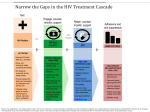
* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download ARV guidelines
Survey
Document related concepts
Pharmacogenomics wikipedia , lookup
Discovery and development of non-nucleoside reverse-transcriptase inhibitors wikipedia , lookup
Discovery and development of integrase inhibitors wikipedia , lookup
Vision therapy wikipedia , lookup
Virtual reality therapy wikipedia , lookup
Transcript
Antiretroviral Therapy DHHS Guidelines Guidelines for the Use of Antiretroviral Agents in Adults and Adolescents II. Background and Principles: Contents Goals of therapy Adherence Risks and benefits of early or delayed therapy Testing viral load and CD4+ T cell Resistance testing Risks and Benefits of Delayed Initiation of Therapy BENEFITS Avoid negative effects on quality of life Avoid drug-related adverse events Delay in development of drug resistance Preserve maximum number of available and future drug options when HIV disease risk is highest RISKS Possible risk of irreversible immune system depletion Possibly greater difficulty in suppressing viral replication Easier to transmit HIV to others Risks and Benefits of Early Therapy BENEFITS Control of viral replication easier to achieve and maintain Delay or prevention of immune system compromise Lower risk of resistance with complete viral suppression Decreased risk of HIV transmission RISKS Drug-related reduction in quality of life Greater cumulative drug-related adverse events Earlier development of drug resistance, if viral suppression is sub optimal Limitation of future antiretroviral 100% 80% 60% 40% CD4 < 200 20% CD4 201-350 HIV-1 RNA (copies/mL) by RT-PCR <1500 1.5K-7K CD4 >350 7K-20K 20K-55K 0% >55,000 Risk of Disease Progression Risk of Progression to an AIDSDefining Illness in 3 Years by Baseline HIV RNA and CD4 Mellors J, et al. Science, 1996; 272:1167-1170. Risk of Progression to an AIDSDefining Illness in 3 Years by Baseline HIV RNA and CD4 Guidelines recommend treatment Guidelines recommend observation 80% 60% 40% CD4 < 200 20% CD4 201-350 <1500 1.5K-7K CD4 >350 7K-20K 20K-55K 0% >55,000 Risk of Disease Progression 100% HIV-1 RNA (copies/mL) Mellors J, et al. by RT-PCR Science, 1996; 272:1167-1170. Testing Viral load CD4+ T cells Resistance testing Decision Making Initiating and Changing Therapy Plasma HIV RNA (viral load) CD4+ T cell count Clinical condition of the patient Measuring Plasma HIV RNA and CD4+ T Cells At the time of diagnosis Every 3-4 months in the untreated patient Immediately prior to initiating therapy 2-8 weeks after initiating therapy Every 3-4 months in patients on therapy As indicated in the opinion of the provider Factors Affecting the Rate of Plasma HIV RNA Decline Baseline CD4+ T cell count Initial viral load Potency of the regimen Adherence to the regimen Prior exposure to antiretroviral agents Resistance Presence or history of opportunistic infections III - Initiation of Therapy III. Initiation of Therapy: Contents Goals of Therapy and Tools to Achieve Them ART in the chronically HIV infected Treatment options Adherence Drug interactions Toxicities Goals of Therapy Eradication of HIV? Not yet… “…in spite of plasma RNA below detection there is evidence of genetic evolution in reservoirs.” Goals of Therapy and Tools To Achieve Goals Maximal and durable suppression of viral load Restoration and/or preservation of immunologic function Improvement of quality of life Reduction of HIVrelated morbidity and mortality Maximize adherence Rational sequencing of therapy Preservation of future treatment options Use of resistance testing in selected clinical settings Before Initiating Therapy... Confirm HIV results Complete H&P CBC, chemistry profile CD4 and T lymphocyte count Plasma HIV RNA measurement Assess “readiness” for rx & adherence Additional tests Before Initiating Therapy Additional Tests VDRL PPD Chest x-ray Hepatitis A,B,C serology Gynecology exam with pap smear Ophthalmology exam (CD4+ T cell <100) Toxoplasma titer CMV serology (if indicated by history) Considerations in Initiating Therapy HIV Asymptomatic Theoretical benefit No proven long-term clinical benefit for CD4 >200 cells/ml3 Expert opinion advises initiation of therapy for CD4 <350 cells/ml3 at any viral load — Consider the viral load when > 350 cells/ml3 CD4+ T cell The “downside” of antiretroviral regimens Considerations in Initiating Therapy HIV Asymptomatic Willingness of patient to begin and the likelihood of adherence Degree of immunodeficiency Plasma HIV RNA Risk of disease progression Potential risks and benefits Indications for ART in the Chronically HIV-Infected Patient TREAT ALL (regardless of viral load) Symptomatic (AIDS, severe symptoms) Asymptomatic, CD4+ <200 cells/mm3 Asymptomatic, CD4+ >200/mm3 but <350 cells/ mm3 * * Treatment should generally be offered, though controversy exists Indications for ART in the Chronically HIV-Infected Patient TREAT Asymptomatic CD4+ >350/mm3 HIV RNA>30,000(bDNA)/55,000(RT-PCR)* * Some experts would recommend initiating therapy, recognizing that the 3 year risk of developing AIDS in untreated patients is >30%. In the absence of very high levels of plasma HIV RNA, some would defer therapy and monitor the CD4+ and level of plasma HIV RNA more frequently. Clinical outcomes data after initiating therapy are lacking. Indications for ART in the Chronically HIV-Infected Patient DEFER TREATMENT Asymptomatic CD4+ cells > 350/mm3 HIV RNA <30,000(bDNA)/55,000(RTPCR)* * Many experts would defer therapy and observe, recognizing that the 3 year risk of developing AIDS in untreated patients is <15%. Indications for ART in the Chronically HIV-Infected Patient Clinical benefit has been demonstrated for patients w/ CD4 <200 mm3. However, most experts would offer therapy at a CD4 threshold <350 mm3. All decisions should be based on prognosis for disease-free survival in the absence of treatment, as determined by the CD4 count and viral load (Table V), the potential benefits and risks of therapy (Table IV), and the willingness of the patient to accept therapy. For further information, see text. WHO HIV Staging System WHO HIV Staging System WHO Guidelines for ARV Therapy in Resource Limited Settings Scaling Up Antiretroviral Therapy In Resource-limited Settings Guidelines For A Public Health Approach- WHO 2002 WHO Guidelines for ARV Therapy in Resource Limited Settings Scaling Up Antiretroviral Therapy In Resource-limited Settings Guidelines For A Public Health Approach- WHO 2002 Current Antiretroviral Medications PI NRTI Abacavir Didanosine Emtricitabine Lamivudine Stavudine Zidovudine Zalcitabine Tenofovir ABC DDI FTC 3TC D4T ZDV DDC TDF Amprenavir Atazamavir Fosamprenavir Indinavir Lopinavir Nelfinavir Ritonavir Saquinavir — soft gel — hard gel APV ATV FPV IDV LPV NFV RTV SQV SGC HGC NNRTI Delavirdine Efavirenz Nevirapine DLV EFV NVP Fusion Inhibitor Enfuvirtide T-20 Antiretroviral Activity: An Historical Perspective HIV RNA change (log10 c/mL) 1987: AZT Monotherapy 1994: Two-Drug Therapy 1997: HAART 0 0 0 -0.5 -0.5 -0.5 -1 -1 -1 -1.5 -1.5 -1.5 -2 -2 -2 -2.5 -2.5 -2.5 -3 24-week response -3 24-week response Fischl, NEJM, 1987 Katzenstein, NEJM, 1996 Eron, NEJM, 1995; Hammer, NEJM, 1996 -3 24-week response Gulick, NEJM, 1997; Cameron, Lancet, 1998 Goal of ARV Therapy: Prolonged Virologic Suppression % With VL BLQ Past Present (Two-Drug Therapy) (Three-Drug Therapy) Future 100 100 100 80 80 80 60 60 60 40 40 40 20 20 20 0 0 0 Weeks MonthsYears Decades Antiretroviral Components in Initial Therapy: NNRTIs ADVANTAGES Less fat maldistribution and dyslipidemia than PI-based