* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download PDF
Visual impairment wikipedia , lookup
Fundus photography wikipedia , lookup
Idiopathic intracranial hypertension wikipedia , lookup
Dry eye syndrome wikipedia , lookup
Mitochondrial optic neuropathies wikipedia , lookup
Eyeglass prescription wikipedia , lookup
Visual impairment due to intracranial pressure wikipedia , lookup
Blast-related ocular trauma wikipedia , lookup
Corneal transplantation wikipedia , lookup
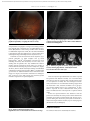
Document downloaded from http://www.elsevier.es, day 03/05/2017. This copy is for personal use. Any transmission of this document by any media or format is strictly prohibited. a r c h s o c e s p o f t a l m o l . 2 0 1 4;8 9(6):235–238 ARCHIVOS DE LA SOCIEDAD ESPAÑOLA DE OFTALMOLOGÍA www.elsevier.es/oftalmologia Short communication Bilateral persistent hyaloid artery. A case report夽 A.M. Borbolla-Pertierra a,∗ , C.K. Martínez-Hernández b , J.C. Juárez-Echenique a a b Instituto Nacional de Pediatría, Mexico City, Mexico Hospital General Manuel Gea González, Mexico City, Mexico a r t i c l e i n f o a b s t r a c t Article history: Case report: A 5-year-old male presented with bilateral poor vision, esotropia and a previous Received 11 December 2012 diagnosis of cataract since he was 1 year old. The physical examination revealed bilateral Accepted 27 May 2013 posterior paracentric capsule opacification, vitreous cavity with a permeable pulsatile blood Available online 13 August 2014 filled hyaloid artery in both eyes. He was kept under observation. Keywords: often unilateral (although it may be bilateral) and sporadic, associated with microphthal- Persistent hyaloid artery mos. It may be complicated with glaucoma and phthisis bulbi. Vitrectomy plus lensectomy Cataract or simple observation is the accepted treatment option. Discussion: Persistent hyaloid artery is an uncommon faulty primary vitreous regression, Microphthalmos © 2012 Sociedad Española de Oftalmología. Published by Elsevier España, S.L.U. All rights reserved. Vitreous body Congenital abnormality Persistencia bilateral de la arteria hialoidea. Reporte de un caso r e s u m e n Palabras clave: Caso clínico: Varón de 5 años de edad con mala visión bilateral, endotropía y diagnóstico Persistencia de la arteria hialoidea previo de catarata desde el año de edad. En la exploración, se observa en ambos ojos opacidad Catarata capsular posterior paracentral, cavidad vítrea con arteria hialoidea permeable, ocupada por Microftalmos sangre y con pulso. Se dejó en vigilancia. Cuerpo vítreo Discusión: La persistencia de la arteria hialoidea es infrecuente y es una falla en la involución Anomalía congénita del vítreo primario. Comúnmente es unilateral (aunque hay casos bilaterales), esporádico y asociado a microftalmos. Puede complicarse con glaucoma y pthisis bulbi. Vitrectomía más lensectomía u observación son opciones de tratamiento según el caso. © 2012 Sociedad Española de Oftalmología. Publicado por Elsevier España, S.L.U. Todos los derechos reservados. Please cite this article as: Borbolla-Pertierra AM, Martínez-Hernández CK, Juárez-Echenique JC. Persistencia bilateral de la arteria hialoidea. Reporte de un caso. Arch Soc Esp Oftalmol. 2014;89:235–238. ∗ Corresponding author. E-mail address: [email protected] (A.M. Borbolla-Pertierra). 夽 2173-5794/$ – see front matter © 2012 Sociedad Española de Oftalmología. Published by Elsevier España, S.L.U. All rights reserved. Document downloaded from http://www.elsevier.es, day 03/05/2017. This copy is for personal use. Any transmission of this document by any media or format is strictly prohibited. 236 a r c h s o c e s p o f t a l m o l . 