* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Postpartum Physiology RNSG 2308
Survey
Document related concepts
Transcript
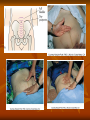
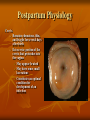
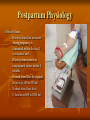
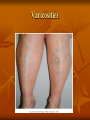
Postpartum Physiology RNSG 2308 Learning Objectives Describe the anatomic and physiologic changes that occur during the postpartum period. Discuss the characteristics of uterine involution and lochial flow, and describe ways to measure them. List expected values for vital signs and blood pressure, deviations from normal findings, and probable causes of the deviations Postpartum Physiology Postpartum period Interval between the birth of the newborn and the return of the reproductive organs to their nonpregnant state. Fourth trimester of pregnancy Also referred to as the puerperium Last on an average of about 6 weeks Postpartum Physiology Reproductive System and Associated Structures Uterus Involution- the return of the uterus to a nonpregnant state after birth Fundus descends 1 to 2 cm every 24 hours Subinvolution- is the failure of the uterus to return to a nonpregnant state Most common causes are retained placenta fragments and infection Postpartum Physiology Contractions Oxytocin- strengthens and coordinates uterine contractions, which compress the blood vessels and thereby promotes hemostasis Postpartum hemostasisis achieved primarily by compression of intramyometrial blood vessels as the uterine muscle contracts, rather than platelet aggregation and clot formation Postpartum Physiology Afterpains Intermittent uterine contractions Maybe intense at times More common in multiparas Frequently occurs with breastfeeding Suckling results in release of oxytocin Oxytocin causes contractions of the lateral ducts in the breast which cause contractions of the uterine muscles A postpartum client asks the nurse about the occurrence of afterpains. The nurse informs the mother that afterpains will be especially noticeable: 1.When ambulating 2.While taking sitz baths 3.During breast-feeding 4.Once the client arrives home and activities are increased Postpartum Physiology Lochia Rubra Last 3 to 4 days Consists of blood, mucus, particles of decidua and trophoblastic debris Bright red Serosa After 3 to 4 days Alba Consists of leukocytes, decidua, epithelial cells, mucus, serum, and bacteria After 10 days-up to 6 weeks Yellow to white A nurse is assessing the lochia discharge on a 1-day postpartum woman. The nurse notes that the lochia is red and has a fleshy odor. The nurse determines that this assessment finding indicates: 1.A normal finding 2.The presence of infection 3.The need for increasing oral fluids 4.The need for increasing ambulating A nurse is providing information about lochia flow to a woman who just delivered a newborn. The nurse tells the woman that the amount of lochia flow: 1.Increases during ambulation 2.Increases during sleep 3.Is scant immediately following delivery 4.Increases in amount on the third postpartum day Postpartum Physiology Cervix Remains edematous, thin, and fragile for several days after birth Ectocervix- portion of the cervix that protrudes into the vagina May appear bruised May have some small lacerations Constitutes an optimal condition for development of an infection Postpartum Physiology Vagina and Perineum Vagina returns to its prepregnancy size by 6 to 10 weeks after childbirth Rugae reappears within in 3 Normal estrogen levels and lubrication return by 6 to 10 weeks Episiotomies heal within 2 to 3 weeks Hemorrhoids usually decrease in size within 6 weeks Postpartum Physiology Endocrine System Placental hormones Human placental lactogen (hPL) decreases to undetectable levels in 24 hours Hcg decreases after birth and remains low until after ovulation Estrogen and progesterone levels decrease markedly after expulsion of the placenta Lowest levels 1 week into the postpartum period Endocrine System Pituitary Hormones and Ovarian Function Elevated serum prolactin levels in breastfeeding women appears to be responsible for suppressing ovulation Ovulation occurs as early as 27 days after birth in nonlactating women Menstruation usually resumes by 12 weeks after birth Mean time of about 70 to 75 days Mean time to ovulation in women who breastfeed is about 6 months Postpartum Physiology Abdomen During the first days after birth, woman’s abdominal muscles protrude and give her a still-pregnant look 6 weeks for the abdominal wall to return almost to it prepregnancy state Return of muscle tone depends on previous tone, proper exercise, and the amount of adipose tissue Abdomen Postpartum Physiology Urinary System Diuresis occurs within 12 hours after delivery Profuse diaphoresis that often occurs, especially at night, for the first 2 to 3 days after childbirth Fluid loss through perspiration and the increased urinary output accounts for weight loss In the immediate postpartum period, the nurse monitors the new mother for which risk related to the urinary system? 