* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download chapter 5 slides.
Survey
Document related concepts
Transcript
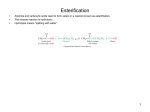
Chapter 5 Lipids Copyright © 2015 McGraw-Hill Education. All rights reserved. No reproduction or distribution without the prior written consent of McGraw-Hill Education. Student Learning Outcomes 1 5.1 Understand the common properties of lipids. 5.2 List three structural forms of lipids (fats) and the role of each in our food supply. Distinguish between fatty acids and triglycerides. Discuss the importance of the essential fatty acids, as well as the balance between omega-3 and omega-6 fatty acids, with respect to health. 5.3 Differentiate among food sources of saturated, monounsaturated, and polyunsaturated fatty acids and cholesterol. 5.4 Explain how lipids are digested and absorbed. Student Learning Outcomes 2 5.5 Name the classes of lipoproteins and classify them according to their functions. 5.6 List the function of lipids, including the roles of phospholipids and the functions of cholesterol in the body. 5.7 Explain the recommendations for fat intake. 5.8 Characterize the symptoms of cardiovascular disease and highlight some known risk factors. 5.1 Lipids: Common Properties 1. What is the common property that all lipid compounds share? Lipids: Common Properties • Diverse group of chemical compounds • One common property, lipids do not readily dissolve in water • Should comprise 20% to 35% of an adult’s total calorie intake 5.2 Lipids: Triglycerides, Phospholipids, and Sterols 1. What are four possible structural forms of lipid? 2. In what ways do fatty acids differ from one another? 3. What is difference between a saturated and unsaturated fatty acid, and between an omega-3 and an omega-6 fatty acid? 4. Which fatty acids are essential? 5. How do triglycerides differ from phospholipids? 6. What are the main functions of cholesterol in body? Types of Lipids and Fats • Types of lipids – Triglycerides – Phospholipids – Sterols (Cholesterol) • Fats (solid) and oils (liquid) – 9 kcal /gm Fatty Acid Structure Saturated Fatty Acid Structure Monounsaturated Fatty Acid Structure Polyunsaturated Fatty Acid Structure Chemical forms of saturated, monounsaturated, and polyunsaturated fatty acids. Fatty Acids and Triglycerides • Found in our body and foods – In triglycerides, composed of three fatty acids bonded to glycerol, an alcohol • Saturated fatty acids, higher in animal fats – Solid form • Unsaturated fatty acids, higher in plant foods – Liquid form – Cis and Trans • Fats are composed of both saturated and unsaturated Cis and Trans Fatty Acids Composition of Common Fats / Oils Chemical Forms of Common Lipids Essential Fatty Acids • Must be supplied by the diet to maintain health • Omega-3 fatty acid (alpha-linolenic acid) • Omega-6 fatty acid (linoleic acid) – immune system function and vision – help form cell membranes – produce eicosanoids, which are involved in practically all important functions in the body Omega-3 Fatty Acid • Primarily from nuts, seeds, fish oil, flax seed oil • Also found in canola, walnuts, mussels, crab, shrimp, and soybean oil • Recommended intake of ~2 servings of fish per week Omega-3 Fatty Acid (alpha-linolenic acid) Omega-6 Fatty Acid • Found in vegetable oils • Need is about 2-4 tablespoons a day Omega-6 Fatty Acid (alpha-linoleic acid) Essential Fatty Acid Categories Health-Related Effects 1 • Archidonic acid (Omega-6 ) – Increases blood clotting – Increases inflammatory responses Health-Related Effects 2 • DHA, EPA (Omega-3) – Decrease blood clotting – Reduce heart attack – Decrease inflammation – Excess may cause hemorrhagic stroke – Other possible uses: lower triglycerides, rheumatoid arthritis, behavioral disorders Signs and Symptoms of Essential Fatty Acids Deficiency • Flaky, itchy skin • Diarrhea • Increased risk of infection • Stunted growth and reduced wound healing Triglycerides • Most common form of fats and oils • 3 fatty acids attached to a glycerol Glycerol + 3 FA’s Triglyceride + 3 H 20 • diglyceride breakdown product of triglyceride consisting of two fatty acids bonded to a glycerol backbone • monoglyceride breakdown product of a triglyceride consisting of one fatty acid attached to a glycerol backbone Phospholipids • Built on a glycerol backbone • Contains phosphorus compound(s) • Found in body • Synthesized by the body as needed • Component of cell membranes Sterols • Multi-ringed structure • Do not have a glycerol backbone • Cholesterol is a sterol • Waxy substance • Do not readily dissolve in water • Found in animal foods 5.3 Fats and Oils in Foods 1. Which foods are the most fat-dense (>60% total calories as fat)? 2. Where is cholesterol found in the food supply? 3. Which types of fat are used as emulsifiers, and what is their function in food? 4. What are some strategies used to produce reducedfat foods? 5. How do fats become rancid, and how can this be prevented? 6. What happens to unsaturated fats during the process of hydrogenation? 7. What regulations are in place to educate and protect the public from trans fats in foods? Lipids in Foods Copyright © McGraw-Hill Education. Permission required for reproduction or display. Dairy Fruits Grains Vegetables Protein ChooseMyPlate.gov MyPlate: Sources of Fats Grains Vegetables Fruits • Crackers • French fried • Fruit pies • Pasta dishes potatoes • Avocadoes with added fat Dairy Protein • Whole milk • Low-fat milk • Marbled meat (1%, 2%) • Bacon • Some yogurts • Poultry (skin) • Many cheeses • Deep-fat-fried • Premium ice meat • Nuts cream 0-18 grams per 0-27 grams per 0-11 gram per 0-10 grams per 7-17 grams per serving serving serving serving serving (Avocados):© Ingram Publishing/SuperStock RF; (chicken and fries): © BananaStock / PunchStock RF; (Cheese): © Pixtal/age fotostock RF Functions of Phospholipids • Emulsifier – Bile acids – Lecithins – Improves food products • Found in wheat germ, peanuts, yolks, soy beans, organ meat Emulsifiers Functions of Cholesterol • Essential component of cell membrane • Produced by the liver • Found only in animal products • Forms important hormones – estrogen – testosterone – vitamin D • Precursor to bile acids Cholesterol Content of Foods Food Sources of Fat Fat Is Hidden in Some Foods • Look on the Nutrition Facts labels • Look on the lists of ingredients • Control portion size Fat in Food • Provides: – Satiety – Flavor – Texture Low-Fat Diets • Need time to adjust to taste of low-fat diet – flavorful fruits, vegetables • Replace whole milk with 1% or skim – In time, whole milk will taste too creamy • Weight control and reduced risk of chronic disease Fat-Replacement Strategies for Reduced-Fat Foods • Fat commonly replaced with sugar – Keeps calories close to the same • Water – Major component of margarine • Z-trim® – Starch derivative that binds with water • Fiber cellulose – Maltrin®, Stellar®, Oatrim • Dairy-Lo® – Protein globules Fat Substitutes • Olestra® or Olean® (links fatty acid to sucrose) – Not digested – FDA approved for fried snack foods – Fat-soluble vitamins absorption issue • Salatrim® or Benefat® – Fat and sucrose – Not digested and/or absorbed well Fat Rancidity • Contains products of decomposed oils • Breakdown of the C=C bonds by UV light, and/or O2 • Unpleasant odor and flavor • Polyunsaturated fatty acid more susceptible • Limited shelf life of food products Prevention of Rancidity • Hydrogenation • Addition of vitamin E • Addition of Butylated hydroxyanisol (BHA) and Butylated hydroxytolune (BHT) Hydrogenation of Fatty Acids • Process used to solidify an oil • Addition of H to C=C double bonds • Increases shelf life of food product • Formation of trans fatty acid – (similar to shape of saturated fatty acid) • Presents health risk like saturated fats Hydrogenation Excessive Trans Fatty Acid Intake • Increases risk for cardiovascular disease • Required to be listed on food labels Minimize Intake of Trans Fat • Limit use of hydrogenated fats • Limit deep-fried foods • Limit high-fat baked goods • Limit use of non-dairy creamers Main Sources of Fatty Acids 5.4 Making Lipids Available for Body Use 1. What enzyme is responsible for digestion of triglycerides? 