* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download general introduction
Survey
Document related concepts
Transcript
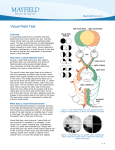
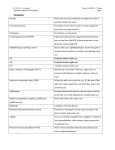
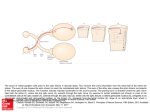
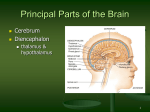
Section Ⅰ Disorders of consciousness 刘 海 若 伦敦火车出轨事故 凤凰卫视金 牌主持脑死亡 中国日报网站消息:据法新 社5月12日报道,在10日伦敦火 车出轨的事故中丧生的7人里, 包括两名台湾电视媒体工作人 员。曾经在台湾电视网TVBS工 作、现为香港凤凰卫视咨询台 主持人的刘海若头部受到重创, 已被诊断为脑死亡。 刘海若不是脑死亡 凌锋教授赴英会诊有结果 2002年05月20日17:04 北京晚报 前往英国为凤凰卫视记者刘海若会 诊的北京宣武医院凌锋教授昨天下 午1时3分返京。据凌教授介绍:刘 海若的伤情已有转机,目前有自主 呼吸,不是脑死亡。 宣武医院神经外科主任凌锋教 授与英国的医生一起检查了刘海若 的全身状况,并仔细讨论了病历及 CT片。 凌教授认为,刘海若已有 自主呼吸,另外对刺激有收缩反应, 并且有咳嗽,这些都证明她不是 “脑死亡”,生存下来是可能的。 刘海若苏醒创医学奇迹 八方援手力催凤凰重生 2002年08月16日每日新报 三个月前在英国因车祸陷入昏迷的凤凰卫视女 主播刘海若,不久前已在北京宣武医院恢复神 志。 8月上旬,海若已经可以清晰地做出各种表情 反应了,当医生说出数字时,海若已经能用手 比划出动作了。主治医生凌锋表示,海若的病 情有了质的变化,虽然距离正常人反应的灵敏 程度还相差很远,但她已经不是植物人了,确 切地说———海若已经醒了。 Ⅰ.Consciousness state of the patient’s awareness of self and environment and his responsiveness to external stimulation and inner need. the Content of consciousness Orientation percepbility attitudes emotions active Structural basis 1.ascending reticular activating system, ARAS reticular formation thalamus cerebral hemisphere alert state 2.cortex Ⅱ clinical manifestation 1.according to level of consciousness 2.according to content of consciousness 1.level of consciousness (1) Somnolent (2) Stupor (3) Coma lesser degree deep Somnolent stupor Can be roused only by vigorous and repeated stimuli, when left unstimulated they quickly drift into a sleeplike state. coma The patient who appears to be asleep and at the same time incapable of being aroused by external stimuli or inner need. lesser degree coma: reflex (+) Deep coma: no reaction of any kind is obtainable, corneal, pupillary, pharyngeal, tenden reflex (-) 2.content of consciousness (1) (2) (3) Confusion Delirium Special Type Decorticated Syndrome Akinetic mutism confusion “clouding of the sensorium” Inability to think with customary speed Marked by some degree of inattentiveness and disorientation accompanied by illusions Delirium state Hallucination, hyperactivity High fever, atropine overdose, alcohol Decorticated syndrome Neocortical death ARAS is normal, arousal-nonarousal cycle Open eyes, blink, swallow, eyes move Coma, Show no signs of awareness of the environment or inner need Vegetative state, decerebrate rigidity 12 in 45 awakened in 2 weeks, >3 month:PVS Akinetic mutism The term akinetic mutism has been applied to yet another group of patients who are silent and inert as a result of bilateral lesions of the anterior parts of the frontal lobes, leaving the intact of the motor and sensory pathways; the patient is profoundly apathetic, lacking to an extreme degree the psychic drive or impulse to action(abulia). The abulic patient registers most of what is happening about him and forms memories. Ⅲ differential diagnosis (1) Abulia (2) Locked-in syndrome abulia The patient are silent and inert as a result of bilateral lesions of the anterior parts of the frontal lobe, leaving intact the motor and sensory pathways, the