* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Pediatric IBD
Infection control wikipedia , lookup
Compartmental models in epidemiology wikipedia , lookup
Epidemiology of metabolic syndrome wikipedia , lookup
Nutrition transition wikipedia , lookup
Race and health wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Alzheimer's disease wikipedia , lookup
Fetal origins hypothesis wikipedia , lookup
Preventive healthcare wikipedia , lookup
Epidemiology wikipedia , lookup
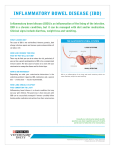
What’s So Special about Pediatric IBD ? David Tuchman, MD Division of Pediatric Gastroenterology and Nutrition Herman and Walter Samuelson Children’s Hospital at Sinai CSGNA Fall Educational Program November 8, 2014 Educational Objectives • Review the different types of IBD • Discuss etiology of IBD • Learn the differences between Pediatric IBD and Adult IBD • Learn the effects of IBD on growth and development • Discuss the effects of IBD on bone development • Learn about the transition of care in IBD Inflammatory Bowel Disease (IBD) • IBD is an term for a group of diseases which Crohn’s disease and Ulcerative colitis • Chronic, debilitating conditions • Distinctly different diseases but are grouped together as IBD – Produce similar signs and symptoms – Intestinal inflammation, abdominal pain and diarrhea IBD – Type and Anatomic Distribution IBD Crohn’s Diseae Ulcerative Colitis Indeterminate Colitis IBD – Facts and Figures • Health care costs: $1.7 billion dollars annually • 1.4 million Americans have been diagnosed with IBD • About 10% of these individuals are children and adolescents under the age of 17 years • Peak age incidence is between 15 and 25 years IBD in Children • Impact on children – 25% of IBD occurs in childhood • Incidence and prevalence – 1.4 million people in the US have IBD – Crohns disease is diagnosed in 5000 children each year – It is estimated that 50,000 – 100,000 children have IBD NASPGHAN 2nd Edition Burril Crohn, Leon Ginzburg and Gordon Oppenhiemer Regional ileitis. Journal of American Medical Association (October 1932) • … to describe, in pathologic and clinical details, a disease of the terminal ileum, affecting mainly young adults, characterized by subacute or chronic necrotizing and cicatrizing inflammation. The ulceration of the mucosa is accompanied by a disproportionate connective tissue reaction of the remaining walls of the involved intestine… (which) leads to stenosis … with formation of multiple fistulas. Aufses, Surgical Clinics of North America, 2001; 81(1) Feb 2001. IBD Presentation Symptom/Sign Crohns Disease Ulcerative Colitis Abdominal Pain ++ ++++ Diarrhea ++++ +++ Rectal bleeding ++ ++++ Weight loss ++++ ++ Growth Failure +++ + Perianal disease ++ Mouth ulcers ++ + Fever + + Erythema nodosum ++ + Anemia +++ +++ Arthritis + + Crohns Disease vs. Ulcerative Colitis Crohns Disease Ulcerative Colitis Any portion of GI tract Colon only Skip areas Continuous Rectal Sparing No rectal sparing Non-caseating granulomas No granulomas Transmural inflammation Mucosal inflammation Fistulae and abscesses Abscesses rare Stictures commom Strictures rare Ileum and cecum commonly involved Perianal disease IBD – Diagnostic Approach • Suspect diagnosis – History (“red flags”), Family History – Labs: • Iron deficiency anemia, elevated ESR, CRP, low serum albumin • Exclude other etiologies – Stools studies • Enteric pathogens, C. difficile, amebiasis, TB skin test • Classify disease • Crohns, UC • Determine extent of disease – “stage” the disease • Evaluate for extra-intestinal manifestations • Evaluate growth and development Laboratory Studies in the Initial Evaluation for IBD • CBC with differential • ESR/CRP • Comprehensive Metabolic Panel – Serum albumin – Liver chemistries • Stool studies – Enteric pathogens – Fecal calprotectin – Stool for occult blood Imaging Studies • Upper GI series and small bowel follow