* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Psoriasis - Dermweek
Epidemiology wikipedia , lookup
Gene therapy wikipedia , lookup
Gene therapy of the human retina wikipedia , lookup
Fetal origins hypothesis wikipedia , lookup
Epidemiology of metabolic syndrome wikipedia , lookup
Public health genomics wikipedia , lookup
Preventive healthcare wikipedia , lookup
Psoriasis
Dr. Lyn Guenther, MD FRCPC
Professor of Dermatology UW O
Medical Director, The Guenther Dermatology Research Centre
Objectives
Very brief Overview today (more in group discussion)
•
State the prevalence of Psoriasis
•
Briefly discuss the pathogenesis of psoriasis
•
Describe the variants of psoriasis
•
Give an overview of the treatment of psoriasis
•
Discuss the burden of disease/QOL
Psoriasis
•
W hen does it onset?
Can onset from birth to 108 years
– 2 peaks
–
•
Type I age 20-30 onset, familial
• Type II age 60, not familial
•
How common is it?
~2% of population
– An estimated 1 million Canadians have psoriasis1
–
1. Guenther L et al. J Cut Med Surg 2004;8:321-37
Psoriasis
WWhat causes it?
–
Autoimmune with activated T cells
Nonlesional Skin
–
Psoriatic Plaque
7-fold increase in transit rate of epidermal cells
Pathogenesis of Psoriasis
DC
DC
Naïve
T cell
Naïve
T cell
IL-23
Cytokines
including
IL-17
IL-22
TNF-α
IL-12
Th17
Th1
Cytokines
including
IFN-γ
TNF-α
IL-2
Inflammation, keratinocyte hyperplasia, neovascularization,
vasodilatation, T cell/neutrophil influx
Plaque formation
Shear N, et al. J Cutan Med Surg 2008;2 Suppl 1:S1
Wilson NJ, et al. Nat Immunol 2007;8:950
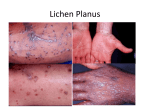
Psoriasis Vulgaris (Plaque Psoriasis)
•
Red, scaly, usually well
demarcated plaques
•
Elbows, knees, lower back,
buttocks and scalp commonly
affected
•
May be generalized
•
May be aggravated/triggered by:
– Beta blockers
–
Lithium
– Antimalarials
– ACE inhibitors
•
May occur in areas of injury
Guttate Psoriasis
•
Many small, drop-like
(gouttes) lesions suddenly
develop
•
Face commonly affected
•
Primarily in children and
young adults
Usually associated with
Streptococcal infections
•
Intertriginous (flexural) Psoriasis
•
Under folds
•
Under breasts
•
Groin
•
Axillae
•
May have minimal scale
Erythrodermic Psoriasis
•
Generalized, inflammatory
redness and scaling
•
Chills, hypothermia
•
Edema
•
Consider other causes:
– Drug reactions
– Atopic Dermatitis
– Contact Dermatitis
– Infections
Palmar Plantar Pustulosis
•
0.05% of population
• Male:female=1:4
• 95% are smokers at the onset of the
disease
• Sterile pustules
• May be associated with psoriasis
vulgaris
– 6-25%
• Difficult to treat
– Recalcitrant to current treatments
– High recurrence rates
Acropustulosis
Distal phalynx
•Often after trivial injury or
infection
•Blisters/pustules burst
•Red, glazed, scaly, crusty
•
Generalized Von Zumbusch Pustular Psoriasis
•
Unstable, reactive form
•
Tender skin with pinpoint
pustules
•
Flexures and genitalia often
affected
•
Fever, malaise, ↑W BC
•
Acutely ill; may die
Nail changes
Pitting
Onycholysis + Oil drop changes
•
In 25-50% of patients
•
Often associated with arthritis
•
Pits most common
•
Onycholysis
•
Oil drop changes
•
Splinter hemorrhages
•
Nail plate thickening and
crumbling
Psoriatic Arthritis
•
In 20-40% of patients
•
Usually onsets 10 years after skin
•
Single or multiple inflamed joints
•
Small joints of hands and feet
– May have flexion deformities
•
Back (spondylitis)
•
May be mutilating
