* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Comparison of the Circulating Metabolite Profile of PF
Survey
Document related concepts
Transcript
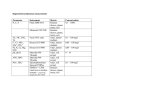
Supplemental material to this article can be found at: http://dmd.aspetjournals.org/content/suppl/2014/11/10/dmd.114.061218.DC1 1521-009X/43/2/190–198$25.00 DRUG METABOLISM AND DISPOSITION Copyright ª 2014 by The American Society for Pharmacology and Experimental Therapeutics http://dx.doi.org/10.1124/dmd.114.061218 Drug Metab Dispos 43:190–198, February 2015 Comparison of the Circulating Metabolite Profile of PF-04991532, a Hepatoselective Glucokinase Activator, Across Preclinical Species and Humans: Potential Implications in Metabolites in Safety Testing Assessment s Raman Sharma, John Litchfield, Arthur Bergman, Karen Atkinson, David Kazierad, Stephanie M. Gustavson, Li Di, Jeffrey A. Pfefferkorn, and Amit S. Kalgutkar Pfizer Inc., Groton, Connecticut (R.S., A.B., K.A., S.M.G., L.D.); and Pfizer Inc., Cambridge, Massachusetts (J.L., D.K., J.A.P., A.S.K.) Received November 7, 2014; accepted November 10, 2014 ABSTRACT [14C]PF-04991532 was attributed to an unchanged parent (>70% in rats and dogs). In contrast with the human circulatory metabolite profile, the monohydroxylated metabolites were not detected in circulation in either rats or dogs. Available mass spectral evidence suggested that M2a and M2b/M2c were diastereomers derived from cyclopentyl ring oxidation in PF-04991532. Because cyclopentyl ring hydroxylation on the C-2 and C-3 positions can generate eight possible diastereomers, it was possible that additional diastereomers may have also formed and would need to be resolved from the M2a and M2b/M2c peaks observed in the current chromatography conditions. In conclusion, the human metabolite scouting study in tandem with the animal mass balance study allowed early identification of PF-04991532 oxidative metabolites, which were not predicted by in vitro methods and may require additional scrutiny in the development phase of PF-04991532. Introduction pancreas, which resulted in increased insulin secretion at inappropriately low glucose levels (Grimsby et al., 2003; Coghlan and Leighton, 2008; Haynes et al., 2010; Meininger et al., 2011; Sarabu et al., 2012; Pfefferkorn, 2013). To mitigate this hypoglycemia risk, several approaches have been reported to limit GK activation to the liver (Pfefferkorn, 2013). PF-04991532 was designed to have low passive permeability, thereby minimizing distribution into extrahepatic tissues, particularly the pancreas (Ghosh et al., 2014). Concurrently, PF-04991532 was also optimized as a substrate for active liver uptake via liver-specific organic anion transporting polypeptide isoforms. In preclinical animal models of diabetes, PF-04991532 was found to robustly lower fasting and postprandial glucose and was devoid of hypoglycemic risks, leading to its selection as a clinical candidate for treating T2DM. The in vivo pharmacokinetics of PF-04991532 were characterized by high systemic plasma clearance (CLp) values of 51 and 35 ml/min per kg in rats and dogs, respectively, and oral bioavailability of ;18% in both rats and dogs (Pfefferkorn et al., 2012). Resistance of PF-04991532 to metabolic turnover in liver microsomes and hepatocytes from a rat, dog, and human suggested that metabolic elimination would be Our laboratory recently identified a glucokinase (GK) activator, PF-04991532 [(S)-6-(3-cyclopentyl-2-(4-trifluoromethyl)-1H-imidazol1-yl)propanamido)nicotinic acid] (Fig. 1), with preferential GK activation in hepatocytes versus pancreatic b-cells (Pfefferkorn et al., 2012). GK is a glycolytic enzyme that catalyzes the phosphorylation of glucose to glucose-6-phosphate (Mithieux, 1996). GK acts as a glucostat in the b-cells of the pancreas, establishing the threshold for glucose-stimulated insulin secretion (Matschinsky et al., 1998). In the liver, GK is involved in the regulation of hepatic glucose utilization and output (Matschinsky and Ellerman, 1968). The therapeutic benefits of GK activators in the treatment of type 2 diabetes mellitus (T2DM) have been reviewed (Matschinsky et al., 2011; Sarabu et al., 2011). Early clinical experience with GK activators indicated significant improvements in glycemic control but with an increased risk of hypoglycemia due to excessive GK activation in the dx.doi.org/10.1124/dmd.114.061218. s This article has supplemental material available at dmd.aspetjournals.org. ABBREVIATIONS: AUC, area under the plasma concentration time curve; CID, collision-induced dissociation; GK, glucokinase; HPLC, highperformance liquid chromatography; LC-MS/MS, liquid chromatography–tandem mass spectrometry; MAD, multiple ascending dose; MH+, protonated molecular ion; MRP, multidrug resistant protein; NOAEL, no observed adverse effect level; PF-04991532, (S)-6-(3-cyclopentyl-2-(4trifluoromethyl)-1H-imidazol-1-yl)propanamido)nicotinic acid; T2DM, type 2 diabetes mellitus; UPLC, ultra-performance liquid chromatography. 190 Downloaded from dmd.aspetjournals.org at ASPET Journals on May 7, 2017 A previous report from our laboratory disclosed the identification of PF-04991532 [(S)-6-(3-cyclopentyl-2-(4-trifluoromethyl)-1H-imidazol1-yl)propanamido)nicotinic acid] as a hepatoselective glucokinase activator for the treatment of type 2 diabetes mellitus. Lack of in vitro metabolic turnover in microsomes and hepatocytes from preclinical species and humans suggested that metabolism would be inconsequential as a clearance mechanism of PF-04991532 in vivo. Qualitative examination of human circulating metabolites using plasma samples from a 14-day multiple ascending dose clinical study, however, revealed a glucuronide (M1) and monohydroxylation products (M2a and M2b/M2c) whose abundances (based on UV integration) were greater than 10% of the total drug-related material. Based on this preliminary observation, mass balance/excretion studies were triggered in animals, which revealed that the majority of circulating radioactivity following the oral administration of Circulating Metabolites of PF-04991532 Fig. 1. Structure of hepatoselective glucokinase activator PF-04991532. Materials and Methods General Chemicals. Commercially obtained chemicals and solvents were of high-performance liquid chromatography (HPLC) or analytic grade. [14C]PF04991532 (specific activity, 0.25 mCi/mg) was synthesized by the radiochemistry group at Pfizer Worldwide Research and Development (Groton, CT). It had a radiochemical purity of . 99%, as determined by HPLC using an in-line radioactivity detector. The location of the 14C label on the nicotinic acid motif is illustrated in Fig. 1. 