* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Slayt 1 - Toraks
Survey
Document related concepts
Transcript
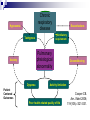
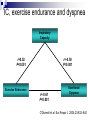
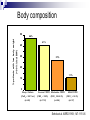
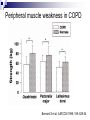
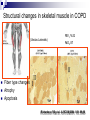
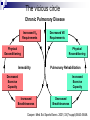
Pulmonary Rehabilitation in Chronic Lung Disease; Components and Organization Prof. Dr. Müzeyyen Erk Cerrahpaşa Medical Faculty Chest Disease Dept. Plan Chronic Respiratory Disease Definition Factors Contributing to Exercise Intolerance in CRD Pulmonary Rehabilitation Definition Patient Assessment Program Setting and Selection Plan Chronic Respiratory Disease Definition Factors Contributing to Exercise Intolerance in CRD Pulmonary Rehabilitation Definition Patient Assessment Program Setting and Selection Chronic diseases Definition “All impairments or deviations from normal which have one of more of the following characteristics: they are permanent they leave residual disability they are caused by non-reversible pathological alterations they require special training of the patient for rehabilitation they may be expected to require a long period of supervision, observation or care Factors limiting exercise CENTRAL • LUNG DYNAMIC HYPERINFLATION • REDUCED VENTILATORY RESERVE • COST OF BREATHING PERIPHERAL • MUSCLE ATROPHY, CAPILLAR DENSITY • POOR NUTRITIONAL STATE • POOR BIOENERGETICS • METABOLIC ACIDOSIS Daily physical activity pattern in COPD Walking Standing Healthy elderly (n=25) 11 COPD patients (n=50) 6 0% Sitting Lying 41 42 27 20% Others 52 40% 60% 4 12 80% 100% Pitta et al. Am J Respir Crit Care Med. 2005;171:972-977 COPD Chronic respiratory Airflow obstruction disease Hypoxemia Exacerbations Ventilatory requirement Tachypnea Air trapping Pulmonary phsiological abnormality Hyperinflation Anxiety Dyspnea Deconditioning Activity limitation Patient Centered Outcomes Poor health-related quality of life Cooper CB. Am J Med 2006; 119(10A): S21-S31. IC, exercise endurance and dyspnea Inspiratory Capacity r=0.52 P<0.001 r=-0.50 P<0.001 Exercise Endurance r=-0.61 P<0.001 Exertional Dyspnea O’Donnell et al. Eur Respir J. 2004;23:832–840 Dynamic hyperinflation during exercise in COPD O’Donnell D, Chest 2000 Body composition 50 41% 40 (< 90% ideal BW) % patients with low body weight 46% 30 27% 20 11% 10 0 R e s p . F a ilu re (P a O 2 < 5 5 T o rr) (n = 4 8 ) S e v e re C O P D M o d e ra te C O P D (F E V 1 < 3 5 % ) (F E V 1 3 5 -5 0 % ) (n = 1 1 2 ) (n = 5 6 ) M ild C O P D (F E V 1 > 5 0 % ) (n = 3 7 ) Schols et al. ARRD 1993; 147: 1151-6 Peripheral muscle weakness in COPD Bernard S et al. AJRCCM 1998; 158: 629-34 Structural changes in skeletal muscle in COPD FEV1 %32 (Vastus Lateralis) PaO2 87 Fiber type changes Atrophy Apoptosis Richardson RS et al. AJRCCM 2004; 169: 89-96 Exercise capacity as a predictor of mortality Proportion surviving 1.0 I II 0.9 0.8 0.7 0.6 0.5 0.4 0.3 III I: Peak VO2: >995 mL/min (n=37) II: Peak VO2: 793 -995 mL/min (n=38) IV III: Peak VO2: 654 - 792 mL/min (n=38) IV: Peak VO2: <654 mL/min (n=37) 0 12 24 36 48 60 Months of follow-up Oga T, et al. Am J Respir Crit Care Med 2003;167:544-549 Interventions aimed at improving exercise capacity (i.e. quality of life) Oxygen Heliox Rehabilitation Bronchodilators LVRS Plan Chronic Respiratory Disease Definition Factors Contributing to Exercise Intolerance in CRD Pulmonary Rehabilitation History Definition Patient Assessment Program Setting and Selection Pulmonary rehabilitation 1970s: The first controlled trials on PR 1980s: Initial skepticism Ideal candidates: Despite optimal medical treatment, significant abnormalities in their function and their participation in everyday life, leading to impaired HRQoL GOLD: PR should be considered in patients with an FEV1 below 80% Most national and international guidelines consider PR an important treatment option NETT: Strong encouragement for the implementation of PR programs for patients with COPD. Definition Pulmonary rehabilitation is an evidence-based, multidisciplinary, and comprehensive intervention for patients with chronic respiratory diseases who are symptomatic and often have decreased daily life activities. Integrated into the individualized treatment of the patient, pulmonary rehabilitation is designed to: reduce symptoms optimize functional status increase participation reduce health care costs through stabilizing or reversing systemic manifestations of the disease. ERS-ATS statement 2006 Pulmonary rehabilitation Integrated into the lifelong management of patients with chronic respiratory disease