* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Venous malformations
Survey
Document related concepts
Transcript
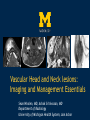
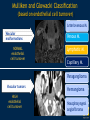
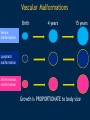
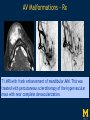
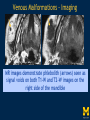
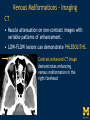
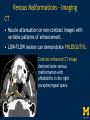
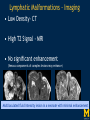
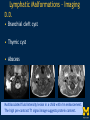
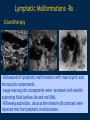
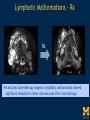
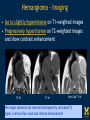
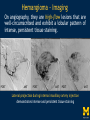
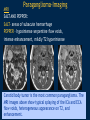
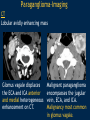
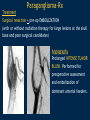
Vascular Head and Neck lesions: Imaging and Management Essentials Sean Woolen, MD, Ashok Srinivasan, MD Department of Radiology University of Michigan Health System, Ann Arbor Disclosures No relevant financial disclosures Purpose Classification and terminology Role of imaging Management Mulliken and Glowacki Classification (based on endothelial cell turnover) Arteriovenous M. Vascular malformations NORMAL endothelial cell turnover Venous M. Lymphatic M. Capillary M. Paraganglioma Vascular tumors HIGH endothelial cell turnover Hemangioma Nasopharyngeal angiofibroma New ISSVA Terminology Cavernous hemangioma Liver hemangioendothelioma Infantile hemangioma Port wine stain Capillary malformation Hepatic/vertebral/orbital hemangiomas Venous malformation Lymphangioma Cystic hygroma Lymphatic malformation Role of Imaging Anatomic localization Assessing extent Often no specific features Vascular Malformations Birth 4 years 15 years Venous malformation Lymphatic malformation Arteriovenous malformation Growth is PROPORTIONATE to body size AV Malformations - Clinical Picture • Commonly manifest later in childhood or adolescence • Pulsatile lesions that can cause clinical bruit, pain, bleeding, and ulceration AV Malformations - Imaging CT and MRI Large dilated vascular structures with arteries and veins being usually indistinguishable Contrast enhanced CT demonstrates abnormal nidus of vessels along the right face with dilated vascular channels, likely draining veins AV Malformations - Imaging ANGIOGRAPHY GOLD STANDARD Early venous shunting, arterial feeders, venous drainage Lateral Projection - ECA Injection Early Arterial Mid Arterial AV Malformations - Staging Stage Description 1 Quiescent: stable 2 Increasing in size 3 Symptomatic: pain, bleeding, disfigurement, disruption of function 4 Decompensating: high-output cardiac failure Schobinger classification helps guide management for AV malformations. Treatment of symptomatic patient's with stage II or above AV malformations. AV Malformations - Rx Gold Standard Preoperative angiography with selective embolization of the nidus and draining veins followed by definitive resection within 24-48 hours. Resistant Malformations Angiography with combination of selective embolization of the nidus and percutaneous sclerotherapy. With limited angiographic access to the nidus, emerging percutaneous cryotherapy is an option. AV Malformations - Rx T1 MRI with frank enhancement of mandibular AVM. This was treated with percutaneous sclerotherapy of the hypervascular mass with near complete devascularization. Venous Malformations – Clinical Picture • Soft, compressible, bluish nonpulsatile mass • Expansion on ipsilateral jugular vein compression, performance of the Valsalva maneuver, or dependent positioning Venous Malformations - Imaging MRI (Best Imaging) • Crucial to assess multispatial extent • Isointense -T1-weighted • Hyperintense - T2-weighted • Intense enhancement Venous Malformations - Imaging MRI • Distinguishing features include DISCRETE AREAS OF HOMOGENEOUS HIGH SIGNAL INTENSITY (venous lakes) and PHLEBOLITHS T2-W T1-W Post Gad T1-W Venous Malformations - Imaging MR images demonstrate phlebolith (arrows) seen as signal voids on both T1-W and T2-W images on the right side of the mandible Venous Malformations - Imaging CT • Muscle attenuation on non-contrast images with variable patterns of enhancement. • LOW-FLOW lesions can demonstrate PHLEBOLITHS. Contrast enhanced CT image demonstrates enhancing venous malformation in the right forehead Venous Malformations - Imaging CT • Muscle attenuation on non-contrast images with variable