2. What are the end products of fat digestion? 3. What are the differences between the absorption of long-versus short-chain fatty acids? Digestion • Enzyme lipase • Fat-digesting enzyme produced by salivary glands, stomach, and pancreas – Acts on triglycerides containing shortand medium-chain fatty acids Digestion of Fat in Small Intestine • Primary site of fat digestion • Hormone cholecystokinin (CCK) – Stimulates release of pancreatic lipase • Bile acid released – Emulsifies digested fat • Fat is broken down – To monoglycerides and fatty acids in watery digestive juices Fat Digestion and Absorption 1 Fat Digestion and Absorpti on 2 Fat Digestion and Absorption Digestion of Phospholipids • Enzymes released – From pancreas – From cells of the small intestine • Broken down to – Glycerol – Fatty acids – Remaining parts Digestion of Cholesterol • Enzymes released – From pancreas • Cholesterol is absorbed Absorption • 95% of dietary fat is absorbed • Diffused into the absorptive cells • Short- and medium-chain (<12 C) fatty acids – Are water soluble – Enter the portal system • Long-chain fatty acids re-form into triglycerides – Not water soluble – Enter the lymphatic system 5.5 Carrying Lipids in the Bloodstream 1. How do lipids move through the bloodstream? 2. How are dietary fats packaged in the small intestine and transported? 3. Where are VLDLs made and what do they contain? 4. Where do the LDLs originate and what is their destination? 5. Why are HDLs considered “good” cholesterol? Dietary Fats Are Carried by Chylomicrons • Fatty acids re-formed into triglycerides • Packaged into chylomicrons • Lipoprotein lipase – Breaks down triglycerides in the chylomicrons • Chylomicron remnant – Delivered to the liver Carrying Lipids in the Bloodstream • Water and oil (fat) do not mix easily • Unique system of fat transportation is needed • Lipoprotein compound in bloodstream containing a core of lipids with shell composed of protein, phospholipid, and cholesterol – Vehicle used for lipid transport Structure of a Lipoprotein Other Lipoproteins Transport Lipids from the Liver to the Body Cells • Made primarily by the liver • Very-Low-Density Lipoprotein (VLDL), bad • Low-Density Lipoprotein (LDL), bad • High-Density Lipoprotein (HDL), good Composition of Lipoproteins Major Lipoproteins in Blood Lipoprotein Production and Function High-Density Lipoprotein (HDL) • Synthesized by liver and intestine • High proportion of protein • Picks up cholesterol from dying cells and other sources • Transfers cholesterol to other lipoproteins • Transfers cholesterol directly back to the liver Benefits of a High HDL level • Removes cholesterol from the bloodstream • HDL may block oxidation of LDL • Reduces risk of cardiovascular disease • Pre-menopausal women have higher HDL Scavenger Cells • Scavenger WBC removes (oxidized) LDL from circulation • Build-up of atherosclerosis plaque on walls of the blood vessels • Development of atherosclerosis • Increased vessel damage caused by – Smoking, diabetes, hypertension, homocysteine, high LDL, infection 5.6 Broader Roles for Lipids in the Body 1. What are functions of triglycerides in body? 2. Where are phospholipids found in body? 3. What are some compounds made from cholesterol in body? Functions of Fatty Acids • Provide energy • Efficient storage of energy • Insulating and protecting body • Transport fat-soluble vitamins A, D, E, and K • Phospholipids, become part of cell membrane • Cholesterol, becomes part of hormones, estrogen, testosterone, and precursor of active vitamin D hormone – Structural component in cells and lipoproteins Phospholipid and Cell Membranes Adipose Cell 5.7 Recommendations for Fat Intake 1. How does percent of calories as fat in North American diet compare to recommendations? 2. What is limit for cholesterol intake? 