* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Parathyroid Glands - bushelman-hap
Survey
Document related concepts
Transcript
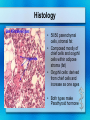
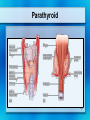
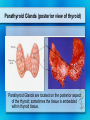
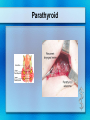
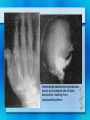
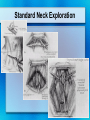
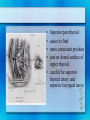
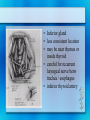
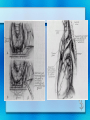
Parathyroid Glands Histology Anatomy & Physiology Diseases Histology • 50/50 parenchymal cells, stromal fat • Composed mostly of chief cells and oxyphil cells within adipose stroma (fat) • Oxyphil cells: derived from chief cells and increase as one ages • Both types make Parathyroid hormone Anatomy • Superior glands usually imbedded in fat on posterior surface of middle or upper portion of thyroid lobe • Inferior glands near the lower part of thyroid gland • Most of blood supply from branches of inferior thyroid artery, although branches from superior thyroid supply at least 20% of upper glands. • Glands drain ipsillaterally by superior, middle, and inferior thyroid veins. Parathyroid Parathyroid Glands (posterior view of thyroid) Parathyroid Glands are located on the posterior aspect of the thyroid; sometimes the tissue is embedded within thyroid tissue. Parathyroid Anatomy & Physiology Usually four – two on each side (2-8 is normal) Parathyroid glands 1. Yellow-brown 2. oval or lentiform structures 3. weigh ~ 50 mg each 4. Measure 3-10 mm x 2-6 mm x 1-4 mm • Lie on the posterior surface of thyroid • May be embedded within thyroid gland • Regulate calcium/phosphate levels • Required for life Parathyroid Hormone • Synthesized in chief cells as large precursor – preproparathyroid hormone • Cleaved intracellularly into proparathyroid hormone then to final 84 AA PTH • PTH then metabolized by liver into hormonally active N-term and inactive C-term Calcium Homeostasis • The parathyroid cells rely on a G-proteincoupled membrane receptor designated the calcium-sensing receptor (CASR), to regulate PTH secretion by sensing extracellular calcium levels • PTH secretion also is stimulated by low levels of 1,25-dihydroxy vitamin D, catecholamines, and hypomagnesemia. Calcium Homeostasis • PTH is synthesized in the parathyroid gland as a precursor hormone,preproparathyroid hormone, which is cleaved first to proparathyroid hormone and then to the final 84-amino-acid PTH. • Secreted PTH has a half-life of 2 to 4 minutes. In the liver, PTH is metabolized into the active N-terminal component and the relatively inactive C-terminal fraction Calcium homeostasis • The calcium-sensing receptor (CASR) senses fluctuations in the concentration of extracellular calcium. • Increased PTH secretion leads to an increase in serum calcium levels by increasing bone resorption and enhancing renal calcium reabsorption. • PTH also stimulates renal 1- Hydroxylase activity, leading to an increase in 1,25dihydroxy vitamin D, which also exerts a negative feedback on PTH secretion Calcium homeostasis • PTH functions to regulate calcium levels via its actions on three target organs, the bone, kidney, and gut. • PTH increases the resorption of bone by stimulating osteoclasts and promotes the release of calcium and phosphate into the circulation. Calcium homeostasis • At the kidney, PTH acts to limit calcium excretion at the distal convoluted tubule via an active transport mechanism. • PTH also inhibits phosphate reabsorption (at the Proximal convoluted tubule) and bicarbonate reabsorption. • PTH and hypophosphatemia also enhance 1hydroxylation of 25-Hydroxyvitamin D, which is responsible for its indirect effect of increasing intestinal calcium absorption. Parathyroid Diseases • Benign adenoma a. Relatively common b. Usually results in hyperparathyroidism • Cancers are rare a. Surgical removal gives > 90% cure rate Parathyroid Diseases • Hyperparathyroidism a. Affects about 100,000 patients per year • Primary Hyperparathyroidism: – occurs in 0.1 to 0.3% of the general population and is more common in women (1:500) than in men (1:2000). – Normal feedback of Ca is disturbed, causing increased production of PTH (does not depend on calcium concentration) – Acts on bone, kidneys, small intestines Primary Hyperparathyroidism Epidemiology – – – – – 25/100,000 50,000 new cases yearly F>M Incidence increases w/ age Most in > 50 years old Etiology – Unknown cause – Ionizing radiation