* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download SMOOTH SURFACE
Survey
Document related concepts
Transcript
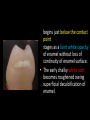
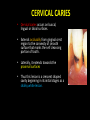
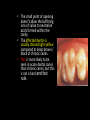
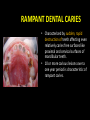
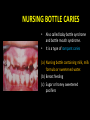
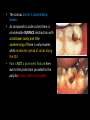
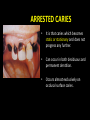
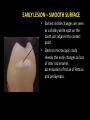
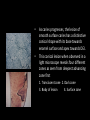
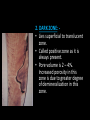
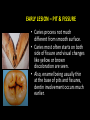
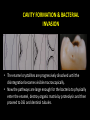
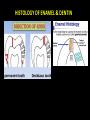
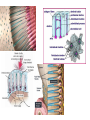
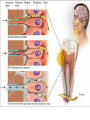
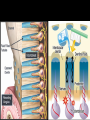
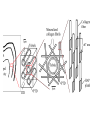
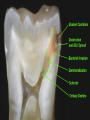
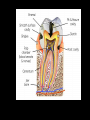
classification of caries SMOOTH SURFACE CARIES • Develops on proximal surfaces of all teeth or on gingival 1/3rd of buccal and lingual surfaces. • Here, the caries is preceded by retention of carbohydrate and bacteria on tooth surfaces, leading to subsequent acid demineralization of enamel. • Smooth surface caries usually begins just below the contact point and appears in initial stages as a faint white opacity of enamel without loss of continuity of enamel surface. • The early chalky white spot becomes roughened owing to superficial decalcification of enamel. • As caries reaches the DEJ, there is rapid lateral spread. • Quite often, caries extends buccally and lingually but not till the actual buccal and lingual surfaces, as these areas are more accessible to the toothbrush. CERVICAL CARIES • Cervical caries occurs on buccal, lingual or labial surfaces. • Extends occlusally from gingival crest region to the convexity of smooth surface that marks the self cleansing portion of tooth. • Laterally, it extends towards the proximal surfaces. • Thus this lesion is a crescent shaped cavity beginning in its initial stages as a chalky white lesion. CERVICAL CARIES • It almost always occurs as an open cavity unlike the smooth surface or pit and fissure caries. • Occurs on all the teeth without predilection as it is directly related to lack of oral hygiene. • No excuse for it to occur on anybody’s teeth since it can always be prevented by maintaining good oral hygiene. ACUTE DENTAL CARIES • It is that form of caries that follows a rapid clinical course and results in early pulpal involvement by carious process. • Predominantly affects children and young adults probably because their dentinal tubules are larger and show no sclerosis. • The point of entry of caries is small even though there is rapid spread of caries at DEJ, producing large internal cavitation. • The small point of opening doesn’t allow the buffering ions of saliva to neutralize acids formed within the cavity. • The affected dentin is usually stained light yellow compared to deep brown / black of chronic caries. • Pain is more likely to be seen in acute dental caries than chronic caries, but this is not a hard and fast rule. RAMPANT DENTAL CARIES • Characterized by sudden, rapid destruction of teeth affecting even relatively caries free surfaces like proximal and cervical surfaces of mandibular teeth. • 10 or more carious lesions over a one year period is characteristic of rampant caries. • Prominently observed in deciduous dentition of young children and permanent dentition of teenagers. • Dietary factors like high carbohydrate intake etc as well as physiological factors affecting saliva are major contributors to etiology of rampant caries. NURSING BOTTLE CARIES • Also called baby bottle syndrome and bottle mouth syndrome. • It is a type of rampant caries and occurs due to – (a) Nursing bottle containing milk, milk formula or sweetened water. (b) Breast feeding (c) Sugar or honey sweetened pacifiers • Usually, the above aids are used at sleeping time after one year of age. • Clinically seen as widespread caries of the 4 maxillary incisors followed by 1st molars and then canines. • Absence of caries in mandibular teeth distinguishes it from ordinary rampant caries. • If milk or other carbohydrates are rapidly cleared from mouth, they aren’t cariogenic, but if they pool in the mouth, then they can cause rampant caries. • Mandibular teeth usually escape the process as the pooled milk or sweet products are washed away by saliva CHRONIC DENTAL CARIES • That type of caries which progresses slowly and involves the pulp much later than acute caries. • Most commonly seen in adults. • Opening to the lesion is invariably larger than that of acute caries. As a result, there is lesser food impaction and greater access to saliva. • Also, the slow progress of caries allows enough time for dentinal sclerosis and deposition of tertiary dentin in response to irritation. • The carious dentin is stained deep brown • As compared to acute caries there is considerable SURFACE destruction with a shallower cavity and little undermining of there is only enamel, while moderate spread of caries along the DEJ. • Pain is NOT a prominent feature here due to the protection provided to the pulp by tertiary dentin formation. RECURRENT CARIES • Occurs around or beneath an existing restoration. • Usually due to inadequate extension of restoration resulting in food impaction • Can also occur if a restorative material is not properly adapted to margins of cavity leading to leaky cavity margins. • This “renewed” carious process follows a similar pattern as that of primary caries. ARRESTED CARIES • It is that caries which becomes static or stationary and does not progress any further. • Can occur in both deciduous and permanent dentition. • Occurs almost exclusively on occlusal surface caries. • • • • Characterized by large, open cavity in which there is no food retention and the softened decalcified dentin is gradually burnished until it assumes a brown polished appearance. Called “Eburnation of dentin”. Sometimes arrest can also occur in initial proximal caries, when the adjacent tooth is extracted for some reason. This is due to the automatic creation