6-Aminonicotinic acid was purchased from SigmaAldrich (St. Louis, MO). A cryopreserved Sprague-Dawley rat (male, pool of 12 donors), beagle dog (male, pool of five donors), and human (pool of 10 donors of mixed gender) were purchased from Celsis (Chicago, IL). Metabolite Scouting Study in Humans. The study was conducted in compliance with the International Conference on Harmonization Good Clinical Practices guidelines, the ethical principles that have their origin in the Declaration of Helsinki, and the US Food and Drug Administration regulations for informed consent and protection of subject rights. The clinical study design with PF-04991532 incorporated a randomized, placebo group, MAD study in which subjects with T2DM on background metformin therapy received either placebo or oral doses of PF-04991532 (30–900 mg) administered once daily for 14 days with food (Gustavson et al., 2013). Venous blood samples from each subject predose (10 ml) and at 2.0, 6.0, and 12 hours postdose (2 ml/time point) on days 1 and 14 were used for metabolite scouting efforts. Blood samples were collected in heparinized tubes. Within 30 minutes after collection, the blood samples were centrifuged at approximately 1700g for ;10 minutes at 4C to generate plasma. Citric acid monohydrate (500 mg/ml) was added to the plasma samples to create a plasma:citric acid (92:8, w/v) mixture. The final concentration of citric acid monohydrate in the sample was 40 mg/ml. All samples were stored at or below 220C until analysis. Samples from the highest dose group (900 mg) in the multiple dose study were used for metabolite scouting. Plasma from each of the nine subjects (five male/four female, 45–65 years of age) that received PF-04991532 (900 mg) was pooled individually according to the Hamilton method (Hamilton et al., 1981). An equal volume of 0.3 ml from each individual patient pool was then combined to make a multisubject pool. This was done for both day 1 and day 14 samples, resulting in two 2.7-ml multisubject pools. Additionally, 0.3 ml from the t = 0 time point for each subject was pooled to make a 2.7-ml predose pool. Each pool was diluted with 12 ml of ice-cold acetonitrile (containing 0.1% formic acid) and sonicated for 5 minutes. The samples were then centrifuged (2000g) for 10 minutes. The supernatants were transferred to clean test tubes and evaporated to dryness in vacuo. The dried residue was then reconstituted in 300 ml of the mobile phase (10% acetonitrile, 0.1% formic acid), and an aliquot (50 ml) was injected on a liquid chromatography–tandem mass spectrometry (LC-MS/MS) system. Metabolite Identification in Hepatocytes. Stock solutions of unlabeled PF-04991532 were prepared in 10% dimethyl sulfoxide and 90% acetonitrile. The final concentration of dimethyl sulfoxide and acetonitrile in the incubation mixtures were 0.1 and 0.9%, respectively. Williams E media was prepared by adding 26 mM sodium carbonate and 50 mM HEPES, followed by 0.2-mm filtration and then 30 min of CO2 bubbling at 37C. This media was used for thawing and suspension of hepatocytes. Upon thawing, the pooled cryopreserved hepatocytes were resuspended in Williams E medium (WEM GIBCOBRL, custom formula #91-5233EC; Life Technologies, Grand Island, NY) supplemented with 50 mM HEPES and 26 mM Na2CO3. The cells were counted using the Trypan Blue exclusion method, and a 24-well hepatocyte plate containing 0.5 million cells/ml was treated with PF-04991532 (final concentration in 1.0-ml incubation = 10 mM) and incubated at 37C for 4 hours, 75% relative humidity, 5% CO2, and 95% O2. Incubations were terminated by the addition of ice-cold acetonitrile (4 ml) and centrifuged (3000g, 15 minutes). The supernatants were dried under a steady stream of nitrogen, reconstituted with 25% aqueous acetonitrile (250 ml), and analyzed via LC-MS/MS for metabolite formation. For metabolite identification via the relay method, the hepatocyte plate was incubated at 37C with 95% O2/5% CO2, 75% relative humidity for 4 hours daily for 5 days. At time t = 0, an aliquot of the hepatocyte incubation (suspension) was quenched with 2 volume of acetonitrile and frozen at 280C for liquid chromatography–mass spectrometry analysis. At 4, 8, 12, 16, and 20 hours, the hepatocyte incubation suspension plate was centrifuged (3000g, 10 minutes, room temperature) and 300-ml supernatant was transferred to a clean 24-well plate and stored at 280C until the next relay experiment. The remaining hepatocyte pellet in the incubation plate was quenched with 2 volume of acetonitrile and frozen at 280C for LC/MS analysis. For the second relay experiment, the supernatant plate was warmed to 37C for 30 minutes, and hepatocytes were added to the samples to give a final cell density of 0.5 million cells/ml. The plates were incubated at 37C for 4 hours, sampled, and processed as described above. Five relays were performed to give a total incubation time of 20 hours. Animals, Dosing, and Sample Collection. Animal care and in vivo procedures were conducted according to the guidelines of the Pfizer Animal Care and Use Committee. The in-life portion of the studies was conducted at Covance Laboratories Inc. (Madison, WI) in accordance with applicable standard operating procedures and the Wisconsin Department of Health Services Radiation Protection Section (License No. 025-1076-01). Jugular vein cannulated Sprague-Dawley rats (192–328 g) were purchased from Charles River Laboratories, Inc. (Wilmington, MA). Purebred beagle dogs (8.5–10.3 kg) were obtained from Ridglan Farms, Inc. (Mt. Horeb, WI). Animals were quarantined for a minimum of 3 days before treatment and maintained on a 12-hour light/dark cycle. The animals were fasted overnight before administration of [14C]PF-04991532 and fed 4 hours postdose. The animals were provided water ad libitum. The doses selected for the mass balance study reflected the no observed adverse effect level (NOAEL) in the respective preclinical species. Rat Study. A group of Sprague-Dawley rats (n = 3/gender) was administered a single 200-mg/kg oral dose of [ 14 C]PF-04991532 for the mass balance study. The dose was formulated as a suspension in 0.5% methylcellulose in reverse osmosis water on the day before dose administration. Each rat received an approximate dose of 40 mCi/200 g of radiolabeled Downloaded from dmd.aspetjournals.org at ASPET Journals on May 7, 2017 inconsequential as a clearance mechanism in vivo. Preliminary studies addressing the in vivo clearance mechanism in rats using unlabeled PF-04991532 revealed biliary (62%) and renal (11%) excretion of the unchanged parent as the principal elimination pathways (Pfefferkorn et al., 2012). At the time of candidate selection, it was presumed that PF-04991532 would be eliminated in an unchanged form via the hepatobiliary route involving active uptake by organic anion transporting polypeptide 1B3 into the liver, followed by biliary elimination through efflux transporters, as evident with related carboxylic acid drugs, such as fexofenadine (Matsushima et al., 2008). Contrary to our hypothesis, plasma samples from the clinical multiple ascending dose (MAD) studies on PF-04991532 revealed several metabolites in circulation whose abundance was greater than 10% of the total drug-related material and would potentially require further qualification in preclinical species as per the metabolites in safety testing guidance from the US Food and Drug Administration and the later published 2009 International Conference on Harmonisation guidance M3 (R2) (U.S. Food and Drug Administration, 2008; European Medicines Agency, 2009; International Conference on Harmonisation, 2012). Consequently, metabolism/excretion studies with [14C]PF-04991532 were triggered in Sprague-Dawley rats and beagle dogs to examine circulating and excretory metabolites in the preclinical toxicology species selected for PF-04991532 development. The collective findings from these studies are summarized herein. 