* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Personal-Psychopath-treatment
Major depressive disorder wikipedia , lookup
Narcissistic personality disorder wikipedia , lookup
Generalized anxiety disorder wikipedia , lookup
Child psychopathology wikipedia , lookup
Psychedelic therapy wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
Emergency psychiatry wikipedia , lookup
Autism therapies wikipedia , lookup
Behavioral theories of depression wikipedia , lookup
Antipsychotic wikipedia , lookup
History of psychiatric institutions wikipedia , lookup
History of psychiatry wikipedia , lookup
Substance dependence wikipedia , lookup
Moral treatment wikipedia , lookup
History of mental disorders wikipedia , lookup
Controversy surrounding psychiatry wikipedia , lookup
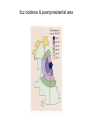
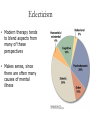
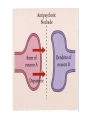
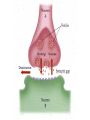
Personality Stability vs. Situation? Personality • Traits vs. States vs. Types • 18,000 personality terms to 32 traits to• Big five: – Extraversion (outgoing, sociable, positive) – Neuroticism (prone to negative emotions) – Conscientiousness (organized, efficient, disciplined) – Openness to experience (non-conventional, curious) – Agreeableness (trusting & easygoing with others) 40 to 60% heritable Situationism • Low correlations across situations – Strong vs. weak situations – But-brain differences and heritability • • • • • Introverts more sensitive to external stimuli More reactive central nervous system Low pain tolerance Underactive Nor-epi system Sensation seeking extraverts Heritability: Big five correlations • Identical twins vs. fraternal twins : Identical • Reared together- .51 • Reared apart.50 Fraternal .23 .21 Personality Theories • Psychoanalytic – Childhood experience, ucs influence, dynamics, conflict, defenses, development and identification • Humanistic – Focus on self & self-actualization, existential approach, flow & happiness • Social-Cognitive Theory – Beliefs, thoughts & personal constructs, often acquired from social interactions & imitation shape behavior • Behavioral Theory – Learning history, self-perception theory, self-control Disorders Who Gets What? Defining Abnormality • Medical approach • Statistical approach • Functional approach These reflect two basic views of disorders --brain based --behavior/experience/situation based The “two worlds” of psychiatry DSM-IV • • • • • • Axis 1: Syndromes (Scz, Depress, etc.) Axis 2: Retardation & Personality Disorders Axis 3: General Medical Condition Axis 4: Social/Environmental Problems Axis 5: Global Assessment & Coping Older classification (primarily of Axis 1 & 2) dichotomized: Neuroses & Psychoses • Mood (Dep. Bipolar) vs. Thought (Scz) Disrdr • Now replaced by highly elaborated DSM-V Three Broad Types/Dimensions • Personality (Psychopathy…..) • Mood (Depression, Bipolar) • Thought (Scz. Delusions, Hallucinations) SCZ Manifestations/Symptoms Positive symptoms: -- Hallucinations – delusions – Disorganized or strange behavior & speech • Negative symptoms: – Flat affect & other behavior – Catatonia – Withdrawel from others Prevalence of Neurotic Disorders by Age Hollingshead & Redlech New Haven Study, 1958 Prevalence of Neurosis by Age & Social Class Prevalence of Psychosis by Age & Gender Treatment Duration & Social Class Psychosis: Age and Social Class Heritability of Psychosis: Schizophrenia Scz incidence & poverty/residential area Some Interim Conclusions • Psychoses (focus on SCZ) is a disorder of heredity and/or prenatal environment • But it’s also a disorder of poverty (and that may be bidirectional)! • Another view of prevalence and recent dramatic changes in prevalence Deinstitutionalization Prevalence • Schizophrenia: approx. 1% • Bipolar Disorder: approx. 