exposure? Hyperparathyroidism Symptoms • Kidney stones, painful bones, abdominal groans, psychic moans, and fatigue overtones • Kidney stones calcium phosphate and oxalate • Osteopenia, osteoporosis, and osteitis fibrosa cystica, is found in approximately 15% of patients with PHPT. Increased bone turnover can usually be determined by documenting an elevated blood alkaline phosphatase level. • Peptic ulcer disease, pancreatitis • Psychiatric manifestations such as florid psychosis, obtubdation, coma, depression, anxiety, fatigue Hyperparathyroidism (cont.) • Secondary Hyperparathyroidism – Defect in mineral homeostasis leading to a compensatory increase in parathyroid gland function • Tertiary Hyperparathyroidism – After prolonged over-compensatory stimulation, hyperplastic gland develops autonomous function Hyperparathyroidism • Hypercalcemia can be from other sources. Intact PTH measurement and elevated PTH level very sensitive for hyperparathyroidism Hypercalcemia – Etimology • Hyperparathyroidism (most common) • Malignancy (most common in hospitalized) – Lytic metastases to bone – PTHrP producer • Sarcoidosis / granulomatous disease • Hyperthyroidism • Familial hypocalciuric hypercalcemia Renal Complications • Generally the most severe clinical manifestations • Calcium phosphate or Calcium oxalate • Severe renal damage • Hypertension secondary to renal impairment Bone Disease • Osteitis fibrosa cystica – Generalized skeletal demineralization due to an increased rate of bone destruction resulting from hyperparathyroidism – In early descriptions of disease, many had severe bone disease (50-90%), but now 515% – Subperiosteal resorption – pathognomonic of hyperparathyroidism Generalized skeletal demineralization due to an increased rate of bone destruction resulting from hyperparathyroidism Gastrointestinal Manifestations • Peptic Ulcer disease • Pancreatitis • Cholelithiasis – 25-35% Emotional Disturbances • Hypercalcemia of any cause – assoc w/ neurologic or psychiatric disturbances – Depression, anxiety, psychosis, coma • Severe disturbances not usually correctable by parathyroidectomy Articular and Soft Tissue • Chondrocalcinosis and Pseudogout 37% • Deposits of Calcium pyrophosphate in articular cartilages and menisci • Vascular and Cardiac calcifications Neuromuscular complications • Muscular weakness, fatigue • More commonly in proximal muscles • Sensory abnormalities also possible Hyperparathyroid Crisis • Most patents w/ hyperparathyroidism chronically ill w/ renal and skeletal abnormalities • Rarely can become acutely ill • Rapidly developing weakness, N/V, weight loss, fatigue, drowsiness, confusion, Azotemia • Uncontrolled PTH production, hyperCa, polyuria, dehydration, reduced renal function, worsening hyperCa Hyperparathyroid Crisis • Definitive therapy - resection • Must reverse hyperCa first – Diuresis - Saline hydration then Lasix to excrete Ca – Calcitonin - rapid affect, inhibits bone resorption – Steroids - take up to a week – Mithramycin - rapidly inhibiting bone resorption Treatment • Only Curative treatment Parathyroidectomy • Who should have surgery? – Many found incidentally, during routine physicals Who should have surgery? • NIH Consensus statement 1991 • All symptomatic • If Assymptomatic – – – – – – Markedly elevated serum Ca H/o episode life-threatening hypercalcemia Reduce renal function Kidney stone on Radiograph Markedly elevated urinary Ca excretion Substantially reduce bone mass Standard Neck Exploration Parathyroidectomy • Must find all four glands • Intraoperative frozen section, PTH measurement useful • If single gland enlarged, removal usually curative • If multiple glands enlarged, removed. Normal just biopsied • If all 4 enlarged (generalized parathyroid hyperplasia) - subtotal (3 1/2 removed) – Can reimplant into forearm muscle • • • • Superior parathyroid easier to find more consistent position just on dorsal surface of upper thyroid • careful for superior thyroid artery and superior laryngeal nerve • Inferior gland • less consistent location • may be near thymus or inside thyroid • careful for recurrent laryngeal nerve betw trachea / esophagus • inferior thyroid artery Success of Surgery • 95% of cases cured at initial neck exploration • If failed intial procedure, can try to localize w/ Radionuclide, detect w/ gamma probe – Sestamibi concentrates in parathyroid tissue – Increasingly used in initial operation – limits dissection – Limits operative time • May need mediastinoscopy