* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download mmol/L
Survey
Document related concepts
Transcript
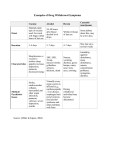
ACUTE GASTROENTERITIS IN CHİLDREN Prof. Dr. Tufan KUTLU • Each day,the adult human gut handles 7 liters of endogenous secretions (salivary, gastric, biliary, pancreatic, intestinal) and 2 liters of ingested fluids. Of this large volume, 3 to 5 liters are absorbed by the jejunum, 2 to 4 liters by the ileum, and 1 to 2 liters by the colon. Only 100 to 200 ml are lost in the stools. • Diarrhea – Increase in the number of stools or a decrease in their consistency Acute gastroenteritis • In Europe the incidence of diarrea ranges from 0.5 to 1.9 episodes per child per year in children up to 3 years of age • In low and middle income countries the incidence of acute diarrhea has declined from 3.4 episodes/child/year in 1990 to 2.9 episodes/child/year 2010 Causes of acute gastroenteritis in children • Bacteria • Viruses • Parasites Bacteria causing diarrhea • • • • • • • • • Vibrio sp Escherichia coli Salmonella sp Campylobacter sp Clostridium difficile Clostridium perfringens Bacillus cereus Staphylococcus aureus Yersinia enterocolitica • • • • • • • • Aeoromonas hydrophila Klebsiella sp Enterobacter sp Proteus sp Citrobacter sp Edwardsiella tarda Pseudomonas aeroginosa Plesiomonas shigelloides.. Viral agents causing diarrhea • Reoviridae: rotavirus, astrovirus • Parvo-like viruses: Norwalk virus • Picornavirus: calicivirus, adenovirus, coronavirus Parasites causing diarrhea • • • • • • • Giardia lamblia Cryptosporidium Entamoeba histolytica Isospora belli Cyclospora sp Blastocystis hominis Microsporidium Patophysiology of infectious diarrhea • Invasion and destruction of the villous intestinal epithelial cells: Shigella dysenteria, E. coli (EIEC), Yersinia enterocolitica, Campylobacter jejuni, Entamoeba histolytica, Salmonella, rotavirus • Enterotoxin production: Vibrio cholera, E. Coli (ETEC), Shigella dysenteria, Campylobacter jejuni, Clostridium difficile, Yersinia enterocolitica, Salmonella, Staphylococcus aureus, Bacillus cereus, Clostridium perfringens • Adherence to enterocytes: E. coli • Invasion of the lamina propria: Salmonella Diagnosis • Vomiting, profuse watery diarrhea (non blood, non mucus): secretory diarrhea – Bacteria: Vibrio cholera, E. coli (ETEC), S. aureus, B. cereus, C. perfringens – Viruses: Rotavirus, Norwalk virus – Parasites: Giardia lamblia, Cryptosporidium Diagnosis • Fever, abdominal pain, tenesmus: inflammatory colitis, ileitis – Bacteria: Shigella, Yersinia, C. difficile – Parasite: Entamoeba histolytica Diagnosis • Bloody diarrhea – Bacteria: Shigella, E. Coli (EIEC), Yersinia, C. jejuni, C. difficile, Salmonella – Parasite: Entamoeba histolytica • Fever and abdominal pain like acute appendicitis: Yersinia enterocolitica Diagnosis • Recent exposure to antibiotics: Clostridium difficile • Many cases affected simultaneously: S. Aureus, C. perfringens • Immunodeficiency, malnutrition: Salmonella, Rotavirus, Isospora, Cryptosporidium, Candida Diagnosis • Stool examination – Presence of erithrocytes and leucocytes: Shigella, E. coli (EIEC, EHEC), Campylobacter,Yersinia, Clostridium – Presence of erithrocytes: Entamoeba histolytica Diagnosis • Stool examination – Microscopic: Parasites (entamoeba, giardia..) – Antigens: Entamoeba, Giardia, Rotavirus, Adenovirus – Culture ? Viral gastroenteritis • Diarrheal diseases caused by viral agents occurs for more frequently than does similar disease of bacterial origin • Rotavirus is responsible for 20 to 70 % of hospitalization for diarrhea among children worldwide • Transmission is primarly from person to person • Most commonly in children between 6 and 24 months of age Viral gastroenteritis • Clinical manifestations – – – – – Incubation period: 48-72 hours Sudden onset of diarrhea and vomiting Diarrhea is watery, rarely bloody, 2-8 days Fever Respiratory symptoms Viral gastroenteritis • Diagnosis – Rota/adenovirus antigen in stools • Treatment – Continue with unrestricted oral feeding – Dehydration • Mild/moderate: oral rehydration treatment • Severe: intravenous fluid Shigella dysenteriae (flexneri, boydii, sonnei) • Clinical manifestations – – – – – – – Fever, malaise Watery diarrhea, blood and mucus Cramping abdominal pain Seizures Arthritis Purulent keratitis Hemolytic-uremic syndrome Shigella dysenteriae • Treatment – Trimethoprim-sulfometoxazole, ampicillin, nalidixic acid, ceftriaxone – Antimicrobial treatment is recommended to • shorten the course of the disease • decrease the period of excretion of the organisms • decrease the secondary attack Yersinia enterocolitica (pseudotuberculosis, pestis) • Clinical manifestations – – – – – – Fever Abdominal pain Diarrhea Pseudoappendicular syndrome Erythema nodosum Reactive arthropathy • Campylobacter jejuni – C. jejuni is a significant cause of diarrhea in children jounger than 2 years of age. – Treatment: erythromicin • Clostridium difficile – Antibiotic associated diarrhea – Treatment: metronidazole, vancomicin, probiotics Cholera • Clinical manifestations – Vomiting – Profuse vatery diarrhea (rice-vater appearence) • Treatment – Rehydration (ORT, IV) – Antibiotics: Tetracycline, furazolidone, ampicillin, chloramphenicol, trimethoprim-sulfometoxazole Salmonella enteridis, cholerasuis, typhi • • • • • 1. Acute gastroenteritis 2. Focal non intestinal infection 3. Bacteremia 4. Asymptomatic carrier state 5. Enteric fever Salmonella • Salmonella is spread with cotaminated water, foods (meat, eggs, milk) • Clinical manifestations – Incubation periode 12-72 hours – Fever, watery diarrhea, blood and/or mucus • Treatment – Patients at high risk (immunocompromized patients, hematologic disease, artificial inplants, severe colitis) – Ampicillin, chloramphenicol, trimethoprimsulfometoxazole, cephalosporins Escherichia coli • • • • • Enteropathogenic Enterotoxigenic Enteroinvasive Enterohemorragic Enteroaggregative and diffuse-adherant Traditional treatment of diarrhea Treatment Disadvantages Intravenous rehydration Hospitalization Increased risk of infection Unnecesssary laboratory investigations Emotional trauma Increased cost Diet Weight loss Risk of malnutrition Antibiotic and antidiarrheal drugs Ineffective Toxic Allergic Risk of secondary infections Treatment of acute gastroenteritis • Treatment of a child with moderate dehydration in hospital (USA) – ORT: 11 hours and 270 USD – IV : 103 hours and 2300 USD Treatment of acute gastroenteritis • Rehydration: IV, ORT • Nutrition • Medical – Antibiotics: bloody diarrhea, infants <3-6 months – Antisecretory drugs • Racecadotril – Adsorbant drugs • Smectite – Anti motility agents – Zinc – Probiotics Assessment of dehydration in children Non Moderate Severe Good İrritable Eyes Normal Sunken Lethargic, hipotonic or comatose Grossly sunken