* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download atrial fibrillation
Survey
Document related concepts
Transcript
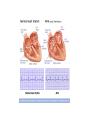
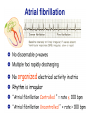
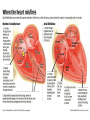
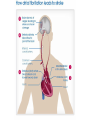
ATRIAL FIBRILLATION PHCP 403 Samirah Abdu-Aguye INTRODUCTION • Atrial fibrillation is the most common sustained cardiac arrhythmia • Occurs in 1-2% of the population in the developed world • Prevalence increases with age • It may occur in isolation or secondary to structural heart disease, hypertension, myocardial ischemia and infarction, hyperthyroidism, obesity and sleep apnea INTRO CONT’D • AF can be asymptomatic or symptomatic • Signs & Symptoms may include palpitations, dizziness, dyspnea, angina and worsening heart failure INTRO CONT’D • Its management depends on the assessment of thromboembolic risk and control of symptoms • In general, a decision is made to pursue either a rhythm or rate control strategy. • With rhythm control the aim is to maintain the patient in sinus rhythm, while with rate control the aim is to control the ventricular rate with medication TYPES Atrial fibrillation may be categorized according to its presentation and duration (paroxysmal, persistent and permanent/chronic ) • Paroxysmal: sudden onset, reverts in 24-48hrs • Persistent: abrupt onset and persists for > 7 days • Permanent/ chronic: patient is unable to return to sinus rhythm ASSESSING STROKE RISK • Systemic thromboembolism, leading to stroke, transient ischemic attacks or embolization to other sites, is the most dreaded complication of AF. • AF is believed to be responsible for up to 40% of all strokes • Anticoagulant therapy reduces this risk. CONT’D • The decision to use anticoagulant or antiplatelet therapy is dictated by the patient's risk of these events • The CHADS2 and CHA2DS2-VASc scores have been commonly used to stratify risk • A score of 1 or more is generally taken to indicate a risk of thromboembolism which may warrant anticoagulant therapy CHADS2 SCORE CHADS2 score: stratifying risk of stroke in patients with atrial fibrillation • Congestive heart failure 1 point • Hypertension 1 point • Age ≥ 75 years 1 point • Diabetes 1 point • Systemic embolism, including Stroke, 2 points (previous episode) CHA2DS2 VaSC SCORE Risk factor Score • Congestive heart failure or left ventricular dysfunction 1 • Hypertension 1 • Age 75 years or older 2 • Diabetes mellitus 1 • Stroke or transient ischemic attack history 2 • Vascular disease (prior myocardial infarction, peripheral artery disease, aortic plaque) 1 • Age 65–74 1 • Sex category (female gender) 1 CHADS2 SCORE 0 Use CHA2DS VaSC SCORE ≥1 Monitor regularly Use anticoagulants TREATMENT OF AF 1. Rhythm control(Conversion to sinus rhythm) -DC shock/ cardioversion -Medication 2. Rate control(Control ventricular rate) -Medication 3. Prevent thromboembolism -Use of anticoagulants Proposed management of nonvalvular AF Anticoagulants • Warfarin used to be the drug of choice for anticoagulation • MOA? • Requires regular INR monitoring, has unpredictable rxkinetics, various interactions and carries a risk of bleeding especially ICH • Newer agents that can be used instead are dabigatran, apixaban and rivaroxaban HASBLED TOOL • • • • • • • HASBLED score Hypertension Abnormal liver or kidney function, Stroke Bleeding Labile INRs Elderly (e.g. >65 years) Drugs or alcohol 1 point 1 point each 1 point 1 point 1 point 1 points 1 point each *Hypertension = systolic blood pressure >160 mmHg *Abnormal renal function = dialysis/renal transplantation/serum creatinine ≥200 mmol/L *Abnormal liver function = chronic hepatic dysfunction (e.g. cirrhosis) or biochemical evidence of significant hepatic derangement (e.g. bilirubin 2 x upper limit of normal in association with aspartate aminotransferase/alanine aminotransferase/alkaline phosphatase 3 x upper limit normal etc.) *Bleeding = history of bleeding or a bleeding diathesis *Drugs = concomitant use of antiplatelet or non-steroidal anti-inflammatory drugs Problems with anti-arrhythmic drugs • Extensive side effects- Pro-arrhythmic, increase mortality • Drug and disease interactions • Negative inotropes except amiodarone and digoxin Rate control Vs. Rhythm