* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Ocular Instrumentation - Heart of America Contact Lens Society
Survey
Document related concepts
Transcript
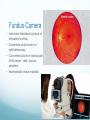
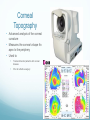
Ocular Instrumentation Lynn E. Konkel, M.S., CPOT Heart of America – February 2013 Overview Identify most commonly used equipment Identify the reason for use Note: there are many different brands of the same type of equipment, all the brands are not depicted in this presentation Recommend maintaining the manuals for all equipment in a central location. The manuals are very helpful for use, calibration, care and servicing of equipment Pretesting Equipment Transilluminator • Handle that contains a rechargeable battery • Preferred over a penlight • Dial control for the brightness of the light • Recommended for assessing pupil reflexes • Also may be used to provide additional light source when needed • Maintain back up light bulb Pinhole Disk • Instrument that looks like an occluder but has multiple holes 0.5 to 2mm in diameter. • Used to assess whether the reduced visual acuity is due to refractive error or some other condition. • If the visual acuity improves with the pinhole then usually expect a refractive error. Maddox Rod • A group of either red or colorless parallel glass rods • Used to dissociate the eyes, prevent fusion • Used to detect or measure amount of heterotropia or heterophoria. • Rods held vertically • Rods held horizontally • Stereopsis plates • Color vision plates • Ishihara • Pseudoisochromatic Keratometer • Kera is the root word for cornea; meter is the suffix for measure therefore this is a instrument that measure the corneal curvature. • Obtains the curvature in diopters along the area of least and most curvature. • Ex: 44.50@175; 45.25@ 85 • Available in manual or automated versions • Maintain a stock of replacement bulbs Tonometer • Tono = pressure, meter again is to measure. This instrument measures the intraocular pressure. • Many styles of tonometers, manual and automated versions. • Pictured here is the noncontact tonometer = automated, “air puff”. • Readings are stated in millimeters of mercury (mmHg) • Record time of day • Diurnal variation Tonometer cont. • Tonopen • Maintain supply of tip covers and batteries • Use with corneal anesthetic • Goldmann • Needs no electricity or special supplies to maintain however, needs an operating slit lamp unless using the hand-held model • Use with combo drug of corneal anesthetic and fluorescein, brand name = Fluress Visual Field Testing • Eye maintains steady fixation and • • • • tests the retina for areas of decreased (or absent) vision. Typically used to test area outside the macula (central vision) Compare/contrast visual field testing to visual acuity testing Typically need to use trial lenses when testing the central visual field (lenses removed for area outside the central 30°) Equipment is complicated, keep manual handy. Visual Field Testing - cont. • Amsler grid • Used when you want to assess the macular area of the retina. • Can detect • Central scotomas • Paracentral scotomas • Distortion = metamorphopsia Auto-refractor • Instrument used to estimate a refractive error. Automated version of a retinoscope • Can be in combination with an auto-keratometer. Examination Room Projector & Slides • Projector – used to project letters, characters, shapes on a silver screen • Slides • Snellen letters • Landoldt rings • Numbers • Tumbling E’s • Worth 4-dot • Means to isolate lines/letters • Filters – red/green Retinoscope • Obtains an estimate of the patient’s refractive error without any input needed from the patient (objective measurement) • Projects light onto the retina, moving the light back and forth gives the doctor input as to whether the patient has myopia/hyperopia/astigmatism. • Use lenses in the phoropter to neutralize the movement of the light. Ophthalmoscope • Instrument used to exam the retina. • Eyes are typically dilated for wider view. • Direct (pictured on left) • Uses internal lenses to assist in focus • Can magnify 15x • Indirect • Monocular – greater magnification then direct, not used much today. • Binocular – allows for stereoscopic and wider view of the retina, worn on head and used with handheld condensing lens. Image is inverted (upside down and reversed left/right). Very commonly used today especially for patient’s with disease. Ophthalmoscope • Binocular indirect Phoropter • Used to obtain patient’s correction for refractive error • Distant Rx • Near Rx • Used to measure phoria’s, accommodation, etc. • Contains concave, convex, cylindrical lenses along with prisms and various other lenses (Maddox rod for example) Trial Lenses • Tray of lenses and accessories • Lenses – sphere & cylinder • Prisms • Occluders • Pinhole disk • Maddox Rod/red lens • Frame • Uses: • Test refractive error of an eye • Let the patient test how a potential Rx will be • Used with other instruments such as visual field bowl analyzers Slit Lamp – Biomicroscope • Instrument used to examine the external and anterior structures of the eye under magnification. • Can have attachments such as: • Goldmann tonometer • Camera • Observation tube • Handheld lenses used in conjunction with slit lamp can be used to examine the retina. Slit Lamp “Accessories” • Hruby lens – 55 D lens • Goniolens – consists of a contact lens and a mirror. Use a corneal anesthetic and a gel (goniogel). • Goldmann tonometer Ancillary Testing Instruments Pachymeter • Measures the corneal thickness • Used to assist in the diagnosis of glaucoma • Do thinner corneas mean increase risk of developing glaucoma? • Do thinner corneas mean we are underestimating the IOP? • Do thicker corneas mean we are overestimating the IOP? • Evaluated prior to refractive surgery • Need a corneal anesthetic A-scan Ultrasound Biometry • Measure the length of the eyeball • Used to calculate the power of the lens implant needed for cataract surgery • Requires corneal anesthetic • Test being replaced by automated instruments such as the IOL Master • Noncontact = no anesthetic Fundus Camera • Instrument that takes a picture of the patient’s retina. • Documents what is seen on ophthalmoscopy. • Can center picture on various parts of the retina – disk, macula, periphery • Nonmydriatic versus mydriatic Automated optic nerve/retina instruments • Heidelberg Retina Tomograph (HRT). • Used to assist in the diagnosis and management of glaucoma • GDx Nerve Fiber Analyzer • Used to assist in diagnosis and management of glaucoma. • Ocular Coherence Tomography (OCT). • Used to assist in diagnosis of retinal pathology Corneal Topography • Advanced analysis of the corneal curvature • Measures the cornea’s shape fro apex to the periphery • Used to: • Treat and monitor patient’s with corneal disease • Prior to refractive surgery Lasers • Tunable dye lasers • Used in the anterior segment • Trabeculoplasty • Iridoplasty • Photodisruptive lasers • YAG laser (pictured), used for secondary cataract, iridotomy. • Thermal photocoagulation • Argon blue-green/argon monochromatic green/krypton red • Extensively used to treat diabetic retinopathy, CRVO, retinal holes, retinal detachments • Excimer laser • Used in phtorefractive keratotomy • Ablates a small amount of the corneal stroma to flatten the corneal Optical Dispensary Lensometer • Lens gauge/clock • Lens thickness gauge • Corneal reflex pupilometer • PD stick Where to obtain more information on this subject: AOA Paraoptometric Section, Self-Study Course for Paraoptometric Assistants and Technicians, Revised 3rd Edition Butterworth-Heinemann 1997 Stein, Stein, Freeman, The ophthalmic assistant (8th edition) Mosby 2006 Cassin, Rubin, Dictionary of eye terminology (6th edition) Traid 2011 Questions?