* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Heart Failure Medication Titration Protocols - sha
Survey
Document related concepts
Transcript
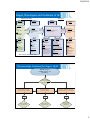
12/5/2013 Heart Failure Medication Titration Protocols Fadwa F. Al-Khuraisi, Bsc.Pharm, SCSCP Clinical Pharmacist ,Prince Sultan Cardiac Center Dec, 2013 Objectives • Introduction • Heart failure medication titration protocols • Heart Failure Medication Titration Problem Solving • PSCC heart failure clinic data 1 12/5/2013 Activation of the SNS; Release of catecholamines Contractility HR Activation of Renin angiotensin aldosterone system Antidiuretic hormone circulatory volume Renal perfusion Vasoconstriction + = preload, SV, CO Renin release + = Preload - = After load - = pulmonary edema Angiotensin II - = cardiac oxygen demand and work, co - = cell death/ apoptosis Aldosterone level Adaptive mechanisms in systolic heart failure PHARMACOTHERAPY OF HEART FAILURE Heart failure Inotropic agents, Digoxin X Reduced cardiac output X Digoxin Beta blockers Renin Sympathetic nervous system activation X Angiotensin I Vasodilators X ACEIs X X Vasoconstriction Angiotensin II X ARBs X Spironolactone X Aldosterone Elevated cardiac filling pressures ARBs X Sodium and water retention X Diuretics Cardiac Remodeling 2 12/5/2013 Stages, Phenotypes and Treatment of HF At Risk for Heart Failure Heart Failure STAGE A STAGE B STAGE C At high risk for HF but without structural heart disease or symptoms of HF Structural heart disease but without signs or symptoms of HF Structural heart disease with prior or current symptoms of HF e.g., Patients with: · HTN · Atherosclerotic disease · DM · Obesity · Metabolic syndrome or Patients · Using cardiotoxins · With family history of cardiomyopathy Structural heart disease THERAPY e.g., Patients with: · Previous MI · LV remodeling including LVH and low EF · Asymptomatic valvular disease THERAPY Goals · Heart healthy lifestyle · Prevent vascular, coronary disease · Prevent LV structural abnormalities Goals · Prevent HF symptoms · Prevent further cardiac Drugs · ACEI or ARB in appropriate patients for vascular disease or DM · Statins as appropriate appropriate · Beta blockers as appropriate remodeling Drugs · ACEI or ARB as In selected patients · ICD · Revascularization or valvular surgery as appropriate ACC,AHA HF GUIDELINE 2013 Development of symptoms of HF STAGE D Refractory HF Refractory symptoms of HF at rest, despite GDMT e.g., Patients with: · Known structural heart disease and · HF signs and symptoms HFpEF HFrEF THERAPY THERAPY Goals · Control symptoms · Improve HRQOL · Prevent hospitalization · Prevent mortality Strategies · Identification of comorbidities Treatment · Diuresis to relieve symptoms of congestion · Follow guideline driven indications for comorbidities, e.g., HTN, AF, CAD, DM · Revascularization or valvular surgery as appropriate Goals · Control symptoms · Patient education · Prevent hospitalization · Prevent mortality Drugs for routine use · Diuretics for fluid retention · ACEI or ARB · Beta blockers · Aldosterone antagonists Drugs for use in selected patients · Hydralazine/isosorbide dinitrate · ACEI and ARB · Digoxin In selected patients · CRT · ICD · Revascularization or valvular surgery as appropriate e.g., Patients with: · Marked HF symptoms at rest · Recurrent hospitalizations despite GDMT THERAPY Goals · Control symptoms · Improve HRQOL · Reduce hospital readmissions · Establish patient’s endof-life goals Options · Advanced care measures · Heart transplant · Chronic inotropes · Temporary or permanent MCS · Experimental surgery or drugs · Palliative care and hospice · ICD deactivation Pharmacologic Treatment for Stage C HFrEF HFrEF Stage C NYHA Class I – IV Treatment: Class I, LOE A ACEI or ARB AND Beta Blocker For all volume overload, NYHA class II-IV patients For persistently symptomatic African Americans, NYHA class III-IV For NYHA class II-IV patients. Provided estimated creatinine >30 mL/min and K+ <5.0 mEq/dL Add Add Add Class I, LOE C