* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Introduction to the Bloodborne Pathogen Standard
Epidemiology of HIV/AIDS wikipedia , lookup
Diseases of poverty wikipedia , lookup
Forensic epidemiology wikipedia , lookup
Compartmental models in epidemiology wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
HIV and pregnancy wikipedia , lookup
Canine parvovirus wikipedia , lookup
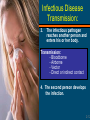
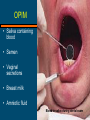
Bloodborne and Airborne Pathogens Introduction to the Bloodborne Pathogen Standard Chapter 1 McGraw-Hill/Irwin Copyright ©2009 by the National Safety Council. All rights reserved. OSHA Bloodborne Pathogen Standard • Designed to eliminate or minimize employees’ exposure to human blood and other potentially infectious materials (OPIM) in the workplace • Went into effect in 1992 1-3 Who is covered? • All employees who may reasonably expect to be exposed to blood and OPIM that may contain pathogens • Anyone whose job involves handling or possibly being exposed to blood or blood products, or OPIM 1-4 What are pathogens? Germs transmitted from one person to another • Germs transmitted from one person through contact with bloodtooranother OPIM through contact with blood or OPIM Microscopic Germs 1-5 Caution! You do NOT need to directly contact someone carrying a bloodborne pathogen to be at risk for exposure! Risks also come from: • Clinical specimens • Biohazardous trash • Blood- or body fluid-soaked laundry • Needles or sharps 1-6 Annual Training Required: • How diseases are transmitted and their symptoms • Protective measures to prevent exposure • Procedures to be followed if exposed 1-7 Exposure Control Plan • OSHA requirement • Must describe: – – – – Exposure prevention Engineering and work practice controls Universal precautions Personal protective equipment • OSHA record keeping requirements 1-8 Other Regulations • Needlestick safety and prevention act – Identify, evaluate, and implement safer medical devices – Keep sharps injury log 1-9 Bloodborne Pathogens Chapter 2 McGraw- Copyright ©2009 by the National Safety Council. A Infectious Disease Transmission Stages of Disease Stages of Disease Transmission: Transmission: 1. Someone has the infection. 2. The infectious pathogen leaves the infected person’s body. 2-11 Infectious Disease Transmission: 3. The infectious pathogen reaches another person and enters his or her body. Transmission: Transmission: -- Bloodborne Bloodborne -- Airborne Airborne -- Vector Vector -- Direct Direct or or indirect indirect contact contact 4. The second person develops the infection. 2-12 Serious Bloodborne Pathogens • Hepatitis B virus (HBV) • Hepatitis C virus (HCV) • Human immunodeficiency virus (HIV) HIV Virus 2-13 Measures • Measures you take to prevent HBV, HCV, and HIV also help prevent diseases caused by other bloodborne pathogens 2-14 OPIM • Saliva containing blood • Semen • Vaginal secretions • Breast milk • Amniotic fluid Blood in saliva during dental exam 2-15 OPIM • Cerebrospinal fluid • Synovial fluid • Pleural fluid 2-16 OPIM • Peritoneal fluid • Pericardial fluid • Any body fluid visibly contaminated with blood (such as vomit or urine) 2-17 Do Exposures Always Cause Infection? NO • Whether pathogens are present in the source blood or body fluid The risk of infection after an exposure depends on: • The type of injury or exposure • The number of pathogens present • Your current health and immunization status 2-18 Hepatitis B 2-19 Hepatitis B • Caused by hepatitis B virus (HBV) • Transmitted by blood and OPIM • Found in all body fluids • Blood and semen are the most infectious 2-20 Hepatitis B • Major cause of liver damage, cirrhosis, and liver cancer • Infections are declining • Still infects about 60,000 people yearly • About 3,000-5,000 people die of liver problems associated with HBV infection every year 2-21 HBV • Incubation period averages 12 weeks • Infection can – Cause acute hepatitis or – A chronic (long-term) infection • Chronic HBV can be infectious for decades 2-22 How is HBV Spread? • Injection – Needlesticks – Puncture wounds • Mucous membranes – Eyes and mouth – Nonintact skin (abrasions) • Sexual activity • Infected mother to newborn at birth 2-23 HBV Transmission • Contaminated environmental surfaces • At room temperature HBV may survive for several days in dried body fluids on surfaces • HBV more easily transmitted than HIV: - Lives longer outside the body - Little blood needed to cause infection 2-24 HBV not transmitted by: • Food or water • Fecal matter • Through the air – sneeze