* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Section Three:
Coronary artery disease wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Atrial septal defect wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
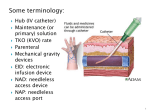
Section Three: Pulmonary Artery Pressure Monitoring The pulmonary artery (PA), flow-directed, balloon-tipped catheter has made possible the assessment of right ventricular function, pulmonary vascular status, and indirectly, left ventricular (LV) function. Cardiac output (CO), right atrial (RA), right ventricular (RV), pulmonary artery (PA) pressures and the pulmonary capillary wedge pressure (PCWP) may be directly measured using a PA catheter. The pressures and cardiac output obtained using this catheter allow the clinician to calculate derived parameters and facilitate diagnosis of cardiovascular and cardiopulmonary dysfunction, determine the therapy needed, and evaluate the effectiveness of the interventions. Pulmonary Artery Catheters Several types of flow-directed, balloon-tipped PA catheters are available in different sizes. The type of catheter used is determined by the parameters to be monitored and additional requirements governed by the patient’s condition. The 7.5-French (Fr. indicates catheter lumen size), 110 cm long, thermodilution catheter is the size used most often. Most PA catheters have several external ports or lumen hubs corresponding to internal lumens and lumen openings into the right heart and PA (Fig. 6). Four lumens with external hubs or ports are common to all PA catheters: proximal hub and lumen distal hub and lumen balloon inflation valve and lumen thermistor connector and lumen. The proximal or RA lumen opens into the right atrium. It may be connected to a transducer and used to obtain RA pressure measurements and display of the RA pressure waveform continuously or intermittently. Fluids or medications may be administered through this port. It is also used as the injectate port for measuring cardiac outputs. Do not use to infuse vasoactive agents such as dopamine or nitroprusside if the injection method is used to do intermittent cardiac outputs as patient will be bolused with the vasoactive agent. Figure 6. Pulmonary Artery Catheter Section Three – Pulmonary Artery Pressure Monitoring 19 The distal or PA lumen hub is always attached to a transducer and a continuous flush system. Heparin is usually added to the flush solution in order to prevent thrombi and fibrin deposits on the catheter tip, although some studies have shown it may not be necessary. Check your unit protocol. The PA waveform is displayed continuously, as are the PA systolic, diastolic, and mean pressures. Mixed venous blood gases, necessary for oxygen extraction, oxygen consumption, and intrapulmonary shunt measurements, may be withdrawn from the distal PA port. The PA port is not usually used for fluid or medication administration. The balloon inflation port and lumen enable the clinician to inflate the balloon at the catheter tip with a small volume of air (1.5 ml maximum) to measure the PA occlusion, or pulmonary capillary wedge pressure (PCWP). The tip of the PA catheter also contains a thermistor. The external thermistor port is connected to the bedside monitor or to a cardiac output computer. The thermistor permits measurement of the patient’s temperature in the PA (core temperature), and it detects the blood temperature change when solution is injected through the RA port to obtain a cardiac output measurement. Specialty PA catheters include the above components and additional features and lumens. Some of the specialty features include: a second proximal lumen that serves as an additional infusion port a right ventricular lumen that may be used for infusions or insertion of a cardiac pacemaker probe (designated for the particular type of PA catheter) if temporary ventricular pacing is required a lumen containing fiberoptic filaments allowing continuous measurement of mixed venous oxygen saturation (SvO2) or continuous measurement and display of cardiac output; and right ventricular ejection fraction determinations. Pulmonary Artery Catheter Insertion Before the catheter is inserted consent for the procedure should be obtained, the reason for the procedure and the procedure itself should be explained to the patient/family, and all necessary equipment should be assembled. The exact setup and equipment used will vary depending on the institution. The tubing and transducer are prepared as described in Section One and the transducer is leveled and zeroed. Prior to insertion each lumen of the PA catheter is flushed with sterile solution from the flush system to ensure all air bubbles are removed. (Note: Fiberoptic SvO2 monitoring catheters are calibrated prior to flushing lumens of the PA catheter). The PCWP balloon should be inflated with air to ensure proper inflation and in order to evaluate for leaks before the catheter is inserted. Many institutions use insertion kits that include a sterile sleeve that is placed over the catheter prior to insertion. This allows catheter manipulation, if necessary, after insertion, without compromising sterile technique. Strict sterile technique is required for the PA catheter insertion procedure. The physician performing the procedure wears a cap, mask, sterile gown, and sterile gloves. The nurse assisting wears a cap and mask and if manipulating the catheter, sterile