Loop Diuretics Class I, LOE A Hydral-Nitrates Class I, LOE A Aldosterone Antagonist 3 12/5/2013 Pharmacological Therapy for Management of Stage C HFrEF Recommendations COR LOE I C I A I A IIa A IIb A III: Harm C Diuretics Diuretics are recommended in patients with HFrEF with fluid retention ACE Inhibitors ACE inhibitors are recommended for all patients with HFrEF ARBs ARBs are recommended in patients with HFrEF who are ACE inhibitor intolerant ARBs are reasonable as alternatives to ACE inhibitor as first line therapy in HFrEF The addition of an ARB may be considered in persistently symptomatic patients with HFrEF on GDMT Routine combined use of an ACE inhibitor, ARB, and aldosterone antagonist is potentially harmful Pharmacological Therapy for Management of Stage C HFrEF Recommendations COR LOE I A I A I B III: Harm B I A IIa B IIa B Beta Blockers Use of 1 of the 3 beta blockers proven to reduce mortality is recommended for all stable patients Aldosterone Antagonists Aldosterone receptor antagonists are recommended in patients with NYHA class II-IV HF who have LVEF ≤35% Aldosterone receptor antagonists are recommended in patients following an acute MI who have LVEF ≤40% with symptoms of HF or DM Inappropriate use of aldosterone receptor antagonists may be harmful Hydralazine and Isosorbide Dinitrate The combination of hydralazine and isosorbide dinitrate is recommended for African-Americans, with NYHA class III–IV HFrEF on GDMT A combination of hydralazine and isosorbide dinitrate can be useful in patients with HFrEF who cannot be given ACE inhibitors or ARBs Digoxin Digoxin can be beneficial in patients with HFrEF 4 12/5/2013 Heart Failure Medication Titration • Heart failure (HF) guidelines recommend timely titration of beta blockers , ACEIs and other heart failure medications to doses shown to be effective in clinical trials. • Doses are often not optimized in clinical practice because of difficulty in organizing frequent clinic visits and greater risk of side effects Assessment of Treatment with Lisinopril and Survival Trial (ATLAS) • Lisinopril given to 3164 patients (NYHA II-IV) EF < 30% • lisinopril 2.5 to 5 mg was given for 2 weeks then 12.5 to 15 mg for an additional 2 weeks . • If the initial doses were tolerated, subjects were randomly assigned to daily therapy with lisinopril 2.5 to 5 mg (low dose) or 32.5 to 35 mg (high dose) 5 12/5/2013 Kaplan-Meier analysis showing time to death in the low-dose and high-dose lisinopril groups. All cause of mortality did not differ significantly between the two groups (8% lower in the highest dose group compared with the lowest dose ; p=0.128) Packer M et al. Circulation 1999;100:2312-2318 Kaplan-Meier analysis showing time to death or hospitalization for any reason in the low-dose and high-dose groups. In high dose group ,hospitalization and the combined end point of death and hospitalization were reduced by 24% (p=0.003) and 12% (p=0.002), respectively. The higher dose was tolerated by 90% of assigned patients Packer M et al. Circulation 1999;100:2312-2318 6 12/5/2013 Heart Failure Clinic Role • The goals for a heart failure clinic must be – Verify diagnosis, – Optimize medication, – and provide comprehensive and intensive medical education and counseling in patients. – increased safety and self-confidence in our patients, creating highly motivated patients with high compliance, increased quality of life , and less need for hospitalization , leading to reduce cost for the heart failure care Clinical Pharmacist Role • • • • • • • Medication histories Medication review Assess the patient compliance Optimizing dosing of key medications Test and investigations Tailoring therapy Close monitoring of response to drug therapy • Dealing with adverse effects 7 12/5/2013 Heart Failure Score Symptoms / sign Value Orthopnea Score 0.5 PND 1 Reduction in exercise tolerance 0.5 Resting tachycardia > 100 0.5 JVP> 4 cm 0.5 HJR Positive 1 S3 present 1 Basal crackles 1 Hepatomegaly 0.5 Peripheral edema 0.5 Total Patient status at the time of