Involves a dynamic, active collaboration among the patient, family, and health care providers ERS-ATS statement 2006 Chronic respiratory conditions that benefit from PR program COPD Asthma Chest wall disease Cystic fibrosis Interstitial lung disease; post-ARDS pulmonary fibrosis Lung cancer Neuromuscular diseases such as post–polio syndrome Exercise program may not be appropriate for advanced disease Flexibility training Optimization of ventilator assistance re: Perioperative states (e.g., thoracic, abominal surgery) Pre- and post–lung transplantation, LVRS Pulmonary vascular disease Indications to pulmonary rehabilitations Symptomatic impairment attributable to pulmonary disability Failure of standard medical regimen to achieve adequate symptomatic relief Motivated, adherent patient Hill N.Proc Am Thorac Soc Vol 3. pp 66–74, 2006 Contrindications to pulmonary rehabilitation Lack of motivation Nonadherence Inadequate financial resources Severe cognitive dysfunction or psychiatric illness Unstable comorbidity (unstable angina, uncompensated congestive heart failure) Severe exercise-induced hypoxemia, not correctable with O2 supplementation Inability to exercise due to severe lung or other disease (arthritis, stroke) Cigarette smoking* Hill N.Proc Am Thorac Soc Vol 3. pp 66–74, 2006 Setting for pulmpnary rehabilitation Pulmonary rehabilitation is administered: inpatient outpatient home settings combination of these inpatient rehabilitation: In the United States: To be disabled to travel to and from an outpatient program Focus of these programs is more often on optimizing medical or ventilator regimens than on the exercise components In Europe: Ambulatory patients may be admitted to an inpatient program to undergo intensive therapy To avoid the inconvenience of daily travel MULTIDISCIPLINARY TEAM PARTICIPATING ON A PULMONARY REHABILITATION TEAM Physicians Therapists Pulmonologist Physiatrist TEAM Physical Occupational Respiratory Nurse or exercise physiologist Nutritionist Social worker Psychologist Hill N.Proc Am Thorac Soc Vol 3. pp 66–74, 2006 Keys for successful pulmonary rehabilitation ? Patient selection Program components PATIENT SELECTION ANY STABLE PATIENT WITH DISABLING SYMPTOMS (ACCP/AACVPR) ? PULMONARY FUNCTION ? AGE ? CO-MORBIDITY ? SMOKING ? PSYCHOSOCIAL CONDITIONS ? MUSCLE WEAKNESS ? MODIFICATION Components of a rehabilitation programme Patient education Psychosocial support Chest physiotherapy Exercise training Muscle training Nutritional support Hill N.Proc Am Thorac Soc Vol 3. pp 66–74, 2006 Main components of PR programmes Donner CF, Decramer M. Pulmonary Rehabilitation ERJ Monograph, 2000: 13:132-142 Education Psycosocial support General exercise training Selected muscle training Chest physiotherapy Occupational therapy Nutritional intervention COPD +++ ++ +++ ++ + ++ + Asthma ++ ++ +++ CF & bronchiect. ++ ++ +++(*) + + Chest wall disor. ++ ++(*) +++ + ++ + Neuromusc. dis + ++ + Respir sleep dis + ++ Pre-post surgery ++ ++ +++ ++ +++ ++ Tracheostom pat ++ ++ + + + + + + + Interst lung dis (+): No evidence, (++): Few evidences, (+++): Good evidence, (*): Before transplantation Topics often covered during group education sessions What’s wrong in common lung diseases Breathing medications Oxygen therapy Energy conservation techniques Relaxation techniques Breathing techniques Pursed lip breathing Diaphragmatic breathing Nutrition What to do in emergencies Traveling with lung disease End-of-life issues Hill N.Proc Am Thorac Soc Vol 3. pp 66–74, 2006 Significant benefits of pulmonary rehabilitation Established by multiple randomized controlled trials (Level A evidence) 1. Improved functional capacity (6-min walk or Shuttle Walk Test) 2. Reduced dyspnea* 3. Improved health-specific quality of life* Observed in some randomized controlled trials (Level B evidence) 1. Reduced need for hospitalization* * Only in patients with COPD with severe airway obstr. Hill N.Proc Am Thorac Soc Vol 3. pp 66–74, 2006 Benefits of Pulmonary Rehabilitation in COPD Improves exercise capacity Reduces intensity of breathlessness A A Improves HRQoL Reduces hospitalizations Reduces anxiety and depression A A A Improves arm function Improves survival Respir. muscle tra. (+ general exer) Psychosocial intervention B B C C GOLD Exc. Summ. 2008 The vicious circle Chronic Pulmonary Disease Increased VE Requirements Physical Deconditioning Decreased VE Requirements Physical Reconditioning Immobility Pulmonary Rehabilitation Decreased Exercise Capacity Increased Exercise Capacity Increased Breathlessness Decreased Breathlessness Cooper. Med Sci Sports Exerc. 2001;33(7 suppl):S643-S646.