* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Rapid Access Atrial Fibrillation/Flutter Clinic
Survey
Document related concepts
Transcript
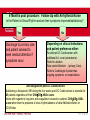
New Atrial Fibrillation/Flutter Pathway and GRASP Tool Kay Elliott Arrhythmia Nurse Specialist Dorset County Hospital NHS Foundation Trust NEW ONSET ATRIAL FIBRILLATION/FLUTTER New Onset Atrial Fibrillation or Flutter Is the patient acutely unwell? Yes Admit to hospital Rate or Rhythm control strategy initiated and discharged back to primary care with followup/onward referrals if required. Patients requiring DC Cardioversion referred to AF/Flutter Clinic No See next slide Primary Care Initiate appropriate stroke/TIA prophylaxis according to CHADS–VASc score (BOX A) and Initiate appropriate rate control (BOX B) BOX A: CHADS–VASc Scoring Risk Factor Point Heart Failure/LV Dysfunction 1 Hypertension 1 Aged > 75 2 Diabetes mellitus 1 Stroke / TIA 2 Vascular disease 1 Age 65-74 1 Female 1 CHADS–VASc Result: 0 = Aspirin 75mg – 325mg daily or no antithrombotic therapy (preference for no therapy) 1 = Either OAC or aspirin (preference for OAC rather than aspirin) > 2 = OAC recommended Box B: Rate control First Line: Beta-blocker (e.g. Bisoprolol) or a rate limiting calcium antagonist (e.g. Diltiazem), if beta-blocker contraindicated Second Line: Digoxin – additional to optimise rate control, where required. As monotherapy only in predominantly sedentary patients. Paroxysmal NEED FURTHER ADVICE? Persistent ARRHYTHMIA NURSE: 01305 254920 Refer to cardiology team: referral letter or choose and book Cardiologist Appropriate strategy initiated with onward plan/referrals made. Patients requiring DC Cardioversion referred to AF/Flutter Clinic Fax Dorset County Hospital intranet or by contacting BHF Arrhythmia Nurse) referral to Rapid Access Atrial Fibrillation/Flutter Clinic. (Form attached. Also available on the intranet Rapid Access Atrial Fibrillation/Flutter Clinic ECHO AND ECG BHF ARRHYTHMIA NURSE CLINIC: Review history, symptoms, test and examination results Patient education Agree treatment plan: Rhythm or Rate control Arrange ongoing follow-up, where required Referral to cardiology clinic if other cardiac issues identified Rhythm Control Arrhythmia Nurse Specialist; arrange DC Cardioversion and/or, if indicated: Refer to electrophysiology centre for ablation Rate Control Manage long-term warfarin and rate-control – Primary Care Prepare for DC Cardioversion: Weekly INR (Target 2.5-3.0), must have INR >2.0 for four full weeks prior to DC Cardioversion DC Cardioversion – DAY SURGERY UNIT Procedure and review of medications/onward management plan (Arrhythmia Nurse and Cardiology Specialist Registrar) pre discharge 4 Weeks post procedure: Follow-Up with Arrhythmia Nurse Is the Patient in Sinus Rhythm and are their symptoms improved/satisfactory? Yes 6 Months post procedure: Follow-Up with Arrhythmia Nurse Is the Patient in Sinus Rhythm and are their symptoms improved/satisfactory? Cont... No Depending on clinical indications and patient preference either: Re-attempt DC Cardioversion with additional AA cover (amiodarone) Refer for ablation Rate control/Warfarin - (primary Care) Refer to Cardiologist if patient has ongoing symptoms or complications 6 Months post procedure: Follow-Up with Arrhythmia Nurse Is the Patient in Sinus Rhythm and are their symptoms improved/satisfactory? Yes Discharge to primary care and patient advised to seek medical attention if symptoms recur No Depending on clinical indications and patient preference either: Re-attempt DC Cardioversion with additional AA cover (amiodarone) Refer for ablation Rate control/Warfarin - (primary Care) Refer to Cardiologist if patient has ongoing symptoms or complications Anti-coagulation post DC Cardioversion: Maintaining a therapeutic INR during the four weeks post DC Cardioversion is essential for All patients regardless of their CHADS–VASc score. Advice with regards to long-term anti-coagulation is based on patients’ CHADS–VASc score rather than the presence of sinus rhythm/absence of atrial fibrillation/flutter on ECG/Holter. Over to You – Any Questions?