patterns of enhancement. • LOW-FLOW lesions can demonstrate PHLEBOLITHS. Contrast enhanced CT image demonstrates venous malformation with phleboliths in the right parapharyngeal space Venous Malformations - Treatment Many venous malformations do not require specific management • Intervention depends on – Hematologic evaluation – Size of the lesion – Functional impact on the patient Venous Malformations - Treatment Hematologic Evaluation Fibrinogen and D-dimer levels can detect the presence of localized intravascular coagulopathy, which may progress to disseminated intravascular coagulopathy with aggressive therapy. If elevated, should start prophylactic Lovenox. Venous Malformations - Treatment Sclerotherapy The sclerosants administered are typically 95% ethanol or sodium tetradecyl sulfate (Sotradecol) Sclerotherapy + Surgery Debulking For large, infiltrating malformations that are difficult to delineate, combined sclerotherapy with ablative and reconstructive surgery is indicated Small & well circumscribed Large & infiltrating Sirolimus is an emerging treatment when extensive venous malformations are refractory to other treatments. Venous Malformations - Treatment Sclerotherapy procedure of right facial venous malformation using ultrasound guidance, 20 gauge angiocatheter access, and injection of bleomycin sclerosant. Lymphatic Malformations Clinical Picture Arises from sequestered portions of the embryonic lymphatic anlage CLINICAL EXAM • Manifest as soft, colorless masses • 60% apparent at birth, while 80-90% manifest by 2 years • Head and neck are the most common site of distribution • Growth proportionate to body size Lymphatic Malformations • Type I lymphatic malformations (macrocystic) – Generally arise below the mylohyoid and occur in the anterior and posterior triangles of the neck. – Historically termed cystic hygromas – >2 cm in size • Type II lymphatic malformations (microcystic) – Generally located above the mylohyoid commonly involving the tongue, floor of the mouth, cheeks, lips, and sometimes the parotid gland – Historically termed lymphangiomas – <2 cm in size Lymphatic Malformations - Imaging • Low Density- CT • High T2 Signal - MRI • No significant enhancement (Venous components of complex lesions may enhance) Multiloculated fluid intensity lesion in a neonate with minimal enhancement Lymphatic Malformations - Imaging D.D. • Branchial cleft cyst • Thymic cyst • Abscess Multiloculated fluid intensity lesion in a child with rim enhancement. The high pre-contrast T1 signal image suggests protein content. Lymphatic Malformations - Imaging Venolymphatic malformation with mixed signal intensity (fluid signal and enhancing components). Venous malformation in white *Both have phleboliths Lymphatic Malformations - Rx Sclerotherapy is advocated for large macrocystic lesions with alcohol, doxycycline, or bleomycin Surgical excision with careful preservation of involved neurovascular structures and laser photocoagulation serve as important therapeutic adjuncts Lymphatic Malformations -Rx Sclerotherapy -Ultrasound of lymphatic malformation with macrocystic and microcystic components. -Large macrocystic components were accessed with needle aspirating fluid (yellow LM and red LVM) -Following aspiration, doxycycline mixed with contrast were injected into the lymphatic malformation. Lymphatic Malformations - Rx Rx Pre and post sclerotherapy images in lymphatic malformation showed significant reduction in lesion size one year after sclerotherapy Hemangioma - Prototype Vascular Tumor Infantile Hemangioma is GLUT1 positive Proliferating and involuting phases Involution Proliferation Birth 6-12 months Up to 9 years Typically complete resolution – 50% by 5 years; 70% by 7 years; 90% by 9 years Hemangioma-Classification Congenital Hemangioma is GLUT1 negative Rapidly involuting congenital hemangioma (RICH) most commonly involute by 14 months Partial-involuting congenital hemangioma (PICH) Non-involuting congenital hemangioma (NICH) can grow in proportion the patients age or stay the same size Hemangioma - Imaging • Clinical history is key to recognizing the proliferating phase CT • Heterogeneity and intense enhancement, often in a delayed manner Contrast enhanced CT in a 6 month old infant shows enhancing right neck mass that was progressively getting larger since birth Hemangioma - Imaging • Iso to slightly hyperintense on