* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Antimicrobial Stewardship and Formulary Management
Survey
Document related concepts
Gastroenteritis wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Neonatal infection wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Globalization and disease wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Germ theory of disease wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Marburg virus disease wikipedia , lookup
Antimicrobial peptides wikipedia , lookup
Carbapenem-resistant enterobacteriaceae wikipedia , lookup
Multiple sclerosis research wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Transcript
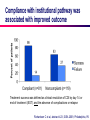
Multidisciplinary Partnerships to Reduce Clostridium difficile Infection: A Success Story Laura Johnson, MD Hospital Epidemiologist, Infectious Diseases Henry Ford Health System Rachel Chambers, PharmD Pharmacy Specialist, Antimicrobial Stewardship Henry Ford Hospital Objectives The burden and severity of Clostridium difficile infection (CDI) has dramatically increased in recent years Multidisciplinary collaboration is key to minimizing CDI in the health care setting This presentation will provide an overview of the key players and multidisciplinary interventions necessary to successfully manage and reduce CDI Clostridium difficile Infection (CDI) Bacterial infection of colon resulting in spectrum of disease from mild diarrhea to severe colitis with sepsis, toxic megacolon, and even death. Spores persist in healthcare environment and are transmitted by fecal-oral route. Hands and Environment Antibiotic exposure kills off normal protective gut flora and C. difficile can grow and produce toxins, resulting in disease. Deaths per million population Yearly Clostridium difficile–related Mortality by Listing on Death Certificates, United States, 1999–2004. Redelings MD, et al. Emerg Infect Dis. 2007;13:1417-1419 Increased and Severe CDI at HFH 2007/8: Patients noted to have severe CDI, some requiring colectomy 1988 to 2007: 8 colectomies March to May 2008: 7 colectomies Surveillance of CDI Initiated Rate per 10,000 Patient Days HFH Nosocomial C. diff Rates 2008-2009 40.0 30.0 20.0 10.0 0.0 Rate JAN FEB MA APR MA JUN JUL AU SEP OCT NO DEC JAN Feb 22.6 14.8 21.5 31.3 24.7 19.3 14.7 17.3 16.8 17.2 26.3 24.0 23.3 21.7 Benchmark 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 Investigation of Problem Infection Prevention started surveillance program Deep dive into severe CDI cases Collaboration of Infection Prevention, Pharmacy, Clinical Quality and Safety Office, and Care Providers Guidelines for C. difficile Prevention and Control CDC Prevention Strategies: Core Contact Precautions for duration of diarrhea Hand hygiene in compliance with CDC/WHO Cleaning and disinfection of equipment and environment Laboratory-based alert system for immediate notification of positive test results Educate about CDI: HCP, housekeeping, administration, patients, families http://www.cdc.gov/ncidod/dhqp/id_CdiffFAQ_HCP.html Dubberke et al. Infect Control Hosp Epidemiol 2008;29:S81-92. CDC Prevention Strategies: Supplemental Extend use of Contact Precautions beyond duration of diarrhea Presumptive isolation for symptomatic patients pending confirmation of CDI Evaluate and optimize testing for CDI Implement soap and water for hand hygiene before exiting room of a patient with CDI Implement universal glove use on units with high CDI rates Use sodium hypochlorite (bleach) – containing agents for environmental cleaning Implement an antimicrobial stewardship program http://www.cdc.gov/ncidod/dhqp/id_CdiffFAQ_HCP.html Implementing CDC Guidelines Requires a “SWOT” Team Clear guidelines to prevent and control C. difficile The challenge Implementation Sustainability C. difficile Task Force created To identify and address our “strengths, weakness, opportunities and threats” To reach multiple disciplines in hospital and facilitate buy-in To change practice and culture related to prevention and control practices C. difficile Task Force Infection prevention practitioners Providers: infectious disease, medicine, surgery, intensive care, gastroenterology Nursing (general practice, intensive care, front line and educators) Pharmacy Laboratory Environmental services Facilities/plant operations Office of clinical quality and safety Reporting to hospital leaders Examples of Collaboration Infection Prevention and Environmental Services Weekly rounds (with “bug meter”) Developed enhanced bleach cleaning protocols Laboratory