* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Lecture 1 Bacterial meningitis
Gastroenteritis wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Hepatitis B wikipedia , lookup
Listeria monocytogenes wikipedia , lookup
West Nile fever wikipedia , lookup
Leptospirosis wikipedia , lookup
Neonatal infection wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Meningococcal disease wikipedia , lookup
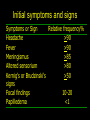
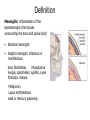
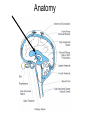
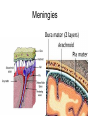
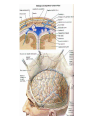
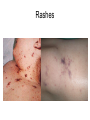
Lecture 1 Bacterial meningitis Dr. Abdelraouf A. Elmanama Islamic University-Gaza Medical Technology Department Lecture outlines • • • • • Introduction Simplified anatomy of the CNS Etiology (causes of bacterial meningitis) Pathophysiology Clinical manifestations Objectives • • • • • Define meningitis Describe prevalence of meningitis Explain pathophysiology Identify clinical manifestations Know the appropriate antibiotic treatment per age group Definition Meningitis: inflammation of the leptomeninges (the tissues surrounding the brain and spinal cord) • Bacterial meningitis • Aseptic meningits: infectious or noninfectious Viral, Rickettsiae, Mycoplasma Fungal, spirochetes: syphilis, Lyme Protozoa: malaria Malignancy Lupus erythematous Lead or mercury poisoning Anatomy Meningies CNS infections • Meningitis Infection of the subarachnoid space with meningeal involvement • Encephalitis Inflammation of brain • Meningoencephalitis Inflammation of brain with meningeal involvement • Brain Abscess Pathogens may be bacterial, TB, viral, fungal, or parasitic CSF • About 85% of CSF produced by the choroid plexus which also controls the constituency of CSF • CSF volume varies by age with a normal adult having a steady state volume of ~150cc Meningitis Bacterial Pathogens • Mechanical Barriers Intact S. pneumoniae (pneumococci) N. meningitidis (meningococci, Groups A,B,C,Y, & W135) H. influenzae (type B or Hib) Immunizations may also affect likely pathogen Special situations B. anthracis • Traumatic alteration or other risk factors S. aureus E. coli or P. aeruginosa May depend on circumstances Meningitis Bacterial Pathogens • Neonatal • Children < 1 month of age • Pathogens acquired from birth canal • E. coli • Group B Streptococci (S. agalactiae) Initial symptoms and signs Symptoms or Sign Relative frequency% Headache >90 Fever >90 Meningismus >85 Altered sensorium >80 Kernig’s or Brudzinski’s >50 signs Focal findings 10-20 Papilledema <1 DESCRIPTION of symptomes • Severe headache .A person with meningitis may describe the headache as the worst one they’ve ever had. • High fever. The infection can cause a high fever (39°C or over) which does not get lower with a tepid bath or fever-reducing medicine. • Stiff neck. Swelling in the meninges (membranes around the spinal cord and brain) causes a stiff neck that makes it extremely painful to move the neck or head. • Nausea and vomiting. Vomiting is common with many illnesses. However, if vomiting happens with the other symptoms listed, it may be caused by meningitis. • Numbness or loss of feeling. Sepsis (also known as blood poisoning) can reduce the amount of blood that gets to a person’s hands and feet, causing numbness, coldness, or loss of feeling. • Light sensitivity. A person with meningitis may find it painful to look at bright lights, and will try to avoid them. • Confusion. Swelling around the brain can make a person confused and seem "out of it.“ • Rash. Purple spots that do not turn white when you press on them are a sign of sepsis (also known as blood poisoning) . • Seizures. Sometimes people with meningitis have seizures similar to the kind that people with epilepsy have Rashes Pathophysiology Nasopharyngeal colonization Local invasion Bacteremia Meningeal invasion Bacterial replication in the subarachnoid space Release of bacterial components (cell wall, LOS) Cerebral microvascular endothelium Macrophages, neutrophils, other CNS Cells Cytokines Increased BBB permeability Cerebral vasculitis Subarachnoid space inflammation Increased CSF outflow resistance Cytotoxic edema Vasogenic edema Hydrocephalus Interstitial edema Cerebral infarction Increased intracranial pressure Decreased cerebral blood flow and loss of cerebrovascular autoregulation Pathophysiology • Meningitis: – Infection of meninges (dura, arachnoid, pia mater). – Caused by: • • • • Bacteria, viruses, fungi, parasites, or toxins. Bacterial ***25% mortality in adults Viral meningitis Fungal meningitis • Bacterial Meningitis: – Infection of the pia mater and arachnoid, the subarachnoid space, the ventricular system, and the CSF. – Infectious agents: • Meningococcus (Neisseria meningitidis) • pneumococcus (streptococcus pneumoniae) – URI---blood borne---CNS entry – Inflammatory response by meninges, CSF, ventricles. – Neutrophils migrate producing exudate that plugs off CSF flow around the brain and spinal cord. Organism Site of entry Neisseria meningitidis Nasopharynx Streptococcus pneumoniae Nasopharynx or direct extension across skull fracture Listeria monocytogenes GI tract, placenta Haemophilus influenzae Nasopharynx Staphylococcus aureus Bacteremia, skin, or foreign body Staphylococcus epidermidis Skin or foreign body • Once in CSF, the absence of antibodies & complement components allows bacterial infection to flourish • Cascade of events: – Cell wall and membrane products of organism disrupt capillary endothelium of CNS (BBB) – Margination and transmigration of PMNs across endothelia in CSF • Release of cytokines and chemokines into the CNS – Inflammation of subarachnoid space • Mortality: 3 to 13% – Rate varies with organism – Higher with gram negative organism • Neurologic Sequelae: 10 % of surviving patients Long-term Neurological Complications Adverse Outcomes at One Year of Age of 12 Infants With Bacterial Meningitis Category of Disability Number Development delay 10 Cerebral palsy 1 Microcephaly 3 Hemiparesis 3 Hearing loss 1 Blindness 2 Seizure disorder 3 Total number of disabilities exceeds the number of infants owing to the presence of multiple disabilities in most subjects Pathogenesis – Majority of cases are hematogenous in origin – Organisms have virulence factors that allow bypassing of normal defenses • Proteases • Polysaccharidases Pathology and Pathogenesis – Sequential steps allow the pathogen into the CSF • • • • • • Nasopharyngeal colonization Nasopharyngeal epithelial cell invasion Bloodstream invasion Bacteremia with intravascular survival Crossing of the BBB and entry into the CSF Survival and replication in the subarachnoid space • Pathology – Hallmark • Exudate in the subarachnoid space • Accumulation of exudate in the dependent areas of the brain • Large numbers of PMN’s • Within 2-3 days inflammation in the walls of the small and medium-sized blood vessels • Blockage of normal CSF pathways and blockage of the normal absorption may lead to obstructive hydrocephalus