• Anti-TNFs can prevent
radiographic progression
•
Distal interphalangeal Psoriatic Arthritis
•
Enthesitis
Often severe nail changes
Psoriatic arthritis
•
Caspar classification (Classification of Psoriatic Arthritis Study Group)
Inflammatory MSK disease (joint, spine or enthesitis)
+ 3+ of the following:
–
•
Evidence of psoriasis (Max of 2) (Current (2), history, family
history)
• Psoriatic nails
• Negative RF (N.B. up to 15% with PSA have RF)
• Dactylitis (Current or history)
• Radiological evidence of juxta-articular new bone formation
–
98.7% specificity, 91.4% sensitivity
Treatment Approach for Psoriasis
•
Amenable to Topical
Therapy
•
Not amenable to topical
therapy
Traditional Psoriasis Treatment Paradigm
•
Patients must fail the
previous “step” of therapy
before initiating a more
“aggressive” therapy
Systemic Therapy
• Cyclosporine
• Methotrexate
• Acitretin
Phototherapy
• UVB broadband
• UVB narrowband
• PUVA
OTC Products
• Emollients
• Other
Rx Topical Agents
• Topical steroids
• Vitamin D analogs
• Topical retinoids
• Calcineurin
inhibitors
• Tar
Typical Order of Treatment Progression
Panel Consensus - Integrating biologic agents in
the management of moderate-to-severe psoriasis
Biologic agents: First-line therapy for moderate-to-severe psoriasis along
with phototherapy & traditional systemic agents
Guenther L et al. J Cutan Med Surg. 8:321-37,2004.
Individual Patient Circumstances
•
•
•
•
•
•
Failure of previous therapy (lack of efficacy +/- A/E’s)
Distance from phototherapy and ability to attend
Contraindication to therapy
– Active, severe infections
– Liver disease
– Ethanol abuse
– Hypertension
– Renal disease
– Hyperlipidemia
– History of malignancy
– Photosensitivity
– Drug interactions
– TB
– CHF
– Demyelinating diseases
– Thrombocytopenia, low CD4+ counts
Need for monitoring
Availability of refrigeration
Desire for injections
Generalized Plaque Psoriasis
•
32-year-old farmer
• Generally healthy
•
8-year history of generalized
skin eruption
• Can be quite itchy
– Itching can keep him up
at night
• W ife tired of vacuuming up
scales
• WW on’t swim
• Barber refuses to cut his hair
due to scales and bleeding
scalp lesions
Psoriasis has a significant Physical impact
Congestive Heart
Failure
**Lower scores reflect worse
35
Psoriasis
patient-reported outcomes
41
Diabetes
42
Chronic Lung
Disease
42
MI
43
Arthritis
43
Hypertension
44
Depression
45
Cancer
45
0
10 20 30 40 50
Physical Component
Summary Score
Rapp SR, et al. J Am Acad Dermatol. 1999;41:401-407.
Ware JE Jr, et al. SF-36® Health Survey Manual and Interpretation Guide. The Health Institute; 1993.
.
Psoriasis has a significant Mental impact
Depression
**Lower scores reflect worse
patient-reported outcomes.
35
Chronic Lung
Disease
44
Psoriasis
46
Arthritis
49
Cancer
49
Congestive
Heart Failure
50
Diabetes
52
Hypertension
52
MI
52
0
10
20 30 40 50
Mental Component
Summary Score
60
Rapp SR, et al. J Am Acad Dermatol. 1999;41:401-407.
Ware JE Jr, et al. SF-36® Health Survey Manual and Interpretation Guide. The Health Institute; 1993.
NAT I O NAL PS O R IAS I S F O U N DAT I O N PAT I E N T S U R V EY
Emotional Impact of Psoriasis
18- to 34- Year-Old Respondents
Concern That Disease Would Worsen
88%
Feelings of Embarrassment
81%
Feelings of Unattractiveness
75%
Depression
54%
Contemplation of Suicide
10%
0
10 20 30 40 50 60 70 80 90 100
Percentage
Krueger G, et al. Arch Dermatol. 2001;137:280-284.