of a self cleansing area RADIATION CARIES • Rampant caries occurring in patients receiving radiotherapy in head & neck region is called as RADIATION CARIES. • Xerostomia (dry mouth )is a major complication of radiotherapy of head & neck region. This, coupled with increase in viscosity and low pH of saliva results in decreased anticariogenic actions of saliva. HISTOPATHOLOGY OF CARIES HISTOPATHOLOGY OF CARIES - ENAMEL • Caries process in enamel progresses through following stages A. Early submicroscopic lesion B. Phase of nonbacterial enamel crystal destruction C. Cavity formation D. Bacterial invasion of enamel * C & D Occur almost simultaneously EARLY LESION – SMOOTH SURFACE • Earliest visible changes are seen as a chalky white spot on the tooth just adjacent to contact point. • Electron microscopic study reveals the early changes as loss of inter rod enamel, accentuation of striae of Retzius and perikymata. • • As caries progresses, the lesion of smooth surface caries has a distinctive conical shape with its base towards enamel surface and apex towards DEJ. This conical lesion when observed in a light microscope reveals four different zones as seen from deepest advancing zone first 1. Translucent zone 2. Dark zone 3. Body of lesion 4. Surface zone 1.TRANSLUCENT ZONE: • Unrecognizable clinically & radiologically. • Occurs due to formation of submicroscopic pores at enamel rod boundaries and striae of Retzius. • This zone is slightly more porous than sound enamel having a pore volume of 1% compared to 0.1% of sound enamel. 2. DARK ZONE: • Lies superficial to translucent zone. • Called positive zone as it is always present. • Pore volume is 2 – 4%. Increased porosity in this zone is due to greater degree of demineralization in this zone. 3. BODY OF LESION: • Forms bulk of the lesion and lies between relatively unaffected surface zone and dark zone. • Area of greatest demineralization, having a pore volume of 5% near the periphery to about 25% in the center of body of lesion. 4. SURFACE ZONE: • Interestingly, this zone not only remains intact during the early stages of attack by caries, but also REMAINS MORE HEAVILY MINERALIZED. • Pore volume of only 1%. • Ions for remineralization come either from those within plaque or from reprecipitation of calcium and phosphate ions diffusing outwards as deeper layers are demineralized. • Eventually, this zone is demineralized by the time caries penetrates dentin. EARLY LESION – PIT & FISSURE • Caries process not much different from smooth surface. • Caries most often starts on both side of fissure and visual changes like yellow or brown discoloration are seen. • Also, enamel being usually thin at the base of pits and fissures, dentin involvement occurs much earlier. • In contrast to smooth surface caries’ lesion, the caries here follows direction of enamel rods, forming a cone shaped lesion with its base towards DEJ and apex directed occlusally. • As a result therefore, greater number of dentinal tubules are affected when lesion reaches DEJ. CAVITY FORMATION & BACTERIAL INVASION • The enamel crystallites are progressively dissolved until the disintegration becomes visible macroscopically. • Now the pathways are large enough for the bacteria to physically enter the enamel, destroy organic matrix by proteolysis and then proceed to DEJ and dentinal tubules. HISTOLOGY OF ENAMEL & DENTIN HISTOPATHOLOGY OF CARIES – DENTIN (EARLY CHANGES) • The initial (non infected) lesion in dentin forms beneath enamel before any cavity has formed. • Even though acids formed from fermentation of carbohydrate substrate diffuse into dentin, they leave the organic matrix intact. • Once bacteria penetrate enamel, they spread laterally along DEJ and attack dentin over a wide area. • The infected lesion of dentin is helped in its course by the presence of tubules within dentin which provide an easy pathway to the bacteria. • Bacteria now liberate proteolytic enzymes and bring about destruction of organic matrix of dentin which is already softened by demineralization. • The first change to occur in the caries process within dentin is fatty degeneration of the tome’s fibers, with deposition of lipid globules within these fibers. • This is then followed by dentinal sclerosis, which is minimal in rapidly advancing acute caries and maximum in slow, chronic caries. • This is considered as a protective measure by dentinal tubules to seal off the invading bacteria. • In spite of all these attempts to prevent spread of caries process, dentin is continually destroyed. • Thus behind the zone of dentinal sclerosis a narrow zone of decalcification is seen, just ahead of bacterial invasion of dentinal tubules. • At this stage, only a few tubules are invaded even before clinical evidence of caries. • These bacteria are called “Pioneer bacteria”. HISTOPATHOLOGY OF CARIES – DENTIN (ADNANCED CHANGES) • Continued decalcification of dentinal tubules leads to their confluence, although the structure of organic matrix may still be maintained for some time. • Confluence of tubules occurs due to packing of the tubules with the invading bacteria. • The coalescence and breakdown of adjacent dentinal tubules leads to formation of “Miller’s liquefaction foci”. • It is an ovoid area of destruction of tubules parallel to the course of tubules and is packed with necrotic debris derived from destruction of tubules. • Continued dentinal destruction by decalcification followed by proteolysis occurs at many focal areas which ultimately coalesce to form a necrotic leathery mass of dentin. • In this mass, clefts occur at right angles to tubules and parallel to the course of lateral branches of tubules or along the collagen fibers of organic matrix. • Due to these clefts, carious dentin can be peeled away in thin layers by hand instruments. ZONES OF DENTINAL CARIES 5 4 3 2 1 • Observing from the pulpal side at the advancing edge of carious lesion following different zones can be seen – ZONE 1 – Zone of fatty degeneration of Tomes’ fibers ZONE 2 – Zone of dentinal sclerosis ZONE 3 – Zone of decalcification ZONE 4 – Zone of bacterial invasion ZONE 5 – Zone of decomposed dentin