* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Distal Convoluted Tubules
Survey
Document related concepts
Transcript
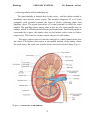
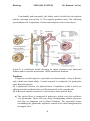
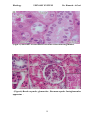
Histology URINARY SYSTEM Dr. Hameda A.Gazi Lecture Objectives By the end of this lecture, students are expected to: 1. List and describe the blood supply of kidney. 2. Outline the histological features of the nephron . 3. Compare the local function and histological features of proximal and distal convoluted tubules. 4. Outline the different types of epithelium within urinary passages. 5. Summarize the functional and histological structure of medulla of kidney. 6. Relate the functional to histological feature of the of cells of proximal and distal convoluted tubules. 7. Outline the structural and functional adaptations of the gastroesophageal glands. 8. Outline the difference in histological features of outer layer of esophagus along its course. The Urinary System Introduction The Urinary System consists of paired kidneys and ureters. unpaired bladder and urethra. The function of Urinary System: Function 1. 2. 3. 4. filter blood and reabsorb nutrients. control the water, ion, and salt balance of the body. maintain the acid-base balance of the blood. excrete metabolic wastes (urea and uric acid), toxins, and drug components. 5. secrete hormones, such as renin and erythropoietin. 6. produce calcitriol (an active form of vitamin D) to help the body absorb dietary calcium into the blood. Kidneys General structure 1. Kidneys are paired bean-shaped organs enveloped by a thin capsule of connective tissue. 2. Each kidney is divided into an outer cortex and an inner medulla. 1 Histology URINARY SYSTEM Dr. Hameda A.Gazi 3. Each kidney contains about 2 million nephrons. A nephron and the collecting tubule into which it drains form a uriniferous tubule. B. The renal hilum is a concavity on the medial border of the kidney. It houses arteries, veins, lymphatic vessels, nerves, and the renal pelvis. C. The renal pelvis (Figure 18.1) is a funnel-shaped expansion of the upper end of the ureter. It is continuous with the major renal calyces, which in turn have several small branches, the minor calyces. D. The renal medulla lies deep to the cortex but sends extensions (medullary rays) into the cortex. 1. Renal (medullary) pyramids are conical or pyramidal structures that compose the bulk of the renal medulla. a. Each kidney contains 10 to 18 renal pyramids. b. Each pyramid consists primarily of the thin limbs of loops of Henle, blood vessels, and collecting tubules. 2. The renal papilla is located at the apex of each renal pyramid. It has a perforated tip (area cribrosa) that projects into the lumen of a minor calyx. E. The renal cortex is the superficial layer of the kidney beneath the capsule. It consists primarily of renal corpuscles and convoluted tubules. 1. Renal columns of Bertin are extensions of cortical tissue between adjacent renal pyramids. 2. Medullary rays are groups of straight tubules that extend from the base of each renal (medullary) pyramid into the cortex. The renal cortex is composed of renal corpuscles and various cortical tubules, which include 1. proximal convoluted tubules. 2. distal convoluted tubules. 3. cortical collecting tubules. F. The renal lobe consists of a renal pyramid and its closely associated cortical tissue. G. The renal lobule consists of a central medullary ray and the closely associated cortical tissue on either side of it, extending as far as an interlobular artery. Its many nephrons drain into the 2 Histology URINARY SYSTEM Dr. Hameda A.Gazi collecting tubules of the medullary ray. The renal medulla is located deep to the cortex , and its tubules extend as medullary rays into the cortex region. The medulla comprises 10 to 18 renal pyramids; each pyramid contains the loops of Henle, collecting ducts, and papillary ducts. The apical projection of a renal pyramid is called the renal papilla. The papillary ducts empty urine at the tip of a renal papilla onto its surface, which is called the area cribrosa (perforated area). Each renal papilla is surrounded by a space, the minor calyx; several minor calices unite to form a major calyx. There are two or three major calyces for each kidney. The major calices unite to form the renal pelvis, which funnels urine into the ureter. The hilum is the region in the medial portion of the kidney where the renal artery, the renal vein, and the ureter enter and exit the kidney (Fig.1). (Figur-1): Overview of the kidney. 