* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Real World Data
Survey
Document related concepts
Transcript
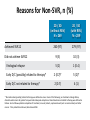
Real World Data REAL-WORLD SAFETY AND EFFECTIVENESS OF OMBITASVIR/PARITAPREVIR/R ± DASABUVIR ± RIBAVIRIN IN THE GERMAN HEPATITIS C REGISTRY Holger Hinrichsen1, Heiner Wedemeyer2, Stefan Christensen3, Christoph Sarrazin4, Axel Baumgarten5, Stefan Mauss6, Jan Hettinger7, Henning Kleine7 Affiliations: 1Gastroenterology-Hepatology Center Kiel, Kiel, Germany; 2Gastroenterology, Hepatology and Endocrinology, Hannover Medical School, Hannover, Germany; 3Center for Interdisciplinary Medicine, Muenster, Germany; 4J.W. Goethe University, Frankfurt, Germany; 5Medical Center for Infectious Diseases, Berlin, Germany; 6MVZ, Düsseldorf, Germany; 7AbbVie GmbH & Co KG, Wiesbaden, Germany 51st Annual Meeting of the European Association for the Study of the Liver • Barcelona, Spain • 16 April 2016 Methods German Hepatitis C Registry (DHC-R): non-interventional, prospective cohort study with 254 study sites in Germany Data were collected between February 1, 2014 and December 7, 2015 Patients must have had HCV GT1 or GT4 infection and been treated with 2D / 3D ± RBV; N = 1017 patients Exclusion criteria: HCV GT 2/3/5/6 or mixed GT1/GT4 infection Limitations: • Choice of treatment and duration was at physician’s discretion and may not be in agreement with the local label or guideline recommendations • Follow up and laboratory testing were at investigator’s discretion Study Profile ¶ = Defined by treatment initiation after June 22, 2015 = Patient files not completed. Queries ongoing. F/U, follow-up. Data presented as of December 7th 2015 * Baseline Demographics 2D / 3D ± RBV; (N = 1017) Male, n (%) 660 (65) Age, mean years ± SD 54.3 ± 12.5 BMI, mean kg/m2 ± SD 26.2 ± 4.4 Caucasian, n (%) 963 (95) HCV Genotype, n (%) 1 892 (88) 1a 261 (26) 1b 614 (60) Other 4 HCV RNA, mean 106 IU/mL ± SD Cirrhosis, n/N (%) Compensated (Child-Pugh A) 17 (2) 125 (12) 2.8 ± 4.0 (n = 973) 228/1017 (22) 149/228 (65) Decompensated (Child-Pugh B/C) 16/228 (7) Data not available 63/228 (28) Deviations in n-values for diagnostic parameters are due to missing documentation in the registry at the time point of analysis Regimen Duration, n (%) 8W 12 W 24 W Other GT1a* N = 137 w/o cirrhosis 1 (0.7) 130 (94.9) 1 (0.7) 5 (3.6) GT1a* with cirrhosis N = 30 1 (3.3) 24† (80.0) 4 (13.3) 1 (3.3) GT1b N = 284 w/o cirrhosis 3 (1.1) 271 (95.4) 0 10 (3.5) GT1b N = 104 with cirrhosis 0 96 (92.3) 1 (1.0) 7 (6.7) GT4 w/o cirrhosis N = 58 0 56 (96.6) 0 2 (3.4) GT4 with cirrhosis N=2 0 2 (100) 0 0 Data is available for patients that reached EOT only (N = 615) Dark green shading indicates the label-recommended treatment duration according to cirrhosis and HCV-genotype at the time of data collection * Includes patients with unspecified (GT1 subtype not determined) or mixed GT1-subtype (>1 GT1 subtypes) † For GT1a-patients with cirrhosis, German guidelines recommend treatment shorting to 12 weeks for patients with defined positive predictors (Viekirax and Exviera SmPC) Reasons for Non-SVR, n (%) 2D / 3D (without RBV) N = 269 2D / 3D (with RBV) N = 289 260 (97) 279 (97) Did not achieve SVR12 9 (3) 10 (3) Virological relapse 5 (2) 1 (0.4) Early D/C (possibly) related to therapy* 2 (0.7)† 5 (2)† Early D/C not related to therapy* 2 (0.7) 4 (1) Achieved SVR12 * Discontinuation (possibly) related to therapy was defined as one or more of the following: on-treatment virologic failure, discontinuation due to AE, patient’s request and inadequate compliance. Discontinuation not related to therapy was defined as follows: loss to follow up before completion of treatment, move of patient, unplanned event (such as incarceration) and other reason. † One patient discontinued, but achieved SVR. Real-world data in co-infected patients Ledipasvir/Sofosbuvir+/-Ribavirin in Patients Co-infected with HCV and HIV: Real-world