or cough • Casual contact – shaking hands, hugging, kissing, or sharing a meal, utensils, or a drinking glass 2-25 Symptoms of HBV About 30% have no symptoms at all Flu-like symptoms may appear gradually Loss of appetite Nausea, vomiting Fatigue Muscle or joint aches Mild fever Stomach pain Occasionally jaundice 2-26 How Do I Know If I Have HBV? • Only certain way to know is to have a blood test • Blood test may not indicate the virus shortly after being infected 2-27 Hepatitis B Vaccine • Best protection • No risk of developing hepatitis • Three doses given by injection on three different dates • Most common reaction is soreness at the injection site 2-28 HBV Vaccine Recommended: • Employees at risk • Those who have unprotected sex with a partner who has HBV or have sex with more than one partner • People who have anal sex 2-29 HBV Vaccine Recommended: • Those who use intravenous recreational drugs • People with hemophilia • Those who frequently travel to or live in countries where HBV is common • Those who live with someone with lifelong HBV 2-30 HBV Vaccine Effectiveness • Prevents hepatitis B in ~ 95% of people • After receiving the three shots, you can be tested to make certain you are protected • Important if you have a compromised immune system or your job frequently exposes you to human blood 2-31 OSHA Standard and HBV Vaccine • Requires employers to offer the HBV vaccine to employees at risk at no cost, at a convenient time and place, and during their normal work hours • You have the right to: • Refuse the vaccine (You must sign a declination form) • Change your mind and have the vaccination at a later date 2-32 OSHA Standard Requires Employers to: • Offer training and HBV vaccine before starting a work assignment • Explain to employees that vaccination is voluntary • Make certain employees receive proper medical treatment following any exposure 2-33 Prevention of HBV Infection • Get the HBV vaccine • Use barrier devices to prevent contact with any blood and OPIM • Handle sharps carefully • Avoid recreational IV drugs, tattooing, and body piercing without sterile tools • Do not share personal items 2-34 Hepatitis C 2-35 Hepatitis C • Liver disease caused by the hepatitis C virus (HCV) • Lives in the blood of people with the disease • Spread via the blood • Incubation period averages 7 weeks • 3.2 million people in the U.S. have chronic HCV infection 2-36 Hepatitis C • About 26,000 new infections occur each year • Many people who carry HCV have some liver damage but do not get sick from it • Other people develop cirrhosis of the liver, resulting in eventual liver failure 2-37 How is HCV Spread? • Most often through drug injections with contaminated needles • Unclean tattoo or body piercing tools • Sharing contaminated toothbrushes, razors or other personal items 2-38 How is HCV Spread? • From a pregnant woman to the fetus • Rarely, though sexual contact • In healthcare, via direct contact with infectious blood through an accidental needlestick or sharps injury 2-39 Symptoms of HCV • Most infected people do not have symptoms • Some have: - Fatigue - Loss of appetite - Nausea - Anxiety - Weight loss - Alcohol intolerance - Abdominal pain - Loss of concentration - Jaundice 2-40 How Do I Know If I Have HCV? Blood test • A false positive test can occur with HCV tests • Positive tests should have a follow-up test • False negative test results may also occur with HCV usually shortly after infection when antibodies have not yet developed 2-41 HCV Testing • Anyone who has: – Been exposed to HCV-positive blood – Used intravenous recreational drugs – Received a blood transfusion or organ transplant – Been on kidney dialysis prior to 1992 – Been treated with a blood product prior to 1987 – Signs of liver disease 2-42 HCV Testing Is Important • Treatment can be given to protect the liver from additional damage • HCV carriers can take preventive measures to avoid spreading HCV to others 2-43 Prevention of HCV Infection No vaccine available for HCV and there is No cure Prevention is critical 2-44 Preventive Measures • Handle needles and other sharps with caution • Use barriers to prevent contact with blood and OPIM (wear gloves) • Avoid recreational intravenous drug use • Never reuse or share syringes, or drug paraphernalia 2-45 Preventative Measures • Don’t share toothbrushes, razors, personal care items • Get vaccinated against HBV • Remember the health risks associated with tattoos and body piercing if tools are not sterile or sanitary practices are not followed 2-46 HIV and AIDS 2-47 HIV and AIDS • Human