patient is lacking to an extreme degree the psychic drive or impulse to action. Locked-in syndrome Lesion of the ventral pons (basis pons) Interrupts the corticobulbar and corticospinal pathways depriving the patient of speech and the capacity to respond in any way except by vertical gaze and blinking wakefulness Ⅳ brain death Harvard medical school committee 1968 1. Absence of cerebral function 2. Absence of brainstem function including spontaneous respiration 3. Irreversibility Brain death 1. Absence of cerebral function: Deep coma, total lack of spontaneous movement, and of motor and vocal responses to all visual auditory and cutaneous stimulation 2. No spontaneous respiration 3. Absence of brain stem function: Dilated midposition fixed pupils, corneal reflex, oculocephalic and oculovestibular test, gag reflex(-), last for 12 hours 4. EEG: flat or isoelectric (<2μV) during a 30-minutes recording 5. Spinal reflex may persist 6. Exclude intoxication, hypothermia, metabolic disturbance Section Ⅱ Aphasia, apraxia, agnosia aphasia A loss or impairment of the production and/or the comprehension of the spoken or written language due to an acquired lesion of the brain No higher order mental function disturbance i.e. Confusion, delirium, mental retardation Not dysarthria Not aphonia classification 1.Parasylvian fissure aphasic syndrome Broca aphasia, Wernicke aphasia Conduction aphasia 2.Transcortical aphasia Transcortical motor, sensory, mixed 3.Global aphasia 4.Anomic aphasia 5.Subcortical aphasia syndrome thalamic aphasia, basal ganglion aphasia Broca aphasia Primary deficit in speech production Dominant hemisphere Inferior frontal gyrus, posterior portion Wernicke aphasia Primary deficit in comprehension Paraphasia: literal: the grass is greel verbal: the grass is blue Disturbance in repetition Wernicke area: posterior portion of supratemporal gyrus Transcortical aphasia Watershed area Repetition is remarkably preserved Anomic aphasia The patient lose only the ability to name people and objects Middle temporal lobe Global (Total) aphasia Left middle cerebral artery occlusion All aspects of speech and language are affected Can say only a few words Subcortical aphasia Thalamic aphasia Basal ganglion aphasia: nonfluent, dysarthric, paraphasic apraxia The term apraxia is applied to a state in which a clear-minded patient with no weakness, ataxia or other extrapyramidal derangement and no defect of the primary modes of sensation loses the ability to execute highly complex and previously learned skills and gestures. apraxia Ideomotor apraxia Ideational apraxia Melokinetic apraxia Constructional apraxia Facial-oral apraxia Dressing apraxia agnosia A highly-ordered perceptual disturbance, no elementary sensation disturbance, can not interpret sensations correctly. Due to disorders of the association areas in the parietal lobes. agnosia Visual agnosia: object, face, verbal Auditory agnosia: verbal Sensory agnosia Body image disturbance non-dominant parietal lobe Gerstmann syndrome finger agnosia, right-left confusion, dysgraphia, Dyscalculation Dominant hemisphere angular gyrus 伦敦火车出轨事故 凤凰卫视金 牌主持脑死亡 中国日报网站消息:据法新 社5月12日报道,在10日伦敦火 车出轨的事故中丧生的7人里, 包括两名台湾电视媒体工作人 员。