* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Tissue Fluid and Lymph
Derivation of the Navier–Stokes equations wikipedia , lookup
Reynolds number wikipedia , lookup
Magnetohydrodynamics wikipedia , lookup
Hydraulic machinery wikipedia , lookup
Bernoulli's principle wikipedia , lookup
Hemorheology wikipedia , lookup
Hemodynamics wikipedia , lookup
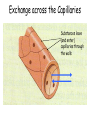
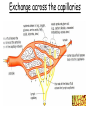
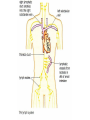
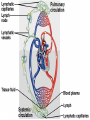
Tissue Fluid and Lymph Objectives: • Explain the differences between blood, tissue fluid and lymph. • Describe how tissue fluid is formed from plasma. Exchange across the Capillaries Substances leave (and enter) capillaries through the walls Formation of tissue fluid • As blood flows through the capillaries some plasma passes out to bathe the surrounding cells. • This tissue fluid is very similar to plasma but does not have large plasma protein molecules in it. They were too big to pass through the tiny gaps between the endothelial cells making up the capillary walls. • The tissue fluid supplies the cells with glucose, amino acids, fatty acids, salts and oxygen. • The fluid then returns to the blood in the capillaries taking any waste products from the cells with it e.g. CO2 and Urea Exchange across the capillaries Arterial End of Capillary • Here the hydrostatic pressure of the blood is high. This will encourage the filtration of the fluid content of the blood through small gaps between the endothelial cells of the walls of the capillary. Blood cells and plasma proteins are too large to be filtered. • However, as the blood has a low (negative) water potential at the arterial end of the capillary, there is a tendency for water to move into the capillary from the surrounding tissue fluid, due to osmosis. • As the hydrostatic pressure encouraging fluid out of the capillary is higher than the osmotic pressure encouraging water into the capillary, the net result is water (and small molecules dissolved in it) moves out of the blood and into the surrounding tissue fluid. Venous End of Capillary • Here the hydrostatic pressure of the blood is lower, as much of the fluid content was lost to the surroundings. The hydrostatic pressure will still encourage filtration of fluid out of the blood into the surrounding tissue fluid, but the size of this force is low. • The blood now has a very low (very negative) water potential, as it consists mainly of blood cells and large plasma proteins with very little fluid. This encourages movement of water (and any small substances dissolved in it) from the tissue fluid into the blood. • As the osmotic pressure encouraging fluid into the capillary is greater than the hydrostatic pressure encouraging it out, the net result is that fluid reenters the capillary. Lymph • Not all the fluid returns to the blood capillary. • 10% enters a separate system of microscopic tubes called lymph capillaries. These are part of the lymph system. • The lymph capillaries join to form lymph vessels. • Lymph vessels have valves that let fluid enter but not leave them FLUIDS • • • • • • Fluid in the blood is called... Plasma Fluid surrounding the cells is called... Tissue fluid Fluid in the lymphatic system is called... Lymph There is very little difference between these three! Lymph • Flow of liquid through the lymph system is very slow • It depends on movement of our muscles, the valves in the vessels and the negative pressure in chest when we breath in. • Flow is in one direction only, from tissues towards the heart. • Most of the lymph re-enters the blood stream at the subclavian veins under the collar bones • Lymph is a milky looking fluid • Digested fat is absorbed into the lymph Lymph • At intervals along the lymph vessels are structures called lymph nodes • These are part of the immune system • Lymphocytes are produced in the lymph nodes • Lymphocytes are white blood cells that produce antibodies. • The lymph nodes swell up at times of infection