* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Introduction
Survey
Document related concepts
Transcript
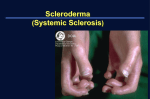
Petra England Case Study Introduction Scleroderma is a rare, autoimmune connective tissue disorder of unknown aetiology. It can have variable clinical manifestations but is mostly characterized by symmetrical thickening and hardening of the skin. The pathogenic pathways of scleroderma are only partially known, but the main causation of tissue thickening is abnormal collagen deposition which can result in eventual fibrosis in the skin as well as internal organs. (Rosenkranz, M, et al. 2006) Scleroderma can be divided into two main subgroups: systemic and localized. The systemic form, also known as systemic sclerosis, involves diffuse skin involvement associated with fibrotic changes in internal organs. Although systemic sclerosis is rare in children, with an incidence rate of approximately 0.27 per million children per year, (Herrick AL, Ennis H, Bhushan M, et al. 2010) it is known to be one of the most severe rheumatic conditions in pediatric practice. (Panda, S, 2010) Diagnosis of systemic sclerosis can be quite delayed from the time of first presenting symptom. A retrospective study (Hawley, DP, Baildam, EM, Amin, TS, et al. 2012) on 89 patients with systemic sclerosis, including 16 with juvenile systemic sclerosis, revealed that the median time from the first symptom to diagnosis was 7 months, with a range of 2-50 months. Raynaud's phenomenon is the first sign of the disease in 70% of the patients, and in 10% it is complicated by peripheral ulceration. Proximal skin hardening is the second most frequent symptom, being present in 40% of cases. (Panda, S, 2010) Case presentation T is an 18 year old male who has always led a very active lifestyle. He is currently 179cm tall and 61kg, giving a BMI of 19.04. In 2010, at age 13, his parents noted that T was experiencing peripheral discolouration in response to temperature changes. T also had been having problems with ulceration and swelling in the ends of his fingers since age 12. T was seen by his local medical team in Tasmania who determined that he had sclerodactyly and facial sclerosis. He was prescribed Sildenafil and prednisolone to manage his condition. T had been seeing his local Rheumatologist who referred him to the Royal Children’s Hospital for further investigation. In early 2012, T moved to QLD and was seen by Dr A, a paediatric rheumatologist. T has an outstanding medical history. He has never had any chest pains or dysphasia. He does not have any history of shortness of breath or modification in his physical activities due to his condition. T also reported that he can play a full soccer game and that he is as fast as his team mates. He has not had any recurrent lower respiratory tract infections and his blood pressure is within normal limits, 125/72. Upon examination in 2012, he presented with significant facial sclerosis and red conjunctivi. Dr A noted that he has very striking sclerosis involving all limbs but particularly noticeable over his upper limbs and trunk. T’s sclerodactyly is still Petra England Case Study significant but his ulceration had been healing well with no major infarction or gangrene. Systemic examination of the heart, lungs and abdomen was within normal limits clinically. A recent blood test revealed very high amounts of Antinuclear Antibody (ANA), indicating systemic involvement of the scleroderma. The impression at this point was that T has systemic sclerosis and needs further investigation. Tests Requested 1. High resolution CT (HRCT) scan of the chest to investigate pulmonary fibrosis 2. Assessment of respiratory status in relation to his current condition, including Spirometry, DLCO, and Lung Volumes 3. Cardiac investigations, including echocardiogram and ECG to check normality and pulmonary hypertension 4. Baseline connective tissue disease screen, including immune markers 5. Bone densitometry to assess osteopenia or osteoporosis in relation to prolonged steroid use Initial Test Results Table 1: T’s Test Results upon presenting to the Royal Children’s Hospital Test Summary