曾经在台湾电视网TVBS工 作、现为香港凤凰卫视咨询台 主持人的刘海若头部受到重创, 已被诊断为脑死亡。 刘海若不是脑死亡 凌锋教授赴英会诊有结果 2002年05月20日17:04 北京晚报 前往英国为凤凰卫视记者刘海若会 诊的北京宣武医院凌锋教授昨天下 午1时3分返京。据凌教授介绍:刘 海若的伤情已有转机,目前有自主 呼吸,不是脑死亡。 宣武医院神经外科主任凌锋教 授与英国的医生一起检查了刘海若 的全身状况,并仔细讨论了病历及 CT片。 凌教授认为,刘海若已有 自主呼吸,另外对刺激有收缩反应, 并且有咳嗽,这些都证明她不是 “脑死亡”,生存下来是可能的。 刘海若苏醒创医学奇迹 八方援手力催凤凰重生 2002年08月16日每日新报 三个月前在英国因车祸陷入昏迷的凤凰卫视女 主播刘海若,不久前已在北京宣武医院恢复神 志。 8月上旬,海若已经可以清晰地做出各种表情 反应了,当医生说出数字时,海若已经能用手 比划出动作了。主治医生凌锋表示,海若的病 情有了质的变化,虽然距离正常人反应的灵敏 程度还相差很远,但她已经不是植物人了,确 切地说———海若已经醒了。 刘海若住院实况首次播放 恢复很快已能开 口说话2002年09月07日北京娱乐信报 信报讯(记者张迪) “真没想到海若的病情会恢复得 这么快,当我听见女儿对我说,‘爸爸,生日快乐’时, 心里真高兴啊。”昨天,凤凰卫视女主持人刘海若的父 昨天,宣武医院首次向媒体播放海若在医院里拍摄 的录像,但为了尊重海若及其家人,海若的面容被“隐 藏”起来。海若身穿浅蓝色条纹的住院服装,能很清晰 地讲话,她对前 来看望她的市卫生局的金局长说: “谢谢金局长,谢谢大家对我的关心!”刘父说:“8 月18日那天,第一次听到了她叫‘爸爸’,前几天过生 Section 3 A.Disturbance of Vision B. Disturbance of Ocular Movement A Ⅰ. Visual pathway Retina→optic nerve→ optic chiasm→optic tract →lateral geniculate nucleus (LGN)→optic radiation→occipital lobe(calcarine sulcus) Optic chiasm: fibers from the nasal retinas cross over Ⅱ reduced vision 1. One eye Central retinal artery occlusion Amaurosis fugax Retro-bulbar optic neuritis multiple sclerosis, neuromyelitis optica Foster-Kennedy syndrome anosmia, optic atrophy on one side Papilledema on the other side , seen in frontal lobe tumor Ⅱ reduced vision 2. Two eyes Cortical blindness : dilated pupil, light reflex is preserved Toxic: methyl Deficiency: pernicious anaemia Ⅲ visual field defect 1. Optic nerve: uniocular blindness Ⅲ visual field defect 2. Optic chiasm: bitemporal hemianopia seen in pituitary tumor, craniopharyngioma Ⅲ visual field defect 3. Optic tract: homonymous hemianopia Ⅲ visual field defect 4. 5. Optic radiation: quadrant anopia Ⅲ visual field defect 6. Visual cortex: homonymous hemianopia with macular sparing Ⅲ visual field defect 1. Optic nerve: uniocular blindness 2. Optic chiasm: bitemporal hemianopia seen in pituitary tumor, craniopharyngioma 3. Optic tract: homonymous hemianopia 4. Optic radiation: quadrant anopia 5. Visual cortex: homonymous hemianopia with macular sparing B. Disorder of ocular movement Ⅰ anatomy 1. Oculomotor nerve: 上睑提肌 levator of lid 上直肌 superior rectus 下直肌 inferior rectus 下斜肌 inferior oblique 内直肌 medial rectus 瞳孔扩约肌 pupillary sphincters 睫状肌 ciliary muscle Ⅰ anatomy 2. Trochlear nerve: 上斜肌 superior oblique muscle 3. Abducens nerve: 外直肌 lateral rectus muscle Ⅱ ocular paralysis 1. Ocular motor nerve paralysis Ptosis Lateral deviation of the eye Inability to rotate the eye upward, inward and downward Diplopia Dilated non-reactive pupil, paralysis of accommodation Ⅱ ocular paralysis 2. Trochlear nerve Can not rotate down and outward The patient complains of special difficulty in reading or going downstairs Ⅱ ocular paralysis 3. Abducens nerve Paralysis of outward movement Eye deviates medially Diplopia Ⅱ ocular paralysis 4. Nuclear ophthalmoplegia Brain stem lesion: infarction, MS Accompanied by ipsilateral cranial nerve paralysis, contralateral hemiplegia Ⅱ ocular paralysis 5. Internuclear