* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Changes in the internal structure of the human crystalline lens with
Survey
Document related concepts
Transcript
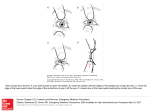
Vision Research 43 (2003) 2363–2375 www.elsevier.com/locate/visres Changes in the internal structure of the human crystalline lens with age and accommodation M. Dubbelman a, G.L. Van der Heijde a a,* , H.A. Weeber b, G.F.J.M. Vrensen c Department of Physics and Medical Technology, VU Medical Centre, P.O. Box 7057, 1007 MB, Amsterdam, The Netherlands b Applied Research, Pharmacia, P.O. Box 901, 9700 AX Groningen, The Netherlands c Department of Ophthalmology, Leiden University Medical Centre, P.O. Box 9600, 2300 RC Leiden, The Netherlands Received 29 August 2002; received in revised form 29 January 2003 Abstract Scheimpflug images were made of the unaccommodated and accommodated right eye of 102 subjects ranging in age between 16 and 65 years. In contrast with earlier Scheimpflug studies, the images were corrected for distortion due to the geometry of the Scheimpflug camera and the refraction of the cornea and the lens itself. The different nuclear and cortical layers of the human crystalline lens were determined using densitometry and it was investigated how the thickness of these layers change with age and accommodation. The results show that, with age, the increase in thickness of the cortex is approximately 7 times greater than that of the nucleus. The increase in thickness of the anterior cortex was found to be 1.5 times greater than that of the posterior cortex. It was also found that specific parts of the cortex, known as C1 and C3, showed no significant change in thickness with age, and that the thickening of the cortex is entirely due to the increase in thickness of the C2 zone. With age, the distance between the sulcus (centre of the nucleus) and the cornea does not change. With accommodation, the nucleus becomes thicker, but the thickness of the cortex remains constant. Ó 2003 Elsevier Ltd. All rights reserved. Keywords: Aging; Accommodation; Crystalline lens; Scheimpflug photography; Cortex; Nucleus 1. Introduction The Scheimpflug camera provides high-contrast images that contain detailed information about the internal structure of the human crystalline lens, which makes it possible to determine changes within the lens with age and accommodation. Knowledge about these changes is of importance in understanding how the human eye is able to focus on near or far objects (the mechanism of accommodation) and why this ability deteriorates with age (presbyopia). Furthermore, knowledge about the change in the internal structure of the lens is necessary for optical modelling of the human eye and mechanical modelling of the accommodation system. The human lens continues to grow throughout life, due to the addition of new lens fibres. With age, the lens becomes more convex (Dubbelman & Van der Heijde, * Corresponding author. Fax: +31-20-4444147. E-mail address: [email protected] (G.L. Van der Heijde). 0042-6989/$ - see front matter Ó 2003 Elsevier Ltd. All rights reserved. doi:10.1016/S0042-6989(03)00428-0 2001) and thicker in the sagittal direction at a rate of approximately 0.024 mm/years (Dubbelman, Van der Heijde, & Weeber, 2001). The various anatomic regions within the human lens are generally divided into two main regions: the nucleus and the cortex. It is convenient to take the dividing line between cortex and nucleus as the point of sudden reduction in brightness on the Scheimpflug image (Fig. 1). Several authors have used Scheimpflug photography to measure the increase in thickness of the cortex and nucleus of the normal human lens. Brown (1976) found that the growth of the cortex was three times the growth of the nucleus. According to Shibata, Hockwin, Weigelin, Kleifeld, and Dragomirescu (1984) and Kashima, Trus, Unser, Edwards, and Datiles (1993), this growth of the cortex would be 1.5 and 1.75 times the growth of the nucleus. Cook, Koretz, Pfahnl, Hyun, and Kaufman (1994) even measured a decrease of 3 lm/years in the thickness of the nucleus with age. Studies that are more detailed showed that alternating light and dark zones could be distinguished within 2364 M. Dubbelman et al. / Vision Research 43 (2003) 2363–2375 Fig. 1. Scheimpflug image of the eye of a 51 year-old female. Using the densitogram above the image, 8 different zones can be distinguished. Using the local maximums of the gradient of the densitogram under the picture, three different cortical zones (C1–C3) can be defined according to the Oxford system. the anterior and posterior cortex (Goldmann, 1964). According to the zone system developed by Sparrow, Bron, Brown, Ayliffe, and Hill (1986), these cortical zones could be sub-divided into four zones: C1–C4. Zone C1, which is located behind the anterior and just in front of the posterior capsule, and C3 are zones of high light scatter, whereas C2 and C4 are dark zones of low light scatter (Fig. 1). The thickness of zone C4 can usually not be determined accurately. The changes with age in the thickness of zones C1–C3 of the anterior cortex have been measured by Smith, Smith, Brown, Bron, and Harris (1992). It appeared that most of the growth of the lens occurred in zone C2, while C3 showed little increase in thickness after it had been established during the second decade of life. The thickness of zone C1 showed a tendency to decrease with age. It is suggested that the growth of the lens is slowed down by the process of compaction (the compression of existing fibres) (Bron, Vrensen, Koretz, Maraini, & Harding, 2000). This term was used by Brown (1976) to explain why glaucoma flecks and traumatic cataracts sank into the cortex of the lens at a faster rate than could be expected on account of the average growth of the lens due the addition of new lens fibres. Support for nuclear compaction has also come from the earlier mentioned study carried out by Cook et al. (1994), in which a decrease in nuclear thickness with age was found. Further support came from the measurement of a small group of patients with lamellar cataract, in whom shrinkage of the lamellar shell of opacity could be determined, particularly in the sagittal plane (Brown, Sparrow, & Bron, 1988). In vitro, compaction in the embryonic nucleus with age has been demonstrated (AlGhoul et al., 2001). The process of compaction has, however, been questioned by Pierscionek and Weale (1995). The change in the internal structure of the lens during accommodation has been measured in three studies (Brown, 1973; Koretz, Cook, & Kaufman, 1997; Patnaik, 1967), from which it appeared that the accommodative increase in the sagittal lens thickness could be attributed to an increase in the thickness of the lens nucleus, while the thickness of the cortex remained almost unchanged. Using optical techniques, such as Scheimpflug imaging, the internal structure of the lens is observed through the preceding refractive surfaces, i.e. the cornea and the anterior lens surface. The refraction at these surfaces will distort the shape of the internal structure of the lens (Richards, Russell, & Andersson, 1988; Dubbelman & Van der Heijde, 2001). Up till now, in all studies measuring the internal structure of the lens with age or accommodation no attempt has been made to correct the Scheimpflug images for this type of