191 192 Sharm et al. evaporative centrifuge (Genevac Inc., Valley Cottage, NY). The mean recovery of radioactivity after extraction was ;99%. The samples were reconstituted with 1 ml of 5 mM ammonium acetate (pH = 3.0):acetonitrile (95:5). An aliquot (;30 ml) was injected onto the HPLC system for analysis. Fecal homogenates were combined such that at least 95% of the radioactivity excreted in feces was represented. Pooled fecal samples were diluted with acetonitrile (3 ml/g homogenate) and sonicated (15 minutes). After centrifugation at 1700g for 10 minutes, the supernatant was transferred to a 100-ml Erlenmeyer flask, and the remaining residue was further extracted with acetonitrile (10 ml). The supernatants were combined, and the mean recovery of radioactivity after extraction was ;90–99% in all species. The supernatants were concentrated to dryness at 37C, and the residues were reconstituted in 500-ml 5 mM ammonium acetate (pH = 3.0):acetonitrile (95:5). Aliquots (;30 ml) were injected onto the HPLC system for analysis. Quantitative Assessment of Metabolites. Metabolite quantification from urine, feces, and plasma was performed by measuring the radioactivity fractions collected from HPLC effluent at 0.25-minute intervals using an FC 204 fraction collector (Gilson Inc., Middleton, WI). Fractions were collected in a 96-well microbeta plate and dried using the Genevac EZ-2 evaporative centrifuge (Genevac Inc.). Prior to counting, 175 ml of Ultima Gold liquid scintillatant (PerkinElmer Life and Analytical Sciences) was added to each well. Radioactivity was then counted using a Trilux 1450 microbeta counter (PerkinElmer Wallac, Gaithersburg, MD). Data were imported into Laura program version 3.1.1.39 (LabLogic System Ltd., Sheffield, UK) to provide an integrated peak representation in counts per minute and the percentage of total radioactivity comprised by each peak within the radiochromatogram. HPLC Analysis. The HPLC system consisted of an Acela quaternary solvent delivery pump, an Acela autoinjector, and a Surveyor PDA Plus photodiode array detector (Thermo Electron North America, West Palm Beach, FL). Chromatography was performed on a Phenomenex hydro RP column (4.6 150 mm, 5 m) with a mobile phase comprised of 5 mM ammonium formate, pH = 3.0 (solvent A), and acetonitrile (solvent B). For metabolic profiling with unlabeled PF-04991532, the mobile phase gradient was programmed in a linear fashion as follows: 95% solvent A (0–3 minutes), 40% solvent A (25 minutes), 20% solvent A (35 minutes), and 5% solvent A (38 min), followed by column reequilibration at 95% solvent A (38.01–49 minutes). For animal mass balance studies with [14C]PF-04991532, the mobile phase gradient was programmed in a linear fashion as follows: 95% solvent A (0–3 minutes), 70% solvent A (37 minutes), and 5% solvent A (43–49 minutes), followed by column reequilibration at 95% solvent A (49.01–56 minutes). A flow rate of 1.0 ml/min was maintained throughout the analysis. Approximately 5% of the postcolumn flow was split to the mass spectrometer. The remainder of the effluent was split to the FC 204 fraction collector or waste. LC-MS/MS. Identification of the metabolites in excreta, plasma, and hepatocytes (4-hour incubation with PF-04991532) was performed on a Thermo Orbitrap mass spectrometer operating in a positive ion electrospray mode. Xcalibur software version 2.0 was used to control the HPLC/MS system. The electrospray ionization tune settings were as follows: capillary temperature = 325C; sheath gas flow = 6 units; auxiliary gas flow = 5 units; sweep gas flow = 2 units; source voltage = 4 kV; source current = 100 uA; capillary voltage = 29 V; and tube lens = 90 V. Full scan data were collected at 15,000 resolution. Datadependent product ion scans of the two most intense ions found in the full scan were obtained at 15,000 resolution. The dynamic exclusion function was used with a 1-minute exclusion duration after three successive product ion scans, with early exclusion if the precursor ion fell below a signal-to-noise ratio of 20. Structural information was generated from the collision-induced dissociation (CID) spectra of the protonated molecular ions (MH+). Chromatographic separation of oxidative metabolites M2a, M2b, and M2c in hepatocyte incubations using the relay method was achieved using an ACQUITY ultra-performance liquid chromatography (UPLC) system (Waters Corporation, Milford, MA), with an ACQUITY UPLC BEH (Ethylene Bridged Hybrid) C18 column 1.7 mM, 2.1 150 mm, maintained at a column temperature of 40C. The mobile phase consisted of water with 0.1% formic acid (A) and acetonitrile (B). The flow rate was 0.35 ml/min, and the linear gradient was as follows: 5% solvent B (0–2 minutes), 35% solvent B (57 minutes), and 5% solvent B (58–59 minutes) followed by a column equilibration at starting mobile phase conditions for 5 minutes. The injection volume was 10 ml. Detection of PF-4991532 and metabolites was performed on Downloaded from dmd.aspetjournals.org at ASPET Journals on May 7, 2017 material. Urine and feces was collected from intact animals predose (212 to 0) and at 0–8 and 8–24, 24–48, 48–72, 72–96, 96–120, 120–144, and 144–168 hours postdose. The volume of urine and feces samples was recorded, and samples were stored at –20C until analysis. For the determination of pharmacokinetic parameters of total radioactivity and identification of circulating metabolites, a third group of jugular vein cannulated rats (n = 5/ gender) was given an oral dose of 200 mg/kg [14C]PF-04991532. Blood was collected at predose and at 0.25, 0.5, 1, 2, 4, 6, 8, 12, 24, and 48 hours postdose into tubes containing K2EDTA. The blood samples were centrifuged at 1000g for 10 minutes to obtain plasma. Citric acid monohydrate (500 mg/ml) was added to the plasma samples to create a plasma:citric acid (92:8, w/v) mixture. The final concentration of citric acid monohydrate in the sample was 40 mg/ml. Plasma was transferred to clean tubes and stored at 220C until analysis. Dog Study. Two male and two female beagle dogs were administered a single oral 80-mg/kg dose of [14C]PF-04991532 in 0.5% methylcellulose in reverse osmosis water for the mass balance study. Each dog received approximately 20 mCi/kg of radiolabeled material. Blood samples were collected