1.Diuresis 2.Stress incontinence 3.Urge incontinence 4.Retention Postpartum Physiology Urethra and Bladder Trauma to the urethra and bladder may occur during the birth process Decreased voiding, along with postpartum diuresis, may result in bladder distention Immediately after birth, excessive bleeding can occur if the bladder becomes distended Adequate emptying of the bladder, bladder tone is usually restored 5 to 7 days after childbirth Postpartum Physiology Gastrointestinal System Spontaneous bowel evacuation maybe delayed until 2 to 3 days after childbirth Discomfort may be anticipated due to lacerations, episiotomies, or hemorrhoids and may cause a delay in evacuation Operational vaginal birth and sphincter lacerations may cause postpartum incontinence May resolve in 6 months A postpartum nurse is providing home care instructions to a woman following delivery of a healthy newborn. The nurse tells the mother that she should expect normal bowel elimination to return: 1.1 day postpartum 2.3 days postpartum 3.7 days postpartum 4.Within 2 weeks postpartum Postpartum Physiology Breasts Breastfeeding Mothers Colostrum-before lactation begins and is yellowish in color Breast milk (true)- after lactation begins and is bluish white in color Breast may feel warm and firm Tenderness may persist for about 48 hours after the start of lactation. Nipples are assessed for signs of irritation such as; cracks, blisters, or reddening A nurse is performing a breast assessment on a client who is preparing to breast-feed her newborn. Which breast finding would the nurse determine to be the most effective for breast-feeding? 1.Erectile nipples 2.Inverted nipples 3.Flat nipples 4.Nipples that are level with the skin surface Postpartum Physiology Nonbreastfeeding Mothers Prolactin levels decrease rapidly Colostrum is excreted for the first few days after childbirth On the 3rd or 4th postpartum day, engorgement may occur and the breast become swollen, firm, tender, and warm to touch Engorgement resolves itself spontaneously, and discomfort usually decreases by 24 to 36 hours Breast binder or tight bra, ice packs, and analgesics may be used as comfort measures Postpartum Physiology Blood Volume Blood volume that increases during pregnancy is eliminated within the first 2 weeks after birth Blood volume returns to nonpregnant values within 6 months Normal blood loss for vaginal delivery is 300 to 500 ml Normal blood loss for a C/Section is 500 to 1000 ml Postpartum Physiology Blood Components Hgb and Hct levels drop moderately for 3 to 4 days WBC increase to 20,000 to 25,000 Increased neutrophils and eosinophils and decreased lymphocytes ( shifts to the left) Clotting factors l,ll, V111, lX, decrease to nonpregnant level within a few days Fibrinogen and thromboplastin remain elevated during the first few days after childbirth Postpartum Physiology Neuromuscular System Numbness of thighs, fingers, or hands disappear in several days Back pain usually resolves in a few weeks or months following birth Postpartum headaches may be caused by various conditions, including; postpartum onset preeclampsia, stress, and the leakage of cerebrospinal fluid into the extradural space during an insertion of an epidural Headaches last from 1 to 3 days to several weeks depend on cause and effectiveness of treatment Varicosities Postpartum Physiology Musculoskeletal System Relaxation of the joints and the changes in the mother’s center of gravity in response to the enlarging uterus Joints are completely stabilized by 6 to 8 weeks after birth Mother may notice a permanent increase in her shoe size Postpartum Physiology Integumentary System Chloasma of pregnancy usually disappears at the end of pregnancy Hyperpigmentation of the areolae, and linea nigra may not regress completely after childbirth Spider angiomas (nevi), palmar erythema, and epulis generally regress Profuse diaphoresis Key Points The rapid decrease in estrogen and progesterone levels after expulsion of the placenta is responsible for triggering many of the anatomic and physiologic changes in the puerperium. Within 6 weeks after birth, the physiologic changes induced by pregnancy have reverted to their normal state. Assessing lochia and fundal height is essential to monitor the progress of normal involution and to identify potential problems. Key Points (Cont.) The uterus involutes rapidly after birth and returns to the true pelvis within 2 weeks. The return of ovulation and menses is determined in part by whether the woman breastfeeds her infant. Few alterations in vital signs are seen after birth under normal circumstances Key Points (Cont.) Hypercoagulability, vessel damage, and immobility predispose the woman to venous thromboembolism. Marked diuresis, decreased bladder sensitivity, and overdistention of the bladder can lead to problems with urinary elimination. Pregnancy-induced hypervolemia, combined with several postpartum physiologic changes, allows the woman to tolerate considerable blood loss at birth. Question 1. Which vital sign deviates from the normal reading as a result of puerperal sepsis? a. b. c. d. Temperature Respirations Blood pressure (BP) Pulse