* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Pituitary Physiology and Deficiencies
Survey
Document related concepts
Transcript
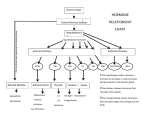
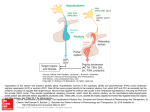
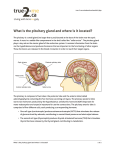
Pituitary Physiology and Deficiencies Heidi Chamberlain Shea, MD Endocrine Associates of Dallas Pituitary • Pituitary – “Master” gland – Most of the pituitary hormones control other endocrine glands Goals of Discussion • Review pituitary anatomy • Understand pituitary physiology • Discuss pituitary hormone deficiencies Nomenclature • Pituitary – Greek • ptuo (to spit) – Latin • Pituita (mucus) – Mucus was produced by the brain and was excreted through the nose by the pituitary Pituitary Development • Evagination of the stromodeal ectoderm from buccal cavity • Infundibulum, neural stalk and posterior lobe from diencephalon • Development 3rd to the 15th week gestation Pituitary Anatomy Gross • Sits in sella turcica • Surrounded by dura • Sphenoid – Lateral and inferior • Lateral – Cavernous sinus • Internal carotid artery • CN III, IV, VI, V1 and V2 Pituitary Anatomy Gross • Symmetrical bean shaped – Brownish red • • • • 13 mm transverse 9 mm AP 6 mm height Adult – 0.4-0.9 grams – Larger in women – Larger in multiparous women – During pregnancy increases to 0.9-1 grams Pituitary Anatomy Microscopic • Anterior lobe – 80% of gland – Brown color • Posterior lobe – Gray/brown color Pituitary Anatomy Microscopic • Anterior lobe 3 divisions – Pars distalis • Largest • Hormone producing cells – Pars intermedia • Poorly defined in the human – Pars tuberalis • Upward extension to the anterior lobe and attached to pituitary stalk • Posterior lobe – Pars nervosa Pituitary Gland Microscopic • Pars distalis – Pink acidophils • Growth hormone • Prolactin – Dark purple basophils • Corticotropin (ACTH) • Thyroid stimulating hormone (TSH) • Follicle stimulating hormone (FSH) • Luteinizing hormone (LH) Pituitary Portal System • Hypophyseal arteries – From carotid – Superior • 80-90% to adenophysis – Inferior • Posterior pituitary • Posterior lobe – Rich nerve supply – Unmyelinated nerves Goals of Discussion • Review pituitary anatomy • Understand pituitary physiology • Discuss pituitary hormone deficiencies Hormones Of The Anterior Pituitary • 6 main hormones secreted by the adenohypophysis: – Growth hormone • Somatotropin – Thyroid-stimulating hormone • Thyrotropin – Adrenocorticotropic hormone • Corticotropin – Prolactin – Follicle-stimulating hormone – Luteinizing hormone Anterior pituitary Hypothalamic product Pituitary product Target organ Hormone product CRH ACTH Adrenal cortex Cortisol TRH TSH Thyroid T4, T3 GHRH (+) SRIH (-) GH Liver; Tissues IGF-I (systemic) IGF-I (local) PRIH (dopamine) PRL Breast [Lactation] GnRH LH, FSH Gonad Sex hormones (LHRH) Hormone Structure Polypeptide/proteins ACTH Polypeptide GH Protein PRL Protein Amino acids/Source 39 191 199 Corticotroph Somatotroph Lactotroph Glycoproteins TSH Alpha* / TSH-beta 110 LH Alpha / LH-beta 115 FSH Alpha / FSH-beta 115 Thyrotroph Gonadotroph Gonadotroph [hCG Alpha / beta-hCG] 147 * 92 amino acids [Placenta] GH_AXIS_ HYPOTHALAMUS (-) HYPOTHALAMICPITUITARY PORTAL SYSTEM SRIH (-) POSTERIOR PITUITARY GHRH (+) ANTERIOR PITUITARY INCR. [FFA] DIRECT INSULIN RESISTANCE EFFECTS GH TISSUES IGF-I IGFBP-3 GROWTH HYPOTHALAMUS (-) HYPOTHALAMICPITUITARY PORTAL SYSTEM (-) CRH (+) ANTERIOR PITUITARY POSTERIOR PITUITARY ACTH ADRENAL Fasiculata CORTISOL HYPOTHALAMUS (-) HYPOTHALAMICPITUITARY PORTAL SYSTEM (-) TRH (+) ANTERIOR PITUITARY POSTERIOR PITUITARY TSH THYROID GLAND T4, T3 (T4 --> T3) HYPOTHALAMUS PRIH (DOPAMINE) (-) POSTERIOR PITUITARY ANTERIOR PITUITARY PRL BREAST HYPOTHALAMUS (-) HYPOTHALAMICPITUITARY PORTAL SYSTEM GnRH (-) (LHRH) (+) ANTERIOR PITUITARY POSTERIOR PITUITARY LH, FSH GONAD SEX HORMONES, INHIBIN Posterior pituitary Hypothalamic source (cell body) Target Effect ADH Collecting duct H2O retention Oxytocin Breast