by venipuncture of a jugular vein before dosing and at 0.5, 1, 2, 4, 6, 8, 12, 24, 48, 72, and 96 hours postdose. Blood was collected into tubes containing K2EDTA anticoagulant and was centrifuged within 1 hour of collection at 1300g for ;10 minutes to obtain plasma. Citric acid monohydrate (500 mg/ml) was added to the plasma samples to create a plasma:citric acid (92:8, w/v) mixture. The final concentration of citric acid monohydrate in the sample was 40 mg/ml. Urine and feces and wash/cage wipes were quantitatively collected for at least 18 hours before dosing and then at 0–6, 6–12–24, and over 24-hour intervals through 168 hours postdose. Determination of Radioactivity. Total radioactivity determination in rat and dog urine, feces, and plasma was conducted at Covance Laboratories Inc. (Madison, WI). The radioactivity in urine and plasma was determined by liquid scintillation counting. Duplicate aliquots of urine (0.1–0.4 g) and plasma (100– 400 ml) were mixed directly with 10 ml of Hionic Fluor scintillation fluid for radioactivity measurement by liquid scintillation counting using a Packard 2500 liquid scintillation counter (PerkinElmer Life and Analytical Sciences, Boston, MA). Fecal samples were weighed and homogenized with deionized water (2–3 times w/v, feces/water). Duplicate weighed aliquots of fecal homogenates (;300–400 mg) were combusted using a PerkinElmer Model 307 sampler oxidizer. Radioactivity in the combustion products was determined by trapping the liberated 14CO2 mixed with liquid scintillation fluid for radioactivity measurement. Acceptance criteria were combustion recoveries of 95–105%. Pharmacokinetic parameters for total radioactivity were determined using noncompartmental analysis. The amount of radioactivity in plasma at each time point was calculated using the specific activity of the dose administered and was expressed as nanogram equivalents per milliliter. Cmax of total radioactivity in plasma were estimated directly from the experimental data, with Tmax defined as the time of first occurrence of Cmax. Terminal elimination rate constants (kel) were estimated by linear regression of the log-linear plasma concentration time curve. The half-life (t1/2) was calculated as 0.693/kel. Area under the plasma concentration time curve (AUC) from time t to infinity [AUC(t–‘)] was extrapolated from AUC(0–t) adding Clast/kel, where Clast is the observed serum concentration at the last quantifiable time point estimated from the log-linear regression analysis. AUC from time zero to infinity [AUC(0–‘)] was estimated as the sum of [AUC(0–t)] and [AUC(t–‘)] values. Extraction of Metabolites from Biologic Matrices. Pooling of plasma samples from rats and dogs was performed for each individual animal according to the method of Hamilton (Hamilton et al., 1981), such that each sample was representative of total exposures (AUC) to metabolites relative to each other. Pooled plasma samples were diluted with 10 ml of acetonitrile while vortexing vigorously for 15–30 minutes. After centrifugation (1700g for 10 minutes), the supernatants were removed. The pellet was re-extracted with 15 ml of acetonitrile, and the two supernatants were combined. Aliquots (100–200 ml) were counted by liquid scintillation counting. The mean recovery of radioactivity after extraction was ;90–95%. The supernatants were concentrated to an approximate volume of 50 ml and then diluted with 200-ml 5 mM ammonium acetate (pH = 3.0):acetonitrile (95:5). Aliquots (;30 ml) were injected onto the LC-MS/MS for analysis. Urine samples from all species were pooled such that the sample pool represented ;90% of the total radioactivity excreted in the urine. Pooled urine samples were evaporated to dryness at 37C using the Genevac EZ-2 193 Circulating Metabolites of PF-04991532 Fig. 2. HPLC-UV (l = 254 nm) of metabolic profile of PF-04991532 (900 mg once daily for 14 days) in human plasma. Results Circulating Metabolites of PF-04991532 in Humans Circulating metabolites of PF-04991532 in humans were qualitatively examined in the 900-mg dose group from the 14-day MAD study. Figure 2 shows a representative HPLC-UV (l = 254 nm) chromatogram of day 14 pooled plasma samples from humans dosed daily with 900 mg of PF-04991532. PF-04991532 [retention time (tR) = 24.6 minutes; MH+ = 397.1485] was the major component in circulation followed by the glucuronide conjugate M1 (tR = 20.2 minutes; MH+ = 573.1803) and possibly three monohydroxylated metabolites, which included M2a (tR = 17.6 minutes; MH+ = 413.1431) and two poorly resolved peaks that have been designated as M2b/M2c (tR = 17.9–18.1 minutes; MH+ = 413.1431), respectively. Based on UV integration, M1 accounted for 11% of circulating drugrelated material, whereas oxidative metabolites M2a and M2b/M2c accounted for 18 and 20% of circulating drug-related material on day 14, respectively. 0.5 hours, respectively. The mean AUC(0–‘) and terminal phase t1/2 for total radioactivity was 25,700 ng-equivalent×h/ml and 4.62 hours, respectively, in female rats. In male rats, elimination t1/2 and AUC(0–‘) values for total radioactivity were not determined because a definitive elimination phase was not apparent in the plasma. Dogs. After administration of a single oral NOAEL dose of [14C]PF-04991532 (80 mg/kg) to beagle dogs, an overall mean (6 S.D.) of 82.9 6 3.74% of the total dose was recovered in urine and feces through 144 hours postdose (Table 1). Most of the excreted radioactivity was recovered in the first 48 hours. No gender-related differences were observed in the excretion pattern of radioactivity. The mean cumulative dose recovered in the feces and urine was 40.1 6 4.5% and 12.0 6 3.1%, respectively. Due to the formation of liquid feces, an unusually high percentage of radioactivity was recovered in the cage debris, rinse, wash, and wipe, and this accounted for 30.8 6 3.6% of the administered dose (Table 1). The mean Cmax for total radioactivity in male and female dogs (n = 2/gender) was 9040 and 6980 ng-equivalent/ml and peaked at 1.5 and 4.0 hours, respectively. The mean AUC(0–‘) values for total radioactivity were 36,600 and 32,900 ng-equivalent×h/ml in male and female dogs, respectively. The mean terminal phase t1/2 for total radioactivity was 2.30 and 1.26 hours for male and female dogs, respectively. Quantitative Profiles of [14C]PF-04991532 and Metabolites in Excreta and Circulation Rat Urine. A representative HPLC radiochromatogram of urinary metabolites from an intact female rat is shown in Fig. 3A. The metabolites were quantified by integration of the radiochromatographic peaks. The mean percentages of the metabolites detected in the urine of male and female rats, expressed as a percentage of the administered dose, are shown in Table 2. Unchanged parent Mass Balance and Pharmacokinetics of Total Radioactivity Rats. After administration of a single oral NOAEL dose of [14C]PF04991532 (200 mg/kg) to Sprague-Dawley rats, an overall mean (6 S.D.) of 91.5 6 1.3% of