of Results (2012) HRCT Normal and clear windows, no fibrosis seen Complex Lung Function Moderate Restrictive Pattern, indicated by: Spirometry: FEV1 65%, FVC 60% and FEV1/FVC 93% (LLN 75%) DLCO: Mild reduction in diffusing capacity at 82%. VA was moderately reduced to 59%, consistent with restriction. DLCO/VA was 132%; this high percentage indicates that there is no true diffusing limitation. Lung Volumes: TLC was reduced to 63%, with RV at 66%, giving a RV/TLC of 122%. All numbers are moderately reduced, consistent with restriction. CPET: TV 51% and VEmax 134%, indicating lack of respiratory reserve. Cardiac Investigation ECG: Sinus Rhythm at 95 bpm; normal ECG Echocardiogram: Normal left and right ventricular size and function. Normal wall thickness. No outflow tract obstruction, no Petra England Case Study aortic or mitral incompetence. Minimal tricuspid incompetence. No ASD, VSD or PDA. No clinical or echocardiographic evidence of pulmonary hypertension. Immune Markers Anti Ribonucleoprotien (RNP) present -> associated with mixed connective tissue disorders and SLE Antiphospholipid syndrome studies and Rheumatoid factor both negative High antinuclear antibody (ANA) with a speckled pattern -> associated with connective tissue disorders and SLE Bone Density Bone mass density is at the lower end of expected range for age Interpretation of test results Examination of his HRCT chest scan revealed clear windows with no evidence of pulmonary fibrosis. A table of standard reference ranges used in interpretation of lung function test is attached as Table 2 in the Appendix. Lung function testing revealed a moderate restricted pattern. (See Fig 1 in appendix) This is evident through a moderately reduced forced expiratory volume in one second (FEV1) of 2.29L (65% predicted) and a moderately reduced forced vital capacity (FVC) of 2.48L (60% predicted). The FEV1/FVC ratio corrects to 93%, with 75% being the lower limit of normal for a male of T’s age and height. (Hibbert, ME, Lannigan, A, Landau, LI, Phelan, PD, 1989) The normality of this ratio, combined with both FEV1 and FVC reduction is indicative of a restrictive disease process. Diffusing Capacity of CO testing showed a mild reduction in diffusing capacity (DLCO) of 82% predicted, along with a moderate reduction in alveolar volume (VA) of 59% predicted. (Cotes, JE, et al, 1993) The DLCO/VA (KCO) ratio corrects diffusing capacity for the available volume for diffusing to occur in. T’s KCO corrects to 132% of predicted, this high percentage indicates that there is no true diffusing limitation, ruling out fibrosis and pulmonary hypertension. Body plethysmography revealed a total lung capacity (TLC) of 3.53L, only 63% predicted, indicating moderate restriction. T’s reserve volume (RV) was 0.84L, 66% of predicted, giving a RV/TLC ratio of 122%. (Hibbert, ME, Lannigan, A, Landau, LI, Phelan, PD, 1989) This ratio may be a little higher than normal due to T’s inability to exhale maximally as his chest wall compliance is compromised due to the sclerosis. A cardiopulmonary exercise test (CPET) was conducted (see Fig 2 in appendix) due to T’s active lifestyle. T was made to exercise maximally on an exercise bike for a Petra England Case Study minimum of 6-8 minutes, while respiratory and cardiac parameters are monitored. T managed to cycle at >85% predicted heart rate for 6 minutes, stopping because of sore feet due to rubbing shoes. His results were mostly normal with an increase in maximum ventilation (VE Max) of 134% predicted and a decrease in Tidal Volume (TV) of 51% predicted. (Hibbert, ME, Lannigan, A, Landau, LI, Phelan, PD, 1989) This indicates a lack of respiratory reserve, consistent with restrictive lung disease. T’s cardiac examination showed normal left and right ventricular size and function, with no septal defects. He had no outflow obstruction and no aortic or mitral incompetence. He has an innocent pulmonary flow murmur with no evidence of hypertension. His ECG was normal with a sinus rhythm of 95bpm. Normal cardiology findings indicate no cardiac involvement with in regards to T’s systemic sclerosis. Pathology tests revealed the presence of Anti Ribonucleoprotien (RNP) and Antinuclear antibodies (ANA) which are consistent findings in patients with systemic sclerosis. These are present in the blood due to the inflammatory pathways associated with sclerosis. T’s bone density was determined to be at the lower limit of normal for a male his age and height, this is suspected to be due to long term use of prednisolone. To combat this, T has also been taking calcium supplements. Dr A confirmed the diagnosis of systemic sclerosis with chest wall restriction and no cardiac involvement. T has had his lung function tested periodically since 2012, with the most recent test being August 2015 (See Fig 3 in appendix). A table of his lung function parameters throughout this period can be seen below, in Graph 1; Petra England Case Study T’s most recent lung function test from July 2015, shows a small decline in FEV1 and FVC, with his total lung capacity remaining stable at 50% of predicted. He has had a slight decline in VA with his DLCO remaining stable, making his KCO much larger on this test date. Management and treatment outcomes There is no single therapy for systemic sclerosis. Initiating the use of a combination of therapeutic strategies early in the disease course has proven to give the maximum beneficial clinical effects. (Rosenkranz, M, et al. 2006) Therapeutic treatments for systemic sclerosis are divided into 3 main groups; antifibrotics, anti-inflammatories, and vasodilators. Antifibrotic agents work against systemic sclerosis by inhibiting the formation of certain molecular collagen crosslinks. They been used to treat systemic sclerosis for several decades, but have questionable efficacy. In some cases, the use of antifibrotics has resulted in skin softening and a reduction in new visceral involvement, but due to a high incidence of adverse events they are not commonly used in children. (Sapadin, AN, Fleischmajer, R, 2002) T was not prescribed any antifibrotic agents. Anti-inflammatory agents are a crucial part in the early management of systemic sclerosis. T has been taking a course of prednisolone, a corticosteroid, since the initial diagnosis of scleroderma. The use of aggressive therapy with glucocorticoids may prevent interstitial fibrosis in the lungs. Once interstitial fibrosis occurs, it is resistant to current treatment modalities and the damage is irreversible. (Pérez Campos, D, Estévez Del Toro, M, et al, 2012) Cyclosporine is occasionally used in combination with glucocorticoids during treatment of juvenile systemic sclerosis. This treatment blocks the pathways for several immune activating and pro-inflammatory cytokines that are elevated in systemic sclerosis. Currently, only small studies have been conducted in regards to the use of cyclosporine in the long term treatment of systemic sclerosis. Larger trials have not been performed due to concern of acute renal crisis in patients. (Rosenkranz, M, et al. 2006) Vasodilators are used to reduce vasospasm and improve peripheral circulation in children who are experiencing Raynaud’s phenomenon and peripheral ulceration. When T first presented with Raynaud’s phenomenon he was prescribed Sildenafil, which is a selective inhibitor of cGMP-specific phosphodiesterase type 5 that provides micro vascular and macro vascular dilation. (Fries, R, Shariat, K, Wilmowsky, H, Böhm, M, 2005) Sildenafil has proven to be an effective, well tolerated treatment in patients with Raynaud’s phenomenon, and is commonly used to restore circulation in patients with peripheral circulatory problems as a complication of systemic sclerosis. The majority of children affected by systemic sclerosis undergo progression of skin and internal organ involvement that often results in morbidity and mortality. Early Petra England Case Study and aggressive treatment using a combination of therapies is crucial to limiting organ damage. Discussion Since his diagnosis in 2010, T has adhered to his treatment consistently. His initial presentation of peripheral discolouration in response to temperature changes was confirmed to be Raynaud’s phenomenon, which is known to occur in >90% of paediatric scleroderma patients. (Rosenkranz, M, et al. 2006) This, in