2 0 1 4;8 9(6):235–238 Case report Male patient, age 5, whose mother reported having chickenpox in the fifth month of pregnancy, consulted for poor vision, inward ocular deviation and bilateral cataract since he was 12 months old. Physical examination produced a visual acuity of no light perception in right eye (RE) and 20/200 in left eye (LE). The following were observed: Refraction: RE +2.00 with −7.25 × 90, LE +1.00 with −5.25 × 70, without achieving visual improvement; endotropia of 25 prismatic diopters, normal duction and version; ocular posterior capsular opacity in both lenses and retrolental tissue in RE (Fig. 1); open iridocorneal angles and intraocular pressure of 15 mmHg in both eyes (BE); vitreous cavity of BE with functional vascular canal from the papilla to the lens, presence of pulse, small and pale optic nerves with coloboma-type defect, hypopigmented macular chorioretinal scar of about 2 papillar diameters in RE (Figs. 2 and 3). Fluorangiography: fetal vessels filled with fluorescein, demonstrating functionality (Figs. 4 and 5). Magnetic resonance: hypotensive central hyaloid canal in T2 projection (Fig. 6). It was decided to maintain the patient under observation. Discussion The persistence of fetal vessels, also known as persistence of hyaloid artery or persistent hyperplastic primary vitreous (PHPV), is a rare congenital anomaly generally of unknown cause. Most cases exhibit retrolental plate in a microphthalmic eye.1 It was initially described as a syndrome by Reese in 1955.2 The defect consists in failed primary vitreous regression.2 The hyaloid artery is formed on the basis of mesenchymatous cells which gained access through the optic fissure.3 This artery surrounds the lens contributing to form the tunica vasculosa lentis.3 Complete primary vitreous regression must take place between the seventh and eighth month of gestation.3 It is anatomically classified on the basis of anterior or posterior primary vitreous persistence. PHPV is the second most common cause of acquired cataract during the first year of life.4 It is most frequently Fig. 2 – Right eye ocular fundus. Tissue beginning in the papilla and partially occupying the vitreous cavity, macular chorioretinal scar with central hyperpigmentation areas and RPE atrophy at the lesion edges. Choroidal vessels can be seen. diagnosed during the first year of life and no relevant familial history has been identified.5 With greater frequency it is unilateral although it can express bilaterally in up to 11%2,5 of cases and is associated to microphthalmos in 2/3 of patients5 . It expresses mainly with leukocoria, which requires differential diagnosis with cataracts, retinoblastoma, retinopathy of prematurity, posterior uveitis and Coats disease, among others.4 Natural history is toward recurring vitreous hemorrhage, retina detachment, uncontrollable secondary glaucoma and phtisis bulbi, for which reason its only treatment on some occasions is enucleation4 . Diagnostic can be clinical. However, A-B mode echography is essential particularly in the presence of opacity, exhibiting a stem from the posterior pole to the lens, in addition to discarding or confirming the presence of microphthalmos or associated retina detachment.5 Color Doppler echography helps to confirm the vascular nature of the lesion.4 Fig. 1 – Microscopic image of anterior segment of both eyes. Superior opacity behind both lenses and presence of retrolental tissue visible in the right eye (left side). Document downloaded from http://www.elsevier.es, day 03/05/2017. This copy is for personal use. Any transmission of this document by any media or format is strictly prohibited. a r c h s o c e s p o f t a l m o l . 