3. What are characteristics of Mediterranean diet? Recommendations for Fat Intake • No RDA but 2010 Dietary Guidelines AMDR 20% to 35% of calories, 44 to 78 grams • AHA recommendations – 20-30% of total kcal from fat – 7-10% can come from saturated/trans fat – 200-300 mg cholesterol/day • Average U.S. intake: – 33% of total kcal from fat – 13% of kcal from saturated fat – 180-320 mg cholesterol/day Goal of Healthy People 2020 • Reduce consumption of saturated fat in population ages 2 years and older to 9.5% of total calorie intake AHA Recommendations Advice from National Cholesterol Education Program and Food and Nutrition Board • Keep saturated fat, cholesterol, and trans fat to a minimum • If diet and exercise are ineffective, medication intervention recommended – E.g., Atorvistatin (Lipitor) – Require physician monitoring Other Recommendations • Fat intake can be higher as long as saturated and trans fatty acid are minimal • Eat plenty of fruits and vegetables • Cut down on red meats • Cut down on simple sugars and refined carbohydrate • Promote healthy weight • Be active Tips for Avoiding Too Much Fat, Saturated Fat, Cholesterol, and Trans Fat Lipids Concept Map Nutrition and Your Health Lipids and Cardiovascular Disease Cardiovascular Disease • Leading cause of death in North America – 600,000 people die each year – Annual cost is $108.9 billion each year • Myocardial infarction – death of part of heart muscle – also termed a heart attack • Cerebrovascular accident – death of part of brain tissue due typically to a blood clot – also termed a stroke Development of Cardiovascular Disease • Plaque – cholesterol-rich substance deposited in blood vessels – contains various white blood cells, smooth muscle cells, various proteins, cholesterol, other lipids, and eventually calcium The Road to a Heart Attack Plaque Buildup in Artery Walls View of cholesterol plaque deposited inside blood vessel Risk Factors for Cardiovascular Disease • Total blood cholesterol > 200 mg/dl • Smoking – Increases clotting – Increases expression of genetic link • Hypertension (greater than 139/89) • Diabetes – Insulin increases cholesterol synthesis – Guarantees development of cardiovascular disease Other Risk Factors • Low HDL (< 40 mg/dl) • Age • Family history • Blood triglycerides > 200 mg/dl • Obesity – Fat around the waist – Insulin resistance • Inactivity Signs of a Heart Attack • Intense, prolong chest pain • Shortness of breath • Sweating • Nausea and vomiting • Dizziness • Weakness • Jaw, neck, shoulder pain • Irregular heartbeat Medications to Lower Blood Lipids • For those who experience a heart attack – Or have CVD or diabetes • Heart Attack Risk Calculator • Medication to lower LDL – Reduce cholesterol synthesis (Statins, “Lipitor”) – Binds to bile acids for elimination • Medication to lower blood triglycerides – Reduce triglyceride synthesis Lowering LDL • See your doctor to assess for other conditions • Reduce dietary saturated fat and cholesterol • Increase mono and polyunsaturated fats in diet • Increase dietary fiber (soluble) Lowering Blood Triglycerides • Is the most diet-responsive blood lipid • Avoid overeating • Limit alcohol • Limit simple sugars • Small frequent meals • Include fish in the diet, 2 times per week Plant Sterols for Cardiovascular Disease • Benecol and Take Control margarines – Plant stanol/sterol esters – Cholesterol-lowering effects – Decrease absorption of cholesterol and lower amount returning via enterohepatic circulation – Liver takes up more cholesterol from the blood Raising HDL • Physical activity • At least 45 min/day, 4 days a week • Don’t smoke • Eat regularly • Eat less total fat • Moderate intake of alcohol increases HDL Sorting Out One’s Goals for Cardiova scular Disease Preventio n/Treatm ent Surgical Treatment for Cardiovascular Disease • Two common surgical treatments – Percutaneous transluminal coronary angioplasty (PTCA) • insertion of a balloon catheter into an artery, once advanced to area of lesion, balloon is expanded to crush lesion – Coronary artery bypass graft (CABG) • removal and use of a saphenous vein (leg), or mammary vein, sewn into aorta, for bypass