* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Document
Survey
Document related concepts
Transcript
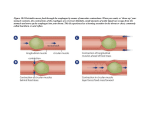
RUNNING HEAD: Concept Care 1 Database: S.M. is a 29 year old male triaged as a level 3 for a sore throat. I took care of S.M. on February 4th, 2015 in the Emergency Department. S.M. is a single, Caucasian male who speaks fluent English. S.M. is currently employed at the mine. He identifies with the Christian faith. S.M. has a girlfriend and their 3 year old daughter in the room with him. Reason for Seeking Hospitalization: Patient claims his throat hurts so bad he can barely swallow. He claims it hurts mostly on the left upper back jaw and throat. Medical Hx- Past and Present medical Dx: Past Dx: 1. Left Shoulder Dislocation: Displacement of the head of the humerus beyond the boundaries of the glenoid fossa. The most common cause is from trauma with the arm in external toation with abduction, causing the head of the humerus to sublux anteriorly; a posterior subluxation may occur from a fall on a n outstretched arm. An inferior dislocation may occur from poor muscle tone as with hemiplegia and from the weight of the arm pulling the humerus downward. Anterior glenohumeral dislocations are common among athletes, especially football players. (Nursing Central Mobile App, Taber’s Medical Dictionary) S/S: A patient with a dislocated shoulder usually has a hollow in place of the normal bulge of the shoulder, as well as a slight depression at the outer end of the clavicle. Glenohumeral range of motion is restricted and such patients often cannot touch their opposite shoulder with the hand of the involved arm. Both shoulders should always be Concept Care Plan 1 2 compared for symmetry. Vital Signs are assessed to provide baseline data. The patient is assessed for pain, and analgesia prescribed and provided as needed. (Nursing Central Mobile App, Taber’s Medical Dictionary) Current Dx: 2. Peritonsillar Abscess: An abscess is a localized collection of pus in any body part, resulting from invasion of a pyogenic bacterium or other pathogen. Staphylococcus aureus, e.g., methicillin-resistant S. aureus (MRSA) is a common cause. The abscess is surrounded by a membrane of variable strength created by macrophages, fibrin, and granulation tissue. Abscesses can disrupt function in adjacent tissues and can be life threatening in some circumstances, e.g., in the lung or within the peritoneal cavity. So, a peritonsillar abscess is an abscess of the tissue around the tonsillar capsule. Needle aspiration of the abscess, with subsequent antibiotic therapy, is an effective treatment in 90% of cases. (Nursing Central Mobile App, Taber’s Medical Dictionary) S/S: The mouth and throat may show a swollen area of inflammation - typically on one side. The uvula may be shoved away from the swollen side of the mouth, lymph glands in the neck may be enlarged and tender, severe sore throat that becomes isolated to one side, painful swallowing, fever and chills, muscle spasm in the muscles of the jaw and neck, ear pain on the same side as the abscess, a muffled voice, often described as a "hot potato" voice (sounds as if you have a mouthful of hot potato when you talk), and difficulty swallowing saliva. (Lubin, J.S., 2014, para.2) My patient exhibited signs of enlarged, tender lymph nodes bilaterally in the neck. He stated he had a very sore throat and that it was even difficult for him to swallow his own spit. His Concept Care Plan 1 3 left tonsil and back, upper jaw are inflamed and reddened. There are significant white patches of pus primarily on the left tonsil and back, upper jaw. Patient had a slightly elevated s Situation temperature at 1348 taken temporally at 99.2 degrees Fahrenheit. Background B Assess what is happening in a short statement Summarize important past assessment data for your patient here. Place lab results and medication on the concept map Patient presents as: S.M. is a 29 year old Caucasian, single male in the ED with a severe sore throat. Patient states he has difficulty swallowing his own saliva and is in pain. He states the pain is located more on his left back, upper jaw and left tonsil. He claims he has had the sore throat for five days prior to coming in for assessment and treatment. He was triaged as a level 3 and was soon swabbed to R/O strep throat. Age: 29 Gender: Male Allergies: Meperidine HCL (From Demerol) Fall Risk: NO, Pt. walks into ED independently with a steady gait. Isolation: Universal precautions A Concept Care Plan 1 4 Use the assessment data to complete your concept map Vital Signs: 11:12: Temp: 97.5, Pulse: 102, Respirations: 16, BP: 126/79, O2: 100. 