conjunction with peripheral ulceration, swelling, and skin thickening, indicated that a circulatory problem was present. T also experienced the most classic symptom of scleroderma, a type of skin tightening called sclerodactyly, which is defined as localized thickening and tightness of the skin of the fingers or toes. Presence of facial sclerosis further indicated that scleroderma was the underlying disease process. In response to this, he was prescribed Sildenafil, to improve circulation, and Prednisolone, to control the pathophysiological process, and ordered to have further testing into systemic involvement. In 2012, T arrived at the Royal Brisbane Children’s Hospital and testing commenced. His first test, a high resolution chest CT, revealed clear windows and no evidence of interstitial fibrosis. Interstitial fibrosis is a well-recognised complication of systemic sclerosis, with it being the major cause of mortality in children with systemic sclerosis. (Rosenkranz, M, et al. 2006) A HRCT scan may detect early fibrosis in children before it is evident on routine chest radiographs. Currently, T has no known interstitial pulmonary fibrosis. He will have routine chest radiography to monitor any interstitial changes in his lungs. Although systemic sclerosis is a multisystem disease, it is especially known to affect the lungs. Approximately 40% of patients develop moderate to severe restrictive lung disease, with the biggest decline in lung function happening in the first 3-5 years since symptom onset. (Pérez Campos, D, Estévez Del Toro, M, et al, 2012) T had full lung function testing and a cardiopulmonary exercise test (CPET) initially, followed by several serial lung function tests throughout the last few years. Initial spirometry revealed a moderate restricted pattern, with his FVC reduced to 2.48L, which is only 60% of his predicted value. There was no evidence of airway obstruction. The restriction was further confirmed during body plethysomography, where his TLC was 3.53L, only 63% of predicted. The lower limit of normal for TLC for T’s height and age is 4.61L, his value of 3.53L is indicative of moderate restriction. (Hibbert, ME, Lannigan, A, Landau, LI, Phelan, PD, 1989) T also had a small increase in his RV/TLC ratio, this can occur in restriction due to inability to exhale maximally. In systemic sclerosis, the thickening of visceral linings can cause submaximal complete exhalation. T’s restrictive lung disease may be more related to chest wall issues, rather than the lung parenchyma, as his chest CT is normal and clinically he has remained well without respiratory symptoms. Petra England Case Study As T had no interstitial fibrosis, it would be expected that his diffusing capacity would be uncompromised, given that pulmonary hypertension is not present. T’s DLCO was 82% of predicted, although, when we correct this number for VA (KCO), it comes up to 132% of predicted. (Cotes, JE, et al, 1993) His high KCO shows no diffusing limitation in the space he has available for gas exchange. T’s CPET revealed a mostly normal exercise capacity, with a slight increase in VE Max and a decrease in TV. Even though T claims that he does not experience any respiratory symptoms upon maximal exertion, these numbers indicate a lack of respiratory reserve which is common in patients with moderate restriction. T had completely normal cardiology findings, indicating no present cardiac involvement in regards to systemic sclerosis. Pathology tests revealed the presence of multiple proteins and antibodies that are consistently found in patients with systemic sclerosis. These are present in the blood due to the inflammatory pathways associated with sclerosis. T had a bone density at the lower limit of normal due to his constant use of prednisolone. High doses of glucocorticoids are known to have adverse effects on bone due to increasing the excretion of calcium from the body (Ton, FN, Gunawardene, SC, Lee, H, Neer, RM, 2005), as T is taking calcium supplements this should not cause any major issues in his future. T is an interesting case due to his early juvenile onset of scleroderma and his consistent adherence to all prescribed