* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Pulmonary Embolism
Remote ischemic conditioning wikipedia , lookup
Coronary artery disease wikipedia , lookup
Myocardial infarction wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiac surgery wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
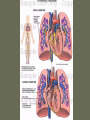
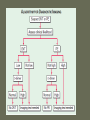
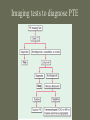
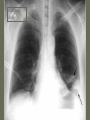
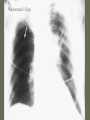
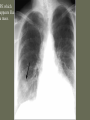
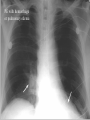
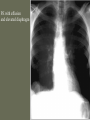
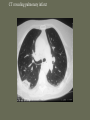
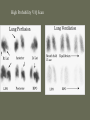
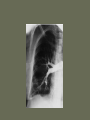
Pulmonary Embolism M.A.ZOHAL PULMUNOLOGIST • Venous thromboembolism (VTE), which encompasses deep venous thrombosis (DVT) and pulmonary embolism (PE), is one of the three major cardiovascular causes of death, along with myocardial infarction and stroke. • VTE can cause death from PE or, among survivors, chronic thromboembolic pulmonary hypertension and postphlebitic syndrome • PE is the most common preventable cause of death among hospitalized patients • Approximately three of four symptomatic VTE events occur in the community, and the remainder are hospital acquired • Approximately 14 million (M) hospitalized patients are at moderate to high risk for VTE in the United States annually: 6 M major surgery patients and 8 M medical patients with comorbidities such as heart failure, cancer, and stroke. • The long-term effects of nonfatal VTE lower the quality of life. Chronic thromboembolic pulmonary hypertension is often disabling and causes breathlessness. A late effect of DVT is postphlebitic syndrome, which eventually occurs in more than one-half of DVT patients PE • • • • • • Epidemiology Pathophysiology Prevention/Risk factors Screening Diagnosis Treatment PE • Epidemiology – Five million cases of venous thrombosis each year – 10% of these will have a PE – 10% will die – Correct diagnosis is made in only 10-30% of cases – Up to 60% of autopsies will show some evidence of past PE PE • Epidemiology – 90-95% of pulmonary emboli originate in the deep venous system of the lower extremities – Other rare locations include • • • • Uterine and prostatic veins Upper extremities Renal veins Right side of the heart Virchow’s Triad • Rudolf Virchow postulated more than a century ago that a triad of factors predisposed to venous thrombosis – Local trauma to the vessel wall – Hypercoagulability – Stasis of blood flow • It is now felt that pts who suffer a PE have an underlying predisposition that remains silent until a acquired stressor occurs Risk Factors • • • • • CHF Malignancy Obesity Estrogen/OCP Pregnancy (esp post partum) • Lower ext injury • Coagulopathy • • • • • Venous Stasis Prior DVT Age > 70 Prolonged Bed Rest Surgery requiring > 30 minutes general anesthesia • Orthopedic Surgery Risk Factors cancer, obesity, cigarette smoking, systemic arterial hypertension, chronic obstructive pulmonary disease, chronic kidney disease, blood transfusion, . long-haul air travel, air pollution, oral contraceptives, pregnancy, postmenopausal hormone replacement, surgery, and trauma Risk Factors • • • • • • • • immobilization surgery malignancy previous thrombophlebitis lower extremity trauma estrogen use Stroke 3 months post-partum. Hypercoagulability state • • • • • • • • Factor V Leiden mutation Protein C deficiency Protein S deficiency Antithrombin deficiency Prothrombin gene mutation A20210 Anticardiolipin antibodies Lupus anticoagulant Hyperhomocystinemia common predisposing factors • • • • • • • • • • cancer, systemic arterial hypertension, chronic obstructive pulmonary disease, long-haul air travel, air pollution, obesity, cigarette smoking, eating large amounts of red meat, oral contraceptives, pregnancy, postmenopausal hormone replacement, surgery, and trauma Factor V Leiden • Most frequent inherited predisposition to hypercoagulability • Resistance to activated Protein C • Single point mutation (Factor V Leiden) • Single nucleotide substitution of