12:27: Temp: 97.8, Pulse: 88, Respirations: 20, BP: 93/61, O2: 91 (Had to reassess after O2 dropped to 86 suddenly, O2 put on via nasal cannula at 1.5 Liters). After intervention: 12:30: Temp: 97.6, Pulse: 86, Respirations: 18, BP: 93/61, O2: 96 13:20: Temp: 98.0, Pulse: 95, Respirations: 18, BP: 106/59, O2: 94 13:48: Temp: 98.0, Pulse: 95, Respirations: 18, BP: 106/59, O2: 92 13:53: Temp: 99.2, Pulse: 97, Respirations: 18, BP: 104/67, O2: 94 General:. Patient is alert and oriented to person, place, and time. He is sitting back in High Fowlers in bed talking to his daughter and girlfriend. Patient claims he is in pain rated at an 8 on a verbal scale from 0-10. He only asks for pain control at this time and has no other unmet needs. He has blue eyes and brown hair. He has adequate hygiene. The patient is a 6’3 tall male weighing 119.7 kg. He has adequate muscle tone, no atrophy or dystrophy noted. S.M. is capable of ambulating with no problem independently with a steady gait bilaterally. S.M. has adequate hearing as evidenced by the ability to respond to questions being asked in an average volume of my voice. He can communicate effectively, but softly due to his throat pain. His skin color is pink and dry and warm with slightly pale lips. Assessment HEENT: Patient has normocephalic skull that is symmetrical. There were no lumps, bumps, or lesions found on scalp. There were no nits or lice found either. The patient had a symmetrical face overall. He has facial hair full with a beard and mustache. His eyes were almond shaped and were blue with no visible discharge. Ears were symmetrical bilaterally. There was no presence of lesions on either ear. The patient’s tympanic membranes were pearly grey equal bilaterally. There was no visible ear wax buildup. The patient’s nose was symmetrical with no septum deviation. His nares were moist and pink with little black hair. There was no discharge or lesions in her nares. His lips were pale and dry and symmetrical. His mucous membranes in his oral cavity were slightly pale, pink and moist. His throat was inflamed and reddened with substantial white pus patches on his left tonsil and back, upper jaw. His teeth were white and straight and there were no carries. The patient’s neck was supple. Lymph nodes are palpable equally bilaterally in neck and also in the left supraclavicular region. Integumentary: Patient’s skin is warm, dry, and pink. He has multiple tattoos covering most of his upper arms bilaterally and partially on his right forearm. His overall skin condition was excellent with no skin breakdown visible. He had a couple of small yellow/green contusions on left shin about 10 mm in diameter. Patient had a left antecubital IV in place that was intact, no redness, swelling, or drainage seen at the site throughout the shift. His nares show no evidence of irritation or redness. The patient’s fingernails were very clean and trimmed. They were white and pink at the nail beds. His toenails were also very clean and trimmed and were white and pink at the nail beds. Braden Scale Score: Sensory Perception: 4=No impairment. Moisture:4=Rarely Moist. Activity:3=Walks Occasionally. Mobility:3=Slightly Limited. Nutrition:4=Excellent. Friction and Shear:2=Potential Problem. TOTAL SCORE=20. Concept Care Plan 1 5 Respiratory: The patient’s fingernails and toenails were pink. His lips looked slightly pale. His mucous membranes were also pale, pink and moist. His respirations per minute were within normal limits from 16-20 breaths per minute. His chest rose and fell equally bilaterally and his respirations are unlabored. He had no nasal flaring or grunting. His anterior posterior chest diameter was normal at a 1:2 ratio. He had clear, vesicular breath sounds in all lobes in each lung. After morphine and Zofran were administered, about 10 minutes later, the patient’s oxygen saturation dropped from 91% to 86% all of a sudden. Pt. exhibited no other signs of cyanosis except pale lips on the verge of a blue tinged. O2 via nasal cannula was put on 1.5 Liters and the patient’s O2 went back up to 96%. His oxygen saturation showed no other major fluctuation except for this instance and was taken off of the nasal cannula after his oxygen saturation reached 96 and he maintained a stable O2 sat. Pt. was negative for bronchophony