gloves. A sterile field is also used. The PA catheter is inserted into a large vein through an introducer catheter, which is usually placed by a percutaneous approach. The most common insertion site is the subclavian vein. Other sites that may be used are the internal jugular vein or femoral vein. Patient condition and practitioner preference are major determinants. Once the introducer is in place, the PA distal port is attached to the transducer/tubing and the PA catheter is inserted by the physician and threaded into place. Determination of the catheter tip location is established by monitoring the waveform and pressures on the bedside monitor as the catheter passes through the vena cava to the right atrium. The strip recorder is started in order to ensure documentation of Section Three – Pulmonary Artery Pressure Monitoring 20 waveform/pressure in each chamber. When the catheter tip is in the right atrium, the PA balloon is inflated with 1.5 mL of air to help “float” the catheter through the tricuspid valve into the right ventricle, across the pulmonic valve into the PA, and eventually into the wedged position (Fig. 7). The balloon is allowed to deflate passively after the PA wedge waveform is noted on the monitor and return of the PA waveform is confirmed. The physician sutures the introducer in place. Determine the goals of therapy. It is important for the RN to know the range of hemodynamic parameters desired by the physician. Nursing responsibilities during the insertion procedure include: Complications of PA Catheters Monitor sterile technique Monitor the changes in hemodynamic waveforms Record the pressures in each chamber of the heart after examining waveform strips Monitor the patient for complications. Ventricular dysrhythmias are the most common complication during PA catheter insertion procedure. Complete documentation of insertion waveform strips and pressures. Obtain cardiac output and hemodynamic profile immediately after insertion in order to document a complete baseline profile. Pneumothorax Pneumothorax is a complication of PA catheter introducer insertion through the subclavian vein. The anatomy of the patient can make placement of a PA catheter difficult, particularly if the patient is obese or has torturous subclavian veins. The needle or introducer sheath may puncture the lung during insertion and cause an apical pneumothorax. Less likely, but possible, is a pneumothorax during insertion through the jugular vein. A routine postinsertion chest radiograph should be obtained and the patient should be evaluated for signs and symptoms of a pneumothorax. Infection Figure 7. Normal cardiac waveforms and pressures seen in heart chambers and PA. After catheter insertion: Apply a sterile dressing over the insertion site. Verify catheter position with a chest radiograph. Set monitor alarms appropriate for the patient. Systemic infection and sepsis are caused by contamination of the PA catheter, insertion site, or pressure monitoring system. Careful attention to sterile technique during pressure tubing assembly, insertion, when entering the system, and caring for the insertion site help to prevent infection. Diagnosis of PA catheter related sepsis is based on blood cultures, white blood cell count, left shift on differential, and fever in the absence of other sources of infection. Clinical studies recommend that PA catheters and catheter introducers should be replaced at least every 5 days and the flush solution, tubing, transducer every 72 hours (less time than that recommended for arterial line system changes. Dressing should be changed according to unit protocol. Ventricular Arrhythmias Ventricular arrhythmias are common during the insertion of a PA catheter, and may occur during the removal of the catheter. As the Section Three – Pulmonary Artery Pressure Monitoring 21 catheter passes through the right ventricle, it may irritate the endocardium and cause PVCs and occasionally VT. The arrhythmias typically resolve when the catheter is advanced into the PA. After the PA catheter is in proper position in the PA, it may become dislodged if not well secured, and the tip may “fall back” into the right ventricle. The patient may experience arrhythmias, and the hemodynamic pressures and waveform will reflect those of the right ventricle. The catheter may be re-advanced by the physician (or nurse, according to unit policy) if protected by a sterile sheath, or may be withdrawn back into RA. It is essential to have ready access to emergency drugs and equipment should the ventricular arrhythmias persist. take experience to detect!) This does not harm the patient, but the balloon port should be labeled as “balloon ruptured” in order to alert subsequent caregivers and prevent injection of air into the pulmonary artery. The PCWP will not be able to be obtained if this happens. Pulmonary Artery Rupture or Perforation A rare but very serious and potentially fatal complication related to PA catheters is rupture or perforation of the PA. Perforation of the PA may occur during insertion or manipulation of the PA catheter. Patients with friable PA may be at some risk; proper advancement of the catheter with the balloon fully inflated with 1.5 mL of air, however, and avoidance of advancing the catheter too far into a small artery minimize the chance of PA perforation. Rupture of the PA is associated with overinflation of the balloon, particularly if the catheter