Etiology of Obstetrical Hemorrhage: Antepartum • Placenta previa • Abruption • Coagulopathy: ITP/pre-eclampsia, FDIU Etiology of Obstetrical Hemorrhage: Intrapartum • • • • • • Placenta previa Abruption Abnormal placentation Genital tract lacerations: (2.4 odds ratio) Uterine rupture Coagulopathy: infection, abruption, amniotic fluid embolism Etiology of Postpartum Hemorrhage (Primary) (Within 24 hours of delivery) • Uterine atony (3.3 odds ratio) • Induction or Augmentation of labor (1.4 odds ratio) • Retained products of conception (3.5 odds ratio) • Placenta accreta, increta, percreta (3.3 odds ratio) • Coagulopathy • Fetal death in utero • Uterine inversion – may need MgSO4, Halothane, Terbutaline, NTG • Amniotic fluid embolism Etiology of Postpartum Hemorrhage (Secondary) (After 24 hours of delivery to 6 weeks postpartum) • • • • • 0.5-2% of patients Infection Retained products of conception with atony Placental site involution Rx: D+C, ABX, uterotonic medications Uterine Atony: 1 in 20 to 1 in 100 deliveries (80% of PPH) • Uterine over distension (Polyhydramnios, Multiple gestations, Macrosomia) • Prolonged labor: “uterine fatigue” (3.4 odd ratio) • Precipitory labor • High parity • Chorioamnionitis • Halogenated anesthetic • Uterine inversion Treatment of Uterine Atony • • • • Message fundus continuously Uterotonic agents Foley catheter/Bakri balloon (500cc) Uterine packing usually ineffective but can temporize • Modified B-Lynch stitch (#2chromic) – Uterine, utero-ovarian, hypogastric artery ligation – Subtotal/Total abdominal hyst. Treatment of Uterine Atony • Oxytocin – 90% success – 10-40 units in 1 liter NS or LR rapid infusion • Methylergonovine (Methergine) 90% success – 0.2 mg IM q 2-4 hours max. 5 doses; avoid with hypertension • Prostaglandin F2 Alpha (Hemabate) 75% success – 250 micrograms IM, intramyometrial, repeat q 20-90 min. max. 8 doses; Avoid if asthma/Hi BP • Prostaglandin E2 suppositories (Dinoprostone, Prostin E2) 75% success – 20 mg per rectum q 2 hours; avoid with hypotension • Prostaglandin PGE 1 Misoprostol (Cytotec) 75% - 100% success – 1000 microgram per rectum or sublingual (ten 100 micrograms tabs/five 200 micrograms tabs) Retained Products of Conception: Etiology • • • • • • Succentiurate lobe Placenta accreta, increta, percreta Previous C-section; hysterotomy Previous puerperal curettage Previous placenta previa High parity Management of Retained Products of Conception • Examine placenta carefully • Manual exploration of uterus • Careful curettage-Banjo curret Placenta Accreta, Increta, Percreta: Risk Factors • • • • • • High Parity Previous placenta previa Previous C-section GTN Advanced maternal age Previous uterine abnormal placentation Management of Abnormal Placentation • Placenta will not separate with usual maneuvers • Curettage of uterine cavity • Localized resection and uterine repair: (Vasopressin 1cc/10cc N.S-sub endometrial) • Leave placenta in situ – If not bleeding: Methotrexate – Uterus will not be normal size by 8 weeks • Uterine, utero-ovarian, hypogastric artery ligation • Subtotal/total abdominal hysterectomy Uterine Inversion: 1 in 2500 Deliveries • Risk factors: Abnormal placentation, excessive cord traction • Treatment – – – – – Manual replacement May require halothane/general anesthesia Remove placenta after re-inversion Uterine tonics and massage after placenta is removed May require laparotomy Coagulopathy • Hereditary • Acquired – – – – – – Preganancy induced hypertension Abruption Sepsis Fetal death in utero Amniotic fluid embolism Massive blood loss Genital Tract Laceration and Hematomas: Etiology • • • • • • Macrosomia Forceps Episiotomy Precipitous delivery C-section incision extension Uterine rupture Therapy of Genital Tract Lacerations • Superficial lacerations and small hematomas: expectant • Large laceration – Repair in layers – Consider a drain Hematomas • Below pelvic