* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Virginia 1992-1999
Dirofilaria immitis wikipedia , lookup
Diagnosis of HIV/AIDS wikipedia , lookup
Gastroenteritis wikipedia , lookup
Epidemiology of HIV/AIDS wikipedia , lookup
Schistosomiasis wikipedia , lookup
Marburg virus disease wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Trichinosis wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Leptospirosis wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Hepatitis C wikipedia , lookup
Oesophagostomum wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
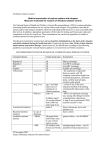
The Epidemiology of Tuberculosis Lex Gibson, Virginia TB Program TB Infection VS TB Disease Infection TB Bacilli in Body Yes PPD Usually Pos. CXR Usually Normal Sputum Smears/Cult Neg. Symptoms None Infected Yes Infectious No A “Case” of TB No Disease Yes Usually Pos. Usually Abn. Usually Pos. Cough, Fever, Wt. Loss Yes Often, before treatment Yes What is a PPD? • Intradermal test of .1ml(5TU) of purified protein derivative. • Measures TB infection • False positives(cross reactions, non-specific in low risk populations) • False negatives(technique, storage) • Read in MM of induration Reading the Mantoux Test • • • • Read in 48-72 hours Measure only raised area, not redness Measure across the widest area The diameter of the raised area should be measured • Measure and report results in millimeters Interpreting the results 5mm is positive for those: – known to have or suspected of having HIV infection – close contacts of a person with infectious TB – with a chest x-ray suggestive of previous TB – who inject drugs(if HIV status unknown) 10 mm is positive for those: – with certain medical conditions, excluding HIV infection – who inject drugs(if HIV negative) – foreign born persons from areas where TB is common – medically underserved, low income populations, including high-risk racial and ethnic groups – Residents of long term care facilities – Children younger than 4 years of age – Locally identified high risk groups Determining Infectiousness • Smear Results • CXR Findings • Symptoms Increased Risk of Transmission • Infectiousness of Source • Duration of Exposure • Environment • Susceptibility of Contact Contact Investigation • Screening individuals who have shared the same air as an infectious case of TB • Investigations are done systematically • Significant reactors receive a cxr and are evaluated for Treatment of disease or preventive therapy Concentric Circle Community Casual/Work close Scenario 1 • Twenty-eight year old school teacher has a positive PPD during a routine screening. No risk factors for TB. What do you do? • CXR shows pleural effusions. What's next? • Obtain sputum, pleural specimen, and possibly start on multiple anti-TB drugs. Sputum's are negative but pleural specimen is sm. Pos. • Now what do you do? • Contact investigation- All family members have negative PPD’s and are asymptomatic, is further testing necessary? • Normally not……unfortunately, word spread through the community that an elementary school teacher has TB. The media, parents and school system are demanding that PPD’s be done on everyone. What do you do? • Educate media, parents and school system • Your initial compromise is to skin test just one classroom rather than the entire school, but your health department receives 45% of its funding from the locality. The city council/board of supervisors wants to know why you are refusing to protect their school children from getting TB. What do you do? • If political pressure prevails and the entire school is tested, what might be some of the consequences? • This is a low risk population group, greater than 50% of the positive PPD’s identified will be false positives. Preventive treatment with INH exposes the individual to possible liver damage from the INH Scenario 2 A sputum smear, culture positive Mtb case is diagnosed in a large open factory that manufactures circuit boards. Air is recirculated within the facility. Three other cases have been diagnosed in the facility during the past three years. Over 90% of the employees are from the Philippines and previous contact investigations have demonstrated a 7080% reactor rate. Less than 7% of past positives have completed an adequate course of treatment for latent TB infection. All close family contacts are previous positive reactors. How do you proceed with the investigation? • Who would you screen and what tools would you use? • PPD past negatives in the immediate vicinity of the case, factory wide symptom assessment of past positives, and collect sputums on