* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download 3. contraindications 1
Survey
Document related concepts
Transcript
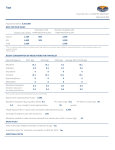
INTERNAL ONLY STANDING ORDER EMERGENCY DEPARTMENTS MORPHINE SULFATE – Intravenous administration by Accredited Emergency Nurses for moderate to severe pain POLICY STATEMENT This order may only be activated under the specific circumstances set out in the section “Indications” and provided there are no contraindications present. The administering nurse must be accredited to administer the drug and record the administration in ink on the once only section of the medication chart. This order must be checked and signed by a medical officer within 24 hours, and preferably within 4 hours, of activation of the standing order. This standing order is only valid until the date noted by the Drug and Quality Use of Medicines Committee under the heading "Effective To:" at the end of this document. 1. NURSING ACCREDITATION REQUIREMENTS Accredited Registered Nurses employed within SESLHD Emergency Departments (ED) who are working in a extended practice nurse or Advanced Clinical Nurse (ACN) capacity must have at least a minimum of two (2) years emergency / critical care experience and must be able to work at a minimum of resuscitation level or above (i.e. triage / clinical initiatives nurse) and/or as approved by the ED Nurse Manager. 2. INDICATIONS Adult patients (16 years of age and over) who present to SESLHD Emergency Department (ED) in moderate to severe pain with verbal numerical rating scale of equal to or greater than five (5). CONTRAINDICATIONS 1 3. REV 1 Less than16 years of age Haemodynamically unstable (meets PACE / Between The Flag criteria2) Acute pain with a verbal numerical rating scale of less than 5 Known hypersensitivity to morphine or other opioids Acute or severe bronchial asthma or other obstructive airways disease Severe CNS depression Diabetic acidosis where there is a danger of coma Severe liver disease or incipient hepatic encephalopathy Following biliary tract surgery or surgical anastomosis Gastrointestinal obstruction or suspected surgical abdomen Monoamine oxidase (MAO) inhibitors within the previous fourteen days Cardiac arrhythmias; heart failure secondary to pulmonary disease Acute alcoholism or delirium tremens Head injuries (Glasgow Coma Scale less than 15) Brain tumour; raised intracranial or cerebrospinal pressure Convulsive states such as status epilepticus Tetanus or strychnine poisoning October 2014 Page 1 of 5 INTERNAL ONLY STANDING ORDER EMERGENCY DEPARTMENTS MORPHINE SULFATE – Intravenous administration by Accredited Emergency Nurses for moderate to severe pain PRECAUTIONS 1 4. 5. Respiratory depression or impairment Bradycardia CNS depression Drug dependence and tolerance Hypotensive effect Supraventricular tachycardias Acute abdominal condition Convulsions Hepatic impairment Renal impairment Elderly Pregnancy (Category C) – morphine crosses the placenta and is associated with foetal CNS effects Lactation – morphine is excreted in milk and breastfeeding is not recommended ACTIONS/MONITORING REQUIRED Pre administration: Assessment of previous pain treatments utilised i.e. over the counter and/or prescription drugs The patient must have a cannula insitu and be laying down A full set if vitals (heart rate, blood pressure, respiration rate, temperature, Glasgow Coma Scale (GCS) and pain score) must be taken prior to administration of morphine sulfate. 10 mg / 1 mL morphine sulfate ampoules are diluted with 9 mL of sodium chloride 0.9% to make concentration of 1 mg / mL OR 5 mg / 1 mL morphine sulfate ampoules are diluted with 4 mL of sodium chloride 0.9% to make concentration of 1 mg / mL All syringes must be labelled with a medication label indicating morphine and the dilution. Documentation: Document patient observations including the patient’s pain score on the ED Standard Adult General Observation (SAGO) Chart and/or electronically within Firstnet. The administering nurse must record the administration in ink on the ‘once-only’ section of the National Inpatient Medication Chart (NIMC) as Emergency Department Standing Order (i.e. “ED SO”) plus print and sign their name. The EDSO drug order must be countersigned by the medical officer that subsequently assesses and treats the patient within 4 hours. Accountable Drug Register documentation must be completed i.e. when documenting in the S8 drug book, the ED Medical Director’s name followed by ‘EDSO’ next to it to indicate this is a standing order. REV 1 October 2014 Page 2 of 5 INTERNAL ONLY STANDING ORDER EMERGENCY DEPARTMENTS MORPHINE SULFATE – Intravenous administration by Accredited Emergency Nurses for moderate to severe pain The signatures of the administering nurse and nurse checking the medication must be clearly documented both in the Accountable Drug Register and on the NIMC and includes completing the date, time, drug, dose, route and time of administration sections. The administering nurse must record in the patient’s progress notes the administration and effect of the medication. Drugs must be checked and ordered according to hospital policy and adhering to the Ministry of Health Policy Medication Handling in NSW Public Health Facilities PD2013_043. Post administration: Evaluate