distortion. In most studies, a correction was made for the distortion due to the geometry of the Scheimpflug imaging system, in which the object and/or image plane is tilted (Ray, 1995). However, correction for the refraction of cornea and lens is also necessary to obtain accurate measurements of the internal structure of the lens and to determine age-related trends. The purpose of the present investigation was therefore to correct for both types of distortion and to measure the change in the internal structure of the crystalline eye lens with age and accommodation. Scheimpflug images were made of the eyes of subjects of various ages at different accommodation levels. Individual ray tracing was applied to correct for the refraction of the front and back surface of the cornea and the front surface of the lens. However, to make it possible to correct for the latter, the refractive index of the lens is needed. Therefore, axial length was measured to calculate the equivalent refractive index of the crystalline lens. Using this method to correct the Scheimpflug M. Dubbelman et al. / Vision Research 43 (2003) 2363–2375 images, it is possible to exclude artefacts that are due to optical distortions and to provide an accurate measurement of the changes that take place in the internal structure of the aging and accommodating lens. 2. Methods 2.1. Measurements The sample population and the experimental design have been described elsewhere in detail (Dubbelman & Van der Heijde, 2001; Dubbelman et al., 2001). Briefly, Scheimpflug images were made of the right eye of 102 healthy subjects aged between 16 and 65 years, who had no history of eye injury or systemic disorders. Experiments were performed with the understanding and written consent of each subject. After full pupil dilation of the right eye (phenylephrine HCl 5%), refractive error and astigmatism of both eyes was measured with a Topcon KR-3500 autokerato-refractometer and subjects with astigmatism larger than 1.5 D were excluded. A topogram of the cornea of the right eye was made with the Keratron corneal analyser (Optikon, 2000). Images of the anterior segment of the right eye were made with the Nidek Eas-1000 Scheimpflug camera (Nidek Co. Ltd., Japan) (Sakamoto & Sasaki, 1994; Sasaki, Sakamoto, Shibata, & Emori, 1990), which was equipped with a black and white CCD camera. The subject was seated with the head in an upright position, and the slit beam of the Scheimpflug was vertically oriented. The left eye was used to focus on an accommodation stimulus, while the right eye was photographed. The accommodation stimulus was an illuminated black Maltese star, which was located 1m from the left eye. To obtain the unaccommodated state of the eye, a +1 D lens and the refractive correction were placed in a lensholder directly in front of the left eye. The subject concentrated first with the right eye on the fixation light in the Scheimpflug camera and the camera was adjusted along the optical axis of the eye by positioning the corneal reflex in the centre of the pupil. Subsequently, the subject fixated with the left eye on the accommodation stimulus, of which the position could be varied by remote control until the subject confirmed that the fixation light was superimposed on the centre of the Maltese star. When the subject indicated that the Maltese star was clearly in focus, a Scheimpflug image was made of the right eye. The subject was then asked to try to maintain focus on the Maltese star, while negative lenses in steps of )1 D were placed in front of the left eye until the subject indicated that it was no longer possible to focus sharply on the star. Each time, the front surface of the cornea was imaged real time on the monitor screen, and convergence was corrected by changing the position of the Maltese star until the corneal reflex re- 2365 turned to the centre of the pupil. Because of limited range of movement of the Maltese star, it was not possible to correct for convergence when accommodation levels were higher than 8 D, and consequently, those levels were not measured. Using the position and power of the different lenses placed in front of the eye, the accommodation stimulus was converted to the accommodation at the corneal plane (Rabie, Steele, & Davies, 1986). For this moment, we will not distinguish between the real accommodative response of the eye and the accommodative stimulus presented, but we will come back to this at the end of paragraph 4.1. Finally, in subjects whose posterior lens surface was clearly visible on the Scheimpflug images, axial length was measured with the IOL Master â Zeiss. This made it possible to calculate the equivalent refractive index of the lens, which was needed to correct for the refraction of the lens itself. If this was not possible, correction was made with the age-dependent equivalent refractive index (Dubbelman & Van der Heijde, 2001; Dubbelman et al., 2001). 2.2. Analysis of measurements The initial stage of the analysis was to identify the different zones within the lens. Fig. 1 shows a Scheimpflug image of an unaccommodated eye of a 51 yearold female. Two different classifications systems were used, to distinguish the different zones on the Scheimpflug image. Firstly, a system often used in cataract research (Hockwin, Dragomirescu, & Laser, 1982; Shibata et al., 1984; Wegener & Laser, 1996), which specifically distinguishes between the nuclear and the cortical zones. This system makes use of the densitogram of the lens indicated in the upper part of Fig. 1, which consists of the grey values along a sagittal strip measuring 8 pixels (1 pixel ¼ ±0.025 mm) on either side of the line through the vertex of the anterior lens surface. The densitograms were sub-divided into eight zones, according to the course of the curve (local minima) representing: (1) anterior capsule and superficial anterior cortex, (2) anterior cortex, (3) anterior supranuclear region, (4) anterior nucleus, (5) posterior nucleus, (6) posterior supranuclear region, (7) posterior cortex, (8) posterior capsule and superficial posterior cortex. The second system distinguishes different layers in the anterior and posterior cortex, and is part of the ÔOxford clinical cataract classification and grading systemÕ (Brown & Bron, 1996; Sparrow et al., 1986). Strictly speaking, zone C1 consists of two narrow zones behind the capsule: the low scatter zone behind the narrow high scatter peak of the capsule (C1 a) and of the subsequent high scatter zone (C1 b), which has also been called the line of disjunction (Niesel, Krauchi, & Bachmann, 1976). Because C1 a and C1 b could often not be resolved accurately in this study, no distinction was made between these two zones, and the C1 width M. Dubbelman et al. / Vision Research 43 (2003) 2363–2375 measurement therefore represented the sum of the capsule and C1. C2 is a zone of low light scatter, and its width is determined by the maxima in the gradient of a densitogram, the latter being a curve representing the rate of change of the densitogram. The same applies to the subsequent high scatter zone C3. Because zone C4 was difficult to distinguish from the anterior and posterior nuclear layers, this layer was not further analysed. In the Scheimpflug image, the cursor of the mouse was used to indicate the various zones depicted in Fig. 1. When the cursor was moved across the Scheimpflug