clinical review will be recorded in the form of a “heart failure score ” . Derived by assigning a value to defined series of clinical variables based on Framingham data for diagnosis of heart failure Heart failure score <2 Initial visit Beta Blocker, ACEIs and diuretics • Step 1: optimization of ACEIs doses • • • Patients do not need to be taking high doses of ACE inhibitors before being considered for Step 2: introduced beta-blockers, for treatment with Beta Blocker. The addition of Beta Blocker to patient s those already on beta-blocker, the taking low dose ACEIs produces a greater dose will be titrated at 2 weekly reduction in symptoms and in the risk of intervals towards maximum goal death than an increase in the dose of an ACEIs based doses 8 12/5/2013 Heart failure score ≥ 2 Step 1: increase furosemide to 120 mg /day or optimization of ACEIs Step 2: add spironolactone (up to 50 mg/day) in patients with persistent class III or IV symptoms Step 3: addition of digoxin 0.25 mg/day Step 4: increase furosemide with twice daily doses up to maximum of 500 mg twice daily with doubling the increments Heart failure score < 2 : Titration of beta blockade Step 5: addition of Metolazone Heart Failure Patients Management Follow Up • Patients intensified therapy will be reviewed in approximately 2 weeks with clinical assessment and measurement of: – ProBNP – Plasma electrolytes and creatinine – Postural hypotension, heart rate – Intolerance of medication 9 12/5/2013 Heart Failure Patients Management Follow Up The over all aim is to: – Establish a stable clinical status with a heart failure score<2 – and maximum goal based doses of ACEIs or ARBs and beta-blockers. Medical Therapy for Stage C HFrEF: Magnitude of Benefit Demonstrated in RCTs GDMT ACE inhibitor or ARB NNT for Mortality RR Reduction in Reduction (Standardized Mortality to 36 mo) RR Reduction in HF Hospitalizations 17% 26 31% 34% 9 41% Aldosterone antagonist 30% 6 35% Hydralazine/nitrate 43% 7 33% Beta blocker 10 12/5/2013 Should an Aldosterone Antagonist Be the Next Step After ACE Inhibitor + -Blocker? Aldosterone Antagonist Angiotensin Receptor Blocker Effect on mortality 15%-30% 5%-10% Effect on risk of death or CHF hospitalization 15%-30% 10%-15% Effect on blood pressure No change Decrease Renal insufficiency Hyperkalemia Renal insufficiency Hyperkalemia Other safety Initiation strategies of ACEIs Stop or reduce dose Start low dose of diuretics ACEIs for 24 hrs those at higher risk of adverse events : • higher doses of loop diuretics. • severe heart failure or diabetes. • Renal impairments • Hypotension . 1 or 2 week • check BP Double the ACEI dose until target • Renal function dose achieved or not tolerated. • and k+ at baseline ,after 1-2 weeks, with any dose increase and periodically In acute HF, may increase dose more rapidly e.g. q 1-2 days . thereafter. • Expect some rise in BUN ,SCr and k+ . 11 12/5/2013 Drugs Commonly Used for HFrEF (Stage C HF) Initial Daily Dose(s) Drug Maximum Doses(s) Mean Doses Achieved in Clinical Trials ACE Inhibitors Captopril 6.25 mg 3 times 122.7 mg/d (421) Enalapril 16.6 mg/d (412) Fosinopril Lisinopril Perindopril Quinapril Ramipril Trandolapril ARBs Candesartan Losartan Valsartan 50 mg 3 times 10 to 20 mg 2.5 mg twice twice 5 to 10 mg once 40 mg once 20 to 40 mg 2.5 to 5 mg once once 8 to 16 mg 2 mg once once 5 mg twice 20 mg twice 1.25 to 2.5 mg 10 mg once once 1 mg once 4 mg once 4 to 8 mg once 32 mg once 50 to 150 mg 25 to 50 mg once once 20 to 40 mg twice 160 mg twice --------32.5 to 35.0 mg/d (444) --------------------------------24 mg/d (419) 129 mg/d (420) 254 mg/d (109) Side Effects of ACE inhibitors • Angioedema: – Although rare, can occur at any time when using ACE inhibitors. Stop ACE inhibitor immediately and seek specialist advice. Trial of an ARBs ,possible cross-sensitivity. • Cough : – Pulmonary oedema should be excluded as a cause if cough. – If cough, that is likely to be caused by the ACE Inhibitor, it is not always necessary to discontinue the drug. – If the cough