glutamine for arginine • Frequency is about 3% in healthy American male physicians participating in the Physicians’ Health Study PE • When venous emboli become dislodged from their site of origin, they embolize to the pulmonary arterial circulation or, paradoxically to the arterial circulation through a patent foramen ovale – About 50% of pts with pelvic or proximal leg deep venous thrombosis have PE – Isolated calf or upper extremity venous thrombosis pose a lower risk for PE Pathophysiology • • • • • Increased pulmonary vascular resistance Impaired gas exchange Alveolar hyperventilation Increased airway resistance Decreased pulmonary compliance Increased pulmonary vascular resistance • vascular obstruction • platelet secretion of vasoconstricting neurohumoral agent such as serotonin Impaired gas exchange increased alveolar dead space from • vascular obstruction, • hypoxemia : – alveolar hypoventilation relative to perfusion in the nonobstructed lung, – right-to-left shunting, – impaired carbon monoxide transfer due to loss of gas exchange surface. Alveolar hyperventilation • reflex stimulation of irritant receptors. Increased airway resistance constriction of airways distal to the bronchi Decreased pulmonary compliance • lung edema, • lung hemorrhage, • loss of surfactant Right Ventricular Dysfunction • Progressive right heart failure is the usual immediate cause of death from PE • As pulmonary vascular resistance increases, right ventricular wall tension rises and perpetuates further right ventricle dilation and dysfunction • Interventricular septum bulges into and compresses the normal left ventricle Clinical Syndromes • Pts with massive PE present with systemic arterial hypotension and evidence of peripheral thrombosis • Pts with moderate PE will have right ventricular hypokinesis on echocardiogram but normal systemic arterial pressure • Pts with small to moderate PE have both normal right heart function and normal systemic arterial pressure Diagnosis • Clinical Syndromes – Pulmonary Infarction usually indicates a small PE, but is very painful, because it lodges near the innervation of the pleural nerves Physical Signs & Symptoms Dyspnea 73% Pleuritc Pain 66% Cough 43% Leg Swelling 33% Leg Pain 30% Hemoptysis 15% Palpitations 12% Wheezing 10% Angina-Like pain 5% Common symptoms Common physical signs Cyanosis 19% Cardiac murmur 23% Thrombophlebitis 32% S3 OR S4 34% Fever 43% Tachycardia 44% Rales 58% Tachypnea 92% Diagnosis • H&P • Always ask about prior DVT, or PE – – – – Family History of thromboembolism Dyspnea is the most frequent symptom of PE Tachypnea is the most frequent physical finding Dyspnea, syncope, hypotension, or cyanosis suggest a massive PE – Pleuritic CP, cough, or hemoptysis Differential Diagnosis • • • • • • • • PE is known as “the great masquerader” pericarditis, acute coronary syndrome , MI Pneumonia, bronchitis, copd CHF Asthma Costochondritis, Rib Fx, Pneumothorax PE can coexist with other illnesses!! A Summary so Far… • History alone is unreliable • Physical exam is close to useless • However, studies have shown that our clinical suspicion of PE is useful in interpreting diagnostic tests WELLS CRITERIA • • • • Suspected DVT 3 An alternative diagnosis is less likely than PE 3 Heart rate > 100 beats / min 1.5 Immobilization>3 days or surgery within four weeks 1.5 • Pervious DVT / PE 1.5 • Hemoptysis 1 • Malignancy(on treatment or treated in past 6 1 months ) Imaging tests to diagnose PTE Diagnosis • Serum Studies – D-dimer • Elevated in more than 90% of pts with PE • Reflects breakdown of plasmin and endogenous thrombolysis • Not specific: Can also be elevated in MI, sepsis, or almost any systemic illness • Negative predictive value – ABG-contrary to classic teaching, arterial blood gases lack diagnostic utility for PE Diagnosis • CXR • A normal or nearly normal chest x-ray often • occurs in PE – Classic abnormalities include: • Westermark’s Sign - focal oligemia • Hampton’s Hump - wedge shaped density above the diaphragm • Enlarged Right Descending Pulmonary Artery (Palla’s sign) Hamptons Hump PE Westermark’s Sign PE PE which appears like a mass. PE with