image, its position in the densitogram and in the gradient of the densitogram could be observed on the computer screen allowing determination of the various zones with an error of maximal one pixel. Only those zones which could be distinguished clearly were indicated. After determination of the various zones, the Scheimpflug image was corrected for distortion. It was assumed that each intraocular surface is rotationally symmetric and could be described by a conic of revolution. Using ray tracing through aspherical surfaces, each Scheimpflug image was corrected for the two types of distortion. This method has been validated by measuring an artificial eye and pseudophakic patients with intraocular lenses of known dimensions (Dubbelman & Van der Heijde, 2001; Dubbelman et al., 2001). After correction of the Scheimpflug images, the thickness of the various zones that were manually marked was measured. For the total group of 102 subjects, the changes in the width of the different zones with age were measured. To investigate the changes with accommodation, measurements were made of a group of 65 subjects, who had an accommodation range of at least 1 D. These subjects were selected because analysis of their Scheimpflug images showed significant changes in the anterior chamber depth, the lens thickness and the radius of the anterior lens surface with accommodation (results will be reported elsewhere). Subjects in this group were between 16 and 51 years of age (mean ± s.d.: 32 ± 9) and had a mean equivalent refractive error of )1.4 D. The group consisted of 31 myopes, 30 emmetropes and 4 hypermetropes. Two different methods were used to analyse the different zones with accommodation. The first method is straightforward, and measures the thickness of the different zones in the lens at different accommodation levels. To calculate the change per diopter in each zone, regression analysis was performed for each subject. Because there is uncertainty in the data in both parameters, orthogonal regression was applied (Press, Flannery, Teukolski, & Vetterling, 1994). On the x-axis, the accommodation level of the unaccommodated state (0 D) was given an error of ±0.5 D, because of the uncertainty in the determination of the refractive error (±0.5 D), which might create an offset of the zero accommodation level. As this offset does not produce any error in the relative difference between the higher accommodation levels, these levels were given an error of ±0.25 D to account for possible focusing errors. The borders of the different zones could be determined with an accuracy of approximately 1 pixel (25 lm). Therefore, an error of 40 lm in the determination of the different zones was assumed, and further analysis confirmed that this value seemed to be realistic. The change in thickness of the zones per diopter was determined by means of orthogonal regression, but because the accommodation range is not the same for all 65 subjects, each measurement is subject to a different error. Therefore, the weighted mean, the weighted standard deviation (s.d.) and the weighted standard errors (S.E.M.) will be presented (Bevington, 1969). A second method was used to investigate the changes with accommodation. This method, compared the difference in the densitogram of the unaccommodated and the accommodated lens, both shown in Fig. 2. The figure shows that the profiles of these two densitograms are very similar, except for the fact that the densitogram of the accommodated lens is more stretched, due to thickening of the lens with accommodation. To determine which parts of the lens account for this accommodative increase in lens thickness, the profile of the densitogram of the unaccommodated lens was stretched, using a non-linear function in the horizontal direction, to match the profile of the accommodated lens in a least square sense (Fig. 3). The horizontal dashed line represents zero stretch, while the line indicated by the arrow represents the parts of the unaccommodated lens that have been stretched (or contracted). The amount of stretch is indicated on the right y-axis. Positive values indicate stretch, while negative values indicate shrink, i.e. contraction. Thus, for this subject the most stretch is found in the nucleus. The method was applied to all 110 100 Grey value (au) 2366 90 80 70 60 50 0D 40 4.6D 30 3.2 4.2 5.2 6.2 7.2 Distance from cornea (mm) Fig. 2. The thick line represents the densitogram of the unaccommodated lens (0 D) of a 34 year-old male. The densitogram at 4.6 D accommodation is indicated by the thinner line. It can be seen that except for the 0.21 mm longer densitogram of the accommodated lens, the shape of the two densitograms is quite similar. M. Dubbelman et al. / Vision Research 43 (2003) 2363–2375 2367 1 110 100 0.8 Nucleus 0.6 80 0.4 70 60 0.2 post. cortex ant. cortex 50 Stretch Grey values 90 0 40 stretch 30 -0.2 0 0.5 1 1.5 2 2.5 3 3.5 4 Distance from anterior lens vertex (mm) Fig. 3. The two densitograms of Fig. 2 after non-uniform stretching of the densitogram of the unaccommodated lens. The horizontal dashed line represents zero stretch. The solid line indicated by the arrow represents the parts of the unaccommodated lens which had to be stretched to match the densitogram of the accommodated lens as accurately as possible. The higher this line is above the line of the zero stretch, the more the densitogram of the unaccommodated lens has been stretched. It can be seen that it is mainly the nucleus which is stretched. densitograms representing the different accommodative states of the lens of each subject. Thus if a subject was able to accommodate 3 diopters, 6 stretch-functions could be obtained. The stretching was performed with the Mathematica Package Software (Version 4.0, Wolfram Research, Inc.), including the Digital Image Processing toolbox as an add-on. For optimisation, part of the programme was written in C++. Before stretching, both densitograms were smoothed using a Block Lee filter (a nonlinear noise reducing operator), after which a set of 12 equidistant points was chosen in each densitogram. The points of both sets had a one-to-one correspondence with each other and the pairs of points define a smooth stretch function, which maps points from one densitogram to the other. The first and the last point of the stretch function are fixed, because after stretching these points should match in both densitograms. In between those points, the stretch function is represented by a spline function, which connects all 12 points together. Using the Powell minimisation method, the distance between the points of the densitogram of the unaccommodated lens was varied to find the optimal stretch function, with which it should be modified to match the densitogram of the accommodated lens in a least square sense. With a uniform stretch, the 12 points of the densitogram of the unaccommodated lens remain equidistant. Because the pupil constricts during accommodation, the intensity of the scattered light of the lens reduces in particular the posterior part of the lens. As a result, the amplitude, but usually not the shape, of the accommodated densitogram becomes smaller in comparison with the unaccommodated densitogram. To compensate for this difference in density, another func- tion was introduced with which the accommodated densitogram should be multiplied. To avoid large changes in the separate peaks of the accommodated densitogram, this function is chosen to be more smooth (less detailed) and is defined as a spline fitted to 4 equidistant points in the densitogram of the accommodated lens. As a result, the amplitude of the peaks of the two densitograms will often not be identical, because of the smoothness of this function. This function and the stretch function were simultaneously included in the minimisation procedure. To avoid confusion, this function is not shown in Fig. 3. 