* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Respiratory PPT part
Hemolytic-uremic syndrome wikipedia , lookup
Schmerber v. California wikipedia , lookup
Blood transfusion wikipedia , lookup
Autotransfusion wikipedia , lookup
Blood donation wikipedia , lookup
Plateletpheresis wikipedia , lookup
Jehovah's Witnesses and blood transfusions wikipedia , lookup
Men who have sex with men blood donor controversy wikipedia , lookup
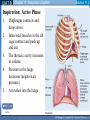
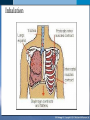
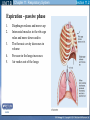
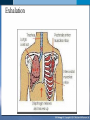
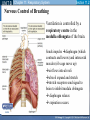
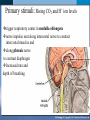
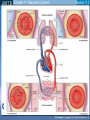
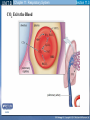
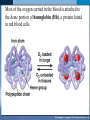
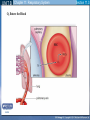
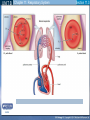
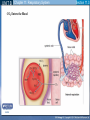
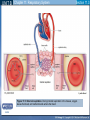
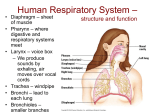
Mechanism of Breathing UNIT B Chapter 11: Respiratory System Inspiration: Active Phase 1. 2. 3. 4. 5. Diaphragm contracts and drops down Intercostal muscles in the rib cage contract and push up and out The thoracic cavity increases in volume Pressure in the lungs decreases (negative air pressure) Air rushes into the lungs TO PREVIOUS SLIDE Section 11.2 Inhalation UNIT B Chapter 11: Respiratory System Expiration - passive phase 1. 2. 3. 4. 5. TO PREVIOUS SLIDE Diaphragm relaxes and moves up Intercostal muscles in the rib cage relax and move down and in The thoracic cavity decreases in volume Pressure in the lungs increases Air rushes out of the lungs Section 11.2 Exhalation Features of Thoracic Cavity For breathing to occur, the thoracic cavity must be airtight: 1. The interior of the thoracic cavity is lined with an airtight membrane called the parietal pleura 2. Each lung is surrounded with an air-tight membrane called the visceral pleura 3. The space between the two pleura (interpleural cavity) contains a lubricant 4. The muscular diaphragm seals the bottom of the thoracic cavity UNIT B Chapter 11: Respiratory System Section 11.2 Nervous Control of Breathing Ventilation is controlled by a respiratory centre in the medulla oblongata of the brain. Sends impulse diaphragm (which contracts and lowers) and intercostal muscles (rib cage move up) air flows into alveoli alveoli expand and stretch stretch receptors send signal to brain to inhibit medula oblongata diaphragm relaxes expiration occurs. TO PREVIOUS SLIDE Primary stimuli: Rising CO2 and H+ ion levels trigger respiratory center in medulla oblongata nerve impulse sent along intercostal nerve to contract intercostal muscles and along phrenic nerve to contract diaphragm Increased rate and depth of breathing Secondary stimuli for Breathing: Decreasing O2 levels trigger chemoreceptors in carotid bodies of carotid arteries and aortic bodies of aorta nerve impulse to respiratory center of medulla oblongata UNIT B Chapter 11: Respiratory System Section 11.3 Gas Exchanges in the Body Respiration includes: 1. External respiration: exchange of gases in the lungs 2. Internal respiration: exchange of gases in the tissues TO PREVIOUS SLIDE Movement of CO2 Carbon dioxide molecules are transported in the blood from body tissues to the lungs by one of three methods: 1. Dissolution directly into the blood (Partial pressure, capillaries and alveoli are both one cell layer thick) 2. Binding to hemoglobin (carbaminohemaglobin) 3. Carried as a bicarbonate ion. – CO2 diffuses into RBC. Carbonic Anhydrases converts it to carbonic acid H2CO3. UNIT B Chapter 11: Respiratory System Section 11.3 External Respiration • Exchange of gases between air (alveoli) blood (pulmonary capillaries) • Both are one cell thick • Gas exchange is by diffusion alone • CO2 leaves the blood, and O2 enters the blood. TO PREVIOUS SLIDE Gas Exchange: CO2 • Partial pressure of CO2 in plasma > atmospheric pressure • So CO2 diffuses out of blood to lungs • CO2 in plasma is carried as bicarbonate ion • As CO2 diffuses out of plasma, carbonic anhydrase speeds