* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Cochlear Implant
Telecommunications relay service wikipedia , lookup
Auditory processing disorder wikipedia , lookup
Hearing loss wikipedia , lookup
Noise-induced hearing loss wikipedia , lookup
Speech perception wikipedia , lookup
Audiology and hearing health professionals in developed and developing countries wikipedia , lookup
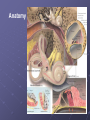
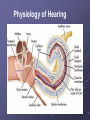
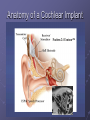
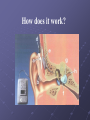
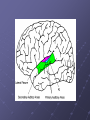
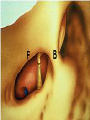
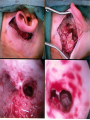
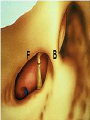
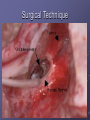
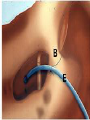
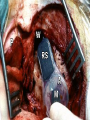
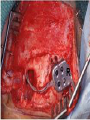
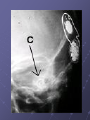
Cochlear Implant Prof. Hamad Al Muhaimeed The Fundamental Concept of Cochlear Implant To bypass the damaged hair cells. History: • Old generation: Sound awareness only • New generation: Improved communication abilities (auditory cues with lip reading, open set speech) • Since 1972 more than 16 different cochlear implants • 1984 FDA approval for adults • 1990 children approval Anatomy Anatomy Anatomy Scala tympani Scala vestibuli Cochlear duct Basilar membrane Vestibular membrane Tectoral membrane Hair cells (outer/inner) Cochlear nerve fibers Anatomy-micro Physiology of Hearing Anatomy Sensorineural Hearing Loss Death of hair cells vs. ganglion cells Otte, et al estimated we need 10,000 ganglion cells with 3,000 apically to have good speech discrimination Apical ganglion cells tend to survive better (?acoustic trauma) Central neural system plasticity Pathologic Anatomy Anatomy of Speech Mix of frequencies Speech recognition is “top-down” process Formant frequencies: frequency maximum based on vocal tract F0 is fundamental frequency F1 & F2—contribute to vowel identification F3—l,r (lateral and retroflex glides) F4 & F5—higher frequency speech sounds Some speech based on amplitude—k, f, l, s Structure of Cochlear Implant 1. External components 2. Internal components Components of Cochlear Implant Types of Cochlear Implants Single vs. Multiple channels Audio example of how a cochlear implant sounds with varying number of channels Monopolar vs. Bipolar Speech processing strategies Spectral peak (Nucleus) Continuous interleaved sampling (Med-El, Nucleus, Clarion) Advanced combined encoder (Nucleus) Simultaneous analog strategy (Clarion) Anatomy of a Cochlear Implant How does it work? Neural Responses to Sound 1. Temporal coding: Provide information about timing cues (rhythm and intonation. 2. Place coding: Rely on the tonotopic organization of a neural fibers. 3. Provide information about quality (timber of a speech signal – sharp to dull) Site of Stimulation 1. Extracochlear 2. Intracochlear 3. Retrocochlear (lateral recess of the fourth ventricle over the cochlear nuclei. Stimulus a. Stimulus type: - Analog (continuous) - Digital (pulsatile) b. Stimulus configuration 1. Bipolar – localized site of stimulation 2. Monopolar – stimulates large population of neurons Speech Coding As speech is produced, the mouth, nose & pharynx modify the frequency spectrum so that peaks and formants are produced at certain frequencies. Speech processing used – 3 formants: F0 = 100 to 200 Hz F1 = 200 to 1200 Hz F2 = 550 to 3500 Hz Number of Channels 1. Single channel – no place coding 2. Multi channel Stimulation Mode 1. Simultaneous: More than one electrode is activated at a given succession - CIS 2. Sequential: A continuous series of electrode activates in succession speak Electrode Design 1. Single electrode 2. Multielectrode Indication for Cochlear Implant Adults 18 years old and older (no limitation by age) Bilateral severe-to-profound sensorineural hearing loss (70 dB hearing loss or greater with little or no benefit from hearing aids for 6 months) Psychologically suitable No anatomic contraindications Medically not contraindicated Indications for Cochlear Implantation -- Children 12 months or older Bilateral severe-to-profound sensorineural hearing loss with PTA of 90 dB or greater in better