3. Results 3.1. Optical correction of the Scheimpflug images Fig. 4 shows the influence of the correction on the densitogram of a 35 year-old male (upper part) and a 64 year-old male (lower part). The thick lines represent the uncorrected densitograms, and the thin lines represent the densitograms after correction for the geometry of the Scheimpflug imaging system and the refraction of the cornea and anterior lens surface. The correction influences the dimensions of the different zones in the lens, and this influence is particularly dependent on the agedependent anterior chamber depth. 3.2. Changes with age It was not possible to determine each zone in the lens accurately for all 102 subjects, and therefore the number of measurements differs for each zone. This was mainly 2368 M. Dubbelman et al. / Vision Research 43 (2003) 2363–2375 1.6 110 Anterior cortex (mm) Grey value (au) 130 uncorrected corrected 90 70 50 35 yrs 30 1.2 1 0.8 0.6 ACT=0.51 + 0.012 * Age r = 0.80; n=102; p<0.0001 0.4 0.2 180 2.8 uncorrected 150 corrected Nucleus (mm) Grey value (au) (a) 1.4 120 90 60 64 yrs 2.4 2.2 2 1.8 NT=2.11 + 0.003 * Age r = 0.25; n=98; p=0.01 1.6 30 0 (b) 2.6 1 2 3 4 5 1.4 Fig. 4. Two examples of a densitogram (upper part: 35 year-old male, lower part: 64 year-old male) to indicate the influence of correction of the Scheimpflug images. The thick line represents the densitogram before correction, and the thin line represents the densitogram after correction. Note that the influence of the correction is not constant with age. because the posterior region of the crystalline lens showed less contrast, or could sometimes not be seen, because the pupil was small. Fig. 5 shows the change in thickness of the cortex and nucleus with age according to the classification of Hockwin et al. (1982), as indicated in the upper part of Fig. 1. With age, a small, but significant (p ¼ 0:01) increase in nuclear thickness could be measured, but the lens thickness increases primarily due to the increase in thickness of the anterior and posterior cortex. The increase of the anterior cortex is approximately 1.5 times greater than that of the posterior cortex. Table 1 shows the mean thickness and possible age-dependency of zones 1–8. Using the Oxford system (lower part of Fig. 1), zones C1–C3 can be differentiated within the anterior and posterior cortex. Fig. 6 shows the change in thickness of these three zones, and it can clearly be seen that the increase in both the anterior and posterior cortex with age is entirely due to zone C2 (Fig. 6b and e). Zones C1 and C3 of both the anterior and the posterior cortex show no significant change in thickness with age (p > 0:05). In the posterior cortex, zones C1–C3 could often not be determined accurately, and the number of measurements is therefore lower than for the anterior cortex. Fig. 7 shows a schematic drawing of the aging lens. The increase in thickness of the lens is mainly due to the increase of the anterior and posterior C2 zone. The curvature and thickness of the young and the old lens are in correct proportion, according to the Scheimpflug measurements. However, because the more pe- Posterior cortex (mm) Distance from anterior lens vertex (mm) 1.4 (c) 1.2 1 0.8 0.6 0.4 PCT=0.33 + 0.0082 * Age r = 0.71; n=89; p<0.0001 0.2 0 10 20 30 40 50 60 70 Age (years) Fig. 5. The change in thickness of the cortex and nucleus with age. See Fig. 1 for the determination of the different zones. (a) The anterior cortex (zones 1 and 2). There was a highly significant increase with age: ant.cortex ¼ 0.51 (±0.04) + 0.0116 (±0.007) age; n ¼ 102; r ¼ 0:8; p < 0:0001. (b) The nucleus (zones 3–6). Significant increase with age: nucleus ¼ 2.11 (±0.04) + 0.003 (±0.001) age; n ¼ 98; r ¼ 0:25; p ¼ 0:01. (c) The posterior cortex (zones 7 and 8). Highly significant increase with age: post.cortex ¼ 0.33 (±0.04) + 0.0082 (±0.007) age; n ¼ 89; r ¼ 0:71; p < 0:0001. ripheral parts of the lens are obscured by the iris, a hypothetical lens equator has been added for convenience, indicated by a dotted line. The age-dependency of the position of the sulcus with respect to the cornea was investigated. The sulcus is well defined in the densitogram as the dip in the centre of the nucleus. Fig. 8 shows the position of the sulcus with respect to the cornea, which showed no significant change with age (p ¼ 0:12). 3.3. Changes with accommodation In a first analysis, the different zones in the lens of every subject were marked, and the rate of change per diopter in the different zones was determined by means of orthogonal regression. Fig. 9 shows the age-dependency of the change in the anterior cortex, nucleus and M. Dubbelman et al. / Vision Research 43 (2003) 2363–2375 2369 Table 1 Zones 1–8 with age (see upper part Fig. 1) Zone Regression (equation) 1 2 3 4 5 6 7 8 ¼ 0.23(±0.03) + 0.012(±0.0008) age ¼ 0.73(±0.03) + 0.0016(±0.0008) age ¼ 0.74(±0.02) + 0.0011(±0.0006) age ¼ 0.18(±0.03) + 0.0076(±0.0008) age n r p Mean s.d. 102 99 102 102 101 100 87 85 )0.03 0.84 )0.04 0.21 0.19 0.14 0.72 0.07 0.73 <0.0001 0.66 0.04 0.055 0.15 <0.0001 0.55 0.28 0.7 0.34 0.79 0.78 0.31 0.5 0.17 0.05 0.2 0.07 0.10 0.07 0.06 0.13 0.04 Simple linear regression was applied and results for each zone are indicated in mm: regression equation, number of measurements ðnÞ, correlation coefficient ðrÞ, probability for rðpÞ, mean and standard deviation (s.d.). If there was no significant age-dependency, the equation is not given. 1 Anterior (a) C1 (mm) 0.8 Posterior (d) C1=0.20 + 0.0005 * Age r = 0.14; n=100; p=0.17 C1=0.13 + 0.00026 * Age r = 0.06; n=57; p=0.59 0.6 0.4 0.2 0 1 C2 (mm) 0.8 (b) (e) C2 = -0.15 + 0.012 * Age r = 0.89; n=100; p<0.0001 C2= -0.06 + 0.0065 * Age r = 0.73; n=56; p<0.0001 0.6 0.4 0.2 0 1 (c) (f) C3 =0.32 - 0.0007 * Age r = -0.15; n=101; p=0.14 C3 (mm) 0.8 C3=0.19 + 0.0005 * Age r = 0.10; n=81; p=0.37 0.6 0.4 0.2 0 10 20 30 40 50 60 Age (years) 70 10 20 30 40 50 60 70 Age (years) Fig. 6. The change in thickness (mm) of the C1, C2 and C3 zones in the anterior cortex (a–c) and posterior cortex (d–f). See Fig. 1 for the determination of the different zones. The C2 zones of the anterior and posterior cortex increased significantly in thickness with age. (a) Mean thickness C1 anterior: 0.22 (±0.04). (b) C2 anterior ¼ )0.15 (±0.04) + 0.012 (±0.001) Age. (c) Mean thickness C3 anterior: 0.30 (±0.06). (d) Mean thickness C1 posterior: 0.14 (±0.04). (e) C2 posterior ¼ )0.06 (±0.04) + 0.0065 (±0.001) Age. (f) Mean thickness C3 posterior: 0.21 (±0.06). posterior cortex during accommodation labeled according to Hockwin et al. (1982) and the Oxford system. It can be seen that there is no significant change per diopter in the cortex, and that the thickening of the lens with accommodation is primarily due to a change in the thickness of the nucleus. Furthermore, it appears that the results are dependent on the definition of the