the total radioactive dose was recovered in the urine, feces, and cage wash/rinse over a period of 168 hours postdose (Table 1). The mean cumulative dose recovered in feces was 77.0 6 8.7%. The mean cumulative excretion in the urine was 11.7 6 5.7%. The majority of excreted radioactivity recovery occurred in the first 48 hours. No gender-related differences were observed in the excretion pattern of radioactivity. The mean Cmax for total radioactivity in male and female rats was 6060 and 10,600 ng-equivalent/ml and peaked at TABLE 1 Material balance and routes of excretion of [14C]PF-04991532 drug-related material in rats and dogs Values represent mean 6 S.D. Species Percentage Percentage Percentage Percentage of of of of dose in urine dose in feces dose in cage debris total dose recovered Rat 11.7 77.0 2.8 91.5 6 6 6 6 Dog 5.7 8.7 0.8 1.3 12.0 40.1 30.8 82.9 6 6 6 6 3.1 4.5 3.6a 3.74 a Due to liquid feces in dogs, an unusually high percentage of radioactivity was recovered in the cage debris, wash, and wipes. Downloaded from dmd.aspetjournals.org at ASPET Journals on May 7, 2017 a SYNAPT G2 (Waters MS Technologies, Manchester, UK) orthogonal acceleration quadrupole time-of-flight MS. The MS was operated in a positive ion mode using electrospray ionization. The desolvation gas was set to 749 l/h at a temperature of 300C. The cone gas was set to 20 l/h, and the source temperature was set to 150C. The capillary voltage was set to 4.3 kV, the cone voltage was set to 45 V, and the extraction cone was set to 5 V. The SYNAPT G2 was operated in V optics mode (sensitivity mode), with a resolution greater than 10,000 at full width at half maximum. The data acquisition rate was 0.10 s/scan; data were collected from 1 to 49 minutes using the dynamically variable collision energy MS acquisition mode, with a collision energy ramp of 25-45 V for high energy scans. The MS was calibrated to a mass accuracy under 5 mDa. Data were collected in the continuum mode from m/z 100 to 900. MassLynx version 4.1 SCN 803 software (Waters Corporation) was used for data processing. 194 Sharm et al. Fig. 3. Representative radiochromatograms of rat urine (A), feces (B), and plasma (C). DPM, disintegrations per minute. Metabolite Identification The structures of metabolites (Table 4) were elucidated by electrospray LC-MS/MS using a combination of full scan and CID product ion (MS2/MS3) scanning techniques. Parent (Unchanged Drug). PF-04991532 had an exact mass of 397.1485 (MH+). Its MS2 product ion spectrum (Supplemental Fig. 1) yielded a diagnostic fragment ion at m/z at 261.1241, resulting from the loss of the trifluoromethyl imidazolyl motif. Fragmentation of the fragment ion at m/z = 261.1241 resulted in diagnostic MS3 fragments at m/z = 243.1133, 193.0607, 179.0452, 165.0295, 139.0501, and 123.0802. The ions at 123.0802 and 139.0501 are formed via cleavage across the amide bond. Metabolite M1. Metabolite M1 had an exact mass of 573.1803 (MH+), which was 176 Da higher than PF-04991532. Its MS2 product ion spectrum showed a diagnostic fragment ion at m/z 397.1485 resulting from the neutral loss of 176 Da, suggesting that M1 was a glucuronide conjugate of PF-04991532. The tR and CID spectrum of M1 was identical to that of a crude preparation of the synthetic acyl glucuronide standard (data not shown). Metabolites M2a and M2b/M2c. Metabolites M2a and M2b/M2c possessed an exact mass of 413.1431 (MH+), which was 16 Da higher than PF-04991532 and suggestive of monohydroxylated metabolites. The MS2 product ion spectra were identical for M2a and M2b/M2c TABLE 2 Relative abundance (percentage of total administered dose) of urinary and fecal metabolites of PF-04991532 in rats and dogs after oral administration of [14C]PF-04991532 Rat Dog Metabolites PF-04991532 M1 M2a/M2b M3 Urine Feces Total Urine Feces Total 10.9 0.1 0.4 0.1 66.6 2.2 8.2 77.5 2.3 8.6 0.1 11.5 0.5 38.7 1.4 50.2 1.9 Downloaded from dmd.aspetjournals.org at ASPET Journals on May 7, 2017 PF-04991532 accounted for 10.9% of the dose. Metabolites accounted for ,1.0% of the administered dose. Rat Feces. A representative HPLC radiochromatogram of fecal metabolites from one intact male rat is shown in Fig. 3B. The mean percentages of fecal metabolites detected in male and female rats, expressed as percentages of the administered dose, are shown in Table 2. Unchanged parent PF-04991532 accounted for 66.6% of the dose. Oxidative metabolites (M2a and M2b) were the major metabolites that collectively accounted for 8.2% of the dose, whereas M1 accounted for 2.2% of the administered dose. There was no evidence for the presence of the putative M2c metabolite in rat feces. Rat Plasma. A representative HPLC radiochromatogram of circulating metabolites from one male rat is shown in Fig. 3C. The mean percentages of total circulating radioactivity are shown in Table 3. The majority of circulating radioactivity was attributed to the unchanged parent drug (71.5%) followed by M1 (28.5%). Dog Urine. A representative HPLC radiochromatogram of urinary metabolites from one male dog is shown in Fig. 4A. The metabolites were quantified by integration of the radiochromatographic peaks. The mean percentages of urinary metabolites detected in the urine of male and female dogs, expressed as percentages of the administered dose, are shown in Table 2. PF-04991532 and one metabolite M1 were detected in the urine of male and female dogs. The unchanged parent drug accounted for 11.5% of the dose. M1 represented 0.5% of the dose. Dog Feces. A representative HPLC radiochromatogram of fecal metabolites from one male dog is shown in Fig. 4B. The mean percentages of fecal metabolites detected in male and female rats, expressed as percentages of the administered dose, are shown in Table 2. PF-04991532 and one metabolite M1 were detected in the feces of male and female dogs. The unchanged parent drug accounted for 38.7% of the dose. M1 represented 1.4% of the dose. Dog Plasma. A representative HPLC radiochromatogram of circulating metabolites from one male dog is shown in Fig. 4C. The mean percentages of total circulating radioactivity are depicted in Table 3. The majority of circulating radioactivity was attributed to the unchanged parent drug (91.4%) followed by M1 (8.6%). 