* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Title here
Scaling and root planing wikipedia , lookup
Forensic dentistry wikipedia , lookup
Oral cancer wikipedia , lookup
Periodontal disease wikipedia , lookup
Calculus (dental) wikipedia , lookup
Focal infection theory wikipedia , lookup
Tooth decay wikipedia , lookup
Remineralisation of teeth wikipedia , lookup
Dentistry throughout the world wikipedia , lookup
Dental hygienist wikipedia , lookup
Dental emergency wikipedia , lookup
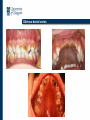
Oral Neglect as part of Child Neglect Alison Cairns Senior Clinical University Teacher/ Honorary Consultant in Paediatric Dentistry Oral Disease • Chronic disease leading to pain and discomfort • Young children with untreated dental caries weigh less than controls • Following treatment of dental caries in young children there is rapid weight gain and improvement in quality of life as well as cognitive development • Weight gain attributed to an improvement in the quality and variety of food the child is able to consume and due to the removal of chronic inflammation known to suppress growth through metabolic pathways Obvious dental caries Prevention of Dental Caries is Basic • Brush twice daily with appropriately fluoridated toothpaste (help and supervision until age 8) • Restrict consumption of sugary food/drink to mealtimes only Dental Caries • Like most other chronic childhood diseases dental caries is predominantly a disease of the poor with the lower socioeconomic groups having the majority share of the problem • Childsmile programmes have been successfully targeting these groups with free brushes/paste, fluoride varnish applications and dental health advice/support, this programme is currently highly successful with a decreasing caries rate in the general child population Dental Neglect • “wilful failure of parent or guardian to seek and follow through with treatment necessary to ensure a level of oral health essential for adequate function and freedom from pain and infection” American Association of Paediatric Dentistry Sept 2010. Dental Neglect • “the persistent failure to meet a child’s basic oral health needs, likely to result in the serious impairment of a child’s oral or general health or development.” British Society of Paediatric Dentistry 2009 BPSD: a policy document on dental neglect on children Recommendations • Gross dental caries in children should be a healthcare priority • Children at risk of abuse or neglect are also at high risk of oral neglect/disease • Dentists should follow local procedures and refer when concerned about possible significant harm • Rigorous follow-up BPSD: a policy document on dental neglect on children Recommendations- Research • More studies to look at the relationship between oral health and child maltreatment • Establish and test diagnostic criteria for dental neglect and thresholds for intervention • Investigate management strategies for untreated dental caries Child Abuse - Caries • • • • 903 children, 5-13years 430 child abuse: 473 controls DMFS -2 dentists logistic regression analysis to control other variables whilst the influence of abuse was evaluated on untreated teeth • Abused children 8 x more likely to have untreated decayed teeth Green at al. Paed Dent 1994 Child Abuse - Caries • 66 children, 56% boys • Children admitted to the Children’s Aid Society of Toronto from 1991-2004 • Age 2-6 yrs (primary dentition) • Untreated caries in- 57% ‘neglected’, 62% physically/sexually abused • General population of 5 yr olds in Toronto with untreated decay = 30% Valencia-Rojas et al 2008 Child Abuse - Caries • • • • 52 witness to violence or subject of violence 65 eating disorder 120 controls Abused children higher plaque index, higher untreated decay, more evidence of gingival bleeding than other 2 groups. Montecchi et al 2009 Comprehensive Medical Assessments GGC • CMA’s were being successfully set up in GGC • Attended a meeting to pitch that a medical assessment cannot be comprehensive if it does not include a comprehensive oral assessment • Answer was “yes”, now all I had to do was persuade oral health directorate management! • Was also lucky enough to get an MSc student on board who undertook the development of the pathway and gathered initial data (paper currently being reviewed by Child Abuse Review- Harris, Welbury and Cairns) Research Question • What is the prevalence of oral disease among children referred for comprehensive oral assessments • Data awaiting publication looks at children seen between 2009- 2011, I can present today information on children seen up until August 2013 Medical team alert dental team re child with a welfare concern Local dental team provide COA on same day as CMA Local or more remote dental team may have to arrange separate appointment for COA Dental notes completed and dental appendix passed onto medical team Treatment needs coordinated with GDP, community or hospital dental services More work required with regard to long term dental follow-up Information we collect • Demographics • dmft/ dmfs scores – D (decay) and quantifies the treatment need – M (missing) which along with f (filled) quantifies past treatment carried out • Plaque and perio scores (oral cleanliness and gum disease) • Erosion, dental defects, soft tissue abnormalities etc • Details of registration with dental services Findings Dec 2009-Aug 2013 • 199 children seen for COA with age range from 4 months to 17 years (mean 6 years) • Children examined over 9 different sites in Greater Glasgow (majority in Bridgeton, Drumchapel and Possilpark) • All resided in areas with SIMD quintiles of 3 or less (83.4% were from SIMD 1) Findings Dec 2009-Aug 2013 • Number of caries free children aged 9 and younger was 32% and for those aged 10 and over was 17%. • Only 28% from the total 199 children were caries free • Much lower than the current national averages (64% for 5 year olds and 62.6% for 12 year olds) Findings Dec 2009-Aug 2013 • Dmft for children aged 9 and younger was 2.52 while for the older age group (>10) it was 5.0 • Higher than local (1.85 for 5 year olds, 0.89 for 12 year olds) and national (1.52 for 5 year olds, 0.7 for 12 year olds) means • For those >10 years the DMFT was 6 (national mean for 12 year olds =2.4) Findings Dec 2009-Aug 2013 • Proportions of children who have evidence of trauma (7.4%) or hypoplasia (5.4%) was broadly similar to the general population (5 – 40% for trauma, 2.4 - 40.2% for hypoplasia) • Evidence of tooth wear in 25% of children aged 9 years and younger and 18% of those aged 10 years and over • A care pathway for children with a welfare concern in Greater Glasgow and Clyde has been developed but still requires refinement especially when it comes to “closing the loop”. Recommendations • COAs integral to CMAs • Other professionals need to be made aware of the type of input paediatric dentistry can give • COA’s should be carried out by dentists who have had extra training not by general dental practitioners • Role of co-ordinator of COAs needs to be developed and always held by someone with extensive knowledge of both the role of dental practitioners in CP and CP systems Recommendations • Targeted prevention of dental caries should be available for all children referred for CMA • Continue efforts to improve pathways of care for dental treatment for this group as these families often have limited ability to engage (possibility of dental health support workers?) • Follow up of these children needs to be improved through better inter agency working Case Study 1 • 13 year old female • Social worker contacts CPU for early sharing and to request CMA • Child already placed on Child Protection Register due to chronic neglect • Dental concerns Case Study 1-Concerns • • • • • • • • Missed health appointments including dental Concern raised by child’s new GDP 84% school attendance Taking caring role for younger siblings 23 calls to Police from neighbour Home conditions – “very poor cleanliness” Bereavement issues Otherwise well and healthy looking Case 1- key learning points • Missed dental appointments is one concern of many but main concern in this case • New GDP raised concerns that brought child to attention of social worker • Input from health services including dental is essential in assessment of child’s circumstance Case 1- Dental history • Significant previous dental treatment including exposure and bonding of gold chain to unerupted central incisor in 2009 • Missed 3 appts with hospital ortho dept, not seen for 18 months • Letter sent to GDP re this • Then seen again for 4 appts in hospital paed dental dept and ortho dept • “Social issues” noted in casenotes as reason for previous missed appts Case 1-Dental history • Missed further 3 appts in paeds and 1 in ortho • Standard letter sent no further hospital appts • Siblings missed dental GAs Case 1- Key learning points • Social history important as is rigorous follow up • GDPs hold info re family situations that dental hospitals etc do not have information regarding e.g siblings Case 1- social history • Father died while mother acutely ill in hospital • Mother had acute grief reaction but social workers believe other issues • No longer interested in children and cold towards them Case 1- Outcomes • Child and siblings accommodated with foster family • Close contact with social worker to ensure attendance at health appts especially dental Case 2 • Siblings- Female 8 years, male 6 years, female 6 months • Referred for comprehensive oral assessment as part of comprehensive medical assessment Case 2 Both older siblings • obvious ingrained dirt on school uniforms • skin and hair visibly dirty • Smelly • Active dental caries Case 2 • 6 year old- poor oral hygiene • 8 year old- good oral hygiene round anteriors, plaque deposits on posteriors • Very compliant for examination • Father blames children- “they never brush their teeth when I tell them to” • Both registered with GDP Case 2- learning points • Extra oral appearance is important • Children need assistance with toothbrushing until approx 8 years of age Case 2 • 6 month old- clean freshly laundered clothes • Hair and skin appeared clean • 2 lower incisors present and oral hygiene good Case 2- Key Learning Points • It may be not all children in a family who are abused/ neglected Case 2 • Father made aware of dental needs of children and elected to go to own GDP for treatment • Copy of dental report sent to GDP Case 2 • Also telephone call to GDP to check registration • GDP confirmed registration but reports children failed to complete treatment and were irregular attenders (though compliant) • Few weeks later GDP contacts to say children not returned Case 2- Key learning points • Irregular attendance and failure to complete treatment are alerting features (www.cpdt.org.uk) • Dentists hold key information other professionals do not • Information sharing essential- without dental report GDP unaware their patient subject to CMA Case 2- Outcome • Children’s social worker contacted re failure to attend subsequent dental appts • Social worker reports children have been accommodated in different health board and requests permission to share dental report with new GDP Where does Dentistry Sit in a Professional Capacity? GDC statement on child protection and vulnerable adults Friday, May 30, 2008 • The GDC expects all registrants to be aware of the procedures involved in raising concerns about the possible abuse or neglect of children and vulnerable adults. • All dental professionals have a responsibility to raise concerns about the possible abuse or neglect of children or vulnerable adults. It is your responsibility to know who to contact for further advice and how to refer to an appropriate authority (such as your local health trust or board). Final Thoughts… • We have received excellent feedback re the contribution of the COA by the medical team and will work to improve communication and pathway development • We feel encouraged that we have managed to identify and provide treatment for this hard to reach group • Hopefully others will be encouraged to incorporate dental into their CMA’s