those with signs and symptoms TB Advances Over Time 400 B.C. Syndrome Described 1882 Bacteria Identified 1895 1934 1950 1990 X-Ray Invented PPD Available Effective Therapy DOT FUTURE ?? Funding Trends $2,100,000 $2,000,000 $1,900,000 $1,800,000 $1,700,000 1996 1997 Not adjusted for inflation nor salary increases 1998 1999 2000 Global Tuberculosis • 8-10 Million new cases/year • 2-3 million deaths/year • Tuberculosis is the 2nd leading cause of deaths by infectious diseases Tuberculosis in the U.S. • 15 million infected • 17,000 + new cases per year • TB cases decreased steadily until 1985, then increased and has now begun to decrease again TB Case Rates US &Virginia 1987-1999 11.5 10.5 9.5 8.5 7.5 6.5 5.5 4.5 19 87 19 88 19 89 19 90 19 91 19 92 19 93 19 94 19 95 19 96 19 97 19 98 19 99 3.5 US Virginia Epidemiology of Tuberculosis Virginia-1999 • • • • • 334 Cases of TB in 1999 4.9/100,000 5000+ people starting INH 77,000+ skin-tests given 4,000+ contacts identified Virginia Tuberculosis Morbidity Rate/100,000 Districts 1999 Rate/100,000 < 3 per 100,000 3.1- 5 per 100,000 5.1 - 10 per 100,000 >10 per 100,000 Virginia Tuberculosis Morbidity # Cases Districts 1999 Number of TB Cases 77 cases No Cases 1-5 6 - 15 16 - 30 > 30 Rapp/Rapidan T. Jefferson Pitt/Dan Southside W. Piedmont Miles 0 20 40 Miles 0 20 40 Virginia Tuberculosis Morbidity # Cases Districts 1999 Number of TB Cases 77 cases No Cases 1-5 6 - 15 16 - 30 > 30 Rapp/Rapidan T. Jefferson Pitt/Dan W. Piedmont Miles 0 20 40 Case rates for selected groups In Virginia(1996) • • • • • • • Homeless- 411.3 /100,000 Vietnamese- 159.5 /100,000 Guatemalan- 108.3 /100,000 Korean- 63 /100,000 Philippines-59.9 /100,000 Foreign born- 49.7 /100,000 Nursing & Adult Homes- 39.7 /100,000 Case Rates for selected groups • • • • • • Chinese- 37.7 /100,000 Corrections- 8.9 /100,000 Hispanic- 26.8 /100,000 >65 years - 17.3 /100,000 U.S. born minorities- 8.1 /100,000 U.S. born whites- 2.1 /100,000 Relative Risk of TB Disease Selected Populations 1996 U.S. Born Minorities 3.8 Foreign Born 15 Elderly(>64) 4.1 Hispanic 5.3 Asian/Pacific Isl. 13.1 Homeless Corrections 73.4 1.7 Nursing/Adult Home 7.8 0 10 20 Populations bases on 1990 Census Data 30 40 50 60 70 80 Percent of Total TB by Race Virginia -1992-1999 45 40 35 30 Hispanic Asian Black White 25 20 15 10 5 1992 1993 1994 1995 1996 1997 1998 1999 US & Foreign-Born TB Cases Virginia 1992-1999 75 70 65 60 55 50 45 40 35 30 25 1992 Foreign US Born 1993 1994 1995 1996 1997 1998 1999 % of Total TB By Age Group Virginia 1992-1999 40 35 30 25 0-14yrs 15-24yrs 25-44yrs 45-64yrs 65+yrs 20 15 10 5 0 1992 1993 1994 1995 1996 1997 1998 1999 % Foreign-Born By Age Group Virginia 1992-1999 60 50 0-14yrs 15-24yrs 25-44yrs 45-64yrs 65+yrs 40 30 20 10 0 1992 1993 1994 1995 1996 1997 1998 1999 % US Whites By Age Group Virginia 1992-1999 70 60 50 0-14yrs 15-24yrs 25-44yrs 45-64yrs 65+yrs 40 30 20 10 0 1992 1993 1994 1995 1996 1997 1998 1999 % US Blacks By Age Group Virginia 1992-1999 40 35 30 25 0-14yrs 15-24yrs 25-44yrs 45-64yrs 65+yrs 20 15 10 5 0 1992 1993 1994 1995 1996 1997 1998 1999 % Foreign-Born By Race Virginia 1992-1999 80 70 60 50 Hispanic Asian Black White 40 30 20 10 0 1992 1993 1994 1995 1996 1997 1998 1999 % Foreign-born Cases By Region* W. Pacific Americas Africa 1999 1990 SE Asia E. Med. Europe 0 *Based on WHO regions 10 20 30 40 50 Foreign-Born TB Cases Arrival to Onset of Disease 1995 - 1997 • • • • • Less than 1 year From 1 to 2 years From 3 to 5 years Over 5 years Unknown 36.1% 11.1% 15.3% 31.5% 6.0% Tuberculosis by Agegroup and Foreign-born 1999 65+ 26% 0-4 3% 5-14 1% 15-24 12% 45-64 24% 25-44 34% US-BORN 52% FOREIGNBORN 48% TB/HIV-1999 12 10 • 324 TB Cases Reported Prior to Death • 231 (72%) were offered HIV testing • 197(85%) were tested • 16 (8%) were Positive 8 6 4 2 0 15-24 25-44 45-64 65+ Agegroup % TB Cases Tested with Drug Resistance 1993-1999 18 16 14 12 10 8 6 1993 1994 1995 1996 1997 1998 1999 % Drug Resistant Foreign-Born & US Born 1993-1999 90 80 70 60 50 40 30 20 US Born Foreign 10 0 1993 1994 1995 1996 1997 1998 1999 DOT The standard of treatment Where one observes client taking meds 216 patients on DOT in 1999 66.6 % of cases on DOT in 1999 Percent 75 60 45 30 15 0 1992 1993 1994 1995 1996 1997 1998 1999 % TB Cases with Social Problems that Impact Treatment 1993-1999 25 20 15 10 5 0 1993 1994 Unemploy 1995 1996 Homeless 1997 Etoh/Drug 1998 1999 Quarantine/Legal Isolation • Intervention of last Resort • Difficult to Accomplish(weak laws, human rights issues) • Limited options for isolation (Corrections) • Have other interventions been exhausted?