1% • Depression: approx. M 13% F 21% Basic Models of Disorder Stress: Functional Disorder -Cognitive & Social Origins Illness: Medical/Biological – Brain-based (synaptic & neural network/connectivity) Mixed Model: VulnerabilityStress Szasz: Radical Anti-medical Approach Treatment Overview • Brief History • Psychological Treatments • Biomedical Treatments • Client-Therapist Relationship • Is Treatment Effective? History • Earliest history – Mental illness believed to be caused by evil spirits. Hippocrates began to dismantle this. – Treatments were harsh, ineffective • Drill holes in skulls to create exits for spirits • Make the body horribly uncomfortable for the spirits • Purge demons through inducing vomiting History • Middle Ages – Mental illness viewed more like a disease, but not treated well! – Mental institutions were created • Purpose: confine “madmen” • Included other social “undesirables” • Inhumane treatment (shackles and chains) Beginning of Reform • Early to Mid 1800s – Philippe Pinel put in charge of Paris’ hospital system • Removed shackles and chains • Patients allowed to exercise, venture outside Beginning of Reform • Dorthea Dix – Fought for humane treatment of patients in U.S. • 19th century – Freud’s “talking cure” (Charcot & hypnosis) Psychological Treatment Overview • Treatment involves addressing three major components of the illness: – Biological – Psychological – Social • Something to keep in mind: – These three major components are not necessarily black-and-white/separable Who provides treatment? • Clinical psychologists • Psychologists • Neurologists • Psychiatric Nurses • Marriage and Family Counselors • Social workers • School counselors • Clergy Who seeks treatment? • People with mental illness, hoping to relieve pain and dysfunction • People looking for assistance in recovering from grief, anxiety, confusion, relationship issues and other life challenges…tilted toward – – – – Women European Americans Financially well off People with Health Insurance (which increasingly controls things)! Psychological Treatments • Focused on changing the way the patient thinks and behaves • Involves discussion, instruction, training, relationship analysis • Over 500 different forms of such treatment – – – – Psychodynamic Humanistic Behavioral Cognitive Psychodynamic Approaches • Illness result of unconscious conflicts developed early in childhood with impact later • Defense mechanisms shield from the inner conflict – This can lead to symptoms of mental illness • Treatment: Uncovering unconscious desires and conflicts, and resolving them – Integrate thoughts and memories coherently Psychodynamic Approaches • “Working through” the conflict – Transference • Used as a therapeutic tool • In order to be effective, therapist must remain neutral Humanistic Approaches • Based off of Freud’s “talking cure” • However, less focused on basic drives • Instead, focus on decisions & creating meaning • Clients need to take responsibility for their lives and actions, and live in the “here and now” • “Tomorrow is the 1st day of the rest of your life” Humanistic Approaches • Client-Centered Therapy (Carl Rogers) – Focuses on achieving self-acceptance – Does not pass judgment, or provide instruction – Aim is to create an environment in which the client feels understood and valued -Requires & elicits a capable client Humanistic Approach • Creating the therapeutic environment – Genuineness- sharing authentic reactions – Unconditional positive regard • Non-judgmental, accepting – Empathic Understanding- putting oneself in the patients’ shoes Behavioral Approaches • Reaction to Freud’s psychoanalysis • Viewed Freud’s approach as too unscientific • Treatment directed at reducing or eliminating problematic behaviors (because behavior is all there is!) • Institutional control mechanism (humane?) • Approach involves replacing old habits with more effective or adaptive behaviors – Classical conditioning, operant conditioning, modeling Behavioral Approaches Classical Conditioning Techniques • Treatment of Phobias – Extinguish the association between the neutral stimulus and the fearful stimulus – Exposure Therapy • Train clients in deep muscle relaxation, pair relaxation with the fearful stimulus • Create a hierarchy of progressively more frightening stimuli • Systematic desensitization: gradual exposure to the real phobic stimulus Systematic Desensitization Behavioral Approaches Operant Conditioning Techniques • Token economies – Earn tokens for positive behaviors, which can be exchanged for prizes – Shaping • Contingency Management – Strict consequences for certain behaviors • Successful for shaping communicative behavior in children with autism (Lovaas) • Modeling Techniques – Therapist perceived as role model Cognitive-Behavioral Approaches • Rational Emotive Behavioral Therapy (Albert Ellis) • People typically think that an event causes them to behave a certain way – But…beliefs matter – Focused therapy on changing beliefs • Teacher-like Cognitive Therapy • Aaron Beck • Focused on changing dysfunctional thought • Cognitive Restructuring – Challenge a person’s unhealthy beliefs or interpretations – Used persuasion and confrontation – Brief, problem-focused • Initially treated depression Cognitive-Behavioral Therapy • Followers of Ellis and Beck blended the two therapies to form CBT • Focus on addressing problems the patient wishes to solve • Intimate relationship between behavior and thought (self perception theory!) • Often clients are assigned homework – Practice new ways skills or thought techniques Eclecticism • Modern therapy tends to blend aspects from many of these perspectives • Makes sense, since there are often many causes of mental illness Client-Therapist Relationship • Therapeutic Alliance – Support • Trust • Hope • Understanding Group Therapies • • Often groups are chosen because they share similar problems (e.g., Alcoholics Anonymous) Focus on the shared problems, less on the individuals’ emotions • Advantages – Social support – Share advice, information – Observe other peoples’ successes – Realize that not alone, others share similar problems – Economic advantage Couple and Family Therapy • Views the family or relationship as a complex system – One person’s negative behavior or cognitions may reflect a larger issue for the entire family or relationship • Can be extended to • treating children who have little control (work with family to change situation/mileau) Biomedical Treatments The Early Gruesome Years • Trephination – Allowed “evil spirits” to escape the skull • Hot or Cold Baths • Spinning Biomedical Treatments Psychosurgery • Prefrontal Lobotomy – Sever connections between thalamus and frontal lobes – Disrupted higher cognitive functions • Modern techniques are more precise and used as a last resort treatment Electroconvulsive Therapy (ECT) • Brief electrical current passed through the brain causing a convulsive seizure • Originally developed to treat schizophrenia • Very effective for treating severe depression (70-90% effective) • Memory impairment • Mechanisms are not known Different Therapies for Different Conditions (& Sometimes a Mix) • Medical: Brain targeted drug interventions examples: --SCZ: Dopamine receptor blockers (the better the block the more effective it is) --Other neurotransmitters involved as well --Depression: ex. Norepinephrine uptake or release+, Serotonin release+, & a host of other neurotransmitter controls involved -- Electro-convulsive shock therapy! Pharmacological Treatments • Psychotropic drugs – Not only helped treat patients, but also further understanding of the illness Pharmacological Treatments • Antipsychotics – Treat positive symptoms of schizophrenia – Not effective for treating the negative symptoms – Most common are Thorazine, Haldol and Stelazine • Block dopamine receptors in particular brain pathways • Atypical Antipsychotics – Treat negative symptoms of schizophrenia, too – Risperdal, Clozaril, Seroquel Antipsychotics and Deinstitutionalization • Movement in the 1950s shortly after development of the first antipsychotics – Aimed to provide less expensive mental health care at local community centers instead of institutions • Pros – Fewer people spending their lives in institutions – Shorter stays – Thomas Szasz argument • Downside – Lack of appropriate care in community settings – Lack of integration into the community (support services, employment) – Many mentally ill are now homeless, or in jail The next slides • The next six slides are for informational purposes to show the variety and nature of particular psycho-pharmacological approaches but should not be memorized! Antidepressants • Monoamine Oxidase Inhibitors (MAOIs) – Nardil • Tricyclic antidepressants – Tofranil • Increase serotonin and norephinephrine for synaptic transmission • Both very effective (significant improvement in 65% of patients) – Many negative side effects Antidepressants • Selective Serotonin Reuptake