cortex and nucleus. Labeling the zones according the system of Hockwin et al. (1982), there is a minimal increase in thickness in the cortex with accommodation. However, defining the cortex and nucleus according to the Oxford system, there is even a suggestion of a reduction in cortical thickness with accommodation. Table 2 shows the mean values for the change in the cortical and nuclear zones with accommodation according to both systems. Furthermore, the movement of the sulcus, or nuclear dip during accommodation was investigated. During 2370 M. Dubbelman et al. / Vision Research 43 (2003) 2363–2375 Change in thickness (mm)/D 0.06 20 yrs a C1β C3 Nucleus C2 Change in thickness (mm)/D C1α p Sulcus C2 0.05 17 0.04 4 0.03 0.02 0.01 8 5 18 17 8 8 7 5 9 8 4 4 0 -0.01 ant. cortex nucleus post. cortex using the system of Hockwin et al. (1982) -0.02 -0.03 0.06 3 14 7 9 0.05 9 3 0.04 0.03 3 0.02 0.01 8 3 18 16 10 9 9 5 8 3 8 0 -0.01 ant. cortex nucleus post. cortex using the Oxford system -0.02 -0.03 19 65 yrs 25 31 37 43 49 Age (years) Fig. 7. Schematic drawing of the zones in the lens of a 20 year-old subject (upper part) and a 65 year-old subject to indicate the growth with aging. The increase in thickness of the lens is primarily due to the anterior and posterior C2 zone. Cornea ~ Sulcus (mm) 9 7 7 6 Fig. 9. Change in the anterior cortex, nucleus and posterior cortex in mm per diopter with age. The data are grouped in 6 bins. The number of measurements is indicated above each bin. In the upper part, the cortex and nucleus were labeled according to Hockwin et al. (1982). In the lower part, they were labeled according the Oxford system, in which the cortex consists of zones C1–C3 and the nucleus is defined as the area between the anterior and posterior C3 zone. Using the Oxford system, the increase in lens thickness is entirely due to the nucleus. 7 whole nucleus is uniformly stretched (indicated by the plateau of constant stretch in the nucleus, see Fig. 3). Thus, we were not able to detect significant recurrent dips, or peaks in the stretch-function, which would indicate that certain parts of the nucleus show a smaller or greater increase in thickness during accommodation. 6.5 6 5.5 5 Thick=5.47 + 0.003 * Age r = 0.15; n=102; p=0.12 4.5 4 10 20 30 40 50 60 70 Age (years) Fig. 8. The distance between the anterior vertex of the cornea and the sulcus. There is no significant change with age: cornea sulcus ¼ 5.47 (±0.08) + 0.003 (±0.002) age; n ¼ 102; r ¼ 0:15; p ¼ 0:12. accommodation there appeared to be a significant movement of the sulcus towards the cornea: mean (±s.d.) ¼ 0.011/D (±0.010), n ¼ 55, p < 0:0001. The results presented in Fig. 9 were obtained by manually marking the different zones of the lens and are consistent with those of the second method, in which the densitogram of the unaccommodated lens was stretched to match that of a lens in a higher accommodative state. These results also show that with accommodation, it is the nucleus that becomes thicker, while the thickness of the cortex generally remains constant. Using this method, it also becomes clear that, for the most part, the 4. Discussion 4.1. Correction of the Scheimpflug images Scheimpflug imaging can be used to determine different dark and lighter zones in the crystalline lens, which have been referred to as the zones of discontinuity. In the present study, the change in thickness of these zones with age and accommodation was investigated. In contrast with earlier Scheimpflug studies, correction was made for distortion due to the geometry of the Scheimpflug imaging system and the refraction of the cornea and lens. The method used to correct the Scheimpflug images has been described and validated in earlier publications (Dubbelman & Van der Heijde, 2001; Dubbelman et al., 2001). To correct the internal structure of the lens for the refraction of the lens itself, a simplification was made. M. Dubbelman et al. / Vision Research 43 (2003) 2363–2375 2371 Table 2 Change in cortical and nuclear thickness per diopter according the classification of Hockwin et al. (1982) and the Oxford system Mean According to Hockwin et al.: D anterior cortex (mm/D) D nucleus (mm/D) D posterior cortex (mm/D) 0.004 0.040 0.0006 S.D. S.E.M. n 0.005 0.011 0.007 0.001 0.0014 0.0006 54 50 47 According the Oxford system D anterior cortex (mm/D) D nucleus (mm/D) D posterior cortex (mm/D) )0.001 0.046 )0.002 0.007 0.013 0.005 0.001 0.0015 0.0014 56 46 44 Total lens thickness (mm/D) 0.045 0.012 0.0015 58 Parameters are the weighted mean, standard deviation, standard error of the mean and the number of measurements ðnÞ of the change per diopter with accommodation. The crystalline lens was assumed to consist of one homogeneous medium with one equivalent refractive index (nl ), whereas it is generally assumed that the lens has a gradient refractive index (GRIN) structure, with a maximum value in the centre of approximately 1.40 and a minimum value of approximately 1.37 in the periphery of the lens (Campbell, 1984; Pierscionek & Chan, 1989; Pierscionek, 1997). Thus, the nl is not intermediate between the index of the shell and the index of the nucleus, but greater than the maximum index found in the lens. However, the precise refractive structure of the human lens is still unknown, and can therefore not easily be implemented in the ray tracing procedure to correct the Scheimpflug images. Because the change in the refractive index is mainly found in the anterior and posterior cortex, the major errors are made in the determination of the dimensions of these zones. However, the values of these errors are small, because the correction for the refraction of the lens itself plays only a minor part in distorting the shape of the lens, compared to the influence of the anterior chamber depth and the refraction of the anterior corneal surface. An estimation of the size of these errors was made by correcting the images, using different values for the nl . Lowering the value for the nl with 0.01 will decrease the thickness of the anterior and posterior cortex no more than 10 and 1 lm, respectively. The nucleus will decrease approximately 12 lm. Thus, if the gradient refractive index of the lens is not taken into account, the size of the anterior and posterior cortex will be underestimated. However, this underestimation will probably not exceed 25 lm, a value that is negligible compared to the interindividual variation of the cortical thickness. For the measurements during accommodation, the effect can be ignored if no great changes in the gradient refractive index will occur during accommodation. In that case, the gradient index will, nevertheless, cause an error in the absolute thickness of the zones, but will hardly influence the measurement of the rate of change in thickness per diopter. It must be noted that the results with accommodation have been obtained by presenting an accommodative stimulus, which is not necessarily the same as the accommodative response of the eye. It has been reported that for a zero accommodation stimulus, the accommodation is not completely relaxed leading to accommodative lead, while for higher accommodation levels, the accommodative response is lower than the accommodative stimulus leading to accommodative lag (Abbott, Schmid, & Strang, 1998; Goss & Zhai, 1994). The implications for the results with accommodation will be that the absolute change in thickness of the whole lens and the various layers per diopter given in Fig. 9 and Table 2 will be slightly underestimated. Obviously, this accommodation lag does not influence the results of the relative change during accommodation of the various zones with respect to each other. 