and Infection Prevention Improved turn around time for lab result Developed process for daily notification of results Enhanced lab testing with better sensitivity and specificity Infection Prevention and ICU Nursing Team Developed protocol for RN-Initiated testing for CDI “Caboodles” for supplies to decrease contamination of supplies in room Eventually, protocol for “fecal transplant” for treatment of difficult cases Transportation and Nursing Identified need to keep chart clean during transport – cover chart in plastic bag during transportation Examples of Collaboration Inter-Nursing Collaboration Sticker on chart in addition to door sign for improved communication Facilities, Nursing, Infection Prevention Identified areas with limited sinks and installed sinks on multiple floors Installed wall caddies for easy access to PPE Stickers on Alcohol Hand Rub canisters Admissions Office, Nursing, Infection Prevention Extended Precautions till discharge Cohorting patients during room shortages Surgeons and Infectious Disease Team Implemented trial of probiotic yogurt in ICU Infectious Disease Fellows and Pharmacy Reviewed management of CDI cases daily with interventions as necessary Enhancement of Antimicrobial Stewardship Program – A major collaboration with pharmacy colleagues… The Case for Antimicrobial Stewardship As much as 50% of antibiotic use is inappropriate Inappropriate antibiotic use associated with poor patient outcomes, resistance development, increased health-care costs Declining antibiotic pipeline in recent years New Antibiotic Approvals 16 14 12 10 8 6 4 2 0 1983-1987 1988-1992 1993-1997 1998-2003 2004-2007 Modified from Spellberg B et al. Clin Infect Dis; 2008;46:155-64 Dellitt TH et al. Clin Infect Dis 2007;44:159-77. Dellitt TH et al. Clin Infect Dis 2007;44:159-77. Highlights of the Stewardship Guidelines Multidisciplinary collaboration: stewardship team, infection control, Pharmacy &Therapeutics Support from hospital leadership and medical staff Appropriate compensation (ideally through offices of quality/patient safety) Administrative support to track outcomes 2 core strategies: Prospective audit with intervention & feedback Formulary restriction with preauthorization Dellitt TH et al. Clin Infect Dis 2007;44:159-77. Antimicrobial Stewardship Strategies Component IDSA/ SHEA Guideline Strength of Evidence Implemented at Henry Ford Hospital Formulary restriction with audit and feedback AI Education AIII, BII Guidelines, pathways AI, AIII Antimicrobial cycling CII No Antimicrobial order form BII Combination therapy CII Not routine De-escalation AII Dose optimization AII IV to PO Conversion AII Dellitt TH et al. Clin Infect Dis 2007;44:159-77. Henry Ford Hospital (HFH) Antimicrobial Stewardship Program (ASP) What is it? A comprehensive system of health-care providers, pathways, guidelines, order sets, and informatics designed to optimize antimicrobial utilization Mission statement To improve patient outcomes through optimization of antimicrobial therapy and support the education of health-care providers in appropriate antimicrobial use 7 Strategies for a Successful Stewardship Program Cooke FJ, et al. Clinical Governance 2004 Key Element Local Action at HFH Integration into Pre-Existing Structures Quality and safety coordination of multidisciplinary CDI task force Strong Leadership Pharmacy and antimicrobial subcommittee ownership for antimicrobial stewardship Dedicated Individuals Responsible for Antibiotic Use Harnessing Existing Resources to Deliver Change Obtaining Local Data on Prescribing and Resistance Communication Education and Training Recommendations implemented by antimicrobial subcommittee of Pharmacy & Therapeutics 7 Strategies for a Successful Stewardship Program Cooke FJ, et al. Clinical Governance 2004 Key Element Local Action at HFH Integration into Pre-Existing Structures Strong Leadership Quality and Safety coordination Dedicated Individuals Responsible for Antibiotic Use Strong multidisciplinary involvement with Chief of Infectious Disease and Gastroenterology directly involved Harnessing Existing Resources to Deliver Change Support from Director of Pharmacy Services, Chief Medical Officer, Hospital Administration Obtaining Local Data on Prescribing and Resistance Communication Education and Training 7 Strategies for a Successful Stewardship Program Cooke FJ, et al. Clinical Governance 2004 Key Element Local Action at HFH Integration into Pre-Existing Structures Strong Leadership Dedicated Individuals Responsible for Antibiotic Use Harnessing