* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download SPLENOMEGALY and LYMPHADENOPATHIES
Brucellosis wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Meningococcal disease wikipedia , lookup
Gastroenteritis wikipedia , lookup
West Nile fever wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Marburg virus disease wikipedia , lookup
Onchocerciasis wikipedia , lookup
Trichinosis wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Hepatitis C wikipedia , lookup
Chagas disease wikipedia , lookup
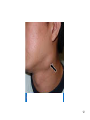
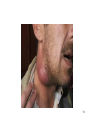
Sarcocystis wikipedia , lookup
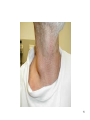
Sexually transmitted infection wikipedia , lookup
Neonatal infection wikipedia , lookup
Hepatitis B wikipedia , lookup
Leishmaniasis wikipedia , lookup
Oesophagostomum wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Leptospirosis wikipedia , lookup
Multiple sclerosis wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Visceral leishmaniasis wikipedia , lookup
Fasciolosis wikipedia , lookup
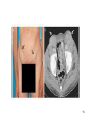
Coccidioidomycosis wikipedia , lookup
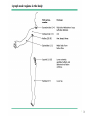
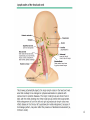
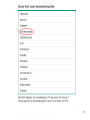
SPLENOMEGALY and LYMPHADENOPATHIES Hasan Atilla Özkan, MD. 1 LYMPHADENOPATIES 1- Anatomy and Definitions • Lymph node regions in the body - head and neck - supraclavicular - deltopectoral - axillary - epitroclear - inguinal - popliteal 2 3 4 • Normal lymph nodes are usually less than 1 cm in diameter (tend to be larger in adolescence than later in life) • Lymph nodes are often palpable in the inguinal region in healthy people, may also be papable in the neck (particularly submandibular) ; because chronic trauma and infection is more common in these regions 5 2. Diagnostic approach A – History B – Physical examination C – Diagnostic tests 6 1. History • Localizing signs or symptoms suggesting infection or malignancy • Exposures likely to be associated with infection (cat stratch disease, high risk behavior) • Constitutional symptoms such as fever, night sweets or weight loss • Use of medications that can cause lymphadenopathy • Foreign travel 7 8 9 2. Physical examination All lymph node groups should be examined with the following characteristics in mind: • Location • Localized or generalized • Size • Tenderness • Consistency • Fixation 10 11 12 13 14 15 Location - 1 • Localized lymphadenopathy - suggest local causes, search for pathology in the area of node drainage - some systemic disease can also present with localized adenopathy * tularemia * aggressive lymphoma, etc 16 Location - 2 • Cervical adenopathy - bacterial infections - infectious mononucleosis - toxoplasmosis - tuberculosis - lymphoma - kikuchi’s disease - head and neck malignancies 17 Location – 3 • Supraclavicular lymphadenopathy - is associated with high risk of malignancy - right supra: mediastinum, lungs or esophagus - left supra (Virchow’s node): abdominal malignancy 18 Location - 4 • Axillary - drainage from the arm, thoracic wall and breast - infections are common causes -in the absence of upper extremity lesions, cancer is often found (particularly breast cancer) 19 Location - 5 • Epitrochlear - always pathologic - infections of the forearm and hand, lymphoma, sarcoidosis, tularemia and secondary syphilis • Inguinal - usually caused by lower extremity infection, sexually transmitted disease or cancer 20 Location - 6 • Generalized lymphadenopathy - Usually a manifestation of systemic disease * HIV infection * mycobacterial infection * infectious mononucleosis * systemic lupus erythematosis * medications * lymphoma / leukemia 21 3. Diagnostic tests • Laboratory testing - CBC Chest X-ray PPD HIV Ab ANA Other spesific test in need 22 • Lymph node biopsy; (If an abnormal node has not resolved after 4 weeks or suspect of malignancy) - Open biopsy: genarally is the best test - Fine needle aspiration: useful when searching for reccurence of cancer - Core needle biopsy: in situtition where the open lymph node biopsy can not be performed 23 • Incision and drainage • Imaging • Observation over time 24 SPLENOMEGALY A. General Information • Hematopoietic organ capable of supporting elements of the erythroid, myeloid, megakaryositic, lymphoid and monocyte-macrophage systems • Participates in cellular and humoral immunity through its lymphoid elements • Removes senescent RBC, bacteria, and other particules from the circulation through monocytemacrophage system (major function) 25 • Splenectomized patients are suspectible to bacterial sepsis, especially with uncapsulated ones • Major lymphoid organ, containing ~ 25% of the total lymphoid mass of the body • About 1/3 of circulating plateletes are suspected in the spleen where they are in equilibrium with circulating plateletes 26 B. Size and Palpability • Median weight is about 150 grams • Average estimated weight of palpable spleen is about 285 grams • Not usually palpable, but may be felt in children, adolescents and some adults, especially those of asthenic build • A palpable spleen usually means the presence of significant splenomegaly • Enlarged spleen on physical examination is more reliable than minimally enlarged on imaging 27 • The clincal or diagnostic significance of a spleen that is minimally enlarged on scan but is not palpable (scanomegaly) is uncertain • Symptoms of an enlarged spleen may include; - pain, a sense of fulness, or discomfprt in the left upper quadrant - pain referred to the left shoulder - early satiety, due to encrachment on the adjacent stomach 28 • Criterias proposed to define the size of normal spleen; * USG – length < 13 cm or thichness ≤ 5 cm * CT scanning – length ≤ 10 cm 29 C. Causes of Splenomegaly • The causes of enlarged spleen are multiple: - most reflect the presence of hepatic or hematologic disease, infection or inflammation 30 • Common causes - liver disease : 33% (cirrhosis) - hematologic malignancy : 27% (lymphoma) - Infection : 23% (AIDS, endocarditis) - congestion or inflammation : 8% - primary splenic disease: 4% (splenic vein thrombosis) - other or uncommon : 5% 31 32 • Massive splenomegaly - chronic myeloid leukemia - myelofibrosis - gaucher disease - lymphoma - Kala-azar (visceral leishmaniasis) - malaria - beta-thalassemia major - AIDS with mycobacterium avium complex 33 34 35 D. Evaluation • History: - chronic alcholism, hepatitis - fatigue, fever, sore throat: inf. Mononucleosis - post-bath pruritis: polycytemia vera • Imaging studies • CBC and pheripheral blood smear • Bone marrow asp. and biopsy 36 • Diagnostic splenctomy * most common pathologic diagnosis; - leukemia / lymphoma 57% - metastatic carcinoma 11% - cyst / pseudocyst 9% - beningn / malign vascular neoplasm 7% - normal 5% • Splenic aspiration / biopsy - is not widely practiced because of a concern for bleeding 37 • General indications for splenectomy - isolated thrombocytopenia, hemolytic anemia or neutropenia - painfully enlarged spleen - traumatic or atraumatic splenic rupture - splenic artery aneurysm - hypersplenism - splenic vascular or parencymal lesion - to allow diagnosis 38 • Spesific conditions in which splenectomy may be considered; – – – – – – – – – – İmmune thrombocytopenia Autoimmune hemolytic anemia Thalassemia major or intermedia Hereditory spherocytosis Primary myelofibrosis Hairy cell leukemia, splenic marginal zone lymphoma Splenic contusion or rupture Splenic abscess or infection Splenic vein thrombosis with bleeding varices Felty’s syndrome 39