195 Circulating Metabolites of PF-04991532 TABLE 3 Relative abundance of circulating metabolites of PF-04991532 in rats and dogs after oral administration of PF-04991532 Metabolite Rat Dog PF-04991532 M1 M2a/M2b M3 Total 71.5 28.5 N.D. N.D. 100 91.4 8.6 N.D. N.D. 100 N.D., not detected. Oxidative Metabolism of Unlabeled PF-04991532 in Cryopreserved Rat, Dog, and Human Hepatocytes Qualitative examination of the metabolic profile in rat and human hepatocytes incubated for 4 hours with PF-04991532 (10 mM) revealed trace levels of M2a and M2b (Supplemental Fig. 4), with an Discussion The availability of plasma samples from the phase 1 MAD study of PF-04991532 in T2DM patients provided an initial glimpse of circulating human metabolites. Metabolite scouting studies used the steady state plasma samples (day 14) from the highest dose group (900 mg once daily) of PF-04991532. HPLC-UV analysis indicated PF-04991532 as the major component in circulation in humans Fig. 4. Representative radiochromatograms of dog urine (A), feces (B), and plasma (C). DPM, disintegrations per minute. Downloaded from dmd.aspetjournals.org at ASPET Journals on May 7, 2017 (Supplemental Fig. 2) and showed diagnostic fragment ions at m/z 277.1186 and m/z 259.1081, which were 16 Da higher than the primary MS2 fragment ions observed for PF-04991532, implying that the trifluoromethylimidazolyl portion of the molecule was unaltered. The MS3 product ion spectrum of m/z at 277 yielded diagnostic fragment ions at m/z 179.0451 and 139.0483, suggesting that the site of hydroxylations in the three metabolites were on the cyclopentyl ring. Additional insights into the structures of M2a and M2b/M2c are offered in the discussion section of the manuscript. Metabolite M3. Metabolite M3 had an exact mass of 139.0502 (MH+), which was 258 Da lower than PF-04991532. Its MS2 product ion spectrum showed a diagnostic fragment ion at m/z 121.0396, which represented the loss of water (Supplemental Fig. 3). The tR and CID spectrum of M3 was identical to an authentic standard of 6-aminonicotinic acid, implying that M3 was derived from an amide bond cleavage in PF-04991532. increased production of these metabolites (Supplemental Fig. 5) using the relay method (total incubation time of 20 hours) previously described in our laboratories (Di et al., 2012, 2013; Ballard et al., 2014). No metabolites of PF-04991532 were detected in dog hepatocytes at 4 or 20 hours. Examination of relay incubations also used a UPLC system with a slower flow rate (0.35 ml/min versus 1.0 ml/min) as a preliminary tactic to resolve M2b from M2c. As seen in Supplemental Fig. 5, M2a, M2b, and M2c (MH+ = 413.1431) now appeared as three distinct peaks at tR = 35.08, 36.14, and 36.30 minutes, respectively, in the human hepatocyte incubations. Metabolite M2c was not detected in the rat hepatocyte relay incubations, which is consistent with the in vivo findings in the rat mass balance/excretion studies. Interestingly, ketone metabolites (MH+ = 411.1274; tR = 36.9 and 37.7 minutes) possibly derived from oxidation of the secondary alcohol metabolites (M2a, M2b, and/or M2c) were also noted in rat and human hepatocyte incubations using the relay method. As mentioned earlier, no ketone metabolites were detected in the course of in vivo rat mass balance studies and human circulatory metabolic profiling. Furthermore, in contrast with the lack of metabolic turnover (t1/2 . 240 minutes) of PF-04991532 in human hepatocyte incubations conducted for 4 hours, the human hepatocyte relay assay yielded a t1/2 value of ;570 minutes, which yielded an unbound intrinsic clearance value of 7.3 ml/min per kg (fraction of PF-04991532 unbound in the incubation = 0.87) using our previously described protocol (Di et al., 2012, 2013). 196 Sharm et al. TABLE 4 Mass spectral characteristics of metabolites of PF-04991532 Metabolite MH+ tR Structure Fragment Ions min 397.1485 24.6 261.1241, 243.1133, 179.0452, 165.0295, 139.0501, 123.0802 M1 573.1803 20.2 437.1558, 397.1485, 261.1234 M2a, M2b/M2ca 413.1431 17.6, 17.9–18.1 M3 139.0502 3.0 277.1186, 259.1081, 179.0450, 139.0498 121.0396, 95.0604 a As shown in Fig. 2, metabolite scouting of FIH plasma samples revealed a well resolved (M1; tR = 17.6 minutes) and two poorly resolved (M2b/M2c; tR = 17.9/18.1 minutes) peaks at MH+ = 413, with an identical fragmentation pattern. The non-Gaussian peak shape (tR = 17.9–18.1 minutes in Fig. 2) strongly suggests the presence of more than one metabolite, and hence we have invoked the designation M2b/M2c. M2b and M2c generated in the human hepatocyte relay method were separated into two distinct peaks (tR = 36.1 and 36.3 minutes, respectively) using a UPLC method. alongside an acyl glucuronide metabolite (M1) and monohydroxylated metabolites M2a and M2b/M2c, respectively. The relative abundance of M1, M2a, and M2b/M2c was estimated to be ;11, ;18, and ;20%, respectively, in human plasma. These results, while preliminary in nature, suggest that metabolism plays a significant role in the in vivo elimination of PF-04991532 in humans. Approximately 38 and 11% of the drug-related material in circulation is attributed to oxidative and glucuronide metabolites, respectively, with the extent of oxidative metabolism in humans exceeding the amount observed in rats and dogs. These findings were somewhat paradoxical with our preclinical observations on the metabolic resistance of PF-04991532 in liver microsomes and hepatocytes from animals and humans. Qualitative profiling of metabolites in hepatocytes from animals and humans with unlabeled PF-04991532 revealed trace levels of M1, M2a, and M2b in rat and human hepatocytes, with no clear differentiation of major versus minor metabolites (Supplemental Fig. 2). The formation of oxidation products (M2a and M2b) in human liver microsomes was dependent on NADPH (data not shown), implying a role for the cytochrome P450 enzyme(s). Collectively, these observations challenge our original hypothesis regarding biliary elimination of unchanged PF-04991532 as the principal clearance mechanism in humans. Likely, PF-04991532 falls into the broad category of slowly metabolized compounds, which often rely on metabolic elimination as a route of clearance in vivo (Li et al., 2014; Ramsden et al., 2014). The metabolic (oxidative and/or conjugation) turnover rates for slowly metabolized compounds cannot be reliably estimated in standard liver microsomal and/or hepatocyte assays that are conducted for short incubation periods. Recently, we described the utility of a novel human hepatocyte suspension relay assay that extends drug residence time in cryopreserved hepatocytes and provides reliable estimates of in vitro intrinsic clearance and metabolic profiling data for slowly metabolized compounds (Di et al., 2013; Ballard et al., 2014). Using the relay conditions, we were able to measure a t1/2 value (;570 minutes) for metabolic decline of PF-04991532 in human hepatocytes that translated into an unbound intrinsic clearance of 7.3 ml/min per kg. The in vitro intrinsic clearance for PF-04991532 correlates with the in vivo unbound hepatic intrinsic clearance estimate of ;10.9 ml/min per kg that has Downloaded from dmd.aspetjournals.org at ASPET Journals on May 7, 2017 Parent Circulating Metabolites of PF-04991532 Fig. 5. Cyclopentyl ring hydroxylation of glucokinase activator 3 by cytochrome P450 (Sarabu et al., 2012). hepatic systems. Consequently, it would be interesting to re-examine the compounds with the in vitro–in vivo disconnect using the hepatocyte relay conditions. A pragmatic first step in this direction was recently communicated by our group (Ballard et al., 2014). To examine circulating metabolites in animals, mass