Existing Resources to Deliver Change Obtaining Local Data on Prescribing and Resistance Communication Education and Training Antimicrobial Subcommittee Stewardship pharmacist Stewardship rounds with Chief of Infectious Diseases Infectious Diseases pharmacy residency program added 7 Strategies for a Successful Stewardship Program Cooke FJ, et al. Clinical Governance 2004 Key Element Local Action at HFH Integration into Pre-Existing Structures Strong Leadership Dedicated Individuals Responsible for Antibiotic Use Harnessing Existing Resources to Deliver Change Obtaining Local Data on Prescribing and Resistance Communication Education and Training Placing a higher priority on the “stewardship agenda” within existing clinical pharmacy and infectious diseases practice model Pharmacy resident project dedicated to validation of CDI management algorithm Infectious diseases fellows performed daily review of C. difficile infected patients 7 Strategies for a Successful Stewardship Program Cooke FJ, et al. Clinical Governance 2004 Key Element Local Action at HFH Integration into Pre-Existing Structures Strong Leadership Dedicated Individuals Responsible for Antibiotic Use Harnessing Existing Resources to Deliver Change Obtaining Local Data on Prescribing and Resistance Communication Education and Training Deep dive into C. difficile cases to identify “problem” antibiotics Stewardship program efficiency improved with implementation of Theradoc® decision support software 7 Strategies for a Successful Stewardship Program Cooke FJ, et al. Clinical Governance 2004 Key Element Local Action at HFH Integration into Pre-Existing Structures Strong Leadership Dedicated Individuals Responsible for Antibiotic Use Harnessing Existing Resources to Deliver Change Obtaining Local Data on Prescribing and Resistance Communication Education and Training Multidisciplinary task force members responsible for disseminating change to their department/ discipline Presentations at grand rounds and departmental meetings Policies and guidelines communicated in hard copy and on Intranet National presentations and posters to describe the work (e.g. C. difficile management algorithm presented at ICAAC 2009) Antimicrobial Stewardship Website: Guidelines and Education C. difficile Management Pathway Adapted from: Drugs 2007; 67(4):487-502 and Infection Cont Hosp Epidemiol 2010; 31:431-455. Compliance with institutional pathway was associated with improved outcome Treatment success was defined as clinical resolution of CDI by day 14 or end of treatment (EOT) and the absence of complications or relapse Richardson C et al, abstract 423, IDSA 2009, Philadelphia, PA 7 Strategies for a Successful Stewardship Program Cooke FJ, et al. Clinical Governance 2004 Key Element Local Action at HFH Integration into Pre-Existing Structures Priorities are set by antimicrobial subcommittee, identification of key messages for educational initiatives Strong Leadership Continuous improvement sought: Dedicated Individuals Responsible for Antibiotic Use • Larger role for ID pharmacist and stewardship pharmacist Harnessing Existing Resources to Deliver Change • More multidisciplinary education, ensure training is at an appropriate level for each group Obtaining Local Data on Prescribing and Resistance • Increase involvement of ID fellows, hospital epidemiology, microbiology Communication Education and Training Follow Through and Accountability Guidelines are well established and often many eager participants – but challenge is to move process forward Consistent data/messages to hospital leadership Problem identified as a priority to leaders Capital and resources Structure to support accountability Office of Clinical Quality and Safety Leaders and executive committees maintain accountability Task Force Results Rate per 10,000 Patient Days HFH Nosocomial C. diff Rates 2009-2011 30.0 25.0 20.0 15.0 10.0 5.0 0.0 Rate Jan Jan Jan Feb M ar A pr M ay Jun Jul A ug Sep Oct No v Dec Feb M ar A pr M ay Jun July A ug Sep Oct No v Dec Feb M ar A pr M ay Jun Jul A ug Sep '09 '10 '11 23.3 21.7 26.8 27.5 16.0 6.7 13.0 8.7 10.5 7.3 7.5 10.80 8.2 5.89 5.6 9.7 6.2 8.0 8.8 7.4 8.9 10.4 7.3 7.1 6.9 4.7 3.4 3.2 3.4 3.6 5.8 4.4 4.9 B enchmk 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 7.00 Summary Implementing improvement projects with sustained results requires: Thorough investigation of problem/issue Communication to key leaders and front line staff Multidisciplinary team approach Process to hold key players accountable with support from hospital leaders