4.2. Origin of the scattering The different zones within the human lens that are visible on the Scheimpflug images result from the different light scattering properties of each zone. However, the exact origin of the scattering is still unclear. The light scattering observed with the slit lamp or Scheimpflug camera is known as backward scattering, and must be distinguished from forward scattering in the direction of the retina, which in fact is much more important for vision. The intensity of the backward light scattering is strongly dependent on the angle of illumination and observation (Van den Berg & Spekreijse, 1999). The protein concentration, which varies within the lens, is an important parameter for light scatter. Nevertheless, such a variation did not explain the different light scattering properties of the various lens zones (Yaroslavsky et al., 1994). Therefore, it is likely that factors such as the configurations of the lens proteins and the orientation or size of the lens fibres contribute to the appearance of the zones of discontinuity. In addition, it has been shown that the lens fibre membranes or extracellular spaces 2372 M. Dubbelman et al. / Vision Research 43 (2003) 2363–2375 also act as sources for the scattering of light (Bettelheim, 1985). Furthermore, a large part of the light scattering is, in fact, not real light scatter, but specular reflection (Weale, 1986a, 1986b). This would suggest that there are ragged surfaces within the lens, which separate areas of different refractive index (Goldmann, 1964; Huggert, 1948). It is also highly probable that the lens sutures play a role in the explanation of the existence of the zones of discontinuity (Kuszak, Deutch, & Brown, 1994). New lens fibres formed from the cells at the equator extend anteriorly and posteriorly to join with other fibres to form the lens sutures, which become more complex as the lens cells form successive layers throughout life (Kuszak & Brown, 1994). According to Koretz, Cook, and Kuszak (1994), the location of the zones of discontinuity is directly correlated with the development of the lens sutures. Furthermore, it has been demonstrated that there is a relationship between optical lens quality and the lens sutures (Kuszak, Peterson, Sivak, & Herbert, 1994; Kuszak, Sivak, & Weerheim, 1991). 4.3. Changes with age Because of the lack of a clear definition of the boundary between nucleus and cortex, it is obvious that the lens nucleus is not a uniform concept, but has to be carefully defined each time it is used. In the present study, two different definitions were used (Fig. 1): zones 3 to 6 (Hockwin et al.) and the area between the anterior and posterior C3 zones (according to the Oxford system). The results with age show that for both definitions of the nucleus the change in thickness of the cortex is approximately 7 times greater than that of the nucleus, which is significantly more than the value reported by other Scheimpflug studies in which no correction was made for the refraction of the cornea and lens. In contrast with the findings of Cook et al. (1994), i.e. a decrease in nuclear thickness with age, in the present study a small increase in nuclear thickness of approximately 3 lm/years was found, which was entirely due to thickening in the central nuclear zone (zones 4 and 5). The thickness of the anterior and posterior cortex increased at a rate of approximately 12 and 8 lm/years, respectively. The increase in thickness of the anterior cortex is thus 1.5 times greater than that of the posterior cortex, which is less than the values of 3 and 2.4 times reported by Kashima et al. (1993) and Cook et al. (1994). Classification according the Oxford system makes it possible to discern which layers of the cortex increase in thickness with age. For the first time, the change in thickness of zones C1–C3 of the posterior lens cortex has been measured. For both the anterior and the posterior cortex, it appeared that C1 and C3 do not significantly change in thickness with age and that the increase of the cortex is entirely due to the increase in thickness of the C2 zone. Thus, the nucleus and the adjacent C3 zones change little in width with age. This implies that after appearance of the C3 zone during the second decade of life, the process of compaction would solely be restricted to the C1 and C2 zones. This is consistent with the observation made by Brown and Bron (1996), that nuclear compaction only occurs during the first 20 years of life, while cortical compaction occurs throughout the entire life span. The latter was supported by the study carried out by Brown (1976) in which it was observed that cortical cataracts sank into the lens at a faster rate than the rate at which the lens was growing. Calculations make it clear that this finding cannot be explained by the distortion due to refraction of the cornea and lens. Nuclear compaction in the first two decades of life could explain why there is almost no increase in lens thickness, and that even thinning of the lens has been observed up to 15 years of age (Mutti et al., 1998). New fibres are added to the surface of C1 a, but no increase in the thickness of C1 was observed. The underlying fibres will therefore enter the C2 zone, which implies a change in their light scattering properties. These fibres pass through a phase of increased light scatter as they enter C1 b, followed by a phase of decreased light scatter when they are regarded to belong to the subsequent C2 zone. A possible explanation for this change of the light scattering properties could be the process of denucleation of the fibres associated with the formation of the nuclear bow and the breakdown of the mitochondria, which lead to the dispersal of particulate material and Ca2þ within the fibre (Bron et al., 2000). There is no evident relationship of the zones observed in vivo using a slit lamp or Scheimpflug camera and the various lens regions distinguished in certain in vitro studies on lens morphology. Taylor et al. (1996) analysed the fibres in five lens regions: deep cortex, adult nucleus (fibre cells formed since puberty), juvenile nucleus (fibre cells formed from birth until the onset of puberty), fetal nucleus (fibre cells formed from the seventh week of development until birth), and embryonic nucleus (formed in the 6 weeks after fertilisation). Each region appeared to have characteristic cell shapes and sizes, and the approximate thickness of each zone was given for an average age of 61 years. Comparing their results with the measurements of the different lens zones in the present study shows that the embryonic nucleus corresponds to the sulcus, and the fetal nucleus (thickness: ±2.14 mm) corresponds well to the nucleus defined according to Hockwin et al. (zone 3–6: ±2.2 mm) and the area between the C4 zones according to the Oxford system (±2.2 mm). This is consistent with the fact that the Oxford system reserves the term nucleus only for that part of the lens, which is present at birth (Brown & Bron, 1996). Thus, only cortical layers are added postnatally. This