is troublesome or interferes with sleep, consider substituting ACE inhibitor with an ARBs. 12 12/5/2013 Initiation strategies of Beta Blockers Start with low doses Initiate only if stable HF and euvolemic Initial worsening of HF , hypotension and bradycardia occur with high doses of loop diuretics and those with severe HF . Initial co-administration of diuretic useful in limiting BB induce fluid retention •Monitor clinical status, •BP sitting & standing •HR at rest & after 1 minute of walking may be useful to assess adequacy of Bblockade dose. Increase by 50 - 100% q 2-4 weeks Beta Blockers in Heart Flaiure Drug Beta Blockers Bisoprolol Carvedilol Carvedilol CR Metoprolol succinate extended release (metoprolol CR/XL) Initial Daily Dose(s) Maximum Doses(s) Mean Doses Achieved in Clinical Trials 1.25 mg once 3.125 mg twice 10 mg once 10 mg once 50 mg twice 80 mg once 8.6 mg/d (118) 37 mg/d (446) --------- 12.5 to 25 mg once 200 mg once 159 mg/d (447) 13 12/5/2013 Beta Blockers titration problem solving Beta Blocker Therapy Hypotension Temporarily reduce vasodilators therapy If hypotension persist decrease BB dose Fluid Retention Temporarily increase diuretic dose If fluid retension persist decrease BB dose Bradycardia Reduce bb dose to the highest tolerated dose If bradycardia persist discontinue BB Beta Blockers in Heart Flaiure Stopping/Holding Beta Blockers : BB should not be stopped abruptly: • Taper over 1-2 weeks. • If exacerbation of HF, may continue with or decrease BB dose by half if not responsive to increasing diuretics dose. • COPD is not a contraindication of cardioselective Betablockers . 14 12/5/2013 Diuretics in Heart Failure Diuretics are used to control fluid overload but the goal is to use the minimum effective dose : • By using the minimum effective diuretic dose, it is more likely that symptomatic hypotension and unacceptable increases in Cr with ACE-I or BB can be avoided • Effective diuretic dose reduction is more often achieved after ACEIs and BB reach target doses. Diuretics in Heart failure Usual Starting Dose Maximum Total Daily Dose Duration Frusemide 20-40 mg daily or BID 600 mg 6-8 hours Bumetinide 0.5-1 mg daily or BID 10 mg 4-6 hours Ethacrynic acid 25-50 mg daily or BID 400 mg 6-8 hours 2.5 mg daily 20 mg 12-24 hours 25 mg daily or BID 200 mg 6-12 hours K+-depleting diuretics Metalazone Hydrochlorothiazide 15 12/5/2013 Aldosterone Antagonists in Heart Failure • Use in stage II-IV HF and EF <30% • Monitir K+: • Q 4-wks x3 , then • Q 12-wks x3, then • Q 6 -monthly • Stop the therapy if: • Renal insufficiency serum creatinine > 2.5 mg/dL in men or > 2.0 mg/dL in women (or estimated glomerular filtration rate <30 mL/min/1.73m2), • Potassium above 5.0 mEq/L. Drug Initial Daily Dose(s) Maximum Doses(s) Mean Doses Achieved in Clinical Trials Aldosterone Antagonists Spironolactone Eplerenone 12.5 to 25 mg once 25 mg once 25 mg once or twice 50 mg once 26 mg/d (424) 42.6 mg/d (445) Direct-acting Vasodilators in Heart Failure • • • Hydralazine and nitrates in combination are effective at reducing afterload and preload with a mortality benefit May have greater benefit in patients of African-American descent Beneficial Subsets for ACE-I intolerant patients Drug Initial Daily Dose(s) Maximum Doses(s) Hydralazine & Isosorbide Dinitrate 37.5 mg hydralazine/ Fixed dose 75 mg hydralazine/ 20 mg isosorbide combination 40 mg isosorbide dinitrate 3 times (423) dinitrate 3 times daily daily Hydralazine and Hydralazine: 25 to 50 Hydralazine: 300 mg isosorbide mg, 3 or 4 times daily in divided doses dinitrate (448) daily and isorsorbide and isosorbide dinitrate: dinitrate 120 mg daily 20 to 30 mg in divided doses 3 or 4 times daily Mean Doses Achieved in Clinical Trials ~175 mg hydralazine/90 mg isosorbide dinitrate daily --------- 16 12/5/2013 Digoxin in Heart Failure Is useful as add-on therapy for HF symptoms especially if EF<30% despite optimal dose of ACEI & BB • Useful For symptom relief , • Shortening hospital length of stay, • and increased exercise