* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Thought Content - International Panel Physicians Association
Survey
Document related concepts
Psychological trauma wikipedia , lookup
Combat stress reaction wikipedia , lookup
Eating disorder wikipedia , lookup
Spectrum disorder wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
Glossary of psychiatry wikipedia , lookup
Child psychopathology wikipedia , lookup
Externalizing disorders wikipedia , lookup
Mental disorder wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Mentalism (discrimination) wikipedia , lookup
Pyotr Gannushkin wikipedia , lookup
Transcript
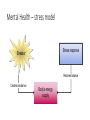
Mental Health Paul Douglas March 30 2017 Purpose of session - Highlight the importance of the mental health assessment as part of the overall Immigration Medical Examination (IME) - How to carry out a Mental Status Evaluation (MSE) - Symptoms and signs to look out for in migrants with mental disorders and substance use disorders - Who may need further assessment Overview of session • Why it is important to know about mental health • What is mental health? • Classifications of mental disorder • Assessment of mental health • Special considerations for travel Mental health context for IME - Dimension of the problem Mental Health - context • Quick Quiz Mental health context for IME - Dimension of the problem - Stress Mental Health - stress • Stress is a condition or feeling experienced when a person perceives that demands exceed the personal and social resources the individual is able to mobilise. • Stress is the physiological response of the body to physical and psychological demands. • The level of stress experienced depends on individual reactions to a situation • The source of stress, or stressor, can be either real or imagined • People feel little stress when they have the time, experience and resources to manage a situation. • They feel great stress when they think they can't handle the demands • Stress is therefore MOSTLY a negative experience. Mental Health – stress sources 1. Psychological stressors can be: • Stressors that cause frustration (blocked from reaching a goal) • Stressors that cause pressure (responsibilities that tax your abilities) • Stressors that cause conflict (torn between two or more courses of action) 2. Causes: • Work-related – demands, role ambiguities or conflicts, ethical dilemmas, interpersonal problems, career development, physical settings • Personal - family events, economic difficulties, individual’s needs, capabilities and/or personality 3. Signs: • Physical – headache, back pain, fatigue, aches and pains • Mental - difficulty concentrating, increased errors, poor decision making Mental Health – stress individual consequences Psychological • • • • • • • Anxiety Depression Low self-esteem Sleeplessness Frustration Family problems Burnout Stress Behavioural • • • • • Excessive smoking Substance abuse Accident proneness Appetite disorders Violence Physiological • • • • • • High blood pressure Muscle tension Headaches Ulcers Skin diseases Impaired immune systems • Musculoskeletal disorders • Heart disease • Cancer Mental Health - stress MYTHS ABOUT STRESS: • All stress is bad • Stress will not hurt you • What stresses you out also stresses me out • No symptoms, no stress • Only major symptoms of stress are harmful Stress Model Mental Health – stress model Stress response Stressor Restores balance Creates imbalance Body’s energy supply Mental health context for IME - Dimension of the problem - Stress – Is NOT an issue for IME!!!!! (unless…….) - Country requirements and assistance for settlement Mental health context for IME • While the USA is the only country that the legislation specifies inadmissibility for mental disorders with associated harmful behaviour, • it is just as relevant to other countries where for : • Australia – danger to community and cost [our regulation covered by 4005(b)(c)] • Canada –similar to Australia (threat to public safety and/or excessive demand) • New Zealand – cost?? • United Kingdom – relevant to refugee population mainly for resettlement purposes (piloting the GMHAT tool) • Assist in settlement – Australia’s new tool in eMedical for refugees Mental Health - definitions • Mental health is defined as a state of well-being in which every individual : • • • • realises his or her own potential, can cope with the normal stresses of life, can work productively and fruitfully, and is able to make a contribution to his or her community1 • "Health is a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity.“ – positive aspects • Mental disorders are generally characterised by some combination of abnormal thoughts, emotions, behaviour and relationships with others. www.who.int/topics/mental_disorders/ Mental disorder are peculiar • Affect mood, emotions & thinking ultimately leading to change in behaviour. • May be inappropriate or harmful behaviour, posing risk to public safety. • Chronic in nature, requiring long-term follow up • May be functionally debilitating and incapacitating, requiring institutionalisation or special therapies (speech, occupational therapies, special schooling, vocational skills training) and can be huge burden to health care systems. • No biological markers…. Mental Disorders • Governed by two systems of Classification: • DSM - American Psychiatric Association (APA) • ICD – World Health Organization (WHO) • The classification of mental disorders, (psychiatric nosology or psychiatric taxonomy), groups symptomatology into various clusters of criteria leading to diagnosis of various disorders. • Allows international consistency and standardisation International Classification of Diseases (Chap. V) • • • • • F0: Organic, including symptomatic, mental disorders F1: Mental and behavioural disorders due to use of psychoactive substances F2: Schizophrenia, schizotypal and delusional disorders F3: Mood [affective] disorders F4: Neurotic, stress-related and somatoform disorders • F5: Behavioural syndromes associated with physiological disturbances and physical factors • F6: Disorders of personality and behaviour in adult persons • F7: Mental retardation • F8: Disorders of psychological development • F9: Behavioural and emotional disorders with onset usually occurring in childhood and adolescence In addition, a group of "unspecified mental disorders". Diagnostic and Statistical Manual (DSM-5) • Neurodevelopmental Disorders • Schizophrenia Spectrum and Other Psychotic Disorders • Bipolar and Related Disorders • Depressive Disorders • Anxiety Disorders • Obsessive-Compulsive and Related Disorders • Trauma- and Stressor-Related Disorders • Dissociative Disorders • Somatic Symptom Disorders • • • • • • Feeding and Eating Disorders Elimination Disorders Sleep-Wake Disorders Sexual Dysfunctions Gender Dysphoria Disruptive, Impulse Control and Conduct Disorders • Substance Use and Addictive Disorders • Neurocognitive Disorders • Personality Disorders • Paraphilic Disorders • Other Disorders Other categorisations of mental illness? • Can be an illness (patient perception) or disease (medical diagnosis) of the mind. • It is also the psychological state of someone who has emotional or behavioural problems • Types of Mental Illness: • Mood disorders, eating disorders, anxiety disorders, psychotic disorders, substance dependency, organic disorders, development disorders and personality disorders • Causes of Mental Illness: • Genetics, infections, long term Substance Abuse https://prezi.com/ Detecting mental health concerns? • Observation through process of IME • History • Exam • Tools/screening • Further assessments (specialists/tests) Mental Health assessment - observation Mental health evaluation begins at the first point of contact • All staff including security, administrative, laboratory personnel etc., • Trained and sensitised on specific indicators to observe • appearance, • attitude • behaviour Some observations that may indicate a problem include: unkempt, withdrawn, mute, restless, agitated, confused and aggressive If abnormal behaviour identified, this should be reported to Panel Physician and ensure safety of applicant and other clients if required Mental Health assessment - history Starts with general data such as name, age, gender, marital status, occupation, religious affiliation etc. If history of a mental disorder: • Symptoms – onset; duration; precipitating event; change over time, • Impacts on the applicant’s life activities i.e. work, important relationships and extent of incapacity • The nature of dysfunction e.g. changes in personality, memory or speech • Presence of any harmful behaviours • Type of treatment received and compliance (including hospitalisation and medication) • Family history • Note: medical conditions mistaken for a primary psychiatric disorder (e.g. hypothyroidism treated with steroids can lead to mania) Mental Health – history specific enquiry 1. 2. 3. 4. Pre and perinatal history. Early developmental history (developmental milestones) Middle childhood (3-11 years). Adolescent period: a. b. c. 5. 6. 7. 8. Behaviours and social activities School history Cognitive and motor development Emotional and social development/issues Young adulthood especially occupational Marital and social Alcohol and substance abuse (Military, Legal, Schooling, Employment, Sexual, Drugs….) Mental Health – alcohol and substance abuse • Which substance is used, how much, how frequently? • Is an increasing amount of the substance required to achieve the ‘high’? • Is there compulsive long-term use of the substance despite significant substance-related physical, psychological, social, occupational or behavioural problems? • Are there any adverse effects suffered when the use of the substance is reduced or stopped? Cage questionnaire (alcohol dependency suspected > 2): 1. 