T1-weighted images • Progressively hyperintense on T2-weighted images and show contrast enhancement T2-W T1-W Post Gad T1-W MR images demonstrate internal heterogeneity, increased T2 signal, internal flow voids and intense enhancement Hemangioma - Imaging On angiography, they are high-flow lesions that are well-circumscribed and exhibit a lobular pattern of intense, persistent tissue staining. POST ANT POST ANT POST Lateral projection during internal maxillary artery injection demonstrates intense and persistent tissue staining ANT Hemangioma -Treatment Treatment when one of the criteria below are met: Emergency • Potentially lifethreatening complication Urgency • Existing or imminent functional impairment, pain, or bleeding Structure Anomalies Elective • Identify structural anomalies associated with infantile hemangioma • Reduce the likelihood of long-term or permanent disfigurement Hemangioma -Treatment Observation remains the preferred management option Vincristine Beta Blockers First line treatment Lesions associated with KasabachMerritt phenomenon Surgery Pulse dye laser Treatment of ulcerating lesions Steroids, Interferon, and Imiquimod Failure/contraindication to pharmacotherapy and Used less commonly because other favorable anatomical treatments have area for resection or better safety profiles resection of residual fibrofatty tissue after involution Paraganglioma- Clinical Picture • Jugulotympanic paragangliomas present with pulsatile tinnitus and hearing loss. Physical exam shows a bluish/pulsating mass behind the tympanic membrane. • Carotid Body present as a painless, non-tender, enlarging mass lateral to the tip of the hyoid bone. Physical exam shows a pulsatile mass which moves side to side, but not vertically. • Glomus Vagale present as a painless non-tender mass posterior to the mandible with cranial nerve symptoms such as dysphagia (IX), hoarseness (X), shoulder drop (XI), aspiration (XII). Paraganglioma-Imaging MRI SALT AND PEPPER: SALT– areas of subacute hemorrhage PEPPER – hypointense serpentine flow voids, intense enhancement, mildly T2 hyperintense Carotid body tumor is the most common paraganglioma. The MRI images above show typical splaying of the ICA and ECA flow voids, heterogeneous appearance on T2, and enhancement. Paraganglioma-Imaging CT Lobular avidly enhancing mass Glomus vagale displaces the ECA and ICA anterior and medial heterogeneous enhancement on CT. Malignant paraganglioma encompasses the jugular vein, ECA, and ICA. Malignancy most common in glomus vagale. Paraganglioma-Imaging Jugulotympanic is the most common primary tumor in the middle ear. Important to notice asymmetric jugular foramen enlargement. The CT image shows asymmetrical right jugular foramen enlargement with moth eaten appearance. Treatment Paraganglioma-Rx Surgical resection + pre-op EMBOLIZATION (with or without radiation therapy for large lesions at the skull base and poor surgical candidates) Angiography Prolonged INTENSE TUMOR BLUSH. Performed for preoperative assessment and embolization of dominant arterial feeders. Summary • Proportionate growth to body size – Vascular malformations • Rapid growth from birth followed by involution – Infantile hemangioma • Phleboliths – Venous malformations • Hemangiomas– Usually no Rx • Venous and Lymphatic malformations – Sclerotherapy +/surgery • AV malformations and Paraganglioma – Preop embolization + Surgery References • Mulliken JB et al. Hemangiomas and vascular malformations in infants and children: A classification based on endothelial characteristics. Plast Reconstr Surg 69:412-422, 1982 • Mulliken JB et al. Classification of pediatric vascular lesions. Plast Reconstr Surg 70:120-121, 1982 • Lowe et al. Vascular Malformations: Classification and Terminology the Radiologist Needs to Know. Semin Roentgenol. 2012; 47 (2): 106-17 • Dasgupta et al. ISSVA classification. Semin in Pediatric surgery. 23: 158-161. 2014. References • Fowell C et al. Arteriovenous malformations of the head and neck: current concepts in management. Br J Oral Maxillofac Surg. 2016. [Ahead of print]. • Nassiri N et al. Evaluation and management of peripheral venous and lymphatic malformations. 4 (2): 257-65, 2016. • Woolen S et al. Paragangliomas of the Head and Neck. Neuroimaging Clin N Am. 2016. [Ahead of print]. • Darrow DH et al. Diagnosis and management of infantile hemangioma. 136 (4): 1060-104. 2015.