through • Abdominal and pelvic CT scan • Magnetic Resonance Imaging Imaging Studies in IBD MR enterography Abdominal CT Scan Endoscopic appearance of normal terminal ileum and colon Terminal Ileum Smooth and shiny Villi seen Lymphoid follicles (Peyer’s patches) Colon Normal vascular pattern No friability Smooth and shiny Normal folds Endoscopic Appearance of Crohns Disease • • • • • Deep fissures Cobblestoning Segmental distribution Relative rectal sparing Terminal ileal involvement • Granulomas on biopsy Endoscopic Appearance of Ulcerative Colitis • • • • Loss of vascular pattern Granularity Exudates Diffuse continuous disease • No ileal involvement IBD Histology IBD – Perianal Disease • Perianal abscesses, fistulae and fissures • Perianal disease is noted in about 10 % of children with newly diagnosed Crohn’s disease 1 1 Keljo et al. Inflamm Bowel Dis. 2009;15 :383-387. IBD - Extraintestinal Manifestations Eye UVEITIS EPISCLERITIS IBD - Extraintestinal Manifestations Skin Erythema Nodosum Pyoderma Gangrenosum IBD - Extraintestinal Manifestations Hepatobiliary Disease Oral Disease Inflammatory Bowel Disease • Etiology – Unknown • IBD occurs in genetically susceptible individuals whose immune systems react abnormally to environmental agents in the gastrointestinal tract Pathogenesis of IBD - Multifactorial Genes IBD Environment Mucosal Immune System Nature Reviews Immunology 8, 458-466 (June 2008) IBD - Genetics • High degree of concordance among monozygotic twins • Increased susceptibility to IBD among first- or second-degree relatives of affected individuals • Linkage between IBD and several genomic regions • Several mutations/single-nuceotide polymorphisms (SNPs) have been found to be associated with increased susceptibility to IBD • Age of onset: younger the onset, more likely a family history of IBD Bousvaros et. Inflamm Bowel Dis 2006; 12(9), 885- 913 Pediatric IBD • • • • • • Severity of Disease Growth (Weight and height gain) Sexual maturation Health Supervision Psycho-social well being Healthcare Provider Transitioning Children with IBD are not just small adults with IBD • Adolescents with IBD have more extensive involvement – 69% of adolescents present with ileo-colonic disease vs. 28% of adults1 – 23% of adolescents with Crohn’s present with upper tract involvement – uncommon in adults1 – Adolescents more likely to have ulcerative pancolitis compared to adults (67 % vs. 44%)1 • Childhood-onset Crohn’s – more extensive involvement than than adult- onset Crohns (43% vs. 3%)2 1Goodhand et al. Inflammatory Bowel Disease 2010:16:947-952 VanLimbergen et al. Gastroenterology 2008;135:1114-1122 Abraham and Kahn Gastro and Hepatol 2014;10:633-640 2 “Idiopathic “ IBD is rare in the young child Pediatric Reference Cutoff Proportion of young children Gupta 2008 (n=989) 5 years 10% (Crohn’s only) Kugathasan 2003 (n=199) 10 years 20 % Cannioto 2007 (n=184) 2 years 9% Bousvaros Boston Children’s Hospital Symposium 2014 IBD in Younger Children (< 5 years) • • • • • • • • Chronic granulomatous disease Glycogen storage disease 1b Hermansky – Pudlak syndrome NEMO Wiskott-Aldrich syndrome IPEX Hyper IgM syndrome Common Variable Immune Deficiency Bousvaros Boston Children’s Hospital Symposium 2014 IBD in young children • Immunodeficiencies frequently involve the gi tract and have IBD like symptoms • Most idiopathic IBD in children under the age of 5 years involves the colon • Caution using immunosuppression in patients with immune deficiency • Optimal treatment is determined after multidisciplinary consultation • www.neopics.org Bousvaros Boston Children’s Hospital Symposium 2014 Growth Failure • Definition – Height < 5th percentile – Decrease in height velocity below 5th percentile – Fall off of the child’s growth curve • Higher incidence at diagnosis in CD vs. UC – – – – Corticosteroids Inadequate calorie intake Malabsorption Increased energy expenditure from