2. 3. 4. Have you ever felt that you should Cut down on your drinking? Have people ever Annoyed you by criticising your drinking Have you ever felt bad or Guilty about drinking? Have you ever taken a drink first thing in the morning (Eye-opener) to steady your nerves or get rid of the hangover? Mental status examination (MSE) Following history should conduct an “activities assessment” - ability to carry out functions of daily living • Practical skills: o bathing/washing, dressing, feeding/drinking, o personal care such as bladder and bowel control (is there urine or stool incontinence?) • Conceptual skills: o learning difficulties; is special schooling required? o special considerations for job placement? o conceptual skills such as language, problem-solving, money and time management? • Social skills: o communication difficulties; o can they live alone? Mental status examination (MSE) 1. Appearance 2. Attitude (towards the examiner ) 3. Behaviour and psychomotor activity 4. Speech 5. Mood and affect 6. Perception 7. Thought processes 8. Thought content 9. Alertness and cognition Mental status examination (MSE) Appearance: • Body type, posture, poise, clothes, grooming • Anxiety (moist hands, perspiring forehead, tense posture and wide eyes). Attitude (towards the examiner ) • Cooperative, friendly, attentive, interested, frank, seductive, defensive, contemptuous, perplexed, apathetic, hostile, playful, ingratiating, evasive or guarded • Establishment of rapport? Behaviour and psychomotor activity • Unusual mannerisms - tics, gestures, twitches, stereotyped behaviour, echopraxia (pathological imitation of movements), hyperactivity, agitation or restlessness, combativeness, rigidity, agility, wringing of the hands, pacing, psychomotor retardation (generalised slowing of movements which occurs in depressive states). Mental status examination (MSE) Speech: • Rate (rapid, slow, halting) • Amount /quantity (taciturn - untalkative, lacking spontaneity, grandiose) • Tone (monotone, singsong, slurred) • Speech impairment (dysarthria, echolalia, stuttering) • Aphasia Note - depressed patients tend to speak in a low monotone and may give monosyllabic answers to questions. They also tend to avoid eye contact Mental status examination (MSE) Mood and Affect: • Mood - emotion that colours the person’s perception of the world: o Depth o Intensity o Duration o Fluctuations • Affect - present emotional responsiveness, inferred from facial expression: o Normal (variation of facial expression, tone of voice, use of hands and body movements) o Constricted - range and intensity reduced o Blunted - further reduced. o Flat - virtually no sign of affective expression (monotonous voice, immobile face ) Note people with depression have low mood, those with mania have elated or euphoric mood Mental status examination (MSE) Perception: involve the sensory nervous system. Need to look for: 1. Hallucinations - false sensory nervous perception (any of the five) not associated with real external stimuli • • • • • 2. Auditory hallucinations occur commonly in psychosis. Visual hallucinations tend to occur in organic states Bodily sensation (feeling) occur mainly in schizophrenia (& alcohol withdrawal). Olfactory hallucinations found epilepsy, schizophrenia and other organic states; Gustatory hallucinations can occur in schizophrenia (& alcohol withdrawal) Illusions - misinterpretation of a real external sensory stimulus: • e.g. the movement of the curtain as a person and become frightened. • occur in schizophrenia but may also occur in delirium 3. Depersonalisation and derealisation - These are alterations in an individual‘s perception of reality. • depersonalisation feels detached and view’s oneself as strange and unreal • derealisation - Objects in the outside world may seem altered in size and shape, and people may appear dead or mechanical Mental status examination (MSE) Thought Process (form of thinking) - the way in which a person puts together ideas and associations (the flow, logic and associations): • Loose associations - no logical connection – words make sense but sentence does not • Circumstantiality – ‘overinclusion of trivia’ – loses the point • Tangentiality – wanders off the subject with related words • Thought blocking – thinking process stops and mind goes blank • Perseveration – repetition out of context of same words & won’t stop • Echolalia – direct repetition of examiner’s words • Clang associations (punning) – associations by sound (rhyme) or (pun - double) meaning • Neologisms – invention of new words by combining or condensing • Word salad – incoherent connections of thought • Flight of ideas - succession of associations move abruptly from idea to idea Mental status examination (MSE) Thought Content • Delusions - fixed, false beliefs, based on incorrect inference about external reality, not consistent with a patient’s intelligence and cultural background and cannot be corrected by reasoning. Types of delusions include: • persecution, morbid jealousy and infidelity, love, misidentification, grandiose, religious, guilt and unworthiness, poverty, hypochondriacal, infestation and delusions of control leading to passivity • Obsessions - persistent intrusive thoughts, ideas and impulses that occur in anxiety states: • • • • Preoccupations Compulsions Phobias Plans, intentions • Suicidal and homicidal thoughts (may need specific enquiry) Mental status examination (MSE) Alertness and Cognition • Alertness (observed) –alert, in stupor or lethargic. • Orientation - capacity of a person to gauge accurately time, place and person. Severity occurs in increasing order from time, to place, and in person • Attention and concentration - Attention refers to the objective observation of another person, object or event. (use serial 7’s, 3’s, spelling backwards etc. • Memory (immediate, recent, recent past, long term) • Abstract thinking – ability to deal with concepts (comparison of objects, simple proverbs) • Impulsivity – capability of controlling urges (sexual, aggressive, others..) • Judgement - understanding likely outcome of behaviour • Fund of knowledge – intellectual capability based on educational and cultural background • Insight - degree of awareness about their own state • Reliability – how honest, dependable Further mental status physical examination Stigmata that may lead panel physician to suspect use of psychoactive drug by the applicant: • characteristic dental discoloration of the teeth and the flattening of the molars and premolars, that occurs with long-term use of khat, betel nut • blood-shot eyes, alcoholic facies (parotid enlargement/hypertrophy, oedema, flushing). • evidence of intravenous puncture-sites on the arms or legs in IV drug users. If identify or suspect should further investigate…… Mental Health – substance abuse detection Psychiatric referral for further evaluations and/or • Random drug screens (ideally three to four over a 12 month period) – note applicant not aware of planned day. • • On the day of planned drug screen, nurse calls the applicant first thing in the morning and advise to present themselves to the clinic the same day for evaluation. • On arrival at the clinic, applicant asked to provide a urine sample (at least 10mls in a clear container). • Anti-fraud measures should be observed to avoid applicant substitution and the collection of the sample must be supervised. The provided sample – warm, bubbly, condensation on the bottle • For known IV drug users remember to do HIV, Hep B and Hep C tests Mental Health – psychiatric/psychologist referral Refer to a specialist consultant if after assessment unable to: • Arrive at a probable diagnosis for purposes of the determination of a mental disorder with associated harmful behaviour. • Arrive at a probable diagnosis of a substance-related disorder. • Arrive at a probable diagnosis for past episodes of mental disorder or determine that previous difficulties in functioning were a result of a mental disorder. • Rule out the presence of a mental disorder. • Determine if harmful behaviour has been associated with a physical or mental disorder • Determine if any associated harmful behaviour is likely to recur or under control. • Determine the likelihood of maintaining remission or effective control of diagnosed physical or mental disorders that affect behaviour. Important information to clarify: • What are the prospects for better prognosis with adequate treatment and care? • Whether the applicant poses a danger to him/herself or to the public Mental Health – travel concerns Note while not the primary aim – consideration for travel may be required: • fitness to travel – airline rules!! • refugee applicants may need medical or other escort. Consider for following conditions: • Schizophrenia and other Schizophrenia Spectrum Disorders, • Bipolar Mood Disorder, • Major Depressive Disorder, • Moderate to Severe Intellectual Disability Disorder, • Anxiety Disorders, including PTSD, General Anxiety Disorder, Specific Phobias, Panic Attacks. Aim for good stabilisation prior to travel. • Quick Mental Status Examination (behaviour, mood, speech, perception, thoughts, cognition) • Risk Assessment for disruptive behaviour i.e. agitation, violence, suicide, panic • Quickly obtain corroborative/collateral information, if possible, from the family members, or whoever is travelling with the migrant. Questions