up break down carbonic acid, driving reaction to right UNIT B Chapter 11: Respiratory System TO PREVIOUS SLIDE Section 11.3 UNIT B Chapter 11: Respiratory System CO2 Exits the Blood TO PREVIOUS SLIDE Section 11.3 UNIT B Chapter 11: Respiratory System Section 11.3 Gas Exchange: O2 o Blood returning from the systemic capillaries has a lower partial pressure of O2 (PO2) than the air in the alveoli o O2 diffuses into plasma and then into red blood cells o Hemoglobin takes up O2 and becomes oxyhemoglobin (HbO2) o Hemoglobin has a higher affinity for O2 at lower temperatures and higher pH o Why is O2 transported via hemoglobin? TO PREVIOUS SLIDE Most of the oxygen carried in the blood is attached to the heme portion of hemoglobin (Hb), a protein found in red blood cells. UNIT B Chapter 11: Respiratory System O2 Enters the Blood TO PREVIOUS SLIDE Section 11.3 Carbon Monoxide Difficult to detect: Colourless, odorless gas. Lighter than air. Lowers Oxygen delivery: Binds to hemoglobin with greater affinity than oxygen. Longer the exposure, the more sites taken up, less oxygen getting to tissues, leading to possible death of tissues. Long clearing time: 4-6 hr Produced by burning gas, wood, propane, charcoal or other fuel UNIT B Chapter 11: Respiratory System TO PREVIOUS SLIDE Section 11.3 UNIT B Chapter 11: Respiratory System Section 11.3 Internal Respiration: Exchange of gases between the blood (systemic capillaries) and tissue fluid. • O2 leaves the blood, and CO2 enters the blood. • Tissues have a higher temperature and lower pH, and the partial pressure of O2 (PO2) in tissue fluid is lower than in blood o Therefore, oxyhemoglobin gives up O2, which diffuses out of the blood into the tissues: TO PREVIOUS SLIDE UNIT B Chapter 11: Respiratory System Section 11.3 CO2 diffuses into the blood from the tissues because the PCO2 of tissue fluid is higher than in blood – About 10% CO2 is taken up by hemoglobin = carbaminohemoglobin (HbCO2) o The remaining CO2 combines with water in the plasma, forming carbonic acid (H2CO3), which dissociates into hydrogen ions (H+) and bicarbonate ions (HCO3-). o The increased concentration of CO2 in the blood drives the reaction to the right TO PREVIOUS SLIDE UNIT B Chapter 11: Respiratory System Section 11.3 o The globin portion of hemoglobin combines with excess H+ to become reduced hemoglobin (HHb), darker in color − Carbon monoxide (CO) poisoning occurs because it has a greater affinity for hemoglobin than O2, stays combined for hours TO PREVIOUS SLIDE UNIT B Chapter 11: Respiratory System CO2 Enters the Blood TO PREVIOUS SLIDE Section 11.3 UNIT B Chapter 11: Respiratory System Section 11.3 Figure 11.10 Internal respiration. During internal respiration in the tissues, oxygen leaves the blood, and carbon dioxide enters the blood. TO PREVIOUS SLIDE Binding Capacity of Hemoglobin affected by pH and Temperature Cooler temperature (37 C) and higher pH (7.40) of lungs raises oxygen binding capacity of hemoglobin to 98% optimal binding of Hb and O2 in lungs where it is cooler and less acidic Warmer temperature (38 C) and lower pH (7.38) of body cells lowers the oxygen binding capacity of hemoglobin to 60% Hb will release oxygen to tissue where its warmer and more acidic 15-27 Saturation of Hb relative to temperature temperature 15-28 Saturation of Hb relative to pH Check your progress 1. Explain the role of hemoglobin. 2. Discuss why arterial blood is bright red in colour, but venous blood is darker. This being the case, why does blood oozing from a cut always appear to be bright red? 3. Explain why carbon monoxide poisoning can be rapidly fatal. 4. How is CO2 transported? 5. What is reduced hemoglobin? Blood pH The pH of the blood is normally 7.35 to 7.45 – a narrow range. During exercise, the concentration of carbon dioxide in the blood and respiring tissues increases. This could lower the pH (making the blood more acidic). To prevent this happening: substances in blood plasma react with the excess carbon dioxide increases in the rate and depth of breathing speed up the rate at which carbon dioxide is removed from the bloodstream