and document therapeutic response to pain via numerical or visual analogue pain score Re-assessment of pain within 3-5 minutes of administration of each 2.5 mg dose. Re-assessment of patient is to occur after each IV bolus including full set of vital signs (heart rate, blood pressure, respiration rate, temperature, Glasgow Coma Scale (GCS) and pain score). Ongoing monitoring of respiratory rate Senior medical review must be obtained if any of the following occur: 1. Respiratory rate less than 10 breaths a minute 2. SpO2 <92% 3. Systolic blood pressure <100mmHg 4. Heart rate <50bpm 5. GCS < 14 6. Sedation score >1 Notify a medical officer if patient meets PACE / Between The Flag criteria2 Monitor for side effects and consider anti-emetics if nausea / vomiting develops. Warn patient of possible sedation and not to drive or operate machinery Sedation scoring Measuring patient sedation in relation to the medication discussed within the document, the following tool is to be used: 0 1 2 Wide awake Easy to rouse Constantly drowsy, unable to stay awake 3 Yellow Zone: Cease administration. Given high-flow oxygen, complete primary survey, alert attending emergency medical officer. If patient respiratory rate less than or equal to 5 breathes per minute, activate emergency call buzzer. Difficult to rouse or unresponsive Red Zone: Activate emergency call buzzer, complete primary survey, administer high-flow oxygen. REV 1 October 2014 Page 3 of 5 INTERNAL ONLY STANDING ORDER EMERGENCY DEPARTMENTS MORPHINE SULFATE – Intravenous administration by Accredited Emergency Nurses for moderate to severe pain 6. PROTOCOL/ADMINISTRATION GUIDELINES: Caution: CHECK for allergies and/or contraindications Drug Dose Route 16 to 65 years: Morphine Sulfate (solution for injection) 2.5 mg – 10 mg over 65 years: 1 mg – 5 mg Intravenous (IV) over 1 to 2 minutes Frequency every 3 to 5 minutes for pain score ≥5 until a maximum dose of 10 mg has been administered every 3 to 5 minutes for pain score ≥5 until a maximum dose of 5 mg has been administered Solution for injection should be clear, colourless to slightly yellow. Sodium chloride 0.9% 5 mL flush should be administered IV after each morphine dose. Unused portions of morphine are to be discarded immediately once the patient is pain free or if it has been greater than 5 minutes since the last dose. The morphine must be discarded by the same two employees who prepared the medication (RN, MO or pharmacist) and recorded in the drug register. 7. POTENTIAL ADVERSE EFFECTS/INTERACTIONS: Most common side effects: Constipation, Lightheadedness, dizziness, sedation / drowsiness, Nausea, vomiting, Sweating, dysphoria and euphoria. Less frequent side effects: Cardiovascular. Flushing of the face, chills, tachycardia, bradycardia, palpitations, syncope, hypotension and hypertension. Central nervous system. Weakness, headache, restlessness, anxiety, agitation, tremor, uncoordinated muscle movements, insomnia, dizziness, vertigo, delirium, confusional symptoms and occasionally hallucinations. Gastrointestinal. Dry mouth, anorexia, , cramps, laryngospasm, colic, taste alterations and biliary tract cramps and biliary spasm. Genitourinary. Urinary retention or hesitancy, ureteric spasm, reduced libido or potency Endocrine. Hyponatraemia, hyperglycaemia. Visual disturbances. Blurred vision, nystagmus, diplopia and miosis Allergic. Pruritus, urticaria, other skin rashes including contact dermatitis and oedema. Allergic reactions may be due to histamine release and may be more frequent in asthmatic patients. Anaphylactic reactions following intravenous injection have been reported rarely Local effects. Pain at injection site or local tissue irritation REV 1 October 2014 Page 4 of 5 INTERNAL ONLY STANDING ORDER EMERGENCY DEPARTMENTS MORPHINE SULFATE – Intravenous administration by Accredited Emergency Nurses for moderate to severe pain Dependence/ tolerance - with long term use. Withdrawal (abstinence) syndrome - Interactions: CNS depressants - including other opioids, sedatives, hypnotics, general anaesthetics, tranquilisers, phenothiazines and alcohol Antihypertensives Muscle relaxants MAO Inhibitors Anticoagulants Diuretics Amphetamines Metoclopramide Delayed gastric emptying may delay absorption of orally administered drugs Anticholinergic agents increase risk of constipation 8. REFERENCES: 1. MIMMS Online. Morphine Sulphate. 2014 [cited 25/8/14] Available from: https://www.mimsonline.com.au.acs.hcn.com.au/Search/FullPI.aspx?ModuleName=Produc tInfo&searchKeyword=Morphine+sulfate&PreviousPage=~/Search/QuickSearch.aspx&Sear chType=&ID=3790001_2 2. SESLHD Patient with Acute Condition for Escalation (PACE): Management of the Deteriorating Adult and Maternity Inpatient SESLHD/PR283. http://www.seslhd.health.nsw.gov.au/Policies_Procedures_Guidelines/Clinical/Other/SESL HDPR283-PACE-MgtOfTheDeterioratingAdultMaternityInpatient.pdf 3. Ministry of Health Policy Medication Handling in NSW Public Health Facilities PD2013_043 http://www0.health.nsw.gov.au/policies/pd/2013/pdf/PD2013_043.pdf Authorised by: Name Designation Professor Gordian Fulde Emergency/ Critical Care Stream Director Endorsed by: Name Designation Signature Signature Chair, SESLHD D&QUM Committee REV 1 Date Endorsed Date Effective To: 30 November 2015 October 2014 Page 5 of 5