regimens PI options preserved for future use DISADVANTAGES Resistance - single mutation Cross resistance among NNRTIs Rash Potential drug interactions (CYP450) Antiretroviral Components in Initial Therapy: PIs ADVANTAGES NNRTI options preserved for future use Longest prospective data DISADVANTAGES Metabolic complications (fat maldistribution, dyslipidemia, insulin resistance) Greater potential for drug interactions (CYP3A4) Antiretroviral Components in Initial Therapy: NRTIs ADVANTAGES DISADVANTAGES Established backbone Lactic acidosis of combination therapy reported with most Limited cross NRTIs resistance within the Triple NRTI regimens class show inferior virologic Minimal drug response compared to interactions efavirenz-based and Triple NRTI regimen of indinavir-based abacavir + lamivudine + regimens zidovudine (or stavudine)* spares PI and NNRTI fortriple future *This is the only NRTI regimen considered acceptable (as an “alternative” regimen) options Initial Treatment: NNRTIBased Regimens #pills /day Preferred Regimen Efavirenz +lamivudine + (zidovudine or tenofovir or stavudine)* *Avoid in pregnant women or women with pregnancy potential 3-5 Initial Treatment: NNRTIBased Regimens #pills /day Alternative Regimens Efavirenz + emtricitabine + (zidovudine or tenofovir or stavudine)* 3-4 Efavirenz 3-5 + (lamivudine or emtricitabine) + didanosine* Nevirapine + (lamivudine or emtricitabine) + (zidovudine or stavudine or didanosine) *Avoid in pregnant women or women with pregnancy potential 4-6 Initial Treatment: PI-Based Regimens #pills /day Preferred Regimen Lopinavir/ritonavir (Kaletra) + lamivudine + (zidovudine or stavudine) 8-10 Initial Treatment: PI-Based #pills Regimens /day Amprenavir/ritonavir + (lamivudine or emtricitabine) + (zidovudine or stavudine) Alternative Regimens Atazanavir + (lamivudine or emtricitabine) + (1) (zidovudine or stavudine) Indinavir + (lamivudine or emtricitabine) + (zidovudine or stavudine) Indinavir/ritonavir + (lamivudine or emtricitabine) + (zidovudine or stavudine) 12-14 4-6 8-10 8-12 Initial Treatment: PI-Based Regimens #pills /day Lopinavir/ritonavir (Kaletra) + emtricitabine + (zidovudine or stavudine) Alternativ e Nelfinavir + (lamivudine or emtricitabine) + Regimens (zidovudine or stavudine) (2) Saquinavir (hard or soft gel capsule)/ritonavir + (lamivudine or emtricitabine) + (zidovudine or stavudine) 8-9 6-14 14-16 Initial Treatment: NRTI-Based Regimens* #pills/ day Alternative Abacavir + lamivudine + to NNRTI- or zidovudine (or stavudine) PI-based regimen 2-6 * To be used only when an NNRTI- or PI-based regimen cannot or should not be used as first line therapy Antiretroviral Medications: Not Recommended in Initial Treatment Modest antiviral activity Delavirdine High pill burden Amprenavir Zidovudine + zalcitabine Saquinavir soft gel capsule Nelfinavir + saquinavir High incidence of toxicities Stavudine + didanosine Ritonavir used as sole PI Antiretroviral Medications: Should not be offered Regimens not recommended: —Monotherapy (except in prevention of perinatal HIV transmission) —Dual NRTI therapy —3-NRTI regimen with abacavir + tenofovir + lamivudine —3-NRTI regimen with didanosine + tenofovir + lamivudine Antiretroviral Medications: Should not be offered Antiretroviral components not recommended: —Stavudine + didanosine —Efavirenz in pregnancy —Saquinavir hard gel capsule (Invirase) as single PI —Stavudine + zidovudine —Zalcitabine + stavudine; zalcitabine + didanosine —Atazanavir + indinavir —Emtricitabine + lamivudine —Amprenavir oral solution in pregnancy, in children <4 years, in renal or hepatic failure, or in patients treated with metronidazole or disulfiram —Hydroxyurea 3TC and ZDV Plus Efavirenz or Indinavir in Naïve Patients: DMP 006 302 HIV-infected patients Open-label study Efavirenz 