Inhibitors (SSRIs) – Prozac, Zoloft, Paxil, Celexa, Lexapro – Minimally effect dopamine and norepinephrine, and maximally effect serotonin • Reduced side effects – Most commonly prescribed • Atypical Antidepressants – Effect serotonin, norepinephrine and dopamine in various ways • Wellbutrin (fewer side effects) Antidepressants • Downside – Takes a while before effective (a month) – Trial-and-error – Side effects • Weight gain, nausea, diarrhea, insomnia, reduced sexual desire or response Mood Stabilizers • Treat symptoms of bipolar disorder • Lithium carbonate – Treats manic episodes as well as depressive episodes – Side Effects • Weight gain, sedation, dry mouth, tremors – Adherence to medication • Often patients do not wish to treat mania, only depression – Lethal at high doses – Effective for 60 – 70% of patients Anxiolytic Medications • Treat anxiety disorders • Increase neurotransmission of GABA • Beta Blockers • Benzodiazepines • Tricyclic Antidepressants and SSRIs Anxiolytic Medications • Beta Blockers – Controls autonomic arousal • Benzodiazepines – Valium, Xanax, Klonopin – Short term treatments – Highly addictive – Interact dangerously with alcohol – New drugs are being developed to reduce these negative side effects – Rebound effect Medication: Costs and Benefits • Can be highly effective • Only treats and controls the symptoms – Relapse • Requires trial-and-error for correct drug and correct dosage • Side effects – Reduce adherence to medication • Overprescription Outcomes: Improvement with Drugs vs. Placebos Emerging Biomedical Treatments • Repetitive TMS – Areas of the brain stimulated with magnetic coil for 20-30 minutes over several weeks – Effective for medicationresistant depression – No cognitive side effects • Deep Brain Stimulation – Electrodes implanted in brain - Future: increased ability to interface with brain sub-areas via many pathways. Combined Treatments • Most therapists use a combination of treatments – Drug treatments for short-term effects – Therapy for long-term effects Evaluating the Efficacy of Treatments • Randomized Clinical Trial (RCT) – Treatment group – Placebo group – Random assignment – Symptoms and severity similar across participants – Follow participants over several months Is therapy effective? • A meta-analysis found that 80% of patients who received treatment fared better than those without Are all Therapies Equally Effective? Who provides the most effective psychological treatment? • Number of years of practice? – Not necessarily • Professional credentials? – No • The rapport between therapist and client seems to be strongest predictor – Respect, trust, comfort Who is most likely to benefit from treatment? • Strong alliance with therapist • Motivated • Optimistic • More effective with more therapy Are All Treatments Equally Effective? • A depression meta-analysis shows… – Drug treatment alone 55% effective – Therapy alone 52% effective – Drug AND therapy 85% effective! (New England Journal of Medicine, 2000) Are all Treatments Equally Effective? • Treatment more effective than no treatment • Combining treatments appears most beneficial • Some therapies seem particularly effective for specific disorders – Exposure therapy phobias Moral of the Story • Treatment is effective! • Modern treatments are much more effective and humane than past treatments • The relationship between therapist and client really matters! Recent Reconceptualization • Some people are able to cognitively overcome even serious levels of disorders – Available to psychotherapy – Find meaning in some symptoms – Able to live normally or quasi-normally – Example in Nash film and in today’s reading If you feel you need help… • Seek it! Ask for advice, or set up an appointment with a counselor. It’s not a weakness. • Make sure the therapist is a good match for you! • Remember it can take time and you may face some setbacks, but also… • Remember treatment is effective! Most people improve! Overview • The “Two Worlds” of psychiatry approach is flawed. • The brain is the source of behavior and thus a possible route of change via medical intervention, but…. • Behavior and experience can modify the brain, thus psychotherapy, while targeting behavior, also “tunes the engine” by acting on the brain.