hemorrhage or pulmonary edema PE with effusion and elevated diaphragm Spiral CT Scan • Identifies proximal PE (which are the ones usually hemodynamically important) • Not as accurate with peripheral PE CT revealing pulmonary infarct DIAGNOSIS OF VENOUS THROMBOEMBOLISM Spiral chest CT scan DIAGNOSIS OF VENOUS THROMBOEMBOLISM Spiral chest CT scan Venous Ultrasonography • Relies on loss of vein compressibility as the primary criterion • About 1/3 of pts will have no imaging evidence of DVT • Clot may have already embolized • Clot present in the pelvic veins (U/S usually inadequate) – Workup for PE should continue even if dopplers (-) in a pt in which you have a high clinical suspicion V/Q Scan • Historically, the principal imaging test for the diagnosis of PE – A perfusion defect indicates absent or decreased blood flow – Ventilation scan obtained with radiolabeled gases – A high probability scan is defined as two or more segmental perfusion defects in presence of nl ventilation scan V/Q Scan • Useful if the results are normal or near normal, or if there is a high probability for PE – As many as 40% of pts with high clinical suspicion for PE and low probability scans have a PE on angiogram High Probability V/Q Scan Pulmonary Angiogram • Most specific test available for diagnosis of PE • Can detect emboli as small as 1-2 mm • Most useful when the clinical likelihood of PE differs substantially from the lung scan result or when the lung scan is intermediate probability Echocardiogram – Useful for rapid triage of pts – Assess right and left ventricular function – Diagnostic of PE if hemodynamics by echo are consitent with clinical hx high risk of an adverse clinical outcome • • • • Hemodynamic instability, RV dysfunction on echocardiography, RV enlargement on chest CT, Elevation of the troponin level due to RV microinfarction outcome Primary therapy • Fibrinolysis • Pharmacomechanical catheter-directed therapy • surgical embolectomy • pulmonary thromboendarterectomy Fibrinolysis (1) dissolving much of the anatomically obstructing pulmonary arterial thrombus, (2) preventing the continued release of serotonin and other neurohumoral factors that exacerbate pulmonary hypertension, (3) lysing much of the source of the thrombus in the pelvic or deep leg veins, thereby decreasing the likelihood of recurrent PE. fibrinolysis • massive PE • For patients with submassive PE, who have preserved systolic blood pressure but moderate or severe RV dysfunction, use of fibrinolysis remains controversial Secondary prevention • • • • Anticoagulant Ivc filter graduated compression stocking Intermittent pneumatic compression devices Treatment • (1) the conventional strategy of parenteral therapy “bridged” to warfarin, • (2) parenteral therapy “bridged” to a novel oral anticoagulant such as dabigatran (a direct thrombin inhibitor) or edoxaban (an anti-Xa agent) • (3) oral anticoagulation with rivaroxaban or apixaban (both are anti-Xa agents) parenteral therapy three heparin-based parenteral anticoagulants are: (1) unfractionated heparin (UFH), (2) low-molecular-weight heparin (LMWH), (3) fondaparinux. For patients with suspected or proven heparininduced thrombocytopenia, there are two parenteral direct thrombin inhibitors: argatroban and bivalirudin Treatment • Begin treatment with either unfractionated heparin or LMWH, then switch to warfarin (Prevents additional thrombus formation and permits endogenous fibrinolytic mechanisms to lyse clot that has already been formed, Does NOT directly dissolve thrombus that already exists) • Warfarin for atleast 3 months, INR 2-3 IVC filter indication (1) active bleeding that precludes anticoagulation (2) recurrent venous thrombosis despite intensive anticoagulation. Softer indication: • Prevention of recurrent PE in patients with right heart failure who are not candidates for fibrinolysis • prophylaxis of extremely high-risk patients IVC filter graduated compression stocking Intermittent pneumatic compression devices Conclusion • PE is often a misdiagnosed clinical disorder. • Rapid identification and appropriate treatment may often prevent unnecessary morbidity and mortality.