chronic inflammation – Pro-inflammatory cytokines, decreased IGF -1 Sawczenko et al Pediatrics 2006;118:124-9 Tigas et al J Pediatr Gastroenterol Nutr 1993;16:373-80 Kocoshis - Presention Growth Failure in IBD Patients Occurrence (%) Pediatric IBD 35 Prepubertal CD 60-85 Children with UC 6-12 Kirschner in Kirsner, ed. IBD 5th ed. 2000 NASPGHAN Growth Failure in Pediatric IBD Suboptimal intake of calories Increased energy needs Malabsorption of nutrients Increased GI losses Malnutrition Growth Failure Corticosteroids Inflammation Growth Problems in Children with IBD • Increased cytokines act on – Brain affecting appetite and calorie intake – Hepatic expression of IGF 1 – Act on chondrocytes of the growth plate of the long – Growth hormone insensitiviy Sanderson Nature Reviews Gastroenterology & Hepatology 11, 601–610 (2014) Growth Velocity Curves Evaluating Growth IBD Treatment Goals • • • • • Maximize therapeutic response Maximize adherence Minimize toxicity Improve quality of life Promote physical growth and pubertal development • Promote psychological growth • Prevent disease complications NASPHGAN slide set IBD – Treatment Approach • Follow up appointment very soon after procedure • Stress that IBD is not rare • Famous people with IBD – President Eisenhower • Review the proposed etiologies • State what IBD is not – allergy, stress, diet • What are the limits? – None, except sky diving and bungee jumping • Introduce the team • Provide literature – CCFA, NASPGHAN Treatment of Crohn’s Disease • Mild to moderate CD – Aminosalicylates • Topical and oral – Antibiotics – Enteral feeds – Corticosteroids • Budesonide • Prednisone • Moderate to severe CD – Enteral feeds (induction) – Corticosteroids (induction) • Budesonide vs. prednisone – Immunomodulators (maintenance) • 6-mercaptopurine • Azathioprine • Methotrexate – Biologics (Induction and maintenance) • Infliximab • Adalimumab • Certolizumab Crohn’s Disease – Antibiotic Therapy • Effect on luminal bacterial concentrations and subsequent down regulation of the local inflammatory response • Selectively eliminate bacterial subsets • Bacterial tissue invasion and microabscess formation • Bacterial translocation and systemic dissemination Sartor; Gastroenterology 2004; 126:1620-1633 Enteral Nutrition – IBD • • • • • • Improves nutrition for all IBD Effective therapy for pediatric Crohn’s UC – not shown to be effective 80-100% calories by formula NG tube vs. oral Proposed mechanism - Modulatoin of intestinal bacteria Baldassano and Kim IBD and Corticosteroid Therapy • Steroids are rarely used as monotherapy • If clinical response to initial therapy is inadequate, add corticosteroids early • Steroids are not maintenance drugs – Many side effects including growth impairment But, use of steroids can “get you out of trouble quickly” Immunomodulators and IBD • • • • 6 MP, Azathioprine, Methotrexate Measure TPMT phenotype Closely monitor CBC, LFT’s Other adverse effects: – Pancreatitis • Increased risk of lymphoma – Slight increased risk for EBV associated lymphoma – Minimal if any risk of non-Hodgkin’s lymphoma Mercaptopurine in Maintaining Remission in CD Markowitz, et al; Gastroenterology 2000: 119:895-902 Biologic Agents – Adverse Events • Infusion reactions – Acute/delayed • Rare complications – HSTCL – TB and increased risk of infection – Lupus – like reaction • Monitor – – – – PPD CXR Skin examnations Labs: CBC, LFT’s Immunomodulators and Biologics for Ulcerative Colitis • 6 MP and AZA used to reduce steroid exposure • Started soon after induction with other agents • Not indicated for acute treatment of fulminant UC • Role of biologics still being defined Immuno-compromised patient • No live virus vaccines – Intra-nasal influenza – MMR, OPV, Varicella • Killed vaccines should be given accroding to recommended schedule – – – – – Influenza Pneumococcus Hepatitis B Meningococcus HPV Melmed. Inflamm Bowel Dis 