Heterogeneous Population from the TRIO Network Douglas T. Dieterich1, Bruce Bacon2, Michael Curry3, Steven L. Flamm4, Lauren Guest5, Kris Kowdley6, Yoori Lee5, Zobair Younossi7, NaokyTsai8, and Nezam Afdhal3 1Icahn School of Medicine at Mount Sinai, 2Saint Louis University School of Medicine,3Beth Israel Deaconess Medical Center, 4Northwestern University Feinberg School of Medicine,5Trio Health Analytics, 6Liver Care Network, Swedish Medical Center, 7Center for Liver Diseases, Department of Medicine, InovaFairfax Hospital, and 8Queens Medical Center, University of Hawaii The Trio Network – HIV/HCV coinfection Treating patients with cirrhosis – benefits for all? The evolution of portal pressure after viral suppression with interferon-free therapies and its correlation with the change in liver stiffness Mattias MANDORFER1, 2, Karin KOZBIAL1, Philipp SCHWABL1, 2, Clarissa FREISSMUTH1, Rémy SCHWARZER1, 2, Rafael STERN1, David CHROMY1, Thomas REIBERGER1, 2, Albert F. STÄTTERMAYER1, Wolfgang SIEGHART1, 2, Sandra BEINHARDT1, Michael TRAUNER1, Harald HOFER1, Arnulf FERLITSCH1, 2, Peter FERENCI1, Markus PECK-RADOSAVLJEVIC1, 2 1Division of Gastroenterology and Hepatology, Department of Internal Medicine III, Medical University of Vienna, Vienna, Austria 3Vienna Hepatic Hemodynamic Lab Mattias Mandorfer and Karin Kozbial contributed equally to the work Study flow chart ACLD advanced chronic liver disease; TE transient elastography Results Δ HVPG: Pronounced portal hypertension at BL • No patient resolved portal hypertension • Regression to subclinical portal hypertension in 5% (1/20) • FU HVPG of 10-15 mmHg in 35% (7/20) • Increase in HVPG in 20% (4/20) Real-world efficacy of generic DAAs High sustained virological response rates using generic direct antiviral treatment for Hepatitis C REDEMPTION-1 James Freeman1, Richard Sallie2, Adam Kennedy3, Pham Thi Ngoc Nieu1, John Freeman4, Greg Jeffreys5, Andrew M. Hill6 1GP2U Telehealth, Hobart, 2Hepatology, Nedlands, 3Kingswood Pharmacy, 4Nephrology, Sandy Bay, 5University of Tasmania, Hobart, Australia, 6St Stephens AIDS Trust, Chelsea and Westminster Hospital, London, United Kingdom International Liver Congress 2016 13-18 April, Barcelona, Spain LB03 31 The Deployment Problem Is Price Source: Significant reductions in costs of generic production of sofosbuvir and daclatasvir for treatment of hepatitis C, Hill et al, EASL 2016 32 The Legal Basis Of Personal Importation • Patents provision monopoly rights, however… • Article 60 of TRIPS - De Minimis Imports – states: – Members may exclude from the application of the above provisions small quantities of goods of a noncommercial nature contained in travellers' personal luggage or sent in small consignments • In line with Article 60 most countries allow some form of personal medication importation • http://fixhepc.com/ helps patients access medication and discuss their treatment online 33 Methods • Generic DAAs were first evaluated for quality using HPLC, NMR and Mass Spectrometry • Patients enrolled on an intention to treat basis via the fixhepc.com website and were assisted in making a personal importation of affordably priced medication • Patients were assessed pre-treatment, during treatment, and then for SVR (cure) following treatment using the gp2u.com.au Telemedicine platform • The objective of this analysis was to assess the safety and effectiveness of the generic medications legally imported by patients 34 Over 400 Patients Worldwide Enrolled 35 Baseline Characteristics 36 REDEMPTION-1 HCV RNA < LLOQ at EOT and SVR4 37 REDEMPTION-1 Overall SVR4 Results by Genotype Note: Some small percentage loss of SVR is expected during the SVR4 to SVR12 period 38 Patient Safety • No new or unknown side effects were reported with headache, fatigue and insomnia being the most common • 3 patients with compensated cirrhosis temporarily decompensated on treatment initiation but continued • 4 patients who enrolled