3 Histology URINARY SYSTEM Dr. Hameda A.Gazi Functionally and structurally, the kidney can be divided into the nephron and the collecting system (Fig .2). The nephron produces urine. The collecting system adjusts the composition of urine and transports urine to the calyces. (Figur-2) A uriniferous tubule showing its major structural and functional features and its vascular associations. ADH, antidiuretic hormone. Nephron Comprises a renal corpuscle, a proximal convoluted tubule, a loop of Henele, and a distal convoluted tubule. A renal corpuscle is composed of a glomerulus and a Bowman capsule. (1) A glomerulus consists of a spherical knot of capillaries, which is fed by an afferent arteriole and drained by an efferent arteriole at the vascular pole. (2) A Bowman capsule consists of a visceral layer and a parietal layer. a) The visceral layer is composed of podocytes, which cover the capillaries of a glomerulus. These cells have long, interdigitating cellular processes and play an important role in blood filtration. The interstitial tissues surrounding the glomerular capillaries contain cells called intraglomerular mesangial cells. 4 Histology URINARY SYSTEM Dr. Hameda A.Gazi b) The parietal layer of the Bowman capsule is a hollow spherical structure lined by simple squamous epithelium. The space between the visceral and the parietal layers of the Bowman capsule is called the Bowman space. Blood flows through the glomerular capillaries, and its plasma passes through the glomerular filtration barrier (the fused basal laminae of the endothelial cells and the podocytes. (Fgur-3): A diagram illustrating components of the renal corpuscle. Podocytes Podocytes are highly modified epithelial cells that form the visceral layer of the Bowman capsule. They have complex shapes and possess several primary processes that give rise to many secondary processes called pedicels. (1) Pedicels (a) Pedicels embrace the glomerular capillaries and interdigitate with pedicels arising from other primary processes. (b) Their surfaces facing the Bowman space are coated with podocalyxin, a protein that is thought to maintain their organization and shape. Filtration slits are elongated spaces between adjacent pedicels. Diaphragms, composed of a layer of filamentous material, bridge each filtration slit. c. The renal glomerulus is the tuft of capillaries that extends into the Bowman capsule. 5 Histology URINARY SYSTEM Dr. Hameda A.Gazi Renal or Blood-Urine Barrier 1. Glomerular endothelium(fenestrated). 2. Basement membrane. 3. Filtration slit diaphragms. Mesangial cells Found adhering to in between capillaries Have cytoplasmic extension which penetrate between endothelial cells. They are contractile and have receptor for angiotensin 2 When activated, the glomerular flow is reduced. The natriuretic factor relaxes the mesangial cells and increase the renal blood flow. Produce cytokines and prostglangins. Juxtaglomerular Apparatus The JG apparatus is located at the vascular pole of the renal corpuscle. Consists of 3 main components 1- Juxtaglomerular cells (a) are modified smooth muscle cells that exhibit some characteristics of protein secreting cells. (b) are located primarily in the wall of the afferent arteriole, but a few may also be present in the efferent arteriole. (c) synthesize renin (a proteolytic enzyme) and store it in secretory granules. 2- Macula densa cells (a) are tall, narrow, closely packed epithelial cells of the distal tubule. (b) have elongated, closely packed nuclei that appear as a dense spot (macula densa) by light microscopy. (c) may monitor the osmolarity and volume of the fluid in the distal tubule and transmit this information to JG cells via the gap junctions between the two cell types. 3- Extraglomerular mesangial cells (a) are also known as polkissen (pole cushion) or lacis cells. (b) lie between the afferent and efferent glomerular arterioles(Fig.6) 6 Histology URINARY SYSTEM Dr. Hameda A.Gazi Proximal Convoluted Tubules a. The proximal convoluted tubule is lined by a single layer of irregularly shaped (cuboidal to columnar) epithelial cells that have microvilli forming a prominent brush border. These cells exhibit the following structures: (1) Apical canaliculi, vesicles, and vacuoles (endocytic complex), which function in protein absorption. (2) Prominent interdigitations along their lateral borders, which interlock adjacent cells with one another. (3) Numerous mitochondria compartmentalized in the basal region by extensive infoldings of the basal plasma membrane, which supply energy for the active transport of Na_ out of the tubule. b. Function (1) The proximal convoluted tubule drains the Bowman space at the urinary pole of the renal corpuscle. (2) It resorbs from the glomerular filtrate all of the glucose, amino acids, and small proteins and at least 80% of the sodium chloride and