* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Food Allergy and Intolerance
Survey
Document related concepts
Transcript
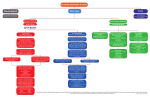
IINH © 2016 Nutrition & Health Coaching Year 1 Health and Disease: Food Allergy and Intolerance Food Allergy and Intolerance Increasing numbers of people are suffering unexplained complaints (treated or untreated), often unaware they may be connected to food(s) eaten on a daily basis. Sensitivities to foods can cause a wide variety of unpleasant and persistent symptoms. Food Allergies and Intolerances* There is confusion in the media, but also among doctors, therapists and people in general, about different types of sensitivity to foods, what mechanisms are involved, the health problems they can cause, how to test for them, and how strict suffers need to be in avoiding problem foods. [*Note: Here, food intolerance means reactions mediated by IgG antibodies. Other types of food insensitivity are covered below.] Food Allergy Classical or ‘true’ food allergy (IgE antibody-‐mediated) is a rapid, inappropriate response of the body’s immune system as it mistakes a normal, safe substance for a foreign invader. Symptoms and signs result from powerful pro-‐inflammatory substances released by immune cells, causing inflammation, swelling, pain, etc. Typical food allergens are fish, peanuts, tree nuts, eggs. [In the EU, 14 foods or ingredients known to cause allergic reactions must be highlighted on food labels] Reading in Moodle under Resources • The 14 ingredients that must be declared as allergens on EU food labels An IgE allergic reaction can be very powerful and start almost at once, or at least within 1-‐2 hours. The skin, airways and/or gut are usually affected. Symptoms can be dramatic and life-‐threatening. An allergy can first emerge at any age, but is then usually a lifelong problem. Fortunately, true food allergy is relatively rare, with only about 2% of the adult population affected. People with true food allergy almost always know what foods or ingredients to avoid. Note: Conventional medicine tends to put all types of food sensitivity (except IgE allergy) under the ‘intolerance’ label. This includes lactose intolerance, as well as sensitivity to histamine, salicylates, additives, nightshades. Most doctors don’t recognise IgG intolerance or the test for IgG antibodies. 1 IINH © 2016 Food Intolerance Reactions to foods that are mediated by IgG antibodies are much more common than food allergies, and becoming more so. They are very different in nature from food allergy, and while not life threatening, they can make people genuinely unwell. Symptoms can take up to 72 hours to appear after eating the culprit food or ingredient, and they tend to be ‘dose dependent’. https://youtu.be/3iKFaXIKUrM -‐ excellent explanation of IgG intolerance from a clinician Intolerance to a food can emerge early or later in life, and may worsen or fade away. Many people suffer for years, however, coping with the symptoms but unable to enjoy optimal health and normal work and home life. Often, food intolerance is ‘hidden’ from sufferers, because they are eating the offending food(s) day after day and their symptoms are habitual. Delayed reaction can make it hard to determine the food responsible. Sufferers often have more than one trigger food. FOOD INTOLERANCE vs FOOD ALLERGY Food Intolerance Food Allergy Reaction delayed up to 72 hours after eating Swift reaction (2 hours or less) Multiple foods can be involved Rarely more than 1 or 2 foods Any organ system can be affected Mainly skin, airways and gut Common (about 30-‐40% of population) Much less common (about 2%) Reaction worsens with dose of food Only trace amounts trigger reactions Often hard to self-‐diagnose (delayed reaction) Usually easy to diagnose (immediate) Mediated and detected by raised IgG Mediated by raised IgE antibodies May clear after avoidance (3-‐6 months) Usually lifelong sensitivity IgG food intolerance reactions When foods are digested their proteins are broken down into smaller fragments (ideally single amino acids) for easy absorption into the body. However, if larger fragments escape into the blood stream without breaking down fully, they may bind to a certain body tissue (e.g. joint cartilage, skin, airways). The immune system may then treat this altered tissue as a foreign invader to be attacked and destroyed, using antibodies called Immunoglobulin G (IgG). This type of autoimmune reaction can occur in any organ or tissue of the body, and lead to a wide range of symptoms. A range of autoimmune diseases can and do result from reactions to habitual foods, but this possibility is almost completely ignored in conventional medicine. Symptoms of Food Intolerance According to Food Intolerance Awareness (www.foodintoleranceawareness.org), common symptoms or disorders that may be caused by food intolerance include: Abdominal pains Lethargy Aches and pains M.E. Arthritis, specially RA Migraine Asthma Nausea 2 IINH © 2016 Bloating Rashes Chronic Fatigue Syndrome Restless Leg Syndrome Constipation Rhinitis Diarrhoea Sinusitis Eczema Skin problems Fatigue Stomach cramps Fibromyalgia Tension Fluid retention Urticaria Headaches Weight loss IBS Wheezing Testing for Food Intolerance Skin-‐prick tests. These are used in hospitals etc and are good for detecting some non-‐ food allergens, e.g. hay fever due to pollen, animal dander. They are increasingly regarded as unreliable (false negative) for detecting food intolerances. IgG blood tests. There are simple DIY blood test kits available to identify food intolerances. They can be very useful in helping people ‘unmask’ hidden food intolerances. Most IgG blood tests use the ELISA (enzyme-‐linked immunosorbent assay) technology (e.g. Fitzwilliam Test, Yorktest, Lorisan) for detecting IgG antibodies produced against the food. A 2012 study found that eliminating trigger foods based on IgG food intolerance test results led to reductions in weight, body mass index, waist and hip circumference, and improvements in all indicators of quality of life that were measured: physical and emotional wellbeing, mental health, social life, pain levels and vitality. *Lewis J et al, 2012: Eliminating Immunologically-‐Reactive Foods from the Diet and its Effect on Body Composition and Quality of Life in Overweight Persons. Journal Obesity & Weight loss Therapy 2:1 Kinesiology and Vega (bioenergy) tests. Again, results can vary (false positives and negatives), but the experience of the practitioner is important. There is no real scientific evidence that they work – but when used by an experienced practitioner they can be useful to point people in the right direction. Unreliability of test results IgG blood tests are useful, but none of the different brands gives completely reliable results (false positives and negatives are common). Also, if a problem food has not been consumed for weeks or more, all antibodies may have disappeared from the system leading to a false negative result. More comprehensive tests (e.g. Cyrex) are available and constantly being improved. They use or combine different detection approaches and may cover a wider range of sensitivities to foods. 3 IINH © 2016 Other problems in detecting a food intolerance Delayed reaction As symptoms/signs can appear up to 2-‐3 days or more after the offending food is eaten, it can be difficult to pinpoint the culprit food or ingredient. [A food diary can be very helpful here] Hidden in broad daylight! When the offending food is eaten every day, symptoms may be more or less ongoing, and thus hard to connect to a particular food, or even to one’s diet at all. Dose dependent A small portion of food can sometimes be eaten with no obvious effect. This confuses people who assume an all-‐or-‐nothing reaction, as with true allergy. But everyone has their own tolerance level – and even this can change due to e.g. stress, pregnancy, stage of menstrual cycle and so on. Stress A common confounding factor is that your ability to tolerate a certain food can fluctuate because of your current condition (stress burden, pre-‐period, tiredness, nutritional status etc). So you might feel bad after eating a certain food when tired and stressed out, but then a week later you might have no reaction to the same food. Some people find certain foods (e.g. gluten, dairy) hard to digest at the best of times, but are OK with modest amounts when their health condition is good. However, when stress weakens the digestion, symptoms appear. The person then assumes a food intolerance and asks the doctor for tests. The standard skin prick test fails to detect a problem so the doctor says there is no food intolerance. The patient remains confused and might look elsewhere for help. 4