600 mg QD Indinavir 800 mg q8h Data presented at 48 weeks as % of patients with viral load <50 c/ml EFV % <50 c/mL 100 90 80 70 60 50 40 30 20 10 0 IDV AT ITT EFV+IDV arm omitted Staszewski S, et al. NEJM, 1999;341:1865-1873. Combivir Plus Nelfinavir or Nevirapine in Naïve Patients: COMBINE 142 antiretroviralnaïve patients Open-label study Nelfinavir 1250 mg BID Nevirapine 200 mg BID Data presented at 12 months as % of patients with viral load <20 c/ml NVP arm % <20 c/mL 100 90 80 70 60 50 40 30 20 10 0 NFV arm AT ITT Podzamczer D, et al. 1st IAS, 2001: Abst. 7. ABC/COM is Comparable to IDV/COM in HIV-1 Infected Antiretroviral-Naïve Adults: CNA3014 342 antiretroviralnaïve patients 60 60 Open label study Median baseline viral load: 54,000 c/mL 48 week data presented as % of patients with viral load <50 c/mL (ITT: Missing/Switch = Failure) 50 50 % <50 c/mL 40 30 20 10 0 ABC IDV Vibhagool A, et al. 1st IAS, 2001: Abst. 63. Lopinavir/r vs Nelfinavir in AntiretroviralNaïve Subjects: M98-863 p=0.001 Randomized, double-blind trial Patients nearly ARTnaïve (n=653) d4T/3TC plus either lopinavir/ritonavir BID or nelfinavir TID Data analyzed at 60 weeks, ITT, % of patients with viral load <20 c/ml 70 63 60 % <20 c/mL 51 50 40 30 20 10 0 LPV/RTV NFV Ruane P, et al. 1st IAS, 2001: Abst. 6. Predicting Long-Term Suppression in ARV-Naïve Patients: Evidence-Based Data ITT Analysis of VL <400 c/mL at Week 48 Dupont 006: EFV + ZDV + 3TC Dupont 006: IDV + ZDV + 3TC BMS Start I: IDV + ZDV + 3TC BMS Start I: IDV + d4T + 3TC Atlantic: IDV + d4T + ddI Agouron 542: NFV TID + d4T + 3TC Agouron 542: NFV BID + d4T + 3TC Abbott 863: NFV + d4T + 3TC Abbott 863: LPV/r + d4T + 3TC Percent: 0 10 20 30 40 50 60 70 Note: Randomized comparative trials with 100 subjects/arm; populations’ entry criteria and adherence differ for each trial. 80 The Advantage of Sequencing Drugs To extend the overall long-term effectiveness of the available therapy options Delay the risk of certain side effects uniquely associated with a single class of drugs Anticipates up to 50% of failure rate and preserves future treatment options Adherence Adherence “The achilles heel of HAART” — G. Friedland “Drugs don’t work if people don’t take them.” — C. Everett Koop Adherence The “rule” of thirds… — 1/3 take medication as prescribed — 1/3 are intermittently adherent — 1/3 take little or no medication Correlation Between Optimal Therapeutic Response and Adherence to Protease Inhibitor Therapy Prospective, observational study, n = 81 Subjects’ adherence to PIs assessed electronically using Medication Event Monitoring System (MEMS) — Median follow-up: 6 months (range 3 - 15 months) Baseline demographics — CD4 count ranged from <50 cells/mm3 (14% of subjects) to >500 cells/mm3 (27% of subjects) — HIV RNA ranged from <400 c/mL (30% of subjects) to >100,000 c/mL (11% of subjects) Paterson D, et al. Ann Intern Med. 2000;133:21-30. What Degree of Adherence Is Needed? Patients With Virologic Failure (%) Adherence to a PI-Containing Regimen Correlates With HIV RNA Response at Median 6 Months 100 82.1 80 66.7 71.4 54.6 60 40 21.7 20 0 <70 70-80 80-90 Adherence (%) Paterson. Ann Intern Med 2000;133:21. 90-95 >95 What Happens to Adherence Over Time? Adherence Declines Over Time (Treatment Fatigue) 100% 80 80%-100% 0%-80% 70 Patients (%) 60 50 40 30 20 10 0 1 Month 4 Months Mannerheimer. 13th IAC; 2000; Durban. Abstract 421. 