water. (3) It exchanges H in the interstitium for HCO3 in the filtrate (Figur,4). (Figur-4):Structure of both Proximal convolute d and straight tubules. The Loop of Henle The Loop of Henle is a continuation of the proximal convoluted tubule. It is a U-shaped structure that includes a descending limb and an ascending limb. The descending limb consists of a thick descending limb (proximal straight tubule) and a thin descending limb (descending thin segment). The ascending 7 Histology URINARY SYSTEM Dr. Hameda A.Gazi limb contains a thin ascending limb (ascending thin segment) and a thick ascending limb (distal straight tubule). The loop of Henle plays a crucial role in generating a high sodium concentration gradient in the interstitium of the renal medulla. This permits water to move passively from collecting ducts into the interstitium. The descending and ascending thin segment tubules are lined by squamous cells and are structurally similar to each other. The descending limb is permeable to water, Cl-, and Na+. The tubules of the descending limb reabsorb water and salts and reduce the volume of the filtrate that has passed through the proximal convoluted tubules. The ascending limb is very active physiologically. It is impermeable to water, and it actively pumps Cl- and Na+ from the lumen into the medullary interstitium (fig,3). Distal Convoluted Tubules Distal Convoluted Tubules are lined by small, simple cuboidal epithelial cells, which have no brush border. They may show a few short, irregular microvilli on their apical surfaces and plasma membrane infoldings on their basal region at the EM level (Fig.5). Their lumens appear clearer and wider than those of proximal tubules. The distal convoluted tubules are located in the cortex of the kidney and are closely associated with the renal corpuscles. At the junction between the distal straight and the convoluted tubules, there is an important specialized sensory structure, the macula densa, which senses and monitors ionic content and water volume of the filtrate. The macula densa is composed of cells that are taller and more tightly packed than other cells of the distal tubule (Fig.6). This portion of the distal tubule is positioned between afferent and efferent arterioles at the vascular pole of the renal corpuscle. The distal convoluted tubules remove Na+ and add K+ to the filtrate if aldosterone stimulation is present; they also reabsorb bicarbonate ions and secrete ammonium to adjust the pH balance. The distal convoluted tubules connect distal straight tubules (thick ascending limb of the loop of Henle) to the collecting tubules. The distal convoluted and straight tubules are structurally similar to each other, differing mainly in their locations and courses. 8 Histology URINARY SYSTEM Dr. Hameda A.Gazi (Figur-5):Structure of both distal convolute d and collecting tubules. (Figur-6):Renal corpuscle, glomerulus , Bowman capsule Juxtaglomerular apparatus . 9 Histology URINARY SYSTEM Dr. Hameda A.Gazi Collecting tubules Collecting tubules (Figure.6) have a different embryological origin from that of nephrons. They have segments in both the cortex and medulla and converge to form larger and larger tubules. 1. Cortical collecting tubules are located primarily within medullary rays, although a few are interspersed among the convoluted tubules in the cortex (cortical labyrinth). They are lined by a simple epithelium containing two types of cuboidal cells. a. Principal (light) cells possess a round central nucleus and a single central cilium. b. Intercalated (dark) cells are less numerous than principal cells and possess microplicae (folds) on their apical surface and numerous apical cytoplasmic vesicles. 2. Medullary collecting tubules. In the outer medulla, medullary collecting tubules are similar in structure to cortical collecting tubules and contain both principal and intercalated cells in their lining epithelium. In the inner medulla, the collecting tubules are lined only by principal cells (Figure 18.6). 3. Papillary collecting tubules (ducts of Bellini) a. Papillary collecting tubules are large collecting tubules (200–300 _m in diameter) formed from converging smaller tubules. b. They are lined by a simple epithelium composed of columnar cells that have a single central cilium. c. They empty at the area cribrosa, a region at the apex of each renal pyramid that has 10 to 25 openings through which the urine exits into a minor calyx. The vascular supply to the kidney The vascular supply to the kidney comes from the renal artery, which enters the kidney at the hilum; segmental branches of the renal artery give rise to the interlobar arteries. These pass through the renal columns between the renal pyramids