treatments. Due to the rarity of juvenile systemic sclerosis, data regarding prognosis and outcome of children with this disease is limited. Results from a paediatric multicentre survey revealed that cardiopulmonary involvement was the most common cause of death, although a few patients have experienced spontaneous remission. (Foeldvari, I, Zhavania, M, Birdi, N, et al., 2000) With increasing understanding of the pathogenesis of systemic sclerosis, new strategies and therapies to target these pathways of disease progression are being developed. (Rosenkranz, M, et al. 2006) Due to T’s strict adherence to medication, he has managed to avoid the progression of pulmonary fibrosis. Currently, T’s sclerosis appears to be in a stable condition, with no new symptoms arising and no cardiac involvement. The chest wall restriction affecting his lungs has remained relatively stable over the last 3 years and has not affected his ability to participate in physical activities. T will need to be closely monitored throughout his life, early identification of new organ involvement is crucial to ensure proper disease management and to minimise the risk of future complications. The natural course of systemic sclerosis varies from patient to patient but with T’s consistent compliance with medications and check-ups, he will hopefully be able to live a long and happy life. Petra England Case Study References Cotes, JE, et al, 1993, “Standardisation of the Measurement of transfer factor (diffusion capacity). Report working party standardisation of lung function tests, European community for steel and coal. Official statement of European Respiratory Society,” European Resp Journal Supplement, vol. 16, pp. 41-52. Foeldvari, I, Zhavania, M, Birdi, N, et al., 2000, “Favourable outcome in 135 children with juvenile systemic sclerosis: results of a multi-national survey,” Rheumatology, vol. 39, no. 5, pp. 556-559. Fries, R, Shariat, K, Wilmowsky, H, Böhm, M, 2005, “Sildenafil in the Treatment of Raynaud’s Phenomenon Resistant to Vasodilatory Therapy” Circulation, vol. 112, pp. 2980-2985. Hawley, DP, Baildam, EM, Amin, TS, et al. 2012, “Access to care for children and young people diagnosed with localized scleroderma or juvenile SSc in the UK,” Rheumatology (Oxford), vol. 51, pp. 1235–1239. Herrick AL, Ennis H, Bhushan M, et al. 2010, “Incidence of childhood linear scleroderma and systemic sclerosis in the UK and Ireland,” Arthritis Care Res, vol. 62, pp. 213–218. Hibbert, ME, Lannigan, A, Landau, LI, Phelan, PD, 1989, “Lung Function values from a longitudinal study of healthy children and adolescents,” Pediatric Pulmonology, vol. 7, pp.101-109. Panda, S, 2010, “Scleroderma in children: emerging management issues”, Indian Journal Of Dermatology, Venereology And Leprology, vol. 76, no. 4, pp. 348-356. Pérez Campos, D, Estévez Del Toro, M, et al, 2012, “Are high doses of prednisone necessary for treatment of interstitial lung disease in systemic sclerosis?”, Reumatol Clin., vol. 8, no. 2, pp. 58-62. Rosenkranz, M, Agle, L, Efthimiou, P, Lehman, T, 2006, 'Systemic and localized scleroderma in children: current and future treatment options', Paediatric Drugs, vol. 8, no. 2, pp. 85-97. Sapadin, AN, Fleischmajer, R, 2002, “Treatment of Scleroderma,” Arch Dermatol, vol.138, no.1, pp 99-105. Ton, FN, Gunawardene, SC, Lee, H, Neer, RM, 2005, “Effects of low-dose prednisone on bone metabolism,” J Bone Miner Res, vol. 20, no. 3, pp 464470. Petra England Case Study Appendix Table 2: Summary of LLN for reference values used in the Respiratory Laboratory Parameters Reported Hibbert et.al(1989; Table 2) GIRLS BOYS Lower 95% confidence interval (CI) as % of mean FEV1 <82 <82 FEV1/FVC <80 <76 Lower and Upper 95% CI as % of mean TLC <83, >121 <82, >122 RV <63, >159 <62, <162 RV/TLC <17, >38 <16, >36 Cotes (1993) DLCO KCO +/- 25.48 +/- 27.44 <74.52, >125.48 <72.56, >127.44 +/- 23.52 +/- 23.52 <76.48, >123.52 <76.48, >123.52 Petra England Case Study Fig 1: T’s Initial Lung Function Test August 2012 Petra England Case Study Petra England Case Study Fig 2: T’s Cardiopulmonary Exercise test 2012 Petra England Case Study Fig 3: T’s most recent lung function test, August 2015