Uterus Milk let down Smooth muscle Contraction Goals of Discussion • Review pituitary anatomy • Understand pituitary physiology • Discuss pituitary hormone deficiencies History • 15yr old WF presents with secondary amenorrhea, polydipsia and polyuria • Normal growth and development • Menarche at 11 years of age – Qmonth menses until 12 years of age – Withdrawal bleeding only with OCP’s History • Drinks 32 oz water Q34hrs during the day • Drinks and urinates Q23hrs at night • ROS: occasional headaches, fatigue and difficulty losing weight Physical Exam • • • • • Wt 62.9kg (75%) Ht 5ft 3.5in (50%) BMI 24.2 kg/m2 HR 80 B/P 117/86 • General: nondysmorphic, wellnourished • HEENT: visual fields intact, no thyromegaly • Breast: no discharge, Tanner V • GU: Tanner V Differential Diagnosis Hypopituitarism • Isolated hormone deficiencies – Acquired or congenital • Tumors – – – – Pituitary adenomas Pituitary apoplexy Hypothalamic tumors Metastatic carcinoma • Inflammatory – Granulomatous disease • Sarcoidosis, TB and syphilis – Eosinophilic granuloma – Lymphocytic hypophysitis Differential Diagnosis Hypopituitarism • Vascular disease – Sheehan’s postpartum necrosis – Carotid aneurysm • Destructive – Surgery – Radiation – Trauma • Infiltration – Hemochromatosis – Amyloidosis Hypopituitary Presentation • Growth hormone production – First hormone to be disrupted • Gonadotropin deficiency – Easily disrupted • Corticotropin – Less frequently affected • Thyrotropin – Rarely affected • Anti-diuretic hormone – Deficiency usually due to tumor – Craniopharyngioma Hypopituitary Presentation • Growth hormone deficiency – Children • Short stature – Adults • Non specific • Fine wrinkling around the face • Improved insulin sensitivity Hypopituitary Presentation • Gonadotropin deficiency – Women • Amenorrhea – Primary or secondary • Infertility – Men • Decreased libido • Decreased beard and body hair Hypopituitary Presentation • Corticotropin deficiency – – – – – Fatigue Decreased appetite Weight loss Decreased pigmentation Abnormal response to stress • Hypotension • Hyponatremia • Fever • Primary Adrenal Insufficiency – – – – – – – Addison’s disease Fatigue Decreased appetite Weight loss Increased pigmentation Hyperkalemia Abnormal response to stress • Hypotension • Hyponatremia • Fever Hypopituitary Presentation • Hypothryoidism – – – – Fatigue Cold intolerance Puffy skin Absence of goiter • Diabetes Insipidus – Polyuria – Polydipsia Evaluation • What testing? – Polydipsia and polyuria • Water deprivation test – Secondary amenorrhea • Prolactin • Gonadotropins • Thyroid function Laboratory • Water deprivation test reveals diabetes insipidus • MRI – pituitary seen, no masses, subtle thickening of 3rd ventricle floor and no hyperintense neurohypophysis in sella noted • TSH 1.61 ug/dl (0.35-5.54) • T4 8.4 uIU/ml (4.0-12.8) Laboratory • • • • • • Cortisol 0800 15.5 ug/dl (5-25) ACTH 14 pg/ml BHCG <5 mIU/ml Prolactin 5 ng/ml (3-27) Estradiol 1.3 ng/dl (3.4-17) ESR 101 Laboratory • • • • FSH 6.9 mIU/ml (Tanner V 1.0-9.2) LH 7.1 mIU/ml (Tanner V 0.4-11.7) IGF-1 207 ng/ml (217-589) Skeletal Xray: no lesions and epiphyses closed. • Dopamine arginine GH stimulation test <5ng/ml Treatment • Growth hormone therapy • Estrogen and progesterone – Birth control pills • Testosterone – Cypianate or enanthate • 200 mg IM Q2 weeks – Gels 5-10 gram per day • Fertility – Refer to Reproductive Endocrinologist • Thyroid – – – – Levothyroxine (generic) Synthroid Levoxyl Unithroid • Dose ranges 75-150 mcg per day Treatment • Cortisol – Hydrocortisone • 10mg AM and 5 mg PM • 6-8 mg/m2/day • Stress dosing – – – – Fever, illness, surgery 20 mg/m2/day Double or triple daily dose 100 mg x1 then 25-50 mg Q6-8hrs • All hypopituitary patients need a medic alert bracelet Treatment • Desmopressin (DDAVP) – Nasal spray • 10 mcg QD-BID – Tablets • 0.1 to 0.2 mg QD-BID – SQ injection • 1-2 ug QD-BID Treatment • DDAVP nasal spray 10mcg QD • Ortho-novum 777 • Growth hormone therapy