has migrated distally into a small PA. Avoid overwedging of the balloon port. (See Figure 7A) Close observation of the PA waveform as the balloon is inflated and only filling the balloon with the amount of air to obtain a PCWP tracing prevent overdistending a small PA. If less air is required to obtain the PCWP waveform, the catheter has migrated out of proper position. Do not inflate the balloon longer than 10-15 seconds. Balloon Rupture The balloon may rupture. When this occurs, the air injected does not passively return into the syringe after being injected and/or it may “feel” different when inflated, there is less resistance. (Although this change in how it “feels” would Figure 7A. Overwedge Nursing Considerations Nursing care of the patient undergoing PA pressure monitoring is complex. The critical care nurse must be able to interpret waveforms and pressure data (discussed in more detail below) and be alert to potential complications. Interventions, outlined previously, that ensure accurate readings and minimize operator error apply to the patient with a PA catheter. Consistency of leveling and measurement techniques are especially important because small variations in the zero reference point will elicit large and erroneous changes in the RAP and PCWP. Identification of technical problems and the ability to troubleshoot possible causes and intervene appropriately are crucial competencies of the critical care nurse. Table 1 outlines possible problems and troubleshooting strategies related to hemodynamic pressure monitoring. Review material from this section by completing the Self-Test that follows, and then compare your answers with those given. Section Three – Pulmonary Artery Pressure Monitoring 22 Problem Causes Waveform overdamped Waveform underdamped Catheter fling, artifact No waveform Abnormally high pressures Abnormally low pressures Backflow of blood into tubing Air bubbles in system Blood clots in system or tip of catheter Catheter or tubing kinks Loss of pressure in pressure bag Catheter against vessel wall Treatment/Interventions Carefully examine system, especially at stopcocks, for bubbles and blood; flush out. Withdraw blood back to dislodge clots at catheter tip, then flush system. Inflate pressure bag to 300 mm Hg Notify physician; may need catheter repositioned Air bubbles, especially pinpoint Tubing too long due to added extentions. Carefully check for tiny air bubbles in system and flush. Ensure tubing is 3 – 4 feet, max. Turn pt. to left side to assist catheter in floating away from pulmonic valve. Stabilize tubing prior to obtaining readings Ensure tubing length is < 3-4 ft Eliminate excess stopcocks Ensure stopcocks are correctly positioned. Check for catheter/tubing kinks Check that monitor channel is on, cable connected and scale is correct. Catheter tip near pulmonic valve (PA catheter) Movement of tubing Excessive tubing length or stopcocks Stopcock turned Catheter/tubing kinked Monitor channel off, transducer cable not connected to monitor, or scale set inappropriately Monitor not zeroed Re-zero Transducer below phlebostatic axis Re-level Monitor not zeroed Re-zero Transducer above phlebostatic axis Re-level Stopcocks turned the wrong way Pressure bag not sufficiently inflated Ensure that stopcock is turned off to patient before opening transducer to air. Flush bag empty Check position of all stopcocks. Check pressure in bag, fluid level. Table 1. Troubleshooting technical problems of hemodynamic monitoring systems. Section Three – Pulmonary Artery Pressure Monitoring 23 Section Three – Pulmonary Artery Pressure Monitoring 24 Section Three Self-Test Match the PA catheter port with its use: 1. _____ Connect cardiac output (CO)computer to this port. a) Proximal port 2. _____ Inject CO injectate through this port. b) Distal port 3. _____ Insert temporary pacemaker lead through this port. c) Balloon port 4. _____ Obtain PCWP with use of this port. d) Thermistor 5. _____ Attach this port to a transducer to obtain e) Right ventricular continuous PA readings port Match the technical problem with the possible cause: 6. _____Scale on monitor set inappropriately. a) Blood backed up into tubing 7. _____ Stopcock or transducer turned the wrong way b) Underdamped waveform with dead-end cap off. 8. _____ Tubing too long. c) Overdamped waveform 9. _____ Blood clot at catheter tip. d) No waveform 10._____ Tubing movement outside patient or catheter moving e) Catheter “fling” inside patient. Section Three – Pulmonary Artery Pressure Monitoring 25 Section Three Self-Test - Answers Match the PA catheter port with its use: 1. D Connect cardiac output (CO)computer to this port. a) Proximal port 2. A Inject CO injectate through this port. b) Distal port 3. E Insert temporary pacemaker lead through this port. c) Balloon port 4. C Obtain PCWP with use of this port. d) Thermistor 5. B Attach this port to a transducer to obtain continuous readings. e) Right ventricular PA port . Match the technical problem with the possible cause: 6. D Scale on monitor set inappropriately. tubing a) Blood backed up into 7. A Stopcock turned the wrong way. waveform b) Underdamped 8. B Tubing too long. waveform c) Overdamped 9. C Blood clot at catheter tip. d) No waveform 10. E Tubing movement outside patient or catheter moving e) Catheter “fling” inside patient Section Three – Pulmonary Artery Pressure Monitoring 26 Section Three – Pulmonary Artery Pressure Monitoring 27