balance/ excretion studies were initiated with [14C]PF-04991532. Following the oral administration of [14C]PF-04991532, mass balance was achieved, with mean total recoveries of 91.5% (rats) and 82.9% (dogs). Excretion of radioactivity was rapid and nearly complete within 48 hours after dosing in both species. Of the total radioactivity excreted in rat feces (77%) and urine (11.7%), unchanged PF-04991532 constituted 84.6% of the dose. Likewise, unchanged PF-04991532 accounted for 60.5% of the total administered dose in dog feces (40.1%) and urine (12.0%), respectively. Minor metabolites identified in rat and dog excreta included an acyl glucuronide (M1), two monohydroxylated regioisomers (M2a and M2b), and 6-aminonicotinic acid (M3). The majority of circulating radioactivity in animals was attributed to unchanged PF-04991532 (71.5 and 91.4% in rats and dogs, respectively). The glucuronide conjugate M1 accounted for 28.5 and 8.6% of the circulating radioactivity in rats and dogs, respectively. However, the monohydroxylated metabolites M2a and M2b/M2c, which were observed as circulating metabolites in humans, were not detected in plasma from rats and dogs. Although oxidative metabolites of PF-04991532 were not detected in circulation in animals, their presence was collectively noted in the excreta of at least one of the preclinical species for toxicological evaluation (M2a and M2b in particular were observed in rat excreta in 8.6% abundance). While oxidative metabolism of PF-04991532 does not result in a major alteration in structure, the process yields metabolites with increased polarity relative to the parent, as assessed from the calculated logP (PF-04991532 = 3.65; M2a/M2b = 1.57) and topological polar surface area (PF-04991532 = 94.36 A2; M2a/M2b = 114.59 A2). Like the parent compound, it is possible that the monohydroxylated metabolites (M2a and M2b/M2c) are also eliminated in the bile to some degree (Smith and Dalvie, 2012). Because of the relatively poor passive permeability of these compounds Fig. 6. Possible diastereomers that can be generated from cyclopentyl ring hydroxylation in PF-04991532. Downloaded from dmd.aspetjournals.org at ASPET Journals on May 7, 2017 been estimated from the oral CLp of PF-04991532 in humans (unpublished observations). Qualitative examination of the metabolic profile using the relay method demonstrated greater oxidative metabolism of PF-04991532 in human (;46% of the total integrated HPLC-UV peak area) and rat (;26% of the total integrated HPLC-UV peak area) hepatocytes relative to that noted in the 4-hour hepatocyte incubations (;5% of the total integrated HPLC-UV peak area). Incidentally, no metabolites of PF-04991532 were discerned in dog hepatocyte incubations conducted for 4 or 20 hours, respectively. Despite the qualitative nature of this study, the in vitro oxidative metabolic profile of PF-04991532 in the hepatocyte relay method has much resemblance to the in vivo oxidative metabolism of PF-04991532 noted in excreta and/or circulation in preclinical species and humans (human . rat . . dog). In a retrospective analysis utilizing ;48 compounds, Dalvie et al. (2009) demonstrated that in vitro metabolism studies in human hepatocytes (under normal incubation periods of ;4 hours) was a reasonable predictor of primary in vivo metabolites for several compounds. In some cases, compounds failed to generate the human metabolites in vitro, which was ascribed to the slow metabolic turnover in the in vitro 197 198 Sharm et al. Authorship Contributions Participated in research design: Sharma, Bergman, Litchfield, Kazierad, Pfefferkorn, Kalgutkar. Conducted experiments: Sharma, Atkinson, Bergman, Kazierad, Gustavson. Contributed new reagents or analytic tools: Sharma. Performed data analysis: Sharma, Litchfield Atkinson, Kalgutkar. Wrote or contributed to the writing of the manuscript: Kalgutkar, Sharma, Litchfield, Bergman, Di, Pfefferkorn. References Ballard TE, Orozco CC, and Obach RS (2014) Generation of major human excretory and circulating drug metabolites using a hepatocyte relay method. Drug Metab Dispos 42:899–902. Coghlan M and Leighton B (2008) Glucokinase activators in diabetes management. Expert Opin Investig Drugs 17:145–167. Dalvie D, Obach RS, Kang P, Prakash C, Loi C-M, Hurst S, Nedderman A, Goulet L, Smith E, and Bu H-Z, et al. (2009) Assessment of three human in vitro systems in the generation of major human excretory and circulating metabolites. Chem Res Toxicol 22: 357–368. Di L, Atkinson K, Orozco CC, Funk C, Zhang H, McDonald TS, Tan B, Lin J, Chang C, and Obach RS (2013) In vitro-in vivo correlation for low-clearance compounds using hepatocyte relay method. Drug Metab Dispos 41:2018–2023. Di L, Trapa P, Obach RS, Atkinson K, Bi Y-A, Wolford AC, Tan B, McDonald TS, Lai Y, and Tremaine LM (2012) A novel relay method for determining low-clearance values. Drug Metab Dispos 40:1860–1865. European Medicines Agency (2009) ICH topic M3 (R2) non-clinical safety studies for the conduct of human clinical trials and marketing authorization for pharmaceuticals, London. Ghosh A, Maurer TS, Litchfield J, Varma MV, Rotter C, Scialis R, Feng B, Tu M, Guimaraes CR, and Scott DO (2014) Toward a unified model of passive drug permeation II: the physiochemical determinants of unbound tissue distribution with applications to the design of hepatoselective glucokinase activators. Drug Metab Dispos 42:1599–1610. Grimsby J, Sarabu R, Corbett WL, Haynes NE, Bizzarro FT, Coffey JW, Guertin KR, Hilliard DW, Kester RF, and Mahaney PE, et al. (2003) Allosteric activators of glucokinase: potential role in diabetes therapy. Science 301:370–373. Gustavson SM, Pfefferkorn JA, Kazierad DJ, Chen D, Bergman A, Wang X, Rolph TP, and Rusnak JM (2013) Pharmacokinetics and pharmacodynamics of PF-04991532, a hepatoselective glucokinase activator (GKA), in T2DM patients on metformin therapy, in 73rd American Diabetes Association Meeting; 2013 June 21–25; Chicago, IL. Abstract 2635-PO, American Diabetes Association, Alexandria, VA. Hamilton RA, Garnett WR, and Kline BJ (1981) Determination of mean valproic acid serum level by assay of a single pooled sample. Clin Pharmacol Ther 29:408–413. Haynes NE, Corbett WL, Bizzarro FT, Guertin KR, Hilliard DW, Holland GW, Kester RF, Mahaney PE, Qi L, and Spence CL, et al. (2010) Discovery, structure-activity relationships, pharmacokinetics, and efficacy of glucokinase activator (2R)-3-cyclopentyl-2-(4methanesulfonylphenyl)-N-thiazol-2-yl-propionamide (RO0281675). J Med Chem 53:3618–3625. International Conference on Harmonisation (2012) Questions and answers (R2), Geneva, Switzerland. Lagas JS, Sparidans RW, Wagenaar E, Beijnen JH, and Schinkel AH (2010) Hepatic clearance of reactive glucuronide metabolites of diclofenac in the mouse is dependent on multiple ATPbinding cassette efflux transporters. Mol Pharmacol 77:687–694. Li Y, Zhou J, Ramsden D, Taub ME, O’Brien D, Xu J, Busacca CA, Gonnella N, and Tweedie DJ (2014) Enzyme-transporter