ear No appreciable benefit with hearing aids (parent survey when <5 yo or 30% or less on sentence recognition when >5 yo) Must be able to tolerate wearing hearing aids and show some aided ability Enrolled in aural/oral education program No medical or anatomic contraindications Motivated parents Factors Affecting Patient Selection a. b. c. d. e. f. g. Onset of deafness (congenital or adventitious) Year of deafness Length of sensory deprivation (i.e. no hearing aids) Socioeconomic factors Educational level Individual ability to use minimal cues General health Factors Affecting Pt. (cont.) h. Personality i. Willingness to participate in rehabilitation program j. Language skills k. Appropriate expectations l. Desire to communicate in a hearing society m. Psychological stability n. Cochlear patency Audiologic Evaluation 1. Pure tone audiometry under headphones 2. Warble tone audiometry with a hearing aid in a monitored free field 3. Immittance testing 4. Speech recognition testing 5. Speech awareness testing Audiologic Evaluation (cont.) 6. Environmental sounds (closed and open set) 7. Speech reading (lip reading) ability 8. Electrical response audiometry 9. Auditory discrimination 10.Transtympanic electrical stimulation (promontory or round window test) Medical Evaluation 1. 2. 3. 4. 5. 6. 7. 8. 9. Clinical history and initial interview Preliminary examination Complete medical and neurologic examination Cochelar imaging using computed tomography (CT or magnetic resonance imaging (MRI) Vestibular examination (electronystagmography) Pathology tests Psychologic or psychiatric assessment or both Vision testing Assessment for anesthetic procedures CT Findings Contraindications Incomplete hearing loss Neurofibromatosis II, mental retardation, psychosis, organic brain dysfunction, unrealistic expectations Active middle ear disease CT findings of cochlear agenesis (Michel deformity) or small IAC (CN8 atresia) Dysplasia not necessarily a contraindication, but informed consent is a must H/O CWD mastoidectomy Labyrinthitis ossificans—follow scans Advanced otosclerosis Surgical Procedure All electrode insertions are carried out through the facial recess approach. Various incision designs are used to allow wide exposure of the mastoid and squamous portions of the temporal bone. The temporalis muscle and periosteum are widely stripped to accommodate a “table” for the pedestal of the Ineraid device or the receiver-stimulator of the other devices. The mastoidectomy is not widely saucerized, but instead overhanging ledges are purposefully maintained. Care must be exercised so as not to damage the fibrous annulus during the facial recess approach.. Surgical Technique Complications: A. Intraoperative 1. Intraoperative cannot be placed appropriately. 2. Insertion trauma 3. Gusher Complications (cont.): B. Postoperative 1. Postauricular flap edema, necrosis or separation 2. Facial paralysis 3. Transient vertigo is more likely to occur on a totally nonfunctioning vestibular system. 4. Pain is usually associated with stimulation of Jacobson’s nerve, the tympanic branch of the glossopharyngeal nerve. 5. Facial nerve stimulation 6. Meningitis 7. Device extrusion Rehabilitation Tuning or mapping of the external processor to meet individual auditory requirements after 3 - 4 weeks postop. 1. Multisensory approach 2. Bimodal stimulation 3. Suprasegmental discrimination training 4. Segmental discrimination and recognition training 5. Speech tracking 6. Counseling Rehabilitation Rehabilitation Rehabilitation Rehabilitation Rehabilitation Rehabilitation Rehabilitation Pediatric Implantation Five years after approval was given for adult implanta-tion by FDA, approval of cochlear implants for use in patients ages 2 to 17 years was granted. The major concerns regarding implantation in children included difficulty in evaluating the young child’s hearing impairment, assessing the performance and effect of implantation on the child’s development compared with traditional types of training, the risks of implantation (both intraoperative and long term), the effects of implantation on the auditory system, and the challenges of effectively programming such sophisticated devices in children. Auditory Brain Stem Any Question ?