tolerance. • Useful in HF patients who also have atrial fibrillation. Digoxin target level in HF: Between 0.6-1.3 nmol/L. Routine levels not recommended in HF Heart Failure Medication Titration Problem Solving • Hypotension • Worsening Renal Function 17 12/5/2013 Heart Failure Medication Titration Problem Solving Hypotension Asymptomatic low BP Symptomatic low BP Doesn't require any change in therapy If no symptoms of congestion ,reduce diuretic. If dizzy, confusion or falls : • Reassess CCBs, diuretics, ISDN/hydralazine • Consider separating the dosing of ACEI and BB . • Take ACEIs and BB with food. Worsening Renal Function • A rise in SCr of ≤30% above baseline is acceptable . • A potassium of ≤ 5.6 is acceptable . • Assess for non-essential vasodilators and k+ supplements/diet/ retaining agents (e.g. ARBs, spironolactone) . • Should receive standard therapy with an ACE-I , ARB or spironolactone. • Use digoxin with extreme caution. • Reduce the ACEI , ARBs and dose by half if necessary . 18 12/5/2013 Worsening Renal Function •If Cr increases by > 30% : • Evaluate the patient's volume status • if volume depleted : Consider reducing \holding diuretic before reducing ACEI, ARB, spironolactone or BB. • Referral to a nephrologist is encouraged when there is kidney impairment as defined by a Cr increase by > 30% and eGFR < 30 mL\min . Drugs That Adversely Affect Clinical Status of Heart Failure • The ACC/AHA guidelines advise to avoid: • NSAIDs can cause sodium retention and peripheral vasoconstriction and can attenuate the efficacy and enhance the toxicity of diuretics and ACEIs. • Antiarrhythmic agents can have cardiodepressant effects and may promote arrhythmia; only amiodarone and dofetilide have been shown not to adversely affect survival. • Calcium channel blockers (verapamil and diltiazem) can worsen heart failure and may increase the risk of cardiovascular events. 19 12/5/2013 Data from Prince Sultan Cardiac Center Heart Failure Clinic, 2013 Data from PSCC Heart Failure Clinic, 2013 20 12/5/2013 Data from PSCC Heart Failure Clinic, 2013 72 patients ages 30-60 years 13 Patients < 29 years old 15 Patients > 60 years old Data from PSCC Heart Failure Clinic, 2013 60% EF < 30 % 35% EF 30-40 % 5% EF > 40 % 21 12/5/2013 Data from PSCC Heart Failure Clinic, 2013 Data from PSCC Heart Failure Clinic, 2013 Serum Creatinine <100 Mmol/L >200Mmol/L 65% 101-150 Mmol/L 151-200 MMol/L ESRD NA 21% 4% 4% 3% 3% 22 12/5/2013 Data from PSCC Heart Failure Clinic, 2013 ACEIor.ARBs.agent * Sr.Potassium Crosstabulation Sr.Potassium <4 4.1-5.4 >= 5.5 NA Total Fosinopril 1 7 0 1 9 Perindopril 11 27 0 1 39 Captopril 1 0 0 1 2 Enalapril 2 9 1 0 12 Valsartan 3 10 0 0 13 Candesartan 5 9 0 1 15 Irbesartan 1 0 0 0 1 NONE 4 2 3 0 9 Total 28 64 4 4 100 Data from PSCC Heart Failure Clinic, 2013 ACEI / ARBs and serum Potassium 45 40 35 30 25 20 15 10 5 0 NA >=>= 5.5 5.5 4.1- 4.5 4.1-5.4 < 4> 4 23 12/5/2013 Data from PSCC Heart Failure Clinic, 2013 On Beta Blockers maximum doses Yes No 30% 24% 76% 22% 12% 8% 21% 1% Bisorprolol Metoprolol TOTAL Carvedilol Data from PSCC Heart Failure Clinic, 2013 On ACEI or ARBs maximum doses No 2% 12% 12% 13% Valsartan Enalapril Captopril Perindopril Fosinopril 1% ACEIor.ARBs.agent 11% 1% 4% 72% 19% Irbesartan 26% 9% Candesartan Yes Total 24 12/5/2013 Data from PSCC Heart Failure Clinic, 2013 Patients on Vasodilators 8% Yes No 92% Data from PSCC Heart Failure Clinic, 2013 25 12/5/2013 Data from PSCC Heart Failure Clinic, 2013 Pt on BB plus ACEI or ARBs plus Aldactone 29% Yes 29% 71% No 71% Conclusion • The goals of therapy for all heart failure patients are to: – – – – Abolishing the symptoms, Avoid complications, arrhythmia, Improve quality of life , and prolong survival . • Clinical trials evidence indicated a relationship between the degree of reduction in HF symptoms and the dose of drug given. • Larger doses are more likely to improve the patients quality of life and reduce the incidence of hospital stay, but the impact of larger doses on mortality is less clear. 26 12/5/2013 27