and egophony. Patient had no crackles, rhonchi, or wheezing. No history of respiratory disease or illness. Pt has no cough. Pt. has difficulty clearing secretions in mouth due to sore throat and difficulty swallowing due to pain. Pt. spits in cup and sputum is clear with no odor. Cardiovascular: Upon auscultation the client’s heart, I heard regular rate and rhythm and so the client had normal S1 and S2 sounds. There were no murmurs heard. The apical pulse was equal to the patient’s radial pulse. The right and left radial pulses were equally bilaterally, both rated at a 2+. The pedal pulses were equally bilaterally, both rated at a 2+. His carotid pulses were rated at a 2+ equally bilaterally. The capillary refill of the patient’s lower extremities was immediate and the capillary refill of the patient’s upper extremities was also immediate. There was no clubbing of his nails noted. Homan’s sign is negative bilaterally. Patient has no evidence of any pitting and non-pitting edema on either lower extremity, sacrum, or on upper extremities. GI: The patient’s abdomen is round and soft and there is no distention. There were no scars or lesions noted on the patients abdomen. He denies any pain or tenderness upon palpation. Patient states he has some nausea rated at a 5 on a verbal pain scale of 0-10. He states he has no vomiting or diarrhea. Upon auscultation, the patient has normoactive bowel sounds heard within 3 seconds in each of the four quadrants. Patient states he was unable to eat today due to the pain caused from the abscess. Pt. denies any problems with bowel movements and denies any abnormal appearance of stools. GU: The patient did not void while I took care of him, but he denied any problems with voiding. He denied any burning or pain upon urination. He claims his urine hasn’t looked cloudy, bloody, and has not noticed any particles either. No history of any UTI’s or kidney stones. Concept Care Plan 1 6 NEURO: Patient is alert and oriented times three. His pupils were round and reactive bilaterally. They were about 3mm in diameter and constricted and dilated bilaterally when light was shined at them. His eyes accommodated equally bilaterally. He was able to follow penlight with both eyes equal bilaterally in all 6 cardinal directions without any head movement. His hand grips were rated at a 5 equal bilaterally and his foot pushes were rated at a 5 equal bilaterally. The patient was able to swallow, but with trouble due to his pain, but his uvula rose and fell equally. The patient had adequate hearing equal bilaterally. There were no abnormal speech patterns upon communicating with the patient. Patient had a symmetrical smile and was able to stick his tongue out and move it side to side equally bilaterally. Patient was able to shrug shoulders against resistance and move head against resistance. All cranial nerves are intact. PAIN: Patient rates pain as an 8 on a verbal pain scale from 0-10. It is located on the left side of his throat and back, left, upper jaw. Cultural: Pt. is 29 year old Caucasian male whose primary language is English. He identifies with the Christian faith. I was able to communicate well and effectively with the patient and he felt comfortable expressing his concerns with me. I started his left, antecubital peripheral IV and he stated that he was scared of needles and hated getting IVs. He showed a lot of anxiety and fear so I talked him through the process and he seemed to calm down a little bit. Concept Care Plan 1 Evaluate your nursing care and make recommendations Related to the achievement of your desired outcomes. Were they met, or do new goals need to be established? Diagnosis 1 7 Goal: Patient will demonstrate effective coughing and clear breath sounds q 2 hours and will maintain a patent airway throughout my clinical shift. Outcome met? Yes I auscultated the lung sounds on this patient q 2 hours and told him to deep breathe and cough and patient did this effectively and lung sounds were clear in all lobes. I gave the patient a cup since he had difficulty swallowing his own saliva due to the pain and inflammation he was experiencing in his throat. He was able to spit out the saliva so he did not risk aspiration. His airway remained patent and the inflammation was controlled by the anti-inflammatory steroid I administered via IVP over two minutes. Diagnosis 2 Goal: Pt will use the verbal selfreport pain tool on a numerical scale of 0-10 q hour with vitals and report that pain management regimen