and give rise to arcuate arteries. The arcuate arteries run along the junction between the cortex and the medulla of the kidney and give rise to the interlobular arteries, which extend into the medulla to supply the afferent arterioles of renal corpuscles. Each afferent arteriole supplies a glomerulus of capillaries from which blood is drained by an efferent arteriole at the vascular pole. The efferent arterioles of corpuscles in the outer cortex feed into the peritubular capillary network, which supplies the cortical tissue surrounding the cortical tubules. These peritubular capillaries provide for gas and material 10 Histology URINARY SYSTEM Dr. Hameda A.Gazi exchange and also receive renal interstitial fluid, which is reabsorbed out of the tubules and goes back into the vascular bed. Venules carry blood to the interlobular veins and to the arcuate veins in the renal corticomedullary junction. The efferent arterioles of deeper (juxtamedullary) corpuscles extend into the medulla where they give rise to capillaries called vasa recta, which receive interstitial fluid (reabsorbed from filtrate) in the medulla and send it back to the circulation. The vasa rectae take a hairpin course in the medulla following the loop of Henle. They return to the corticomedullary junction to join the interlobular veins and then drain into the arcuate veins. The arcuate veins drain blood into the interlobar veins, which then merge to form the branches of the segmental renal veins, which in turn finally merge into the renal vein (Fig.7). (Figur-7): Vascular Supply of the Kidney Ureters The two ureters lie in the extraperitoneal connective tissue, laterally positioned on each side of the vertebral column. The ureters are long, relatively small tubules lined by transitional epithelium and surrounded by a thin layer of smooth muscle and connective tissue. Superiorly, they drain the funnel-shaped renal pelvis, and inferiorly, they empty into the bladder by penetrating its posterior wall. The ureters have a much thinner wall than the bladder. Like most tubular organs, the wall of the ureter is composed of several layers of tissues: mucosa, muscularis, and adventitia. It possesses a two-layer muscularis (an inner longitudinal and outer circular layer of smooth muscle) in its upper two-thirds. 11 Histology URINARY SYSTEM Dr. Hameda A.Gazi The lowest third possesses an additional outer longitudinal layer of smooth muscle. Urinary Bladder The urinary bladder, a distensible sac-shaped organ located in the pelvic cavity, temporarily stores urine. The wall of the bladder has three openings, two of them for ureters to enter and one for emptying urine into the urethra. Like the ureter, the urinary bladder wall consists of mucosal, muscularis, and adventitial layers, but the bladder wall is much thicker, having three substantial layers of smooth muscle in the muscularis. (1) The mucosa consists of a transitional epithelium lining and a layer of connective tissue (lamina propria) containing blood vessels and nerve fibers. (2) The muscularis contains the three layers of smooth muscle: inner longitudinal smooth muscle, middle circular smooth muscle, and outer longitudinal smooth muscle.The muscularis contracts in different directions to enable the urinary bladder to empty urine. (3) The outer portion of the bladder is protected by both a serosa and an adventitia depending on whether it projects into the peritoneal cavity. The superior surface of the bladder is covered by serosa, which is a layer of connective tissue covered by mesothelium; the in Urethra 1. Overview a. The urethra conveys urine from the bladder outside the body. In males, the urethra also carries semen during ejaculation. b. It has a two-layer muscularis consisting of an inner longitudinal and an outer circular layer of smooth muscle. c. It is surrounded at some point by an external sphincter of skeletal muscle, which permits its voluntary closure. 2. Male urethra a. The male urethra is about 20 cm long and is divided into prostatic, membranous, and cavernous portions. b. It is lined by transitional epithelium in the prostatic portion and by pseudostratified or stratified columnar epithelium in the other two portions. The 12 Histology URINARY SYSTEM Dr. Hameda A.Gazi fossa navicularis, located at the distal end of the cavernous urethra, is lined by stratified squamous epithelium. c. It contains mucus-secreting glands of Littre in the lamina propria. 3. Female urethra a. The female urethra is much shorter (4–5 cm long) than the male urethra. b. It is lined primarily by stratified squamous epithelium, although patches of pseudostratified columnar epithelium are present. c. It may contain glands of Littre in the lamina propria. 13