avoids the confusing of regarding a set of M. Dubbelman et al. / Vision Research 43 (2003) 2363–2375 lens fibres as cortex at one period, but as nucleus at a later period when they occupy a deeper position in the lens. For the cortex, it becomes more difficult. Zones 2 and 7, defined by Hockwin et al. as the anterior (±1 mm) and posterior cortex (±0.65 mm), roughly correspond to the adult and juvenile nucleus combined (±1.25 mm) according Taylor et al. (1996). As a result, zones 1 and 8 (±0.22 mm) should therefore be identical to what Taylor et al. define as the deep cortex (±0.7 mm). The difference in thickness, however, is large. The C4 zone (±0.2 mm) according to the Oxford system corresponds to the juvenile nucleus (±0.19 mm), but relating zones C1–C3 to the remaining adult nucleus and deep cortex is difficult. This might be explained by the fact that zones C1–C3 correspond to zones in the lens with different light scattering properties, whereas in the in vitro study carried out by Taylor et al. (1996) several regions were distinguished on account of the shape and size of the cells. It can be expected that there is a relationship between the former and the latter, but this does not need to be obligatory, especially because the exact origin of the scattering is still unclear. According to Koretz, Kaufman, Neider, and Goeckner (1989a, 1989b), the anterior chamber shallows with age at a rate equal to the increase in thickness of the lens, i.e. the anterior segment length (distance from the cornea to the posterior lens surface) remains constant. Consequently, in a subsequent analysis of the change in the internal structure with age (Cook et al., 1994), their results showed that the nucleus is gradually translated anteriorly (towards the cornea) with increasing age at the rate of posterior cortical thickening. However, in an earlier study (Dubbelman et al., 2001), it was shown that correction of the Scheimpflug images leads to significantly different results with regard to the change in the anterior segment length with age. It appeared that the posterior lens surface receded from the cornea with age, and that this backward movement did not differ significantly from the forward movement of the anterior lens surface. In the present study, it was found that the distance between the cornea and the sulcus, which can be regarded as the centre of the nucleus, did not change with age. Thus, the nucleus is not gradually translated anteriorly (towards the cornea) with increasing age, but stays in the same position. 4.4. Changes with accommodation The results of the change in the internal structure of the lens with accommodation are consistent with earlier Scheimpflug studies measuring accommodation: the increase in lens thickness is mainly due to an increase in the thickness of the nucleus. The magnitude of this thickening depends on the definition of the nucleus. The anterior and posterior C3 zone are zones of high light scatter, and in between is the rather dark zone of low 2373 light scatter, which is regarded as the nucleus. According to Hockwin et al. (1982), the peri-nuclear zone (zones 3 and 6) begins and ends when the side of the C3 zone orientated towards the centre of the lens reaches a local minimum in the densitogram. According to the Oxford system, the nucleus was defined at the steepest part (maximum gradient) of the side of the C3 zone (actually, behind the C3 zone there is first the low scatter C4 zone that is considered to precede the nucleus, but because this C4 zone is difficult to determine, the nucleus was defined as the area between the C3 zones). According to this definition, the thickening of the lens with accommodation is entirely due to a change in the thickness of the nucleus and there is even a suggestion of a reduction in cortical thickness with accommodation. Defined according to the system of Hockwin et al. (1982), there is still a slight increase in cortical thickness with accommodation. This indicates that there is a small accommodative increase in width between the position of the highest gradient of the side of the C3 zone adjacent to the nucleus and the point where this side reaches a local minimum. It must be noted that the differences between the two systems are smaller than the pixel size, which is approximately the precision with which a transition between the lens zones can be determined. Nevertheless, it can be concluded that the anterior and posterior cortex, defined as zones C1–C3, show no change in thickness with accommodation. This finding is also supported by the non-uniform stretching of the densitogram of the unaccommodated lens. The stretching generally shows a plateau of constant stretch within the nucleus, which makes it clear that with accommodation there is a uniform thickening of the nucleus. This can also be observed from the Scheimpflug images: the nuclear dip in the centre of the lens, of which the minimum represents the position of the sulcus, becomes wider with accommodation. The stretch could provide insight into the stiffness profile within the lens. The sudden change in stretch at the transition between anterior cortex and nucleus indicates an abrupt change in the stiffness of the lens. However, the subsequent plateau of constant stretch in the nucleus does not necessarily reflect constant nuclear stiffness. There is a complex distribution of forces within the lens, and it is possible that uniform stiffness in the lens does not result in uniform stretch. The fact, however, that there is a uniform stretch in the nucleus can be used to model the forces within the lens during accommodation. Furthermore, the growth of the cortex with age also alters the distribution of the accommodative forces within the lens. The zonular forces must be transmitted through the capsule and the cortex to influence the nuclear shape with accommodation. This transmission could be more difficult if the nucleus is surrounded during the growth of the lens by a continuously increasing cortex, and this could possibly be a factor in the occurrence of presbyopia. 2374 M. Dubbelman et al. / Vision Research 43 (2003) 2363–2375 Acknowledgements This research was partially supported by a grant from Pharmacia Groningen, The Netherlands. We wish to thank T.J.T.P. van den Berg, PhD, and J.C. Coppens, MSc, from the Netherlands Ophthalmological Research Institute and AMC/Department of Medical Physics in Amsterdam, for their helpful comments and for giving us the opportunity to use their Nidek EAS-1000 Scheimpflug camera. References Abbott, M. L., Schmid, K. L., & Strang, N. C. (1998). Differences in the accommodation stimulus response curves of adult myopes and emmetropes. Ophthalmic Physiological Optics, 18(1), 13–20. Al-Ghoul, K. J., Nordgren, R. K., Kuszak, A. J., Freel, C. D., Costello, M. J., & Kuszak, J. R. (2001). Structural evidence of human nuclear fiber compaction as a function of ageing and cataractogenesis. Experimental Eye Research, 72(3), 199–214. Bettelheim, F. A. (1985). Physical basis of lens transparency. In E. Maisel (Ed.), The ocular lens. Structure, function and pathology (pp. 265–300). New York: Marcel Dekker. Bevington, P. R. (1969). Data reduction and error analysis for the physical sciences. New York: McGraw-Hill, pp. 77–80. Bron, A. J., Vrensen, G. F., Koretz, J., Maraini, G., & Harding, J. J. (2000). The ageing lens. Ophthalmologica, 214(1), 