* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download TB Disease
Dirofilaria immitis wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Neonatal infection wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Chagas disease wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Epidemiology of HIV/AIDS wikipedia , lookup
Leptospirosis wikipedia , lookup
Onchocerciasis wikipedia , lookup
Hepatitis B wikipedia , lookup
Hepatitis C wikipedia , lookup
Diagnosis of HIV/AIDS wikipedia , lookup
Schistosomiasis wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Oesophagostomum wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Microbicides for sexually transmitted diseases wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Visceral leishmaniasis wikipedia , lookup
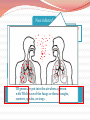
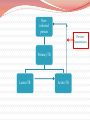
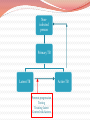
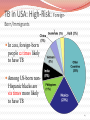
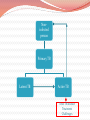
Sarah Al-Obaydi M.B.Ch.B, MPH(c) Fulbright scholar Tuberculosis Tuberculosis (TB) is an infection caused mostly by Mycobacterium tuberculosis. TB is a multisystem disease (affects most organs) TB can also be caused by other Mycobacteria like: M. bovis M. africanum M. microti M. canetti Not all Mycobacteria cause TB e.g., M. avium intercellulare complex M. tuberculosis Tuberculosis (TB): History TB is an ancient disease Historically known by a variety of names, including: Consumption Wasting disease White plague Tuberculosis (TB): History Before TB drugs were available most went to sanatoriums: TB hospitals regimen of bed rest, open air, and sunshine Sanatorium patients resting outside TB patients who could not afford sanatoriums often died at home 4 Non-infected person Transmission by Respiratory droplets Primary TB (usually in Lungs) Healthy individual with good immunity Often Asymptomatic Poor Immunity TB germs are put into the air when a person with the Immunity lungs or throat coughs, Latent TBTB disease ofPoor Active TB sneezes, speaks, or sings Latent TB vs TB Disease Latent TB Infection (LTBI) TB Disease (in the lungs) Inactive, contained tubercle bacilli Active, multiplying tubercle bacilli in the body in the body TST or blood test results usually positive TST or blood test results usually positive Chest x-ray usually normal Chest x-ray usually abnormal Sputum smears and cultures negative Sputum smears and cultures may be positive No symptoms Symptoms such as cough, fever, weight loss Not infectious Often infectious before treatment Not a case of TB A case of TB Progression to TB Disease Risk of developing TB disease is highest in the first 2 years after infection Progression from Latent TB infection to TB disease can be prevented with TB drug (usually one TB drug): TB prophylaxis However, not practiced in many developing countries where TB is endemic Therefore detecting TB infection, early starting TB drugs helps to prevent new cases of TB disease 8 Noninfected person Prevent Transmission Primary TB Latent TB Active TB How to Prevent TB Transmission? Isolate infectious persons Those with Lung TB disease only Treat TB dis. as soon as possible They stop shedding TB bacteria with in a few weeks after starting treatment Noninfected person Primary TB Latent TB Active TB Prevent progression Testing Treating latent Control risk factors Prevention of Latent TB to Active TB progression : Testing high risk groups for Latent TB Treating Latent TB Control risk factors TB in USA: High-Risk: ForeignBorn/Immigrants In 2011, foreign-born people 12 times likely to have TB Among US-born nonHispanic blacks are six times more likely to have TB 14 High-Risk – decreased immunity: HIV infection Diabetes Mellitus Prolonged steroids treatment Substance abuse Recent TB infection: If exposed to TB in the last 2 yrs Noninfected person Primary TB Latent TB Active TB Treat TB disease Treatment Challenges Treatment of TB disease Several drugs for 6 to 9 months. Why? Regimens for treating TB disease have initial phase of 2 months continuation phase of either 4 or 7 months Treatment must contain multiple drugs to which organisms are susceptible Treatment with a single drug can lead to the development of drug-resistant TB Treatment: Different Phases Initial Phase Continuation Phase •8 weeks with 4 drugs (INH, RIF, EMB, Pyrazinamide) • Most bacilli killed during this phase •They don’t spread TB • 4- 7 months with 2 TB drugs only • remaining Bacilli (in reservoirs) are cleared in this phase Challenges to TB treatment and prevention: Relapse: 1. when treatment is not continued for long enough Surviving bacilli may cause TB recurrence Multidrug resistant TB (MDR TB) is TB resistant to at least two of the best anti-TB drugs-INH and Rifampin. 2. Mostly because of poor adherence to treatment regimen How to ensure adherence to treatment? Directly Observed Therapy (DOT) Challenges 3. Drug interactions interfere with treatment In TB and HIV co-infection: many ART drug interact with Rifampin 4. Lack of awareness of TB or HIV status can prevent adequate treatment • How to prevent this? Anyone who is newly diagnosed with HIV or TB should be tested for co-infection. Resurgence of TB Risk of TB disease The risk of developing TB disease 10% each year in people with HIV infection 10% over a lifetime if otherwise healthy Globally: Dual Epidemic Globally TB is a leading cause of death in HIV patients What is the leading cause of death among HIV patients in USA? Hepatitis C Effect of CD4 count on risk of TB among HIV-infected people Incidence of TB (per 100 pyrs) 20 >350 200-350 <200 15 10 5 0 Italy US South Africa Antonucci JAMA 1995;274:143; Markowitz Ann Int Med 1997;126:123; Badri Lancet 2002;359:2059 Treatment of TB in HIV co-infection Generally same as for those without HIVinfection But there are challenges - Drug interaction between TB and HIV drugs - Adherence to TB and HIV drugs Immune Reconstitution Inflammatory Syndrome (IRIS) In patients with TB & HIV infection If TB is not diagnosed ART started for HIV treatment Patient worsens This is a PARADOXICAL reaction Immunity is improving but patient appears worse temporary and usually not dangerous But important to inform patient, watch and manage Quiz The risk of developing TB disease in healthy v/s HIV population? 10% each year in people with HIV infection 10% over a lifetime if otherwise healthy What is the leading cause of death among HIV patients in USA? Hepatitis C