achieves comfort-function goal without side effects throughout my clinical shift. Outcome met? Yes Initially, I administered 2 mg of Morphine via IVP. The patient stated that he did not feel much relief after the administration of Morphine. Then, Phenol Chloraseptic Throat Spray was self-administered, 2 puffs PRN and patient stated that it “worked better than the morphine” and lowered his pain level from an 8 to a 4. Diagnosis 3 Goal: Client will identify and Outcome met? verbalize symptoms of anxiety whenever they feel it and will YES identify, verbalize, and demonstrate techniques to control anxiety throughout my shift. Concept Care Plan 1 Evaluate your nursing care and make recommendations Related to the achievement of your desired outcomes. Were they met, or do new goals need to be established? 8 The patient displayed signs of anxiety with increased rate and shallow respirations and tachycardia and feeling of faintness because I told him I would have to start an IV on him. He told me he was deathly afraid of needles and that he was scared. He said that he was “freaking out”. I talked him through the procedure and told him to look away while I put the needle in and it calmed him down a little bit as evidenced by lowered respiratory rate and lowered heart rate. Diagnosis 4 My client will be educated about the signs and symptoms of bleeding postoperatively and will maintain warm, dry skin throughout my clinical shift. Outcome Met? NO I was unable to monitor my patient for bleeding because he was admitted to the floor for observation over-night. He was scheduled to get surgery for his abscess the next day. Name/ Classification Indication Adverse Reaction Morphine/Opioid Analgesics Pain rated at an 8, intolerable to patient. Pain location on left side of throat and upper left jaw. Respiratory depression, constipation, hypotension, sedation, dizziness. Phenol Spray/ Chloraseptic Throat Spray/ Analgesic/Oral Anesthetic Pain in throat on left side rated at an 8 after morphine did not touch the pain. Headache, nausea, vomiting Ondansetron/ Anti-emetic Nausea rated at a 5 on a 0-10 verbal scale. Headaches, dizziness, constipation, diarrhea, dry mouth CNS depression, euphoria, hypertension, anorexia, nausea, fragility, adrenal suppression Allergic reactions, Concept Care Plan 1 Methylpredinsolone/Corticosteroids Throat inflammation. Cefazolin/ Anti-infectives Prophylaxis for Medications administered and nurse evaluation 9 of Patient response 2mg IVP Now. Pt. states his pain is still at an 8. He states he doesn’t feel like the morphine helped much. Pt.’s O2 saturation dropped to 86% after administration, pt. was put on O2 via nasal cannula at 1.5 Liters. Pt.’s O2 saturation went back up to 96 within 1 minute and the O2 nasal cannula was discontinued. 2 puffs PRN. Pt. states the chloraseptic spray immediately relieved his pain in his throat and that it “works better than the morphine you gave me.” He rated his pain at a 4 after using the spray. Pt. denies any complaint of nausea after Zofran is administered. Pt. tolerated well with no adverse reactions. Inflammation in throat was still visible. Pt. tolerated well Concept Care Plan 1 Clindamycin/Anti-infectives 10 potential surgery and also to treat the already existing abscess in throat. Prophylaxis for potential surgery and also to treat the already existing abscess in pt.’s throat. diarrhea, nausea, vomiting, rash, pruritis. with no adverse reactions. Diarrhea, nausea, bitter taste, headache, hypotension. Pt. tolerated well with no adverse reactions. XRAYS: CT Neck with Contrast Findings: Asymmetric soft tissue swelling in the left oral tonsil, central low density with this tissue and I suspect this could represent a very early tonsillar abscess, though there may not yet be complete liquidation. Low density area measures 1x1.7cm in max size. Asymmetric effacement of the lower oral and upper hypopharynx. Epiglottis is thin, some lymph nodes in the neck and left supraclavicular region, which are presumably reactive. Impression: Asymmetric soft tissue swelling of the left oral tonsil. I suspect there is a small/evolving, left tonsillar abscess measuring 1x1.7 cm in maximum dimension. ENT consultation might be of additional benefit. Concept Care Plan 1 11 Lab (consider diagnosis) NEUT% LYMPH% Value (high or low) 79.2 HIGH 11.4 LOW WBC EOS% BASO% NEUT# MONO# EOS# Total Bilirubin 14.17 HIGH 0.0 LOW 0.1 LOW 11.21 HIGH 1.28 HIGH 0.00 LOW 2.07 HIGH Group A Strep Screen NEGATIVE Clinical indication Infection Septicemia, malnutrition, pneumonia Inflammatory infection Infections Acute infection Infections Infections Infections Infectious mononucleosis, hepatitis, hypothyroidism Negative for Strep Throat Psychosocial: I experienced a moment with this patient that I found to be interesting and further proves that each patient is an individual and has unique and diverse needs and reactions to interventions. I had to start an IV in this patient and when I entered the room with the IV start kit, I noticed his eyes got wide and he anxiously asked me, “What’s all that stuff for?”