immunodeficiency virus (HIV) causes acquired immunodeficiency syndrome (AIDS) • There are almost one million HIV-positive people in the U.S. ¼ of people are unaware of their HIV infection 2-48 HIV and AIDS • AIDS damages cells essential for immune function • People with AIDS are more susceptible to opportunistic infections • The disease is eventually fatal 2-49 How Is HIV Spread? Through an infected person’s body fluids: • • • • • Blood Semen Vaginal secretions Breast milk OPIM if blood is present 2-50 Transmission in Healthcare Some health workers are infected with HIV through workrelated exposures involving blood or OPIM 2-51 Transmission in Healthcare • Infection is most likely to occur with exposure to HIV-contaminated blood, blood components, or blood products through: • Injection through the skin • Unprotected mucous membranes • An open skin wound 2-52 HIV not Transmitted Through Casual Contact: • Sharing a drinking glass, a meal, or fork • Kissing, hugging, or touching • Sneezes or coughs • Sharing a phone or bathroom • With mosquitos, fleas, ticks, or other bloodsucking vermin 2-53 Symptoms of HIV • Many people with HIV have no symptoms • HIV can take many years to develop into AIDS Microscopic HIV Virus 2-54 AIDS Symptoms • • • • • • • • • Loss of appetite Weight loss Fever Skin rashes Swollen lymph nodes Diarrhea Tiredness Night sweats Inability to fight off infection 2-55 How Do I Know If I Have HIV? • A blood test • The result is usually positive 12 weeks after exposure • A confirmation test is recommended 6 months after an exposure 2-56 Prevention of HIV Infection No vaccine available for HIV and there is No cure Prevention is critical 2-57 Prevention of HIV Infection • Regular hand washing • Use of barriers • Universal precautions 2-58 Preventing Infection from Bloodborne Pathogens Chapter 3 McGraw-Hill/Irwin Copyright ©2009 by the National Safety Council. All rights reserved. OSHA Standard Requires employers to use strategies to reduce occupational exposures: • Engineering controls • Work practice controls • Personal protective equipment • Universal precautions 3-60 Engineering Controls • Needleless IV systems • Eye wash stations • Handwashing facilities • Sharps containers • Biohazard labels 3-61 Sharps • Needles and other sharps are a great risk to healthcare workers • Other systems are needleless, have needle shields, retractable needles, or other protective devices • Employers are required to evaluate the feasibility of such devices annually 3-62 Sharps Containers • Employers must document engineering controls being considered – OSHA requires employee input • Must be present for safe disposal of used sharps • Must be: – – – – Leak proof Puncture resistant Securely closeable Labeled with a biohazard warning 3-63 Handwashing and Eye Wash Stations • Handwashing facilities must be provided (when possible) – Waterless antiseptic hand cleanser may be provided when handwashing is not possible • Eye wash stations must be available when appropriate 3-64 Warning Labels Must be displayed on: Must be displayed on: • Containers for waste that may contain biohazardous waste • Freezers and refrigerators used for blood or OPIM • Containers used to transport, ship, or store blood or OPIM 3-65 Warning Labels Must be displayed on: • Contaminated equipment until properly cleaned • Laundry bags used to hold and transport contaminated clothing • Entrances to places containing OPIM 3-66 Infectious waste must be disposed of in labeled red containers or in containers clearly marked with a universal biohazard symbol Waste 3-67 Work Practice Controls 3-68 Work Practice Controls • Use of personal protective equipment (PPE) • Handwashing • Decontamination and sterilization of equipment and areas 3-69 Work Practice Controls • Safely handling sharps • Correctly disposing of wastes • Safely handling laundry • Work area restrictions 3-70 Handwashing Guidelines • Immediately wash any exposed skin (ideally with antibacterial soap) • Be gentle with any scabs or sores 3-71 Handwashing Guidelines • Wash all surfaces, including the backs of hands, wrists, between the fingers, and under fingernails • Wash hands immediately after removing gloves or other PPE 3-72 Waterless Handwashing • Antiseptic towelettes and waterless antibacterial handwashing liquid can be used when soap and running water are not available • After a potential exposure, a thorough scrubbing with soap and water is still recommended as soon as possible 3-73 Decontamination and Sterilization • Clean and sterilize all reusable sharps after use (i.e., knives, scissors, scalpels) • Decontaminate equipment and working surfaces, bench tops, and floors with 10% bleach solution – At end of work shift – As surfaces become obviously contaminated – After any spill of blood or OPIM 3-74 Decontamination and Sterilization • Disinfect nail brushes, etc. after handwashing 3-75 Handling Sharps 3-76 Handling Sharps: Guidelines: Guidelines: • Employers must put sharps disposal containers in easily accessible areas where sharps are used • Needles must not be recapped, removed, bent, sheared, or broken • The entire needle/syringe assembly must be disposed of in a sharps container 3-77 Handling Sharps: Guidelines: Guidelines: • A mechanical device may be used to recap a contaminated needle or remove it from a disposable syringe when necessary – The exposure control plan must specify when, why, and how this is done and by whom 3-78 Regulated Waste Regulated waste requiring Special handling: • Blood or OPIM in liquid or semi-liquid state • Items contaminated with blood or OPIM that could release liquid or semiliquid blood or OPIM if squeezed 3-79 Regulated Waste Regulated waste requiring Special handling: • Items with dried blood that could be spread by handling • Contaminated sharps • Lab specimens containing blood or OPIM 3-80 Laundry • Uniforms, clothing, and cloth supplies should be kept free from contamination when possible • Clothing that becomes contaminated with blood or OPIM must be put in special labeled and colorcoded laundry bags 3-81 Laundry • Must be sent to an approved laundry facility for cleaning • Anyone handling contaminated laundry must be trained to handle bloodborne pathogens • Never take contaminated clothing home to wash 3-82 Work Area Restrictions • Smoke In places where blood is stored/handled • Put on lip balm, hand lotion, DO NOT! or cosmetics • Eat or drink • Handle contact lenses • Store food 3-83 Work Area Restrictions DO NOT! • Put objects in your mouth where potentially infectious materials may be present (i.e.. pencils, pens) • Use a sink that is used for food preparation 3-84 Personal Protective Equipment PPE 3-85 PPE • Gloves • Jumpsuits, aprons • Eye shields, goggles • Face masks, face shields • Caps • Booties 3-86 OSHA Standard Requires that your employer: • Provide PPE at no cost • Train you how to use equipment • Must clean, repair, or replace it as needed 3-87 Medical Exam Gloves • Made of – nitrile – vinyl – latex or other • Latex allergy risk: ask for latex-free or hypoallergenic gloves 3-88 Medical Exam Gloves • Check that gloves are intact – If not, replace glove • Avoid petroleumbased hand lotions 3-89 Medical Exam Gloves • Remove contaminated gloves carefully, not touching any part of the outside of the gloves 3-90 Medical Exam Gloves • Dispose of gloves in a container clearly marked for biohazardous waste 3-91 Jumpsuits, Aprons, and Lab Coats • Can protect clothing from contamination • Available in different thicknesses and materials 3-92 Jumpsuits, Aprons, and Lab Coats • Remove contaminated clothing immediately • Avoid contact with skin • Put article in a clearly marked biohazardous laundry bag 3-93 Goggles and Eye Shields PPE for eyes includes goggles, safety glasses with side shields, and face shields 3-94 Goggles and Eye Shields • A splash in the eyes may allow bloodborne pathogens into the body • Eye protection recommended when cleaning spills or performing first aid • Use side shields with prescription glasses 3-95 Face Shields and Face Masks • Face shields protect eyes, mouth, and nose • Face masks protect the mouth and nose – With goggles or safety glasses, face masks help protect the whole face 3-96 Caps and Booties • Cover hair and forehead • Cover shoes or boots 3-97 PPE Improvise! • Be creative to avoid contact, use items including: – plastic bag – a sheet – towels or clothing • Dispose of or decontaminate any articles used as barriers 3-98 PPE •Dispose Dispose of contaminated PPE of contaminated PPE: • Different protective equipment require different disposal methods • Put articles such as used gloves in a designated disposal container • Store contaminated clothing in clearly labeled bags until decontaminated, laundered, or properly disposed of 3-99 Universal Precautions (Standard Precautions) 3-100 Universal/Standard Precautions Handle all blood and OPIM as if they are contaminated 3-101 Universal/Standard Precautions Treat all materials as if they are infected with bloodborne pathogens, including: • • • • • • Blood Semen and vaginal secretions Saliva that may contain blood Cerebrospinal fluid Synovial fluid Pleural