died, all from HCC – 1 patient died prior to treatment commencement – 2 withdrew early in treatment and entered palliative care – 1 patient died prior to SVR4 39 Summary • In this interim analysis, treatment with legally imported generic DAAs led to high SVR rates • These SVR rates are similar to those seen in the Phase 3 trials of branded treatments • Mass global treatment with generic DAAs is a feasible alternative where high prices prevent access to branded treatment 40 HCV Re-infection in HIV+ in Europe Hepatitis C virus reinfection incidence and outcomes among HIV-positive MSM in Western Europe Thomas Martin MD On behalf of: Ingiliz P, Martin TCS, Rodger A, Stellbrink HJ, Mauss S, Boesecke C, Mandorfer M, Bottero J, Baumgarten A, Bhagani S, Lacombe K, Nelson M, Rockstroh JK and the NEAT study group Reinfection with HCV after treatment or spontaneous clearance occurs often • Reinfection with HCV – Amsterdam 15.2/100py – London 8.0/100py • Reinfection is important for a number of reasons – Could affect cost/benefit of treatment with expensive DAAs – Could demonstrate a need for additional education/prevention interventions – Supports ongoing screening for HCV after successful treatment – People with reinfection may be at greater risk of transmission of infection including HIV 1. Lambers FAE et al. Alarming incidence of hepatitis C virus re-infection after treatment of sexually acquired acute hepa- titis C virus infection in HIV-infected MSM. AIDS (London, England) 2011; 25:F21–F27. 2. Martin TCS et al. Hepatitis C virus reinfection incidence and treatment outcome among HIV-positive MSM. AIDS 2013, 27:2551-2557 HCV reinfection among HIV positive MSM in Western Europe • Aims: – Primary: to calculate reinfection incidence among the European AIDS Treatment Network (NEAT) consortium centres in Western Europe (UK, Germany, Austria and France) – Secondary: to look for factors associated with reinfection and spontaneous clearance of reinfection HCV reinfection among HIV positive MSM in Western Europe • Analysis: – Reinfection definition: newly positive HCV PCR any time after cure or earlier if HCV geno-/subtype switch occurred – Start of from end of treatment for those treated and the first negative HCV PCR for people who spontaneously clear – Date of reinfection taken as first newly positive HCV PCR – End of follow up - last negative HCV PCR • Kaplan Meier survival methods. • Comparison using log-rank and Cox proportional hazards • Multiple logistic regression to assess factors associated with spontaneous clearance of reinfection Overall population Incident infection 1st Reinfection Number included 606 606 Number reinfected (%) N/A 149 (24.6) Median time (years) to reinfection (IQR) N/A 1.8 (1.1-3.2) Genotypes (%) GT1: GT2: GT3: GT4: Genotype switches (%) N/A 71/136 (52.2) Median age at reinfection (IQR) 39 (34-44) 41 (37-45) Median HIV duration at infection (only data for patients that were reinfected) (IQR) Median CD4 at reinfection 5 (2-11) 9 (6-14) Proportion with suppressed HIV VL SC proportion 376(70.5) 13(2.4) 46(8.6) 96 (18) GT1: GT2: GT3: GT4: 104(73.2) 1(0.7) 12(8.5) 25(17.6) 553 (412-760) 91/111 (82.0%) 111/605 (18.3%) 21/135 (15.6%) (failed treatment not in denominator) 113 treated with 87 achieving SVR (78%) Overall population 2nd Reinfection 3rd reinfection 4th reinfection Number included 69 13 2 Number reinfected (%) 29 (42.0) 4 (30.8) 1 (50) Median time (years) to reinfection (IQR) 1.7 (1.2-2.4) Genotypes (%) GT1: GT2: GT3: GT4: GT1: GT2: GT3: GT4: GT1: GT2: GT3: GT4: Genotype switches (%) 13/25 (52.0) 2/4 (50) 1/1 (100) Median age at reinfection (IQR) 43 (40-49) - - SC proportion 6/21 (28.6%) 1/3 (33.3%) 0/1 (0%) 22(84.6) 0 1(3.8) 3(11.5) 3(75) 0 0 1(25) 1 (100) 0 0 0 HCV reinfection incidence is high Reinfection incidence of 7.6/100py (95% CI 6.3-9.1) [1583 py f/u with 121 reinfections] 2nd Reinfection incidence is even higher than 1st reinfection 19.9/100py (95% CI 