Control • No difference, both treatments are equivalent to each other Rate control • Most patients with atrial fibrillation are managed by controlling the ventricular rate • The ventricular rate may be controlled using beta blockers( 1st line), non-dihydropyridine calcium channel blockers (for example verapamil) or digoxin. • Target heart rate is less than 110 beats/min • Anticoagulation should be continued in these patients Rhythm control • In severely symptomatic patients it may be reasonable to attempt to restore sinus rhythm. • Patients who present within 48 hours of the onset of AF, immediate cardioversion (electrical or drug) may be attempted. RHYTHM CONTROL CONT’D DC Cardioversion - Requires anesthesia - Maintainance of sinus rhythm is variable • ≤ 48 hrs of onset best outcome • Appropriate anti-coagulation • Usually requires drug therapy to maintain sinus rhythm e.g. beta blockers, flecainide and amiodarone RHYTHM CONTROL CONT’D Pharmacological Simpler, but less effective than DC cardioversion • Acutely if < 48 hours - 1st line: Flecainide - 2nd line: Amiodarone • Anticoagulation is needed • May also require long term drug therapy for maintenance Practice Question • Mr John Jones (61 years) is admitted to the emergency assessment unit at his local hospital complaining of palpitations, breathlessness and dizziness. • He has a 5-day history of some dizziness and palpitations. In the last 24 hours he complained additionally of shortness of breath. He collapsed at home and was then admitted to hospital via the emergency department. • He experienced similar symptoms two months ago but did not seek medical advice at that time and seemed to recover quickly. On examination and review by the admitting doctor the following information is obtained: Previous medical history • Hypertension (diagnosed 5 years ago), no previous history of cardiovascular disease. • The patient is a regular cigarette smoker (>20 per day) and drinks approximately 20 units of alcohol per week. Drug history • No known allergies. • Mr Jones had been prescribed lisinopril tablets 20 mg once daily but was poorly compliant with treatment. Signs and symptoms on examination • Blood pressure 100/70 mmHg • Heart rate 175 bpm, irregular • Respiratory rate 25 breaths per minute • No basal crackles in the lungs. Diagnosis • Atrial fibrillation. Relevant test results • Full blood counts, liver function tests, electrolytes and renal function were all normal at admission and throughout the admission to discharge • Mr Jones is subsequently transferred to the cardiology ward where his continuing atrial fibrillation is later confirmed as persistent atrial fibrillation. Questions 1. What is this patients CHADS Score? What does it mean for him? 2. What are the most common signs and symptoms exhibited by patients with atrial fibrillation? Indicate which of these signs and symptoms the patient is exhibiting 3 What are the two options in terms of treatment strategy that may be employed to manage atrial fibrillation? Indicate what would be the most appropriate strategy that you could recommend to the doctor managing this patient and why you think this is the case. 4 Assuming a rate control strategy is to be used what class of drug should be the firstline treatment for this patient? If the first-line drug was contraindicated what class of drug could be used as alternative treatment? 5 What patient parameters should be monitored to assess therapy with the usual firstline treatment and what is an appropriate treatment target for such parameters? 6 Suggest 2 drugs that can be used as anticoagulants in this patient 7 Assuming the patient is to be discharged on warfarin, what counselling does the patient require? REFERENCES • Samardhi H, Santos M, Denman R, Walters D, Bett N. Current management of atrial fibrillation. Australian Prescriber [Internet]. 2011 [cited 21 February 2015];(Volume 34, Issue 4):100-103. Available from: http://www.australianprescriber.com/magazin e/34/4/article/1204.pdf • Munns A. Atrial Fibrillation Introduction. Lecture presented at; 2011; University of Queensland. • NPS Medicinewise. Good anti-coagulant practice. Internet: http://www.nps.org.au/publications/healthprofessional/medicinewise-news/2013/goodanticoagulant-practice#References; 2013.