8 Months CPCRA 057, 058 Duration of Antiretroviral Adherence Predicts Biologic Outcomes in Clinical Trials Randomized clinical trials (n = 732 subjects) — Patients had 1 month follow-up — Adherence measured using confidential, self-report, 7-day recall questionnaires Results up to 12 months Adherence HIV RNA (log10 c/mL) % HIV RNA <50 c/mL CD4 (cells/mm3) 0 - 79% 80 - 99% 100% -0.65 -2.27 -2.72 19% 46% 70% 41 175 152 Friedland GH, et al. 1st IAS, 2001: Abst. 33. Virologic Response by Daily Pill Burden Size of symbol is directly proportional to weight of data point in the analysis Bartlett JA, et al. AIDS, 2001; 15:1369-1377. Who Will Be Adherent? Age, race, sex, socioeconomic level educational level, socioeconomic status, and a past history of alcoholism or drug use are not reliable predictors of poor adherence Active drug use or alcoholism, unstable housing, mental illness, and major life crises ARE predictors of poor adherence Adherence – Predicting Success The more severe the symptoms or illness the better adherence Improved adherence if patients believe in efficacy of treatment Adherence – Keep It Simple Once daily therapy - 90% adherence Twice daily therapy - 80% adherence Three or more times daily - 65% adherence Improving Adherence A trusting provider-patient relationship Education Development of treatment plan with patient Social support network Simple regimen Adherence in Special Populations Flexible clinic hours Accessible clinical staff Incentives Bilingual staff Adherence discussion during support groups Individualized adherence programs Others? Adherence Strategies Negotiate a treatment plan Assess patient readiness Educate Reminder devises Social support Others? Poor Adherence – Now What? Increase the intensity of clinical follow up Shorten the follow up interval Recruit additional health team members — Mental health — Chemical dependency counselor — Others Involve family and friends Take a break Simplified Dosing Strategies NRTIs Initially recommended dose (mg) Amended dose (mg) ddI 200 BID 400 QD (pill, suspension) AZT 100 five times a day 300 BID AZT + 3TC AZT 300 BID 3TC 150 BID 1 (300/150) pill BID (Combivir) AZT + 3TC + ABC AZT 300 BID 3TC 150 BID ABC 300 BID 1 (300/150/300) pill BID (Trizivir) IV - Changing Therapy AETC NRC Slide Set Version 1.0, February 2001 IV. Changing Therapy: Contents Considerations Patterns of change Criteria for change Alternatives Monitoring Testing for resistance Treatment interruption Changing Therapy: Considerations Recent clinical history and physical examination Two plasma HIV RNA levels CD4+ T cell count Remaining treatment options Assessment of adherence Patient education Changing Therapy Drug failure or drug toxicity? Medication adherence Pharmacology & drug interactions Testing for antiretroviral drug resistance Changing Therapy Three Different Patients - 1 Individuals who are receiving incompletely suppressive antiretroviral therapy with detectable or undetectable plasma viral load Changing Therapy Three Different Patients - 2 Individuals who have been on potent combination therapy and whose viremia was initially suppressed to undetectable levels but has again become detectable Changing Therapy Three Different Patients - 3 Individuals who have been on potent combination therapy and whose viremia was never suppressed to below detectable limits. Criteria for Changing Therapy Less than a 0.5-0.75 log reduction in plasma HIV RNA by 4 weeks following initiation of therapy, or less than a 1 log reduction by 8 weeks (CIII) Criteria for Changing Therapy Failure of a 1st or 2nd line regimen to suppress plasma HIV RNA to undetectable levels within 4-6 months of initiating therapy (BIII) Repeated detection of virus in plasma after initial suppression to undetectable levels, suggesting the development of resistance (BIII) Criteria for Changing Therapy Any reproducible significant increase, defined as 3-fold or greater, from the nadir of plasma HIV RNA in two or more consecutive viral loads not attributable to intercurrent infection, vaccination, or test methodology except as noted above (BIII) Criteria for Changing Therapy Undetectable viremia in the patient receiving double nucleoside therapy (BIII) Persistently declining CD4+ T cell numbers, as measured on at least two separate occasions (CIII) Clinical deterioration (DIII) Changing Therapy Other Considerations Adherence Results of resistance testing Limited choices Reduction of future choices Change Options Patient With Intolerance to One Drug Substitute for offending drug Use agent in same class Changing other medications unnecessary Change Options Patient on Non-preferred Regimen Viral Load below detection Continue treatment and carefully monitor* or Add drugs to the current regimen (intensify) in limited defined setting *most authorities feel that treatment with regimens not in the strongly recommended category is associated with eventual failure and recommend the latter tactic. Change Options Patient on Recommended Regimen Few specific strategies Theoretical considerations should guide decisions Broad crossresistance among drugs within a class Reinforcement of adherence Guided by resistance testing Option to delay changing therapy Consult an experienced clinician Evidence of better outcomes with using a new class Implications of Treatment Failure at 2 Years EuroSIDA Cohort (n = 8507) Regimen cohort Virologic failure (VL > 500 c/mL) Immune and clinical Clinical failure events 20% 5% 1st HAART 40% 2nd HAART 50% 30% 24% 3rd HAART 67% 40% 25% Mocroft A, et al. Antivir Ther, 2000. Interruption of Antiretroviral Therapy Intolerable side effects Drug interactions First trimester pregnancy Unavailability of drugs Numerous other possible causes Interruption of Antiretroviral Therapy Stop all antiretroviral medications at once V - Special Issues V. Special Issues: Contents Acute HIV infection Advanced HIV infection Adolescents Interruption of therapy Adherence Early Intervention Theory Should be limited to the clinical trial setting Suppress the initial burst of viral replication Decrease the severity of acute disease Alter the viral “set point” Reduce the rate of mutation Reduce risk of viral transmission Preserve immune function Risks and Benefits of Delayed Initiation of Therapy BENEFITS Avoid negative effects on quality of life Avoid drug-related adverse events Delay in development of drug resistance Preserve maximum number of available and future drug options when HIV disease risk is highest RISKS Possible risk of irreversible immune system depletion Possibly greater difficulty in suppressing viral replication Easier to transmit HIV to others Risks and Benefits of Early Therapy BENEFITS Control of viral replication easier to achieve and maintain Delay or prevention of immune system compromise Lower risk of resistance with complete viral suppression Decreased risk of HIV transmission RISKS Drug-related reduction in quality of life Greater cumulative drug-related adverse events Earlier development of drug resistance, if viral suppression is sub optimal Limitation of future antiretroviral The Patient With Advanced Disease Treatment of the Patient With Advanced HIV Disease Offer to all with AIDS and patients with symptomatic HIV infection with thrush or unexplained fever Clinical Issues in the Patient With Advanced HIV Disease Drug toxicity Ability to adhere Drug interactions Laboratory abnormalities Advanced HIV Infection Often complicated drug regimens Wasting and anorexia Co-infection Treatment of the Patient with Advanced HIV Disease Recovery of immune function Immune reconstitution syndromes : Immunologic response to subclinical pathogen, e.g.: MAC or CMV Immune reconstitution syndromes are different from clinical failure Treat new opportunistic infections The HIV Infected Adolescent Timing of infection; perinatal vs. acquired as an adolescent Early intervention The HIV Infected Adolescent Normal adolescent development Drug pharmacology in puberty Dosing based on Tanner stages