* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
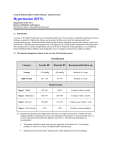
Download 1 Hypertension Shirley Paski Classifications Category Systolic
Survey
Document related concepts
Transcript
Hypertension Shirley Paski Classifications Category Normal Prehypertension Hypertension Stage 1 Stage 2 Isolated systolic Systolic mmHg <120 120-139 Diastolic mmHg <80 80-89 140-159 ≥160 ≥140 90-99 ≥100 <90 History Signs and Symptoms o Usually asymptomatic o Headache, dizziness, palpitations, easy fatigue, impotence o Epistaxis, hematuria, blurred vision, focal neurologic symptoms, angina, SOB o Polyuria, polydipsia, muscle weakness (1° aldo) o o Diagnosis Recommendation: check blood pressure at each office visit for patients over age 21 End-organ damage: only one measurement required 1. Neuro: ischemic stroke, ICH, TIA, aneurysmal SAH 2. Retinopathy 3. Cardiac: LVH, LVdysFx, MI, angina, CHF, PAD 4. Nephropathy: GFR<60, proteinuria >150mg/24h No end-organ damage, mild hypertension: persistently elevated blood pressure on 3-6 visits over weeks to months Weight gain, emotional lability (Cushings) Episodic headaches, palpitations, diaphoresis, postural dizziness (pheo) Past Medical History o Family history of HTN including age of onset o Smoking, alcohol, other drugs o Medications: OCP, cold meds, sympathomimetics, steroids o Diabetes o Dyslipidemia o Diet, exercise Physical Examination Goals: 1. Measure and stage the blood pressure 2. assess overall CV risk (comorbidities – central obsesity, DM, CHOL, smoking; target EOD) 3. identify secondary causes (<5%) – not cost-effective in most pts General H&N o Obvious neurological signs of o Thyroid CVA/bleed/encephalopathy. Cardiovascular exam (signs of EOD) o Signs of systemic associated diseases like o JVP Cushing’s syndrome, acromegaly, polycythemia, o Carotid upstroke and bruits chronic renal insufficiency, thyroid dz, OSA o Precordial exam: rythym, LVH, S3, S4, acute Vitals/Blood Pressure MR or AR o Sitting in both arms (R/O dissection), average of o Chest 3 measurements, standing @ 2mins. N: DBP o Peripheral pulses (absent, diminished) will on standing in essential hypertension Abdomen o If coarctation suspected, palpate radiofemoral o Waist circumference delay and measure BP in legs. N: BP legs>arm o Striae, central obesity Fundi o Renal or adrenal masses (ex. Polycystic KD) o Grade 1: silver wiring of arteries (“sclerosis of o Renal or abdominal bruits *RCExam vessel wall reduces transparency so central light Loud, systolic-diastolic, epigastrum streak becomes broader and shinier”) Normal in 6-31%, less in older o Grade 2: grade 1 + AV nicking o Uterine fundus for pregnancy o Grade 3: grade 2 + flame hemorrhages + cottonwool spots + hard exudates o Grade 4: grade 3 + papilledema Basic Investigations Always included: o Urine for protein, blood, glucose, UA o Hb o K o BUN, Creatinine o Fasting glucose o Total cholesterol o EKG (LVH, old MI) Usually included: o TSH o WBC o HDL, LDL, trigs o Ca, PO4 o CXR o Limited echocardiogram (LVH) 1 Special Studies to Screen for Secondary Causes Renovascular disease: captopril renal scan, renal Doppler flows, MRI angiography Pheochromocytoma: 24h urine creatinine, metanephrines, catecholamines Cushing’s syndrome: overnight dexamethasone suppression test or 24h urine cortisol and creatinine Primary aldosteronism: plasma aldosterone:renin activity ratio Suspect secondary causes if: ? 1. onset < 30y or >55 2. htn refractory to >/= 3 drugs 3. suspicious clinical situation (sx suggestive of secondary cause) Treatment When to start: o SBP ≥ 180 or DBP ≥ 110 Start drug treatment and lifestyle modification o SBP < 180 and DBP <110 Start lifestyle modification, stratify absolute risk o High risk (3+ CV risk factors, diabetes) Start drug treatment, stongly consider combination therapy as initial treatment o Moderate risk (1-2 CV risk factors) or low risk (0 CV risk factors) SBP 130-139 or DBP 85-89 on several occasions No treatment, monitor BP and other RF’s SBP 140-179 or DBP 90-109 on several occasions Start drug treatment Lifestyle modification: o Diet (DASH), regular exercise, weight reduction, smoking cessation, stress management, control of other risk factors contributing to the development of arteriosclerosis Drug management: o Caveats Start with an agent that may also treat / not harm coexisting conditions Start with an agent that the patient is likely to tolerate best to optimize adherence For low or moderate risk pts, start with a low dose and increase gradually to achieve control Add an additional agent from a different, complementary class if bp not controlled on a moderate dose of the first agent Use a diuretic when 2 agents are used, in nearly all cases Use thiazide diuretics only at low doses unless some pressing reason exists For medium to high risk patients, strongly consider low dose combination therapy as initial therapy: Diuretic + betablocker, ACEi, ARB CCB + ACEi, betablocker o Guidelines for selecting initial drug therapy for hypertension: Drug Class Compelling indications Possible Compelling Possible indications contraindications contraindications Diuretics Heart failure DM Gout Dyslipidemia Elderly Sexually active male Systolic HTN Beta blockers Angina Heart failure Asthma Dyslipidemia Post-MI Pregnancy COPD Athletes Tachyarrhythmia DM Grade 2-3 AVB PVD ACE inhib Heart failure Pregnancy LV dysfunction Hyperkalemia Post-MI Bilat RAS Diabetic nephropathy CCB Angina PVD Grade 2-3 AVB CHF (verapamil or Elderly diltiazem) Systolic HTN ARB ACE inhib cough Heart failure Pregnancy Bilat RAS Hyperkalemia Goals: <140/90 generally speaking; <130/80 for those with DM, CRI, CV disease. Careful not to drop DBP < 65 in those with isolated systolic hypertension since this actually increases the risk of stroke. References Canadian Hypertension Guidelines, Harrison’s, UpToDate 2