ophthalmoplegia (INO) Ⅱ ocular paralysis 5. Internuclear ophthalmoplegia (INO) Gaze:frontal lobe→ paramedian pontine reticular formation→ abducens medial longitudinal fasciculus →ocular motor Ⅱ ocular paralysis 5.1 Anterior internuclear ophthalmoplegia With a lesion of the left MLF, the left eye fails to adduct when the patient looks to the right, this condition is referred to as left internuclear ophthalmoplegia. Ⅱ ocular paralysis 5.2 One-and-a-half syndrome Pontine center for gaze and ipsilateral MLF One eye lies fixed in the midline for all horizontal movements; the other eye can make only abducting movements. Ⅱ ocular paralysis 6. Superanuclear ophthalmoplegia Middle frontal gyrus No diplopia Two eyes are equally affected Reflex movements are spared Ⅲ alterations of the pupils 1. Pupillary light reflex Optic nerve→optic chiasm→optic tract→ Pretectal area→bilateral E-W nuclei→ Oculomotor nerve→pupillary sphincter Ⅲ alterations of the pupils 2. Horner sign Miosis Ptosis Retraction of eye-ball Loss of sweating on the same side of face Due to interruption of the sympathetic fiber. Section 4 vertigo and deafness Ⅷ cranial nerve: vestibular nerve cochlear nerve Ⅰ. Vertigo All subjective and objective illusion of motion or position, usually rotational. Ⅰ Vertigo To maintain balance: visual system proprioceptive system vestibular system Vestibular system: labyrinth vestibular nerve central pathway to cerebellum, MLF, autonomic center Ⅰ Vertigo Peripheral Central Location Labyrinth, vestibular nerve Brain stem, cerebellum, cortex Etiology Vertigo Labyrinthitis, meniere’s disease, vestibular neuronitis, otitis media Severe, short attack VBI, acoustic neuroma, temporal epilepsy May be prolonged Nystagmus horizontal May be vertical Other sign Deafness, tinnitus Cranial nerve palsy, contralateral pyramidal sign Ⅱ deafness Auditory system: External auditory canal→tympanic membrane→ stapes→oval window→ organ of corti, hair cell→cochlear nerve→ pons→bilateral lateral lemniscus→inferior colliculus→medial geniculate body→temporal lobe Ⅱ deafness 1. Conductive deafness Otitis media, rupture of the tympanic membrane, cholesteatoma 2. Sensorineural deafness Meniere’s disease, drugs—aminoglycosides, acoustic neuroma, infarction, multiple sclerosis Exam: Auditory evoked potentials Section 5 Syncope Ⅰ. Syncope an episodic loss of consciousness and postural tone and an inability to stand, due to diminished flow of blood to the brain. Section 5 Syncope Ⅱ. Causes: 1. Reflex syncope vasodepressor syncope, orthostatic hypotention, carotid sinus hypersensitivity, micturitional, vagoglosssopharyngeal, associated with glossopharyngeal neuralgia Section 5 Syncope 2. Cardiac syncope arrythmia, myocardial, obstruction 3. Brain TIA, arteritis 4. Other causes anemia, hypoglycemia, hypoxia Section 5 Syncope Ⅲ clinical feature 1. Prodrome dizziness, vertigo, pallor, sweating, dim vision, tinnitus 2. Episode loss of consciousness, fall to ground, Bp<60mmHg, if more than 25 seconds may have convulsion 3. Post episode Regain consciousness, no sequela Thank you for listening! 佡剑非 nǎo [email protected]