NAT I O NAL PS O R IAS I S F O U N DAT I O N PAT I E N T S U R V EY
Social Impact of Severe Psoriasis
Telephone interview of patients with >10% BSA (n=502)
Psoriasis Mistaken as Contagious
57%
Psoriasis Mistaken as Other Disease
Trouble Receiving Equal Treatment
in Service Establishments
48%
40%
(e.g. hair salons, pools, health clubs)
0 10 20 30 40 50 60 70 80 90 100
Percentage of Respondents
Krueger G, et al. Arch Dermatol. 2001;137:280-284.
Psoriasis impacts patients
•
Personal appearance
•
Itching
•
Anxiety/Depression
•
Choice of clothing
•
Daily activities
•
Leisure activities
•
W ork/school
•
Personal relationships including intimacy
•
Finances
•
5% decreased life span with moderate-to-severe psoriasis1
1, Gelfand JM et al. Arch Dermatol 2007;143:1493-9.
Cardiovascular/Metabolic Co-morbidities in
Psoriasis Patients
•
CV disease & risk factors increased
– Myocardial infarction
(severe psoriasis ~7-fold)2
– Hypertension (~2-fold)3
– Obesity (~2-fold)3,4
1
Diabetes (~1.5-fold)3
– Metabolic syndrome (~2-fold) 5
– Increased CV mortality among
inpatients (~1.5-fold)6
–
1. Kimball AB, et al. Dermatology 2008;217:27
2. Gelfand JM, et al. JAMA 2006;296:1735
3. Henseler T, Christophers E. J Am Acad Dermatol 1995;32:982
4. Herron MD, et al. Arch Dermatol 2005;141:1527
5. Sommer DM, et al. Arch Dermatol Res 2006;298:321
6. Mallbris L, et al. Eur J Epidemiol 2004;19:225
Phototherapy
•
UVB
•
PUVA (Psoralen + UVA)
•
2-5 times/wk
•
Access problems (# centers, hours)
•
Contraindications:
–
Photosensitivity, LE
– Skin cancer
– Photodamage
•
Adverse events:
–
Sunburn
– Skin cancer
– Photoaging
Traditional Systemics
•
Methotrexate
–
–
•
Once a week
Hepatotoxicity, GI intolerance, bone marrow toxicity,
pulmonary fibrosis, teratogenic
Cyclosporine
2.5-5 mg/kg/day (BID dosing)
– Nephrotoxicity, hypertension, tremors, hyperlipidemia
– Drug interactions (cytochrome P450)
–
•
Acitretin
–
–
–
Hyperlipidemia
Skeletal changes
Teratogenic (2-3 yrs)
Biologic Agents
•
•
Large, well controlled studies
– Good efficacy, safety & tolerability
– Few drug interactions (Caution with other immunosuppressants)
– Have a significant impact on QOL in psoriasis
– Long-term safety data still pending
5 approved Biologics
– T cell agents:
• Alefacept (Amevive)
– Anti-TNF agents (also
• Adalimumab (Humira)
• Etanercept (Enbrel)
• Infliximab (Remicade)
help psoriatic arthritis)
– Anti-IL-12/23
• Ustekinumab
Guenther L et al. J Cutan Med Surg 2004;321-337
Biologics target key steps in psoriasis
Alefacept
↓
Ale↓acept
DC
DC
Naïve
T cell
Naïve
T cell
Ustekinumab →
IL-23
Cytokines
including
IL-17
IL-22
TNF-α
IL-12
Th17
Th1
←Ustekinumab
Cytokines
including
IFN-γ
TNF-α ←
IL-2
{
Etanercept
Infliximab
Inflammation, keratinocyte hyperplasia, neovascularization,
vasodilatation, T cell/neutrophil influx
Plaque formation
Shear N, et al. J Cutan Med Surg 2008;2 Suppl 1:S1
Wilson NJ, et al. Nat Immunol 2007;8:950
Psoriasis responds to Biologics
Baseline
12 weeks