fluid 3-102 Universal/Standard Precautions All Body Fluids OSHA now applies universal precautions to all body fluids because it is impossible to know by looking whether other body fluids may contain blood 3-103 Universal/Standard Precautions All Body Fluids • Assume that all body fluids may be infectious and always follow universal precautions • Body substance isolation (BSI) guidelines also define all body fluids and substances as infectious 3-104 For Unexpected Exposure • If blood or OPIM splashes in your eyes or other mucous membranes, flush area with running water for 20 minutes • Wash any exposed area well with soap, using an antibacterial soap 3-105 For Unexpected Exposure • Gently treat any scabs and sores • Report the exposure to your supervisor • Save any potentially contaminated object for testing purposes • Seek medical care 3-106 Employer Responsibilities • Identify and document source of blood or OPIM • Obtain consent and arrange to test the source blood • Inform you of the test results 3-107 Employer’s Responsibilities • Arrange for you to have your blood tested • Arrange counseling and medical care for you as needed 3-108 Follow-up After Exposure Treatment and medical care depend on the type of exposure: • Substance involved • Route of transmission • Severity of the exposure 3-109 Follow up After Exposure • Treatment may include HBV vaccination or hepatitis B immune globulin (HBIG) • Confidential exposure report form kept in the employee’s personnel file 3-110 Exposure Control Plan • Identify the job positions and individuals to receive training • Establish necessary engineering controls and work practice controls • Specify PPE to be used 3-111 Exposure Control Plans • Require using universal precautions • State the opportunity for HBV vaccination • Include other measures appropriate for your specific work environment • Review at least annually 3-112 Additional Employer Requirements • Inform new employees about their plan • Conduct training before performing any work that puts you at risk for exposure • Provide refresher training annually or whenever changes made to policies and procedures 3-113 Airborne Pathogens Chapter 4 McGraw-Hill/Irwin Copyright ©2009 by the National Safety Council. All rights reserved. OSHA Regulations • Specific employee protections not currently mandated Airborne Diseases • OSHA expects employers to protect employees from known hazards 4-115 Three Types of Airborne Pathogens Viral Bacterial Fungal 4-116 Airborne Precautions for tuberculosis also lower the risk for other airborne pathogens Pathogens Meningitis Influenza Pneumonia Tuberculosis 4-117 Airborne Pathogens • Spread by inhaling the germ • Coughing or sneezing tiny droplets of moisture into the air containing pathogens • Pathogens can remain airborne for several hours 4-118 Airborne Transmission Depends On: • How contagious the infectious person is • Where the exposure occurs • How long the exposure lasts • How healthy you are at the time of the exposure 4-119 Tuberculosis 4-120 Tuberculosis • 14,000 cases in 2005 in U.S. • Caused by a specific bacteria • Affects the lungs but it can also affect: – brain – spine – kidneys • Many people with TB infection are not sick (the body effectively fighting the bacteria) and are not contagious 4-121 Tuberculosis Those with TB disease are contagious • 5%-10% of people develop the disease at some point • Risk is higher for people with HIV, diabetes mellitus, severe kidney disease, low body weight, or certain types of cancer 4-122 Tuberculosis • HIV infection is most important risk factor for progression from latent TB infection to TB disease • Progression to TB disease is rapid among HIV-infected people • TB outbreaks can rapidly expand in HIV-infected patient groups • CDC recommends HIV testing for all TB patients 4-123 Employees at Risk • • • • • • Correctional facilities Drug and treatment centers Homeless shelters Healthcare facilities Long-term care facilities Morgues 4-124 How Is TB spread? • Inhaling the TB pathogen after an infected person coughs or sneezes • The TB pathogen can live up to 1½ hours outside the body • Infection detectable 2-12 weeks after infection • Some bacteria lay dormant for years 4-125 Symptoms of TB Many people with TB infection have no symptoms! With TB disease: • • • • Weight loss Fever Night sweats Weakness 4-126 Symptoms of TB If TB affects the lungs, the common symptoms include: • • • • Coughing Production of sputum Chest pain Coughing up blood 4-127 Tests to Determine TB Infection • Tuberculin skin test (Mantoux test) -Performed on the