Tears Present Absent to reduced Absent Mucous membranes Moist Dry Very dry Thirst Absent Present Can’t drink Pinc retracts immediately At home Pinc retracts slowly Pinc retracts very slowly IV General appearance Skin elasticity Treatment ORS Treatment of diarrhea • Protective factors – Human milk: IgA, lactoferrin, leucocytes, antiviral factors, bifidobacteries – Gastric acid – Secretory IgA – Intestinal motility Zinc for diarrhea • Twenty four trials , 9128 children – Zinc is clearly of benefit in children aged six months or more. – Children aged less than six months showed no benefit with zinc. – Vomiting was more common in zinc-treated children with acute diarrhoea • Lazzerini M, Ronfani L. Oral zinc supplementation for treating diarrhea in children. Cochrane Database of Systematic Reviews 2012 Treatment of acute gastroenteritis • Rehydration – ORT > 90 % – IV < 10 % • Continue with unrestricted oral feeding • Antibiotic when necessary (age<3-6 months, dysenteria, cholera..) • Do not use antidiarrheal agents WHO-ORS • Should contain carbohydrate (glucose) and sodium (glucose/sodium: between 1/1 and 2/1) – Glucose: 74-111 mmol/L (rice-flour: 50 g/L) – Sodium • Rehydration: 60-90 mmol/L • Maintenance: 40-60 mmol/L • Osmolarity < 290 mOsm/L • Potassium: 20 mmol/L • Bicarbonate: 30 mmol/L (or citrate: 10 mmol/L) Composition of the ORS recommended by WHO NaCl g/L 3.5 KCl 1.5 Na K Cl Mmol/L 90 20 80 Citrate (Bicarbonate) 2.9 (2.5) Citrate (Bicarbonate) 10 30 Glucose (Rice-flour) 20 (50) Glucose 110 Electrolyte losses in diarrheal disease (mmol/L) Normal stools Cholera Adult Child Enteritis Child ORS Na K Cl HCO3 5 10-12 2-3 3 140 101 13 27 104 92 44 32 56 90 25 20 55 80 14 30 Glucose 111 Comparison of some fluids used for rehydration Fluid Cola Apple juice Chicken soup WHO-ORS Pedialyte Rehydralyte Osmosal CHO mmol/L Na mmol/L CHO/Na K mmol/L Base mmol/L Osmolarity mOsm/L 700 690 0 111 140 140 144 2 3 250 90 45 75 60 350 230 0 1.2 3.1 1.9 2.4 0.1 32 8.2 20 20 20 20 13 0 0 10 10 10 10 750 730 500 311 250 310 304 Treatment of diarrhea at home • Recommended foods – Water, soup (rice), yoghurt, fruit juice… – <6 months: breast-feeding, formula • Recommended amount of fluids – After every watery stools • <2 ages: 50-100 ml • >2 ages: 100-200 ml Treatment of diarrhea at home • To prevent malnutrition – Don’t stop breast feeding or formula feeding – Don’t dilute formula or milk – Older children: give rice cereal, bananas, fruit juices, potatoes, yoghurt, good cooked meat, fish… ORS treatment at home Age Amount of ORS after every watery stools <2 50-100 ml 2-10 100-200 ml >10 Not limited ORS treatment Rehydration Duration Maintenance* Duration Mild Moderate Severe* 50 ml/kg 4-6 hours 100 ml/kg 4-6 hours 100-150 ml/kg 4-6 hours 100 ml/kg 18-20 hours 100 ml/kg 18-20 hours 100 ml/kg 18-20 hours Probiotics for acute gastroenteritis • Lactobacillus GG administered in oral rehydration solution to children with acute diarrhea: a multicenter European trial. Guandalini et al. J Pediatr Gastroenterol Nutr 2000 Rice-based ORS • • • • • • • Cheaper Better taste Hypoosmolar (280 mOsm/L) Prevent vomiting Decrease frequency and duration of diarrhea More nutritive Traditional Contraindication of ORS use • • • • • • • Shock, stupor, coma Severe electrolyte imbalence and dehydration Severe and repeated vomiting Acidosis Oliguria or anuria Abdominal distention, ileus Glucose-galactose malabsorption