2 0 1 4;8 9(6):235–238 Fig. 3 – Left eye ocular fundus. Tissue beginning in the papilla and partialLy occupying the vitreous cavity. Computerized tomography is useful for discarding calcification although this is extremely rare4 in PHPV. Magnetic resonance (MR) enables a clearer image of PHPV and is excellent for differential diagnostics. In MR, the retrolental membrane is hyperintense after the application of contrast and shows a tube-shaped image which represents the hyaloid vessel.6 Treatment is controversial and has three objectives: (1) to prevent glaucoma, (2) pupil esthetics and (3) visual improvement.5 Pollord4 and Haddad5 reported long series including vitrectomy and lensectomy in some cases, concluding that the patients who only exhibited the anterior primary vitreous persistence variety have good results, in contrast with those having the posterior variety who, despite all efforts, did not obtain visual improvements and exhibited complications with greater frequency. Mittra7 concluded that good results are obtained with the latest vitreoretinal techniques for surgery and intensive treatment for amblyopia. Sisk8 treated 81 cases with surgery and observed greater incidence of glaucoma in operated patients. Fig. 5 – Left eye fluorangiography at 4:17 min. Persistence of hyaloid artery hyperfluorescence with contrast diffusion toward surrounding tissue. Fig. 6 – Orbitary magnetic resonance, T2 projection, axial section, showing hypointense central hyaloid canal vis-à-vis the vitreous in both eyes. There are very few reported bilateral cases. Hunt9 reported five patients with bilateral anomaly out of 55 with PHPV, and reported only two patients with isolated hyaloid artery as sole expression of PHPV, who were managed conservatively. Said author also recommended avoiding surgery when the visual axis is free, anatomic anomalies are not progressive and the chamber angle is not compromised.9 In turn, Kumar10 reported 11 cases of bilateral fetal vessel persistence and indicated this could represent a separate clinical entity. In the case reported herein it was decided to treat the patient conservatively due to the presence of blood flow in the remaining vessel (vitreous hemorrhage risk), absence of progression during the observation period, lack of alteration of iridocorneal angles and the certainty of poor visual prognosis (RE macular scar, LE amblyopia). Conflict of interest Fig. 4 – Right eye fluorangiography at 40 s. Hyperfluorescence of the macular chorioretinal scar edge. 237 No conflict of interest was declared by the authors. Document downloaded from http://www.elsevier.es, day 03/05/2017. This copy is for personal use. Any transmission of this document by any media or format is strictly prohibited. 238 a r c h s o c e s p o f t a l m o l . 2 0 1 4;8 9(6):235–238 references 1. Lambert SR. Chilhood cataracts. In: Hoyt C, Taylor D, editors. Pediatric ophthalmology and strabismus. 4th ed. Elsevier; 2013. p. 341–2. 2. Reese AB. Persistent hyperplastic primary vitreous. Jackson Memorial Lecture. Trans Am Acad Ophthalmol Otolaryngol. 1955;59:271–86. 3. Cook CS. Embriology. In: Wright KW, editor. Handbook of pediatric eye and systemic disease. 2nd ed. New York: Springer; 2006. p. 19–20. 4. Pollord Z. Persistent hyperplastic primary vitreous: diagnosis, treatment and results. Trans Am Ophthalmol Soc. 1997;XCV:487–549. 5. Haddad R, Font RL, Reeser F. Persistent hyperplastic primary vitreous. A clinicopathologic study of 62 cases and review of the literature. Surv Ophthalmol. 1978;23:123–34. 6. Sun MH, Kao LY, Kuo YH. Persistent hyperplastic primary vitreous: magnetic resonance imaging and clinical findings. Chang Gung Med J. 2003;26:269–76. 7. Mittra RA, Huynh LT, Ruttum MS, Mieler WF, Connor TB, Han DP, et al. Visual outcomes following lensectomy and victrectomy for combined anterior and posterior persistent hyperplastic primary vitreous. Arch Ophthalmol. 1998;116:1190–4. 8. Sisk RA, Berrocal AM, Feuer WJ, Murray TG. Visual and anatomic outcomes with or without surgery in persistent fetal vasculature. Ophthalmology. 2010;117: 2178–83. 9. Hunt A, Rowe N, Lam A, Martin F. Outcomes in persistent hyperplastic primary vitreous. Br J Ophthalmol. 2005;89:859–63. 10. Kumar A, Jethani J, Shetty S, Vijayalakshmi P. Bilateral persistent fetal vasculature: a study of 11 cases. J AAPOS. 2010;14:345–8.