86–104. Brown, N. (1973). The change in shape and internal form of the lens of the eye on accommodation. Experimental Eye Research, 15(4), 441– 459. Brown, N. (1976). Dating the onset of cataract. Transactions of the Ophthalmological Society of UK, 96(1), 18–23. Brown, N. P., & Bron, A. J. (1996). Lens disorders: a clinical manual of cataract diagnosis. Oxford: Butterworth-Heinemann, pp. 23–26. Brown, N. A. P., Sparrow, J. M., & Bron, A. J. (1988). Central compaction in the process of lens growth as indicated by lamellar cataract. British Journal of Ophthalmology, 72, 538–544. Campbell, M. C. (1984). Measurement of refractive index in an intact crystalline lens. Vision Research, 24, 409–415. Cook, C. A., Koretz, J. F., Pfahnl, A., Hyun, J., & Kaufman, P. L. (1994). Aging of the human crystalline lens and anterior segment. Vision Research, 34(22), 2945–2954. Dubbelman, M., & Van der Heijde, G. L. (2001). The shape of the aging human lens: curvature, equivalent refractive index and the lens paradox. Vision Research, 41, 1867–1877. Dubbelman, M., Van der Heijde, G. L., & Weeber, H. A. (2001). The thickness of the aging human lens obtained from corrected Scheimpflug images. Optometry and Vision Science, 78(6), 411–416. Goldmann, H. (1964). Senile changes of the lens and the vitreous. American Journal of Ophthalmology, 57, 1–13. Goss, D. A., & Zhai, H. (1994). Clinical and laboratory investigations of the relationship of accommodation and convergence function with refractive error. A literature review. Documenta Ophthalmologica, 86(4), 349–380. Hockwin, O., Dragomirescu, V., & Laser, H. (1982). Measurements of lens transparency or its disturbances by densitometric image analysis of Scheimpflug photographs. Graefes Archives of Clinical and Experimental Ophthalmology, 219(6), 255–262. Huggert, A. (1948). On the form of the iso-indicial surfaces of the human crystalline lens. Acta Ophthalmologica (Suppl. 30), 1–128. Kashima, K., Trus, B. L., Unser, M., Edwards, P. A., & Datiles, M. B. (1993). Aging studies on normal lens using the Scheimpflug slitlamp camera. Investigative Ophthalmology and Visual Science, 34(1), 263–269. Koretz, J. F., Cook, C. A., & Kaufman, P. L. (1997). Accommodation and presbyopia in the human eye. Changes in the anterior segment and crystalline lens with focus. Investigative Ophthalmology and Visual Science, 38(3), 569–578. Koretz, J. F., Cook, C. A., & Kuszak, J. R. (1994). The zones of discontinuity in the human lens: development and distribution with age. Vision Research, 34(22), 2955–2962. Koretz, J. F., Kaufman, P. L., Neider, M. W., & Goeckner, P. A. (1989a). Accommodation and presbyopia in the human eye, aging of the anterior segment. Vision Research, 29, 1685–1692. Koretz, J. F., Kaufman, P. L., Neider, M. W., & Goeckner, P. A. (1989b). Accommodation and presbyopia in the human eye. 1: Evaluation of in vivo measurement techniques. Applied Optics, 28, 1097–1102. Kuszak, J. R., & Brown, H. G. (1994). Embryology and anatomy of the lens. In D. A. Albert, & F. A. Jacobiec (Eds.), The principles and Practice of ophthalmology. Basic sciences (pp. 82–96). Philadelphia: W.B. Saunders. Kuszak, J. R., Deutch, T. A., & Brown, H. G. (1994). Anatomy of aged and senile cataractous lenses. In D. A. Albert, & F. A. Jacobiec (Eds.), The principles and practice of ophthalmology. Clinical practice, vol.1 (pp. 564–575). W.B. Saunders: Philadelphia. Kuszak, J. R., Peterson, K. L., Sivak, J. G., & Herbert, K. L. (1994). The interrelationship of lens anatomy and optical quality II. Primate lenses. Experimental Eye Research, 59(5), 521–535. Kuszak, J. R., Sivak, J. G., & Weerheim, J. A. (1991). Lens optical quality is a direct function of lens sutural architecture. Investigative Ophthalmology and Visual Science, 32(7), 2119–2129. Mutti, D. O., Zadnik, K., Fusaro, R. E., Friedman, N. E., Sholtz, R. I., & Adams, A. J. (1998). Optical and structural development of the crystalline lens in childhood. Investigative Ophthalmology and Visual Science, 39(1), 120–133. Niesel, P., Krauchi, H., & Bachmann, E. (1976). Der Abspaltungsstreifen in der Spaltlampenphotographie der alternden Linse. Albrecht Von Graefes Archiv fur Klinische und Experimentelle Ophthalmologie, 199(1), 11–20. Patnaik, B. (1967). A photographic study of accommodative mechanisms: Changes in the lens nucleus during accommodation. Investigative Ophthalmology, 6, 601–611. Pierscionek, B. K. (1997). Refractive index contours in the human lens. Experimental Eye Research, 64(6), 822–829. Pierscionek, B. K., & Chan, D. Y. (1989). Refractive index gradient of the human lens. Optometry and Vision Science, 66, 822–829. Pierscionek, B. K., & Weale, R. A. (1995). The optics of the eye-lens and lenticular senescence. Documenta Ophthalmologica, 89, 321–335. Press, W. H., Flannery, B. P., Teukolski, S., & Vetterling, W. T. (1994). Numerical recipes in C. Cambridge: Cambridge University Press, pp. 666–670. Rabie, E. P., Steele, C., & Davies, D. E. (1986). Anterior chamber pachymetry during accommodation in emmetropic and myopic eyes. Ophthalmic and Physiological Optics, 6(3), 283–286. Ray, S. F. (1995). Applied photographic optics (p. 452). Oxford: Focal Press. Richards, D. W., Russell, S. R., & Anderson, D. R. (1988). A method for improved biometry of the anterior chamber with a Scheimpflug technique. Investigative Ophthalmology and Visual Science, 29(12), 1826–1835. Sakamoto, Y., & Sasaki, K. (1994). Accuracy of biometrical data obtained from the Nidek Eas-1000. Ophthalmic Research, 26(Suppl. 1), 26–32. Sasaki, K., Sakamoto, Y., Shibata, T., & Emori, Y. (1990). The multipurpose camera: a new anterior eye segment analysis system. Ophthalmic Research, 22(Suppl. 1), 3–8. Shibata, T., Hockwin, O., Weigelin, E., Kleifeld, O., & Dragomirescu, V. (1984). Biometrie der Linse in Abh€angigkeit vom Lebensalter und von der Kataraktmorphologie. Klinische Monatsbl€atter f€ur Augenheilkunde, 185(1), 35–42. M. Dubbelman et al. / Vision Research 43 (2003) 2363–2375 Smith, G. T., Smith, R. C., Brown, N. A., Bron, A. J., & Harris, M. L. (1992). Changes in light scatter and width measurements from the human lens cortex with age. Eye, 6, 55–59. Sparrow, J. M., Bron, A. J., Brown, N. A., Ayliffe, W., & Hill, A. R. (1986). The oxford clinical cataract classification and grading system. International Ophthalmology, 9(4), 207–225. Taylor, V. L., Al-Ghoul, K. J., Lane, C. W., Davis, V. A., Kuszak, J. R., & Costello, M. J. (1996). Morphology of the normal human lens. Investigative Ophthalmology and Visual Science, 37(7), 1396– 1410. Van den Berg, T. J., & Spekreijse, H. (1999). Light scattering model for donor lenses as a function of depth. Vision Research, 39(8), 1437– 1445. 2375 Weale, R. A. (1986a). Real light scatter in the human crystalline lens. Graefes Archive for Clinical and Experimental Ophthalmology, 224(5), 463–466. Weale, R. A. (1986b). New method for visualising discontinuities in the crystalline lens. British Journal of Ophthalmology, 70(12), 925– 930. Wegener, A., & Laser, H. (1996). Imaging of the spatial density distribution on the capsule of the lens with Scheimpflug photography. Ophthalmic Research, 28(Suppl. 2), 86–91. Yaroslavsky, I. V., Yaroslavsky, A. N., Otto, C., Puppels, G. J., Vrensen, G. F., Duindam, H., & Greve, J. (1994). Combined elastic and Raman light scattering of human eye lenses. Experimental Eye Research, 59(4), 393–399.