. I explained to him that the doctor ordered an IV and that I was going to be the one to do it. He gave me permission to do so, but with a lot of fear. He admitted that he was really scared of needles and his respirations started to increase in rate and became shallow. He closed his eyes and looked away from his left arm which is where I chose to start the IV. He said he started to feel a little dizzy, due to his anxiety. I calmly and slowly talked him through the process as I started his IV and drew blood. This seemed to gradually help reduce his anxiety and once the blood draw was over, he claimed his anxiety was relieved. What I found to be interesting deals with stereotyping. This patient was a very tall, well-built young male with facial hair and tattoos all over his arms. Initially I viewed him as a “tough-guy”, and yet he was not afraid to reveal his fear of needles, which to some could be emasculating. Concept Care Plan 1 Nursing Diagnosis 1 Ineffective Airway Clearance r/t pain in throat AMB difficulty swallowing and spitting into cup. 1)Auscultate breath sounds q2 hours. (Ackley &Ladwig, 2012, Pg.130) 2) Monitor respiratory patterns, including rate, depth, and effort. (Ackley &Ladwig, 2012, Pg.130) 3) Administer Oxygen as ordered. (Ackley &Ladwig, 2012, Pg.130) 4) Position the client to optimize respiration HOB at 30-45 degrees. (Ackley &Ladwig, 2012, Pg.130) Nursing Diagnosis 4 Risk for bleeding r/t surgical intervention for abscess. 1)Watch for signs of bleeding including: bleeding of the gums, blood in sputum, emesis, urine, or stool q 1 hour. (Ackley &Ladwig, 2012, Pg.157) 2)Assess vital signs q 1 hour looking for tachycardia, tachypnea, and hypotension. (Ackley &Ladwig, 2012, Pg.158) 3) Monitor all medications for the potential to increase bleeding such as aspirin and NSAIDS throughout my shift. (Ackley &Ladwig, 2012, Pg.158) 4) Perform admission risk assessment for falls and for signs of bleeding. (Ackley&Ladwig, 2012, pg. 157) Nursing Diagnosis 2 Acute Pain r/t left tonsil abscess AEB rating pain at an 8 and intolerable verbally on a scale from 0-10. 1)I will determine if the client is experiencing pain at the time of the initial interview. If pain is present, conduct and document a comprehensive pain assessment and implement or request orders to implement pain management interventions to achieve a satisfactory level of comfort. (Ackley &Ladwig, 2012, Pg. 577) 2)I will assess pain intensity level in a client using the verbal 0-10 numerical pain rating scale. (Ackley &Ladwig, 2012, Pg. 577) 3)I will assess the client for pain presence routinely with vital signs and after pain med admin. (Ackley &Ladwig, 2012, Pg. 577) 4)I will ask the client to describe prior experiences with pain, effectiveness of pain management interventions, responses to analgesic medications and their side effects on the pt. (Ackley &Ladwig, 2012, Pg. 577) Condition: Peritonsillar Abscess, Left Tonsil and left,back, upper jaw. 12 Nursing Diagnosis 3 Anxiety r/t fear of needles AMB patient stating, “I’m deathly afraid of needles.” 1)Use empathy to encourage the client to interpret the anxiety symptoms as normal throughout my shift during feared procedures. (Ackley &Ladwig, 2012, Pg.138) 2) If irrational thought or frears are present, offer the client accurate information and encourage him to talk about the events contributing to the anxiety throughout my shift. (Ackley &Ladwig, 2012, Pg.138) 3) Explain all activities, procedures, and issues that involve the client throughout my shift. (Ackley &Ladwig, N 2012, Pg.138) 4) Intervene u when possible to remove r sources of anxiety throughout s my shift. (Ackley &Ladwig, i 2012, Pg.138) n g Age: 29 D i a g n o s i s 5 Concept Care Plan 1 13 References Ackley , B.J., Ladwig, G.B. (2014). Nursing Diagnosis Handbook An Evidence-Based Guide to Planning Care. Taber's Medical Dictionary, Nursing Central Mobile APP.