skin in lower arm -Result is checked after 2-3 days • A blood test (QFT-G) also reveals if a person is infected 4-128 Special Considerations for TB Testing Generally recommended for employees at risk because of being near people who may have TB: •• Certain Certainhealthcare healthcarefacilities facilities •• Drug Drugtreatment treatmentfacilities facilties •• Homeless Homelessshelters shelters •• Nursing Nursinghomes homes •• Prisons Prison and and jails jails 4-129 Special Considerations for TB Testing • Testing recommended for at-risk employees • Pregnant employees should be tested via TST, not GFT-G • Consider booster effect • Those with other disease or illness more likely to develop TB • Use 2-step testing for those who will take TST periodically 4-130 How Do I Know If I Have TB? • Skin and blood tests cannot distinguish between TB infection and TB disease • Chest x-ray and phlegm sample needed to determine diagnosis 4-131 Preventing TB Infection • Administrative controls • Environmental controls • Respiratory controls 4-132 Administrative Controls Consider the most important control measure: • Assign responsibility for TB infection control • Work with health department • Ensure timely lab processing and reporting • Implement effective work practices 4-133 Administrative Controls, continued Consider the most important control measure: • Test and evaluate workers at risk • Train workers about TB infection control • Ensure proper equipment cleaning • Use appropriate signage 4-134 Environmental Controls These controls remove or inactive M. tuberculosis: • Local exhaust ventilation • General ventilation • Air cleaning methods - HEPA filtration - UVGI 4-135 Respiratory Protection Controls Used in settings where other controls will not prevent inhalation of infectious droplet nuclei • Implement respiratory protection program • Conduct annual training in respiratory protection • Initial and periodic fit testing • Training patients in respiratory hygiene 4-136 TB Exposure and Recordkeeping • Exposure to a known TB source should be reported to employer • Employees have right to know about exposures • After exposure employees may be tested for TB • If infected, employer will arrange for appropriate treatment 4-137 TB Exposure and Recordkeeping • Employers must maintain records • Active TB disease must be reported to public health officials • OSHA 300 log used to record work-related exposure and infection 4-138 Treatment of TB Depends on: • Age • Overall health • Lifestyle • Occupation TB disease can be cured with antibiotics 4-139 Definition of Flu Flu is a virus that infects the respiratory tract 4-140 How Humans Spread Flu 4-141 How Humans Spread Flu Transmission Vehicles ►Hands ►Air ►Contaminated Objects 4-142 How Humans Spread Flu Entry Points Mouth Eyes Nose 4-143 Flu Symptoms • • • • • • Cough Running or stuffy nose Thick mucus Muscle pain Stiffness Fatigue 4-144 Flu Symptoms, continued • • • • • • Headache Sore throat Shaking chills Fever Dehydration Difficulty breathing 4-145 Steps to Prevent Flu 1. Hand hygiene 2. Respiratory hygiene 3. Social distancing 4. Flu shot 4-146 Hand Hygiene 4-147 Respiratory Hygiene 1. Cough or sneeze into a tissue, or into upper sleeve 2. Dispose of tissues in waste can 3. Avoid touching your eyes, nose or mouth 4. Wear a surgical mask 4-148 Social Distancing 1. Avoid crowded settings 2. If you have to be in a crowd, make the time short 3. Avoid sick people, or keep a distance of six feet 4. If you or your children are sick, stay home 4-149 Immunization • Protects from seasonal flu • Does not prevent bird flu 4-150 If You Are Sick 1. Stay home! 2. Get plenty of rest 3. Drink lots of fluids 4. Avoid alcohol and tobacco 5. Take medication 6. Call your doctor if you have a high fever 7. Wear a surgical mask 4-151 Caring for the Sick 1. One person should give care 2. Avoid mingling items 3. Disinfect objects touched by the sick 4. Wash your hands frequently 5. It is okay to mingle dishes and laundry, but wash them in very hot water 6. Wear disposable gloves 4-152 Seasonal Influenza ►Occurs every year ►Everyone gets it at some point ►Most people have some immunity and can get a vaccine for more immunity ►Can cause severe illness and death 4-153 Bird Flu ►Infects wild birds and domestic poultry ►Can have a high death rate ►Has jumped species to infect humans ►Concern that humans can infect one another if virus mutates 4-154 Epidemic An outbreak of a disease in a community or a region 4-155 Pandemic An outbreak that spreads beyond a community or region throughout the world 4-156