2009;15:1410-1416 Bone Health in children with IBD • Bone mineral density if often reduced in children with IBD • Pathogenesis is multifactorial • Decreased bone turnover more likely than increased resorption • Vertebral compression fractures can occur Sylvester et al J Pediatr 2006; 148:461-466 NASPGHAN slide set Therapy for Decreased Bone Density • Control the underlying disease • Optimize nutrition – Calories/protein – Calcium/Vitamin D • Promote physical activity • Consider referral to a specialist in bone health Nutritional Complications of IBD • Osteopenia and osteoporosis • Anemia • Micronutrient deficiencies – Iron – Folate – B12 – Zinc Depression and Anxiety in Children with IBD • 25 -30% of children with IBD have symptoms of depression and/or anxiety • 10-30% meet criteria for clinical depression or an anxiety disorder • Predictors of depression – Stressful life events; maternal depression – Family dysfunction; steroid treatment; older age • These rates are similar to children with other chronic illnesses Mackner et al . Inflamm Bowel Dis 2006;12:239-244 MESSAGE Acronym for Depression Screening M Mood (depressed or irritable) and Motor (hyper or hypo) E Energy (fatigue) S Sleep (insomnia or hypersomnia) S Suicide or Self-Esteem A Anhedonia (lack of pleasure) G Guilt E Eating (change of appetite) Rufo et al. NASPGHAN monograph - June 1 2011 Pediatric and Adult IBD - Transitions Compared with adults, adolescents with IBD had • Fewer clinic visits • More documented noncompliance • More active IBD on endoscopic evaluation • Higher Crohn’s disease activity1 1 Bollegala et al. J Crohns Colitis 2013; 7:e55-e60 Pediatric vs. Adult Healthcare • • • • Pediatric Care Family centered Multi-disciplinary Parent primary caregiver and decision-maker May ignore growing independence and increasingly adlt behavior • • • • Adult Care Patient centered Single physician Acknowledges patient autonomy and independence May neglect family concerns Healthcare Provider Transitioning Checklist from Digestive Health for Life, CDHNF, NASPGHAN Age Patient 12-14 Early Adolescence – New knowledge and responsibilities • I can describe my GI condition • I can name my medications, the amount and times I take them • I can describe the common side effects of my medications • I know my doctors and nurses names and roles • Mid Adolescence – Building knowledge and practicing independence • I know the names and purposes of the tests that are done • I know what can trigger a flare of my disease • I know my medical history • Late Adolescence – Taking Charge • I can describe what medications I should not take because thety might interact with the medication I am taking for my health condition • I carry insurance information (card) with me in my wallet/purse/backpack • 14-17 17 + Health Care Team • • • Discuss the idea of visiting the office without parents or guardians in the future Encourage independence by performing part of the exam with the parents or guardians out of the examining room Always focus on the patient instead of the parents or guardians when providing any explanations Allow the patientto select when the parent or guardian is in the room for the exam Remind patient and family that at age 18 the patient has the right to make his or her own health choices Develop specific plans for selfmanagement outside the home (work/school) Resources and Tools for Successful Transition Educational Resources for Providers Transition in IBD www.ibdtransition.org.uk/ Transition Guidelines for Providers NASPGHAN guidelines (Baldassano et al J Pediatr Gastroenterol Nutr 2002;34:245-248 Transition Readiness Assessment and Tools www.naspghan.org Resources and Tools for Adolescents and Parents Crohns and Colitis Foundation of America (CCFA) Transition Advocacy and Support for Patients, Parents and Providers Society for Adolescent Health and Medicine Abraham and Kahn Gasto and Hepatol 2014:10:633-640