13.3-29.7) HR 2.59 (95% CI 1.67- 4.03) Reinfection following spontaneous clearance is reduced compared to treatment HR 0.55 (95% CI 0.32-0.95) Reinfection incidence by location Associations with spontaneous clearance of reinfection Variable OR 95% CI P-value HCV VL ≥500000 0.5 0.1 – 1.9 0.28 CD4 ≥ 500 cells/ml 0.7 0.2 - 2.6 0.55 Max ALT reinfection ≥1000 IU/ml 19.6 3.6-105.8 0.001 Max ALT initial infection ≥ 1000 IU/ml 0.6 0.1 – 3.2 0.53 Spontaneous clearance of initial infection 12.7 2.3 – 70.2 0.004 HIV VL detectable 0.3 0.4 – 1.4 0.11 Age ≥30 3.7 0.8 – 17.6 0.10 Conclusions • Substantial HCV reinfection risk among HIV/HCV coninfected MSM – 7.6/100 py with 25% reinfected at 3 years • Failure of current prevention interventions – Urgently need prevention strategies • Importance of rapid identification and treatment to prevent transmission of HCV or HIV – Suggest 3-6 month testing with HCV RNA PCR after initial infection – And every 3 months after a HCV reinfection • Spontaneous clearance associated with reduced risk of reinfection (HR 0.55) and increased chance of spontaneous clearance if reinfected (OR 12.7) Can short-duration DAA-based therapy be used for acute/early HCV infection? New drugs for G3? DAA failures? High Efficacy of Sofosbuvir/Velpatasvir Plus GS9857 for 12 Weeks in Treatment-Experienced Genotype 1–6 HCV-Infected Patients, Including Those Previously Treated With Direct-Acting Antivirals Eric Lawitz1, Kris Kowdley2, Michael Curry3, Nancy Reau4, Mindie Nguyen5, Paul Kwo6, Ira Jacobson7, Tram T. Tran8, Ronald Nahass9, Federico Hinestrosa10, Robert Herring Jr.11, Michael Bennet12, Jenny C. Yang13, Luisa M. Stamm13, Di An13, Hadas Dvory-Sobol13, Diana M. Brainard13, John G. McHutchison13, Eugene Schiff14, Mitchell Davis15, Kyle Etzkorn16, Raymond T. Chung17, David Pound18, Maribel Rodriguez-Torres19, K. Rajender Reddy20, Ziad Younes21, Edward J.Gane22 1Texas Liver Institute, San Antonio, Texas, USA; 2Swedish Medical, Seattle, Washington, USA; 3Beth Israel Deaconess Medical Center, Boston, Massachusetts, USA; 4Rush University Medical Center, Chicago, Illinois, USA; 5Stanford University, Palo Alto, California, USA; 6Indiana University School of Medicine, Indianapolis, USA; 7Mount Sinai Beth Israel, New York, USA; 8Cedars Sinai Medical Center, Los Angeles, California; 9ID Care, Hillsborough, New Jersey, USA; 10Orlando Immunology Center, Florida, USA; 11Nashville Gastrointestinal Specialists Inc., Tennessee, USA; 12Medical Associates Research Group, Inc., San Diego, California; 13Gilead Sciences, Inc., Foster City, California; 14University of Miami, Florida, USA; 15Digestive CARE-South Florida Center of Gastroenterology, Wellington, Florida, USA; 16Borland-Groover Clinic, Jacksonville, Florida, USA; 17Massachusetts General Hospital, Boston, Massachusetts; 18Indianapolis Gastroenterology Research Foundation, Indianapolis, Indiana, USA; 19Fundación De Investigación De Diego, San Juan, Puerto Rico; 20University of Pennsylvania , Philadelphia, USA; 21Gastro One, Germantown, Tennessee, USA; 22Auckland Clinical Studies, New Zealand EASL 2016, Barcelona Study Designs GS-US-367-1168 and GS-US-367-1169 Week 0 12 N=128 SOF/VEL + GS-9857 24 SVR12 • Two Phase 2, multicenter, open-label studies (US, New Zealand) – GS-US-367-1168: GT 1 – GS-US-367-1169: GT 2, 3, 4, 5, 6 • Broad inclusion criteria – HCV treatment experienced, including DAA experienced • GT 1: NS5A inhibitor or ≥2 DAA classes • GT 2–6: Peg-IFN + RBV or any DAA – 50% with compensated cirrhosis 71 Results: Demographics and Baseline Characteristics SOF/VEL + GS-9857 12 weeks N=128 Mean age, y (range) 58 (37–77) Male, n (%) 96 (75) White, n (%) 105 (82) Mean BMI, kg/m2 (range) 29 (18-53) IL28B non-CC, n (%) 93 (73) Cirrhosis, n (%) 61 (48) Mean HCV RNA, log10 IU/mL (range) 6.3 (3.8–8.1) HCV GT, n (%) 1 63 (49) 2 21 (16) 3 35 (27) 4, 6 9 (7) DAA experience, n (%) None (GT 2-6 only) 27 (21) 1 DAA class 36 (28) ≥2 DAA classes 65 (51) 72