interplay in the formation and clearance of abundant metabolites of faldaprevir found in excreta but not in circulation. Drug Metab Dispos 42:384–393. Matsushima S, Maeda K, Hayashi H, Debori Y, Schinkel AH, Schuetz JD, Kusuhara H, and Sugiyama Y (2008) Involvement of multiple efflux transporters in hepatic disposition of fexofenadine. Mol Pharmacol 73:1474–1483. Mithieux G (1996) Role of glucokinase and glucose-6 phosphatase in the nutritional regulation of endogenous glucose production. Reprod Nutr Dev 36:357–362. Matschinsky FM and Ellerman JE (1968) Metabolism of glucose in the islets of Langerhans. J Biol Chem 243:2730–2736. Matschinsky FM, Glaser B, and Magnuson MA (1998) Pancreatic b-cell glucokinase: closing the gap between theoretical concepts and experimental realities. Diabetes 47:307–315. Matschinsky FM, Zelent B, Doliba NM, Kaestner KH, Vanderkooi JM, Grimsby J, Berthel SJ, and Sarabu R (2011) Research and development of glucokinase activators for diabetes therapy: theoretical and practical aspects. Handbook Exp Pharmacol 203:357–401. Meininger GE, Scott R, Alba M, Shentu Y, Luo E, Amin H, Davies MJ, Kaufman KD, and Goldstein BJ (2011) Effects of MK-0941, a novel glucokinase activator, on glycemic control in insulin-treated patients with type 2 diabetes. Diabetes Care 34:2560–2566. Pfefferkorn JA (2013) Strategies for the design of hepatoselective glucokinase activators to treat type 2 diabetes. Expert Opin Drug Discov 8:319–330. Pfefferkorn JA, Guzman-Perez A, Litchfield J, Aiello R, Treadway JL, Pettersen J, Minich ML, Filipski KJ, Jones CS, and Tu M, et al. (2012) Discovery of (S)-6-(3-cyclopentyl-2-(4(trifluoromethyl)-1H-imidazol-1-yl)propanamido)nicotinic acid as a hepatoselective glucokinase activator clinical candidate for treating type 2 diabetes mellitus. J Med Chem 55:1318–1333. Ramsden D, Tweedie DJ, Chan TS, Taub ME, and Li Y (2014) Bridging in vitro and in vivo metabolism and transport of faldaprevir in human using a novel cocultured human hepatocyte system, HepatoPac. Drug Metab Dispos 42:394–406. Sarabu R, Berthel SJ, Kester RF, and Tilley JW (2011) Novel glucokinase activators: a patent review (2008 - 2010). Expert Opin Ther Pat 21:13–33. Sarabu R, Bizzarro FT, Corbett WL, Dvorozniak MT, Geng W, Grippo JF, Haynes NE, Hutchings S, Garofalo L, and Guertin KR, et al. (2012) Discovery of piragliatin—first glucokinase activator studied in type 2 diabetic patients. J Med Chem 55:7021–7036. Smith DA and Dalvie D (2012) Why do metabolites circulate? Xenobiotica 42:107–126. Smith DA and Obach RS (2009) Metabolites in safety testing (MIST): considerations of mechanisms of toxicity with dose, abundance, and duration of treatment. Chem Res Toxicol 22:267–279. U.S. Food and Drug Administration (2008) Guidance for industry: safety testing of drug metabolites, Center for Drug Evaluation and Research, U.S. Food and Drug Administration, U.S. Department of Health and Human Services, Rockville, MD. Address correspondence to: Amit S. Kalgutkar, Pharmacokinetics, Dynamics, and Metabolism–New Chemical Entities, Pfizer Worldwide Research and Development, 620 Memorial Drive, Cambridge, MA 02139. E-mail: [email protected] Downloaded from dmd.aspetjournals.org at ASPET Journals on May 7, 2017 (Ghosh et al., 2014), the interplay between the export of the parent and its metabolites from the liver into the blood and/or bile will likely rely on the individual affinities of these molecules for active transport via influx [multidrug resistant protein (MRP) isoforms 3, 4, and 6] and efflux transporters (MRP2, P-glycoprotein and/or breast cancer resistant protein), respectively, in rats and humans. If so, then the finding that comparative MRP3 transport activity is higher in humans than in rodents (Lagas et al., 2010) provides a possible explanation for the greater percentage of oxidative metabolites in circulation in humans compared with rats. Examination of the in vitro active transport of PF-04991532 and its oxidative metabolites will shed additional light on this matter. The mass spectra of M2a and M2b/M2c were identical and indicated that these metabolites were derived from a single site of oxidation on the cyclopentyl ring in PF-04991532. With the aid of UPLC, we were further able to chromatographically resolve M2b and M2c into two distinct peaks in the human hepatocyte relay assay. Preliminary insights into the structures of M2a, M2b, and M2c were obtained via comparison of the known metabolic fate of the structurally related glucokinase activator, referred to as compound 3 (Fig. 5), in the publication of Sarabu et al. (2012). In liver microsomes, compound 3 was shown to undergo monohydroxylations on the C-2 and C-3 positions on the cyclopentyl group, generating the corresponding alcohol regioisomers (Sarabu et al., 2012). It is noteworthy to point out that hydroxylation at either the C-2 and/or C-3 position of the cyclopentyl ring in PF-04991532 and compound 3 will result in the conversion of the prochiral methine at C-1 into a chiral carbon atom and lead to the formation of diastereomeric products. Our present study as well as the one from Sarabu et al. (2012) characterized three metabolites derived from cyclopentyl ring oxidation. In theory, single site oxidations on the C-2 or the C-3 positions on the cyclopentyl ring could potentially lead to the formation of eight diastereomers, as shown in Fig. 6. Therefore, in the case of PF-04991532, it is possible that additional diastereomers are also formed and will need to be resolved from the distinct M2a, M2b, and M2c peaks detected in our present studies. Sarabu et al. (2012) demonstrated that the diastereomeric mixture of C-2 and C-3 hydroxylated metabolites of compound 3, generated via independent synthesis, were ;2 orders of magnitude less potent as GK activators as compared with the parent compound. By inference, we conclude that the propensity of M2a, M2b, and M2c to activate GK would be significantly lower than PF-04991532. In conclusion, a human metabolite scouting study in tandem with the animal mass balance study allowed early identification of oxidative metabolites in circulation in humans but not animals. A human mass balance study with a clinically efficacious dose of [14C]PF-04991532 (estimated to be 450 mg q.d. based on phase 2 clinical efficacy data) is currently in progress to supplement the animal mass balance/excretion data. Ongoing activities also include the elucidation of the human cytochrome P450 isoforms responsible for PF-04991532 oxidation and the isolation and characterization of the diastereomeric oxidative metabolites. Obtaining authentic metabolite standards will be critical for the determination of absolute amounts (total/unbound) of systemic exposures in humans and animals as opposed to percentage values for metabolites as comparators since toxicity thresholds are ultimately related to absolute exposure values (Smith and Obach, 2009). These collective findings will be reported in due course.