diaphragm: (vulva, paracolpos, ischiorectal fossa) – – – – – Leave alone if possible Legate bleeder - often difficult to find Pack open Drain May need combined abdominal/perineal approach • Above the pelvic diaphragm – Laparotomy- especially if expanding – Combined abdominal/perineal approach Selective Artertial Embolization by Angiography • Clinically stable patient – Try to correct coagulopathy • Takes approximately 1-6 hours to work • Often close to shock, unstable, require close attention • Can be used for expanding hematomas • Can be used preoperatively, prophylactically for patients with accreta • Analgesics, anti-nausea medications, antibiotics Selective Artertial Embolization by Angiography • • • • • Real time X-Ray (Fluoroscopy) Access right common iliac artery Single blood vessel best Embolize both uterine or hypogastric arteries Sometimes need a small catheter distally to prevent reflux into nontarget vessels • May need to treat entire anteriordivision or even all of the internal iliac artery. • Risks: Can embolize nearby organs and presacral tissue, resulting in necrosis • Technique – – – – Gelfoam pads – Temporary, allows recanalization Autologous blood clot or tissue Vasopressin, dopamine, Norepinephrine Balloons, steel coils Evaluate for Ovarian Collaterals May need to embolize Mid-Embolization “Pruned Tree Vessels” Post Embolization Post Embolization Pre Embo Post Embo Uterine Rupture • Scarred versus scarless uterus • Uterine scar dehiscence: separation of scar without rupture of membranes – 2-4% of deliveries after previous transverse uterine incision – Morbidity is usually minimal unless placenta is underneath or it tears into the uterine vessels – Diagnosis after vaginal delivery • Often asymptomatic, incidental finding • Difficult to diagnose because lower uterine segment is very thin • Therapy is expectant if small and asymptomatic – Diagnosed at C-section: Simple debridement and layered closure Uterine Rupture Etiology • Previous uterine surgery - 50% of cases – C-section, Hysterotomy, Myomectomy • • • • • • Spontaneous (1/1900 deliveries) Version-external and internal Fundal pressure Blunt trauma Operative vaginal delivery Penetrating wounds Uterine Rupture Etiology • • • • Oxytocics Grand multiparity Obstructed labor Fetal abnormalities-macrosomia, malposition, anomalies • Placenta percreta • Tumors: GTN, cervical cancer • Extra-tubal ectopics Classic Symptoms of Uterine Rupture • • • • • • Fetal distress Vaginal bleeding Cessation of labor Shock Easily palpable fetal parts Loss of uterine catheter pressure Uterine Rupture • Myth: Uterine incisions which do not enter the endometrial cavity will not • subsequently rupture • Type of closure: no relation to tensile strength – Continuous or interrupted sutures: chromic, vicryl, Maxon – Inverted or everted endometrial closure • Degree of complications – – – – Inciting event- spontaneous, traumatic Gestational age Placental site in relation to rupture site Presence or absence of uterine scar • Scar: 0.8 mortality rate • No scar: 13% mortality rate – Location of scar • Classical scar- majority of catastrophic ruptures • Transverse scar- less vascular; less likely to involve placenta – Extent of rupture Management of Uterine Rupture • Laparotomy – Debride and repair in 2-3 layers of Maxon/PDS – Subtotal Hysterectomy – Total Hysterectomy Pregnancy After Repair of Uterine Rupture • Not possible to predict rupture by HSG/Sono/MRI • Repair location – Classical -------------------------48% – Low transverse------------------16% – Not recorded---------------------36% • • • • Re-rupture-------------------12% Maternal death--------------1% Perinatal death--------------6% (Plauche, W.C 1993) Modified Smead-Jones Closure • Running looped #1 PDS/Maxon – Contaminated wounds/under tension • Additional Interruptured sutures - 2 cm apart – Fascial edges should be approximated – No tension